Ultraviolet B Phototherapy Intervention in Patients with Multiple Sclerosis: A Prospective, Randomized Pilot Trial
Abstract
Background
There is substantial evidence, from well-conducted epidemiological studies, that low vitamin D levels are correlated with increased risk for MS, and multiple case control studies have implicated the involvement of vitamin D deficiency in MS etiology. Narrow-band Ultraviolet B (NB-UVB; 300nm - 311 nm) induced vitamin D production has not previously been studied in a multiple sclerosis (MS) randomized placebo-controlled trial (RCT).
Objectives
To investigate NB-UVB induced vitamin D production, immunomodulation and MS symptomology following NB-UVB phototherapy in a MS cohort.
Methods
Using a blinded RCT study design, twelve individuals 18 years or older with MS were enrolled and assigned (1:1) into individualized NB-UVB dose (10-30kJ/m) phototherapy, or into placebo treatment, delivered 3 times per week, for 8-weeks. Serum vitamin D levels, walking performance, strength, cognitive function, mood and circulating progenitor cells (CPCs: CD34+CD45dim), monocyte populations (Intermediate CD14+CD16+, Classical CD14+CD16-), and T regulatory cell (CD4+/CD25+/FoxP3+Tregs) count were assesed. The data were analyzed by 2 x 3 mixed factor ANOVA.
Results
A statistically significant condition by time interaction on vitamin D levels (F=7.14, p<.005, partial η2=.42) was identified. NB-UVB phototherapy may provide immunomodulation in a select group of MS individuals.
Conclusion
UVB phototherapy corrects vitamin D deficiency. This study adds to the growing research investigating UVB treatment in MS.
Author Contributions
Academic Editor: Sidharth Mehan, Associate Professor, Department of Pharmacology, ISF College of Pharmacy (ISFCP), Ghal Kalan, Ferozpur G.T. Road, Moga-42001, Punjab, India
Checked for plagiarism: Yes
Review by: Single-blind
Copyright 2019 Robert W. Motl, et al.
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
This study was funded by a grant from Sun Health Technologies. BJR is the chief scientific officer for Sun Health Technologies, and the University of Illinois created a conflict management plan for minimizing bias and undue influence in running the trial and interpreting the data. This was necessary as BJR was the study neurologist. The funding source did not play any role in the writing of the manuscript and the decision to submit the manuscript for publication.
Citation:
Introduction
Multiple sclerosis (MS) is an incurable debilitating autoimmune disorder. It is the most common nontraumatic chronic degenerative disease of the central nervous system (CNS). The worldwide MS prevalence, approximately 2.4 million people, follows an established geographic gradient that directly correlates with latitude and decreased sunlight intensity.1 The lowest incidence of MS occurs in equatorial regions, and the highest MS prevalence areas occur in temperate regions with low levels of sunlight exposure including: Canada, Northern parts of the US, Northern Europe, Southeastern Australia and Southern New Zealand.The regional MS prevalence distribution led to the early speculation that reduced sunlight exposure, or the subsequent reduction in vitamin D production, is responsible in part for MS disease incidence and activity.2,3,4 Numerous epidemiological and preclinical studies have demonstrated associations between the risk of MS development and a worsening of MS severity, with reduced sunlight. 4,5 Likewise, vitamin D insufficiency ((25 hydroxyvitamin D (25(OH)D) values between 40-70 nmol/L) and Vitamin D deficiency (25(OH)D values less than 40 nmol/L) have been associated with an increased risk of MS, and with a worsening of MS manifestations and clinical course. 3,6,7,8,9,10Conversely, there is evidence that sunlight suppresses MS through induced 25(OH)D production. Independent studies show that high levels of vitamin D, or vitamin D adequacy (25(OH)D values greater than 70 nmol/L), is linked with a reduced risk of developing MS, a reduced number of lesions on MRI and a reduced risk of MS relapse.10,11
Vitamin D is a series of secosteroids obtained primarily through skin exposure to ultraviolet B radiation (UVB, 280-315 nm) from sunlight, and through both animal and vegetable dietary sources. The circulating 25(OH)D form of the hormone represents the principle vitamin D reservoir and is used as an indicator of overall vitamin D status. The primary approach for changing 25(OH)D levels in MS has involved supplementation with standard over-the-counter vitamin D preparations.12,13 Existing supplementation studies have not been universally successful in raising 25(OH)D levels or in changing MS outcomes.12,13,14 The lack of conclusive findings may be related to the uncertainty regarding an optimal supplementation treatment dose, variations in supplementation compliance, as well as differences in individual absorption and metabolism, laboratory techniques and value reporting, or other unknown factors.8,10 A more recent and alternative approach for increasing 25(OH)D involves the delivery of ultraviolet B irradiation (UVB) using phototherapy.15
Sunlight may suppress MS through a 25(OH)D independent mechanism as well. More recent investigations into the inverse relationship between MS incidence and sunlight exposure led to the discovery that a narrow band of light (300–315 nm) prevents experimental autoimmune encephalomyelitis (EAE), which is the animal model of MS, without a change in 25(OH)D levels. 16,17 This finding led to human clinical trials designed to examine the possible use of this narrow band UVB light (NB-UVB) as a treatment to stop the conversion or progression of MS, as well as to explore the mechanisms of action of the narrow band light. 17,18Patients with relapsing-remitting MS (RRMS) treated with NB-UVB had an attenuated systemic immune response accompanied with elevated serum vitamin D levels.17 The phototherapy for clinically isolated syndrome (CIS) trial (PhoCIS trial) found that 12 months of NB- UVB treatment given to CIS patients resulted in a halt or delay in MS conversion in 30% of the NB-UVB study participants as compared to 100% conversion from CIS to MS in the no phototherapy group.CIS is a condition which includes an episode of neurological symptoms caused by CNS inflammation or demyelination that does not fulfil the diagnostic criteria for MS). 18
The purpose of this study is to evaluate the effects of UVB phototherapy (UVB lamp radiation; 300nm - 311 nm) on serum 25(OH)D levels, immune modulation and clinical benefit. We sought to determine whether UVB phototherapy increases 25(OH)D levels in individuals with MS, and we aimed to investigate whether UVB phototherapy effects circulating immunomodulatory cells or MS symptomology. We chose to investigate immunomodulatory cells, because MS is described broadly as being mediated by activated T-cell and B-cell lymphocytes, and because CNS inflammation is induced through myelin reactive T cells from the peripheral immune system.
Current MS therapies include targeting the destruction, depletion, or suppression of these autoreactive circulating T and B cell lymphocyte populations.19 Regulatory T cells (Tregs) limit self-reactive cells, and thus have emerged as key immune modulators, capable of suppressing pathological autoimmune disease, through their maintenance of peripheral immune tolerance. UVB irradiation has been shown to induce the expansion of Treg cells for up to 2 weeks.20 It is thought that MS results from a disturbance in systemic tolerance mechanisms involving Tregs.19,20,21,22,23,24 Tregs prevent the expansion of self-tissue antigens including those directed against myelin determinants. Treg numbers have been shown to be reduced in individuals with MS, and the number of Treg cells were reported to be lower in severe MS forms (Secondary progressive MS (SPMS), Primary progressive MS (PPMS), and Secondary progressive MS (PRMS)), as compared to the mild forms (CIS and RRMS).21,23 Thus, boosting Treg cell number, function and migration may prove to be a beneficial MS therapeutic strategy.19
Methods
Study Design and Participants
We performed a single center, triple-blind, randomized placebo-controlled, pilot trial. The study was registered with ClinicalTrials.gov, NCT02365259. The study protocol and ethics were approved by the University of Illinois at Urbana-Champaign (UIUC) Institutional Review Board (IRB). All participants provided written informed consent. Participant screening was undertaken over the telephone by the project coordinator, and participants were not enrolled until after receiving verification of inclusion and exclusion criteria status, and approval for participation by the study neurologist.
Community-residing women and men 18 years of age or older, with relapsing MS, who did not have any of the following exclusion criteria: (a) inability to stand still in a stabilized fashion without risk of falling for up to 6 minutes; (b) medical history of calcium disorder or knowledge of high calcium levels; (c) medical history of hyperparathyroidism; (d) current supplementation with oral vitamin D; (e) allergy to vitamin D; (f) history of cancer of any type including but not limited to skin cancer; (g) obesity defined as body mass index > 30; (h) history of fat malabsorption conditions (i.e., steatorrhea); (i) current use of anti-epileptic medication; (j) current use of glucocorticoids; (k) Fitzpatrick skin types I and VI; and (l) current use of tanning facilities, were recruited into the study. The study subjects were diagnosed with relapsing-remitting MS (RRMS) according to the McDonald criteria. 25
Randomization and Masking
One randomization event occurred during the study. Study enrollees underwent baseline testing, and were randomized into an intervention condition (UVB phototherapy or Placebo control) by a computer-generated random sequence using standard methods. The final sample completing the study included 12 persons with MS who were evenly distributed between treatment conditions. The study participants, site personnel and clinical neurologist involved in the study were masked to the results of randomization. The University of Illinois created a conflict management plan for monitoring and minimizing bias and undue influence in running the trial and interpreting the data. The study phototherapy technician responsible for administering the intervention treatment was the only person aware of the intervention assignments.
Procedures
Serum 25(OH)D level, circulating progenitor, monocyte subsets, andTreg numerical status, walking performance, hand-grip strength, cognitive function and mood were assessed at baseline, 4 weeks and again at 8 weeks after beginning the UVB phototherapy or placebo-controlled intervention. The UVB intervention condition consisted of an individualized regimen. Each sub-minimal erythema dose (10-30kJ/m2) of UVB (Sun Health FS UVB 298-313 nm, 40WT10) phototherapy delivered was based on skin sensitivity, and took into consideration subject Fitzpatrick skin type classification per the 2014 guidelines issued by the American Academy of Dermatology (AAD).26 The regimen was pilot tested for safety, standardized and manualized for reproducibility. UVB phototherapy was delivered 3 times per week over the 8-week period with a minimum of 24 hours between exposures. The placebo-controlled condition (sham light) was identical in every component as the intervention, except that participants were exposed to non-UVB florescent light (Philips 40WT, alto supreme T12, 4100K). The subjects received the phototherapy or placebo light irradiation to the back, chest, arms and legs through standup medical devices. The study occurred during the winter in order to avoid confounding the results by varied daytime sunlight exposure. Study participants were also asked not to undertake additional sun or light exposure (i.e., not visit a tanning facility) over the duration of the study, and they were asked to wear protective covering (e.g., hat, long sleeve shirt, and pants) during the hours of 10:00-14:00 daily.
Venous blood was collected from an antecubital vein after an overnight fast at the same time of day for all assessments to quantify 25(OH)D levels. Blood was allowed to clot in serum tubes (BD Vacutainer: Franklin Lakes, NJ) for 60 min at room temperature, then serum was separated by centrifugation at 1300 × g for 15 minutes. Serum was aliquoted and stored at −80OC until analysis. 25(OH)D concentrations were quantified in serum by a standard protocol, and based on the manufacturer’s instructions (Immunodiagnostic Systems, United Kingdom). All samples were analyzed in triplicate, and 25(OH)D concentrations were expressed as nmol/L.
Circulating progenitor cells (CPCs: CD34+CD45dim), monocyte populations (Intermediate CD14+CD16−, Classical CD14+CD16+), and Tregs (CD4+/CD25+/FoxP3+Tregs) were isolated and purified from peripheral blood, stained with FITC- or PE-conjugated antihuman monoclonal antibodies (mAbs), in conjunction with anti-human FoxP3 for the enumeration of Treg cells, and quantified by flow cytometry. PE conjugated monoclonal CD34 (BI-3C5), FITC conjugated monoclonal CD45 (HI30), PE conjugated Monoclonal CD14 (TuK4), and FITC conjugated monoclonal CD16 (3G8) mAbs were used; all antibodies were purchased from Invitrogen (Grand Island, NY). Peripheral blood lymphocytes were stained with BioLegend’s True-Nuclear™ Human Treg Flow™ Kit (FOXP3 Alexa Fluor® 488/CD4 PE Cy5/CD25 PE) and were isolated by AutoMACS cell sorter (Miltenyi Biotec). All flow cytometry analysis was performed on a FACSCalibur (BD Biosciences) with BD CellQuest analysis software.
Walking performance was measured using the Timed 25 Foot Walk (T25FW). The protocol involved two trials of walking 25-feet as fast, but safely, as possible. We expressed T25FW performance as ft/sec based on an average of the two trials. This study included a measure of hand-grip strength, wherein participants were asked to squeeze a hand dynamometer (Jamar Hydraulic Hand Dynamometer, Lafayette Instruments, Lafayette, IN) as hard as possible. Participants were given 3 trials per hand with a 1-minute rest between trials, and the highest recorded value was taken as maximal grip strength (kg). Cognitive function was assessed using the Brief International Cognitive Assessment for Multiple Sclerosis (BICAMS) battery (Langdon DW, 2012) that includes the oral version of the Symbol Digit Modalities Test (SDMT), the California Verbal Learning Test-II (CVLT-II) and the revised Brief Visuospatial Memory Test (BVMT-R). The SDMT is a timed thinking task that involves associating numbers with symbols; the range of scores is 0-110. The CVLT-II is a test of verbal memory and involves recalling a list of 16 words read aloud by the examiner; the range of scores is 0-90. The BVMT-R is a test of visual memory that involves recalling and manually drawing a series of 6 abstract designs; the range of scores is 0-36. Mood was measured by the 30-item version of the Profile of Mood States (POMS) using a seven-day response set for capturing mood during the past week. We expressed the POMS score by summing the items into Total Mood Disturbance (TMD; 0-80) with lower scores reflected a better overall mood state.
All outcome assessments, data processing and analysis were conducted in a blinded fashion. Participants received remuneration for completing the measurements and for completion of the intervention sessions. Safety and adverse events were assessed at each visit by the study coordinator and were monitored monthly by the UIUC IRB committee.
Statistical Analysis
Data were analyzed using SPSS version 24.0. Results are reported as mean and standard deviation (SD), unless otherwise noted (e.g., percentages, frequencies, medians). We compared initial differences between conditions using independent samples t-tests and chi-square analyses. We compared changes in outcomes over time between conditions based on a mixed-factor, 2-way analysis of variance (ANOVA). Time was a within-subjects factor, whereas condition was a between-subjects factor. We expressed the magnitude of effects as partial eta-squared (η2) and Cohen’s d. All participants who received UVB or placebo were included in the study and safety analysis.
Results
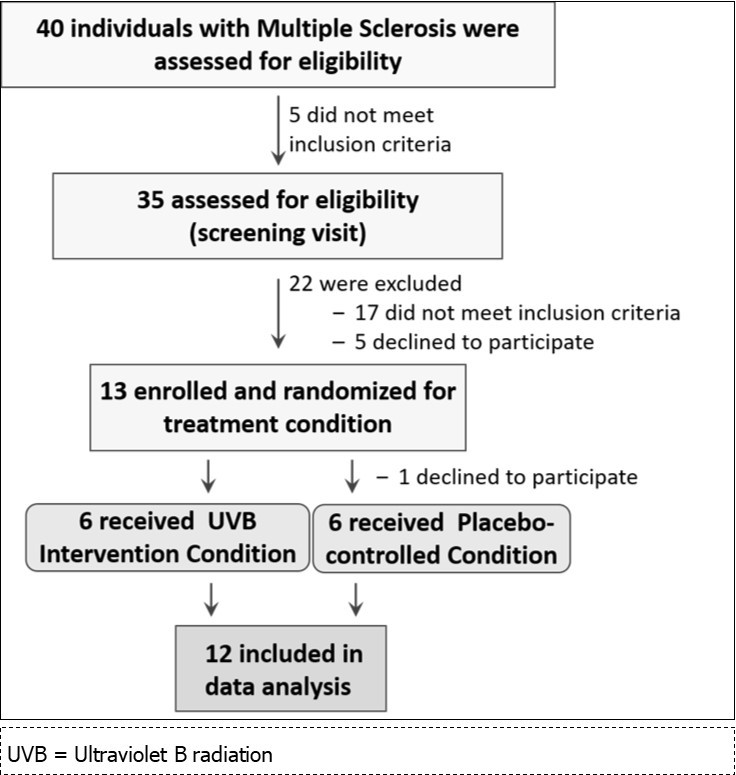
We contacted 40 individuals with relapsing MS about the study, and 35 underwent screening for inclusion. Of these 35 individuals, 18 satisfied inclusion criteria, and 17 were enrolled and scheduled for baseline testing. There were 4 individuals who subsequently withdrew. The remaining 13 individuals underwent baseline testing and were randomized into an intervention condition (UVB phototherapy or placebo control). One person randomized into the phototherapy condition withdrew because of a family event. The final sample completing the study included 12 subjects with relapsing MS who were evenly distributed between treatment conditions (i.e., UVB Intervention, n=6; placebo-controlled condition, n=6); see the trial profile in Figure 1.
The descriptive characteristics of the study participants are provided in Table 1. There were no significant differences between conditions in age, height, weight, or sex, based on independent samples t-tests. All subjects in this study had relapsing MS- that is they were being treated for the occurrence of new symptoms or the worsening of old symptoms. All subjects were on disease modifying therapy. These included glatiramir acetate (Copaxone), interferon beta-1b (Betaseron, Extavia), natalizumab (Tysabri), and fingolimod (Gilenya).
Table 1. Descriptive characteristics per condition of random assignment.| Characteristic | UVB-Intervention Condition (n=6) | Placebo-Controlled Condition (n=6) | Test Statistic | p-value | |
| Age (yr) | 49.2 (14.8) | 55.0 (9.6) | t=0.81 | .44 | |
| Height (cm) | 167.1 (6.5) | 164.8 (6.8) | t=0.58 | .57 | |
| Weight (kg) | 70.0 (18.3) | 76.3 (17.7) | t=0.61 | .56 | |
| Sex (n/% female) | 5/83% | 6/100% | χ2=1.09 | .30 | |
| Skin type (n/%) | |||||
| II | 1/17% | 0/0% | χ2=2.14 | .34 | |
| III | 1/17% | 3/50% | |||
| IV | 4/66% | 3/50% | |||
| Assistive Device (n/% none) | 6/100% | 5/83% | χ2=1.09 | .30 |
The groups did not differ in skin type nor use of an assistive device for ambulation based on chi-square tests. Pre-study blood draws revealed that 25% of our study subjects were vitamin D deficient, 25% were vitamin D insufficient, and 50% had adequate vitamin D values. Vitamin D deficiency, insufficiency and adequate vitamin D was defined as 25(OH)D values less than 40 nmol/L, 25(OH)D values falling between 40-70 nmol/L and 25(OH)D values greater than 70nmol/L, respectively.At the completion of the study, 100% of the UVB intervention study subjects had adequate vitamin D levels as compared to only 50% of the placebo condition subjects. (see Table 2).
Table 2. Vitamin D Status| Total Study Subjects | UVB Intervention Condition | Placebo Controlled Condition | |||||||
| Vitamin D Level | Pre | Mid | Post | Pre | Mid | Post | Pre | Mid | Post |
| Adequate (>70 nmol/L) | 50% | 58% | 67% | 33% | 67% | 100% | 67% | 50% | 50% |
| Insufficient (40-70 nmol/L) | 25% | 25% | 17% | 50% | 33% | 0% | 0% | 17% | 17% |
| Deficient (<40 nmol/L) | 25% | 17% | 17% | 17% | 0% | 0% | 33% | 33% | 33% |
The mixed-factor ANOVA identified a statistically significant condition by time interaction on serum vitamin D levels (F=7.14, p<.005, partial η2=.42). The UVB intervention condition had an increase in serum vitamin D levels over time, whereas there was no change for the placebo-controlled or sham condition; see Figure 2. The effect size for the change from pre- to mid-testing with the intervention condition was moderate in magnitude (d=0.64), and was large in magnitude (d=1.05) from pre- to post-testing. The condition by time interaction accounted for 42% of the variance in serum 25(OH)D levels.
Figure 2.Time by condition interaction of serum vitamin D levels. Values are mean scores (standard deviation). Intervention Condition referes to the UVB phototherapy, and Placebo-Controlled Condition refers to the florescent light condition. The increase in mean vitamin D concentration from Pre, Mid to Post UVB intervention was stastistically different from the vitamin d values observed in the Placebo contolled condition over the duration of the study from Pre, to mid to post intervention; p< 0.05.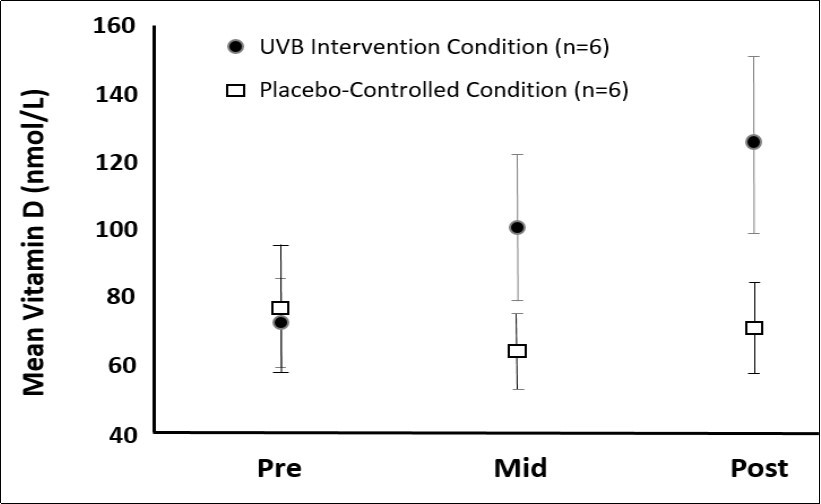
The descriptive and inferential statistics for the primary and secondary outcomes are provided in Table 2, Table 3 and Table 4, respectively. The mixed-factor ANOVAs for secondary outcomes did not identify statistically significant condition by time interactions on any variable. There was a significant time main effect for revised Brief Visuospatial Memory Test (BVMT-R) scores (F=7.52, p<.005, partial η2=.43). This time main effect indicates an improvement in BVMT-R scores over time for both treatment conditions (i.e., no treatment effect) and likely reflects a practice effect following the tests repeated administration. CPC, classical monocyte, intermediate monocyte, and Treg numerical status were not found to be correlated with treatment or 25(OH)D level as shown in Table 4and Table 5
Table 3. Descriptive statistics for outcome variables| Outcomes | Variable | UVB Intervention Condition (n=6) | Placebo-Controlled Condition (n=6) | ||||
| Pre | Mid | Post | Pre | Mid | Post | ||
| Primary | Vitamin D (nmol/L) | 71.7 (37.9) | 100.4 (51.6) | 124.7 (63.1) | 76.5 (41.1) | 62.5 (26.8) | 70.1 (34.7) |
| Secondary | T25FW (ft/sec) | 5.2 (1.3) | 5.3 (1.3) | 5.5 (1.3) | 4.6 (2.5) | 5.4 (2.6) | 5.0 (2.6) |
| Strength (kg) | 33.8 (14.7) | 33.5 (11.3) | 32.3 (9.8) | 29.2 (6.2) | 28.0 (8.6) | 25.8 (6.5) | |
| SDMT (0-110) | 55.0 (22.1) | 59.0 (23.7) | 54.0 (13.9) | 54.5 (14.1) | 57.7 (13.5) | 57.7 (12.7) | |
| CVLT (0-90) | 60.3 (7.6) | 55.2 (10.9) | 60.0 (4.7) | 54.3 (9.8) | 57.3 (8.8) | 58.3 (14.1) | |
| BVMT-R (0-36) | 21.9 (7.4) | 25.7 (4.5) | 29.2 (4.7) | 19.2 (7.9) | 19.3 (6.5) | 23.8 (7.6) | |
| TMD (0-80) | 36.5 (12.2) | 30.0 (15.1) | 32.0 (14.5) | 32.3 (6.9) | 25.0 (10.7) | 26.7 (12.7) | |
| Outcomes | Variable | Time | Condition | Time by Condition | |||
| F-value | p-value | F-value | p-value | F-value | p-value | ||
| Primary | Vitamin D | 4.32 | <.05 | 1.52 | .25 | 7.14 | <.005 |
| Secondary | T25FW | 2.57 | .10 | 0.13 | .73 | 0.21 | .81 |
| Strength | 2.55 | .10 | 0.98 | .35 | 0.35 | .71 | |
| SDMT | 1.49 | .26 | .01 | .95 | 0.78 | .47 | |
| CVLT | 0.73 | .50 | .14 | .71 | 1.39 | .27 | |
| BVMT-R | 7.52 | <.005 | 2.05 | .18 | 0.72 | .50 | |
| TMD | 2.39 | .12 | 0.65 | .44 | 0.02 | .98 | |
| UVB Intervention Condition (n=6) | Placebo-Controlled Condition (n=6) | |||
| Variable | Pre | Post | Pre | Post |
| Circulating progenitor cells(CD34+/CD45dim) | 0.17(0.13) | 0.17(0.12) | 0.11(0.05) | 0.28(0.34) |
| Intermediate Inflammatory monocytes (CD14+/CD16+) | 1.07(0.63) | 1.58(0.68) | 1.83(1.66) | 1.83(1.73) |
| Classical Phagocytic monocytes (CD14+/CD16-) | 2.98(1.41) | 5.66(3.46) | 4.02(3.04) | 4.05(4.28) |
| Regulatory T cells -Tregs (CD4+/CD25+/FoxP3+) | 5.54(3.74) | 8.52(4.89) | 9.79(6.15) | 9.73(4.84) |
Individual longitudinal changes in classical monocyte and Treg numerical status profiles appear different between the UVB treated subjects versus the placebo control group. For subjects 1, 3 and 6 a profile of increased intermediate monocyte, classical monocyte and Treg numerical status following UVB intervention occurred. The differences however, are not statistically significant, and the changes are not uniform across all UVB - treated subjects see Figure 3 and Figure 4.
Figure 3.Individual subject changes in Circulating Progenitor Cells (CPCs, CD34+/CD45dim), Intermediate monocytes (Inflamatory, CD14+/CD16+), Classical monocytes (Phagocytic CD14+/CD16-) and Regulatory T cells (Tregs, , CD14+/cd25+/FoxP3+). Filled black circles are individual Pre-intervention values and the white filled circles are the corresponding Post-intervention values for the 12 study subjects.
Figure 4.Individual longitudinal immune cell changes in the NB-UVB treated group (study subjects 1-6), versus the placebo control group (study subjects 7-12). Grey bars are Circulating Progenitor Cells, CPCs. Black bars are Intermediate Monocytes. White bars are Classical Monocytes. Black and white patterned bars are Regulatory T cells (Tregs).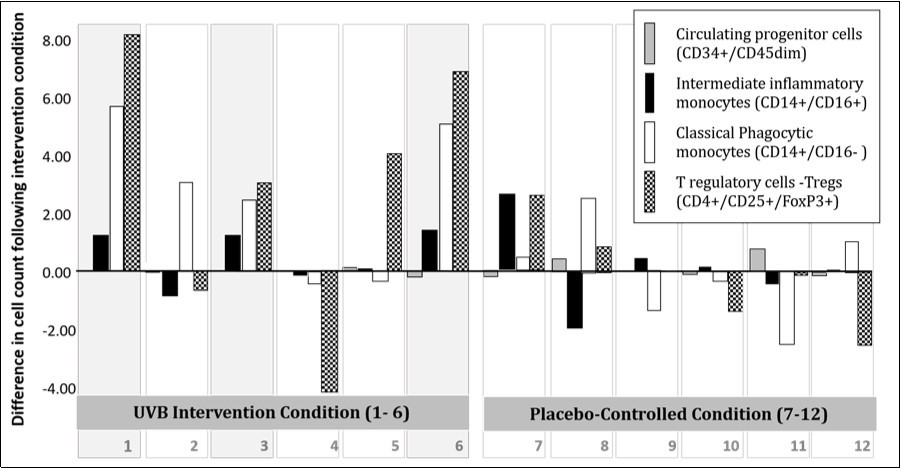
Discussion
Although this study was unable to show significant UVB-induced MS immunoregulation or neurological improvement over the duration of the study, we do report some compelling observations. The UVB phototherapy condition, unlike the placebo-controlled condition, resulted in a statistically significant increase in serum 25(OH)D levels over the course of the 8-week trial. And while the changes in CPC, classical and intermediate monocyte and Treg cell counts following UVB intervention were not significantly different from those observed in the placebo control group, individual Treg cell profile changes following UVB light treatment, including a marked increase in Treg counts in 4/6 UVB treated individuals versus 1/6 of the placebo treated subjects was noted. This may reflect subject response variability and warrants further investigation. The trend towards an increase in Tregs in this population following UVB treatment represents an exploitable therapeutic potential given that Tregs play a critical role in the active suppression of autoimmunity. MS patients have been found to have lower circulating Treg cell numbers compared to healthy controls, 21,22,23 and Treg numeric and functional deficiencies have been shown to play a pathogenic role in inflammatory demyelinating CNS disorders. 21,24
The observed variations in classical monocyte levels relative to alterations in intermediate monocyte levels may also indicate differences in disease duration, activity, or recovery. Classical monocytes are thought to primarily play a phagocytic role, whilst intermediate monocytes are thought to be associated with an inflammatory response. An increase in intermediate monocytes could be a differentiating factor between acute and chronic inflammation.27 It is unclear whether the observed increase in Treg and classical phagocytic monocyte number in a subset of the individuals is a cause or consequence of the disease status, or whether it is related to disease duration or medication differences among the study subjects. Subjects 1, 3 and 6 share a common increase in intermediate and classical monocyte, and Treg numerical status following UVB treatment which is distinct from the other study subjects. There were no UVB phototherapy associated clinical benefits. Cautious interpretation of these results is warranted because the patients were on different immunosuppressive therapies and duration of disease was not adjusted for.
These results complement and extend those reported in a previous study of UVB persons with MS. 27 Our study design is different from the previous study in that we included a placebo-controlled sham device, as well as treatment- and data-blinded assessors. Collectively, the UVB phototherapy trials show that we can correct vitamin D deficiency within 8 weeks. A longer study duration is likely to be necessary for improved clinical outcomes to become apparent.
The limitations of the current pilot RCT include the small sample size, the short time course of the study, and the fact that the participants in our study were not all vitamin D deficient at baseline. Additionally, we did not consider disease duration or concurrent therapeutic interventions (medication) in our analysis. These factors did not preclude the demonstration of an intervention effect on serum vitamin D, but undermined our capacity to confidently interpret the UVB-induced changes in CPC, intermediate and classical monocyte, and Treg cell populations, and likely limited our ability to detect differences in secondary clinical end-points. Clinical benefits of UVB phototherapy may be more pronounced in patients with MS that have had a history of chronic vitamin D deficiency. This is important considering the evidence for vitamin D insufficiency and deficiency in MS, 6 combined with the association between serum vitamin D deficiency and both the increased risk of MS and worsening clinical course and MS symptomology, as reflected by radiologic and clinical outcomes over time.6,9,11,28,31,32
Our observations have potential therapeutic implications, as the observed immunopathological heterogeneity in MS is likely to be both patient- and context-dependent, and may reflect either different host genetic factors that define different immune-mediated inflammatory responses, and the subsequent susceptibility to neuronal injury, or distinct triggers, respectively.29 We expect that the degree of disease chronicity, concomitant illnesses, therapeutics, and individual-specific disease modifying factors, such as: weight; overall health; and prior immunogenic exposures, effect circulating immune cell profiles as well as overall clinical outcome. Variable responses of MS patients to UVB immunomodulatory therapies may also relate, in part, to differences in repair processes or the underlying effector mechanisms mediating disease. These observations have potentially significant implications for individualized MS therapeutic approaches.
Given the report that the prevalence of MS in the US has been on a steady rise over the past 5 decades 30, and because there is currently no curative FDA-approved therapy for MS, novel clinical strategies for the management of MS are needed. In a subset of MS patients, UVB phototherapy may shorten the duration of acute MS exacerbations, decrease relapse frequency and provide symptomatic relief by providing neuroprotection mediated through a decreased autoimmune responsivity mechanism. UVB phototherapy, as a Treg augmentation therapy, may confer immune directed neuroprotective prophylaxis, and may provide therapeutic benefit in MS.
The results presented in this study support the need for larger UVB phototherapy trials of longer duration to further investigate the Treg inductive capability of UVB radiation. In the future, we hope to evaluate UVB –induced immune profile changes, and their relative impact on MS disease course and relapse rate, in relation to vitamin D status. The individual longitudinal changes in the monocyte and Treg numerical status following UVB phototherapy shown here, highlight the necessity of individualized MS therapeutics, and the need for sophisticated computational strategies to aid in complex multivariable patient data analysis. Interventional studies designed to determine whether UVB phototherapy results in immunomodulation and subsequent amelioration of MS disease activity are justified.
We do not advocate chronic excessive sunlight exposure as a MS therapy, because of the associated increased risk of nonmelanoma skin cancer. We do however, support the recommendation for sensible sun exposure, as defined as 5-10 minutes of exposure of the arms, hands, legs and face 2 to 3 times per week, and increased dietary and supplementation of vitamin D intake to help ensure vitamin D sufficiency. This is particularly important in the context of the growing concern about vitamin D deficiency being an unrecognized epidemic among both children and adults in the US.7
Conclusion
The results of this pilot trial indicate that UVB phototherapy represents a novel, safe, inexpensive and effective, nonpharmacological approach to increasing vitamin D levels in MS. UVB phototherapy corrects vitamin D deficiency. At the completion of the study, 100% of the UVB treated condition subjects had adequate vitamin D levels as compared to only 50% of the subjects in the placebo controlled condition (see Table 2). Vitamin D’s pleiotropic effects on health and role in the immune response suggest that UVB phototherapy may be a successful component in combatting MS. Using UVB phototherapy, as an add-on therapy in this still incurable disorder, may offer a therapeutic approach to control autoimmune inflammation and MS relapse and progression. Based on our findings, and in the context of a growing literature that supports the hypothesis that UVB induces neuroprotection in MS through immunomodulation, larger and longer duration UVB phototherapy studies in MS that consider the multifactorial intrinsic and extrinsic disease modifying factors are warranted. Given that MS is a remarkably heterogeneous condition, future studies should attempt to identify the specific subpopulation of patients most likely to benefit from UVB phototherapy. UVB phototherapy may need to be initiated in early stage MS to confer protection against, or resilience towards, the autoimmune response responsible for CNS injury in MS. This study, like the previous NB-UVB MS clinical trials, provides encouragement to other investigators to conduct larger scale UVB phototherapy studies designed specifically to investigate the potential MS disease modifying effects of UVB phototherapy.
Contributors
RM and CBP wrote the paper. BJR, BP, GN, MDL, SS and RM conducted the research. RM and CBP conducted the data analysis.
Declaration of Interests
This study was funded by a grant from Sun Health Technologies. BJR, the studies neurologist is also the chief scientific officer for Sun Health Technologies. Thus, the University of Illinois created a conflict management plan for minimizing bias and undue influence in the running of the trial and data interpretation by triple blinding the study, and by restricting control of the study and access to the data to the University of Illinois primary investigator. The funding source aims to develop propriety phototherapy devices. The company did not play any (italics was added for emphasis) role in the study design, the writing of the manuscript, or in the decision to submit the manuscript for publication.
Author Contributions
RM and CBP wrote the paper. BJR, BP, GN, MDL, SS and RM conducted the research. RM and CBP conducted the data analysis.
Funding
Sun Health Technologies
Acknowledgements
This study was supported by a grant from Sun Health Technologies
References
- 1.Simpson S, Blizzard L, Otahal P. (2011) Latitude is significantly associated with the prevalence of multiple sclerosis: a meta-analysis.JNeurolNeurosurgPsychiatry.82:. 1132-1141.
- 2.Summerday N M, Brown S J, Allington D R, Rivey M P. (2012) Vitamin D and Multiple Sclerosis Review of a Possible Association.Journal of pharmacy practice. 25(1), 75-84.
- 3.Munger K L, Levin L I, Hollis B W, Howard N S, Ascherio A. (2006) . Serum 25-Hydroxyvitamin D Levels and Risk of Multiple Sclerosis.JAMA 296(23), 2832-2838.
- 4.Beretich B D, Beretich T M. (2009) Explaining multiple sclerosis prevalence by ultraviolet exposure: a geospatial analysis.MultScler.15:. 891-898.
- 5.Lucas R M, Ponsonby A L, Dear K Sun. (2011) exposure and vitamin D are independent risk factors for CNS demyelinationNeurology76:. 540-548.
- 6.Shahbeigi S, Pakdaman H, Fereshtehnejad S-M, Nikravesh E, Mirabi N et al. (2013) . Vitamin D3Concentration Correlates with the Severity of Multiple Sclerosis.International Journal of Preventive Medicine 4(5), 585-591.
- 7.Holick M F. (2004) Sunlight and vitamin D for bone health and prevention of autoimmune diseases, cancers, and cardiovascular disease,The American Journal of Clinical Nutrition. 80(6), 1678-1688.
- 8.Mowry E M. (2011) Vitamin D: Evidence for its role as a prognostic factor in multiple sclerosis. , J Neurol Sci 311, 19-22.
- 9.Pierrot-Deseilligny C, Rivaud-Pechoux S, PR de Paz Clerson, Souberbielle J C. (2012) Relationship between 25-OH-D serum level and relapse rate in multiple sclerosis patients before and after vitamin D supplementation,TherAdvNeurolDisord. 5(4), 187-98.
- 10.Manousaki D, Richards J B. (2019) Vitamin D deficiency is an etiological factor for MS-YesMultiple Sclerosis Journal. 25(5), 637-638.
- 11.Ascherio A, Ascherio A, Munger K L, White R. (2014) Vitamin D as an early predictor of multiple sclerosis activity and progression.JAMA Neurol.71(3):. 306-314.
- 12.James E, Dobson R, Kuhle J. (2013) The effect of vitamin D-related interventions on multiple sclerosis relapses: A meta-analysis.MultiScler.19:. 1571-1579.
- 13.Kampman M T, Steffensen L H, Mellgren S I, Jørgensen L. (2012) Effect of vitamin D3 supplementation on relapses, disease progression, and measures of function in persons with multiple sclerosis: exploratory outcomes from a double-blind randomized controlled trial.MultScler.18:. 1144-1151.
- 14.Pozuelo-Moyano B, Benito-Leon J, Mitchell A J, Hernandez-Gallego J. (2013) A systematic review of randomized, double-blind, placebo-controlled trials examining the clinical efficacy of vitamin D in multiple sclerosis.Neuroepidemiology. 40, 147-153.
- 15.Ala-Houhala M J, Vahavihu K, Hasan T. (2012) Comparison of narrowband ultraviolet B exposure and oral vitamin D substitution on serum 25-hydroxyvitamin D concentration.Br. , J Dermatol 167, 160-4.
- 16.Wang Y, Marling S J, Beaver E F.(2015).UV light selectively inhibits spinal cord inflammationanddemyelinationinexperimental autoimmune encephalomyelitis.ArchBiochemBiophys,567:. 75-82.
- 17.Breuer J N, Schwab T, Schneider-Hohendorf M. (2014) Ultraviolet B light attenuates the systemic immune response in central nervous system autoimmunity.Ann. Neurol.75: 739-758.
- 18.Hart P H, Lucas R M, Booth D R. (2017) Narrowband UVB Phototherapy for Clinically Isolated Syndrome: A Trial to Deliver the Benefits of Vitamin D and Other UVB-Induced Molecules.Frontiers inImmunology. 8, 3.
- 19.Danikowski K M, Jayaraman S, Prabhakar B S. (2017) Regulatory T cells in multiple sclerosis and myasthenia gravis.Journal of neuroinflammation. 14-17.
- 20.Yamazaki S, Nishioka A, Kasuya S. (2014) . Homeostasis of Thymus-Derived Foxp3+ Regulatory T Cells Is Controlled by Ultraviolet B Exposure in the Skin.J Immunol,193(11): 5488-97.
- 21.Kouchaki E, Salehi M, Reza M, Nikoueinejad H, Akbari H. (2014) . Numerical status of CD4+CD25+FoxP3+ and CD8+CD28- regulatory T cells in multiple sclerosisIran J Basic Med Sci,17: 250-255.
- 22.Venken K, Hellings N, Thewissen M. (2008) Compromised CD4+ CD25(high) regulatory T-cell function in patients with relapsing-remitting multiple sclerosis is correlated with a reduced frequency of FOXP3-positive cells and reduced FOXP3 expression at the single-cell level.Immunology;. 123(1), 79-89.
- 23.Haas J, Hug A, Viehöver A.(2005).Reduced suppressive effect of CD4+CD25highregulatory T cells on the T cell immune response against myelin oligodendrocyte glycoprotein in patients with multiple sclerosis.Eur. , J. Immunol; 35, 3343-3352.
- 24.Viglietta V, Baecher-Allan C, Weiner H L. (2004) Loss of functional suppression by CD4+CD25+regulatory T cells in patients with multiple sclerosis. , J. Exp. Med,199: 971-979.
- 25.Polman C H.Reingold SC, Edan G et al.(2005).“Diagnostic criteria for Multiple Sclerosis: revisions to the McDonald Criteria”.Ann Neurol,58:. 840-846.
- 26.Sidbury R, David D M, Cohen D E. (2014) American Academy of Dermatology. Guidelines of care for the management of atopic dermatitis: Section 3. Management and treatment with phototherapy and systemic agents. , J AmAcadDermatol 71, 327-349.
- 27.Mukherjee R, Barman P K, Thatoi P K. (2015) Non-Classical monocytes display inflammatory features:. Validation in Sepsis and Systemic Lupus Erythematous.SciReports,5: 13866.
- 28.Brola W, Sobolewski P, Szczuchniak W. (2016) Association of seasonal serum 25-hydroxyvitamin D levels with disability and relapses in relapsing-remitting multiple sclerosis.EJCN. , European Journal of Clinical Nutrition,70 995-999.
- 29.Metz I, Weigand S D, BFG Popescu. (2014) Pathologic Heterogeneity Persists in Early Active Multiple Sclerosis Lesions.Annals of neurology. 75(5), 728-738.
- 30.Wallin M T, Culpepper W J, Campbell J D. (2019) . The prevalence of MS in the United StatesNeurologyMar 92(10), 1029-1040.
Cited by (2)
This article has been cited by 2 scholarly works according to:
Citing Articles:
Photochemical & Photobiological Sciences (2025) OpenAlex
Photochemical & Photobiological Sciences (2025) Crossref
Uwe Riedmann, Chris Dibben, F. D. de Gruijl, S. Gorman, Prue H Hart et al. - Photochemical and Photobiological Sciences (2025) Semantic Scholar