Uptake of Breast Screening Among Female Staff at A Tertiary Health Institution in South-West Nigeria
Abstract
Background
Breast cancer is one of the most common types of cancer affecting women globally. It has shown increasing morbidity and mortality rates over the past years. Several screening methods ranging from simple breast self-examination to a highly sensitive test procedures for early detection and treatment are available, but uptake is a challenge. Lack of a national screening programme in the country makes available regional screening programme unsuccessful. This study aims to assess the factors affecting the uptake of breast cancer screening programme among female staff in a tertiary hospital, Southwest Nigeria.
Method
This descriptive cross-sectional study involves 375 participants selected by a stratified random sampling technique, with proportional allocation to population size and the use of a semi-structured questionnaire. Respondents were questioned on their basic knowledge of breast cancer symptoms, risk factors and treatment, over a score of 50 and above, were set as the cut-off mark to determine good knowledge of breast cancer. Patients attitudes towards breast cancer screening as well as factors affecting uptake were also measured. Descriptive statistical analysis was done using SPSS-20 while the predictors of the uptake of screening were determined using logistic regression at p ≤ 0.05.
Results
There were 360 respondents, comprising of 13.3% clinical and 86.7% non-clinical female staff within the age bracket of 20 to 58 years (38.2±0.42 years). Out of the respondents, 97.8% have heard about breast cancer but only 52.3% had been screened while 65.5% had “Good knowledge” of breast cancer. Positive attitude to breast cancer screening was displayed in 52.5% while over 90% claimed to be practicing breast self-examination. Only 36.1% of respondents above 40 years old have had mammography done. Most frequent barriers to screening uptake include cost, poor accessibility to screening facilities, shyness (unfamiliar screener), unavailability of female doctors, careless attitude, fear of cancer and other more pressing family problems. Using logistic Regression at p ≤ 0.05, females with a negative attitude, young unmarried (less than 30years) and lack of easy accessibility to screening facilities were significant factors affecting uptake of breast cancer screening services.
Conclusion
Due to knowledge-uptake gap of breast cancer screening revealed in this study. It is therefore obvious from these findings that a concerted effort is needed to actively remove these barriers by repeated education, training and re-training strategies among health workers and to improve their uptake and level of advocacy and campaign for breast cancer screening among their patients and clients.
Author Contributions
Academic Editor: Padmavathi Kora, Gokaraju Rangaraju Institute of Engineering & Technology, Hyderabad.
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2021 Adesoji E. ADETONA, et al.
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Background
Globally, the leading cause of morbidity and mortality among non-communicable diseases is cancer1, and the most common cancer among women is Breast cancer2 and this requires highly sensitive test procedures to detect, especially at the appropriate age (usually above 40 years) 3. Some of the common forms of cancer have standard screening programmes, especially breast and cervical cancer in women. In most developed countries in the world, the screening tests for breast cancer include a self-breast examination, clinical breast examination and the more sensitive mammography and their uptake is also high 3, 4. However, in developing countries, while the uptake of Self Breast Examination is very high, that of Mammography by female above 40 has been very low 5, 6, 7, 8, 9.
There are several factors affecting uptake of breast cancer screening which varies from developed to developing countries, urban to rural dwellers, high to low socioeconomic status. These factors include the level of understanding of the disease and methods of screening, availability and accessibility of the national or facility-based screening programmes, awareness of the available screening programme, level of income, appropriate national policy for uptake, cultural factors, individual attitude and religious belief together with the outcome of the result 10.
A recent study showed that the most common cancer among Nigerian women, in 2009–2010 (in the record of Ibadan and Abuja cancer registries), were breast and cervical cancer with a significant increase in breast cancer and no rise in incidences of cervical cancer 1. The age-standardized incidence rate for breast cancer in Nigeria was 13.7 per 100,000 between 1960 and 1969. These rates rose to 24.7 per 100,000 by 1998–1999, amounting to a doubling of incidence over four decades and 54.3 per 100 000 in 2009–2010 study which represented a 100% increase in the last decade 1, 11. This, therefore, will require important strategies toward the reduction of this incidence and mortality of breast cancer which will facilitate early detection and prompt management of pre-invasive or early diagnosed breast cancer.
This study will determine factors responsible for poor uptake of breast cancer screening programs among female staff of this tertiary hospital in this environment which may have a significant influence on the low level of screening among women in this environment. However, the report of this study could be used in formulating policies that will ensure adequate understanding and full participation of both female health providers and eligible women in the available screening programs to reduce the cancer burden.
Methodology
This study was a descriptive cross-sectional study conducted at a tertiary health institution in South-West Nigeria, among female staff of both clinical and non-clinical departments within the age group of 18 and 60 years with a percentage ratio of clinical to non-clinical female members of staff of 9.8% to 90.2%. Leslie Kish formula for determining single proportion (for descriptive studies) was used to determine sample size as follows:
Formula: n = Zα2pq/d2with degree of precision (5 % = 0.05) and p = 32%
An allowance for 10% Non-response rate (and Attrition Rate) was applied resulting into an estimated sample size of 372 participants.
The inclusion criteria included all female members of staff, age 18 – 60, who gave their consent to participate while all the female members of staff on contract and female temporary workers were excluded.
The selection of the participants was by a stratified random sampling technique. The female staff were stratified into clinical and non-clinical female staff members, then a proportional allocation to population size in each stratum based on the approximate calculated sample size of 375 resulting in approximately 40 clinical staff and 335 non-clinical staff. The proportional allocation was repeated among each subgroup to arrive at the number of participants to be interviewed per department. Finally, a simple random sampling method was used to select the participants that eventually participated in the study from each department
This study was conducted between June and December 2014. A pre-test of the instrument was carried out at a state tertiary hospital for validation before the onset of the research. All obstacles encountered were then considered and the questionnaire was subsequently reviewed with some modification. The data collected in the field were primarily from the respondents, through an interview with the help of the self-administered semi-structured questionnaire. Three hundred and seventy-five (375) questionnaires were administered out of which 360 participants responded with 15 non-respondents, resulting in only 4% non-response rate. All ethical issues were duly considered, and ethical approval was obtained from the appropriate Local Ethical Committee.
The questionnaires were serialized, edited, and safely stored; thereafter, SPSS version 20 was used for data entry. Descriptive statistics were used to illustrate the sociodemographic variables, the occurrence of the knowledge and attitude of participants to breast cancer and the available screening programs and factors influencing the uptake of the screening programs. Chi-square statistics were used to determine the association between some selected categorical variables while non-parametric correlation analysis was used to determine the relationship and strength of the uptake of the screening programs with some selected variables. All analysis was done in 2014.
The knowledge of participants and their uptake was assessed by the frequency of occurrence of ‘yes’ to the positive questions and ‘no’ to the negative questions regarded as positive while the inverse was regarded as negative. For the attitude, Likert scale was used. For direct positive questions, each response was rated 1-5, which was coded as 5 - Strongly agree, 4- Agree, 3 – Undecided, 2 – Disagree, 1 – Strongly disagree while a reverse coding was used for negative questions. The attitude score of each respondent was generated and the mean, as well as the minimum and maximum scores, were used to determine the scores. The scores ranged from 10-50, and the mean score of 30 was used, therefore, scores of 30 and above were tagged as positive attitude, while scores <30 were tagged as a negative attitude.
Logistic regression analysis was performed to predict the uptake of breast cancer screening services. The selection of explanatory variables for "barrier" was based on correlation analysis and variables which had statistically significant correlation coefficient (p < 0.05) with the outcome variable were selected
Result
Socio-Demographic Characteristics
Among the 375 participants recruited into this study, 360 returned a completed questionnaire giving a response rate of 96%.
The result from Figure 1 below shows the distribution of the study participants into 48 (13.3%) clinical and 312 (86.7%) non-clinical staff members and the socio-demographic characteristics of the respondents. The largest proportion of the respondents 177 (49.2%) were within the age group 30-39 years while the lowest proportion of 39 (10.8%) was within 20-29 years. The mean age of all respondents was 38.2±0.43 years, with age range of between 20 and 58 years. All the respondents were females, the highest educational status was first degree (43.3%) while 21.4% had postgraduate degrees, the majority were married (87.2%), while the remaining 25.3% had no child and included those that were single and those that were married but with no children yet.
Awareness and Source of Information on Breast Cancer
Majority of the respondents, (97.8%) had heard of breast cancer while only (2.2%) were ignorant of the disease. Most of the respondents got their information from their relatives (41.9%) and health workers (30.6%). Other sources included Neighbours (11.1%), friends (10.3%), and media (4.7%).
Knowledge of Breast Cancer
Regarding the risk factors for breast cancer, 282 (78.3%) of the respondents stated that breast cancer is hereditary, 266 (73.9%) understood that breastfeeding decreases the risk, 262 (72.8%) reported that risk increases with advancing age while some said painless breast lump is a risk factor (66.9%). Surprisingly, 130 (36.1%) of the participants claimed magic and evil spirit been risk factors also.
The knowledge on the commonly presenting symptoms of breast cancer was also assessed, 284 (79.8%) of the respondents reported breast lump, 213 (59.2%) bloody nipple discharge, 208 (57.8%) disparity in breast sizes, 197 (54.7%) ulcer on the breast while 186 (51.7%) admitted pain in the breast. Other women stated that skin discoloration, recurrent boils in the breast and foul-smelling nipple discharge are symptoms.
There was a good knowledge of the available screening methods for breast cancer among the respondents. Majority alluded to breast self-examination (295, 81.9%), mammography (225, 62.5%) and clinical self-examination (186, 51.7%). The staff of age 40 and above also have good knowledge of mammography (117, 81.2%).
The respondents also had good knowledge of the available forms of treatment of breast cancer, 243 (67.5%) surgical treatment, 237 (65.8%) medical treatment and 193 (53.6%) radiotherapy. Alternative medicines were considered in 49 (13.6%) of the respondents while 115 (31.9%) said no specific treatment modality is available.
Majority of the respondents, 276 (76.7%) also stated that early detection of breast cancer can improve outcome.
Concerning the knowledge score of the respondents on breast cancer screening, 213 (61.9%) had good knowledge of breast cancer while only 131 (38.1%) had poor knowledge.
Attitude to Breast Cancer Screening
Most of the respondents, 346 (96.1%) have positive attitudes toward breast cancer screening while 14 (3.9%) have negative attitudes toward the screening. The participants above 40 years, 141 (97.9%) also have good attitudes to the screening.
The Practice of Breast Cancer Screening
Only 155 (43.1%) of respondents have had a breast cancer screening (Figure 1). Reasons given by respondents for non-uptake of screening services included indecision in 42.5% of all respondents, lack of information (22.9%), and feeling of good health (17.7%) (Figure 2). Most of respondents 224 (90.0%) said they practiced breast self-examination (Figure 3), while a greater proportion (139 62.3%) said they had gone for clinical breast examination before. Only 107(29.7%) reported having done MRI, 43 (7.8%) reported having done both mammography and biopsy for histology, while the least reported breast screening procedure done by respondents was ultrasound (32, 8.9%). However, of the respondent's age 40 and above (who are eligible for mammography screening and made up 40% of the respondents), only 36.1% have had mammography done (Figure 3).
Figure 1.Proportion of respondents previously screened for Breast Cancer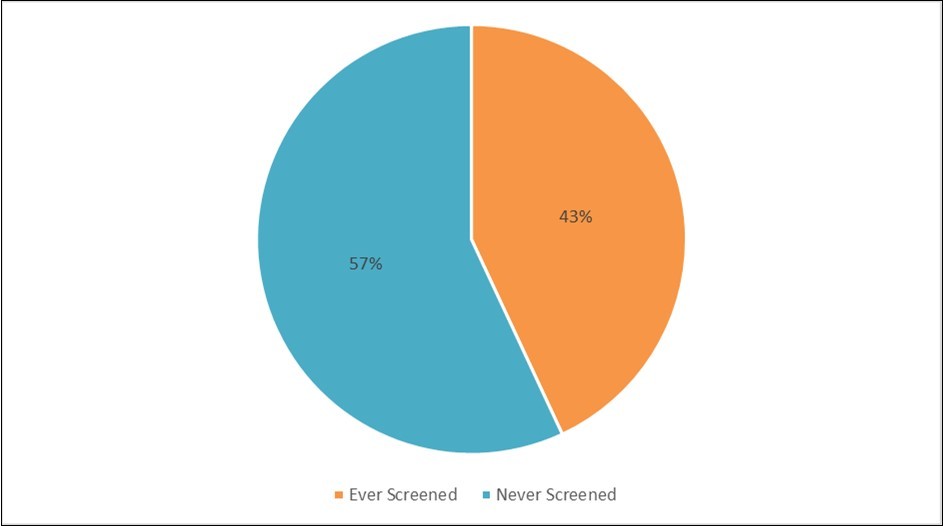
Figure 2.Different barriers to uptake of Breast Cancer Screening
Figure 3.Frequency of different types of screening uptake among respondents
Figure 4.Family history of breast cancer versus Uptake of the Screening Programme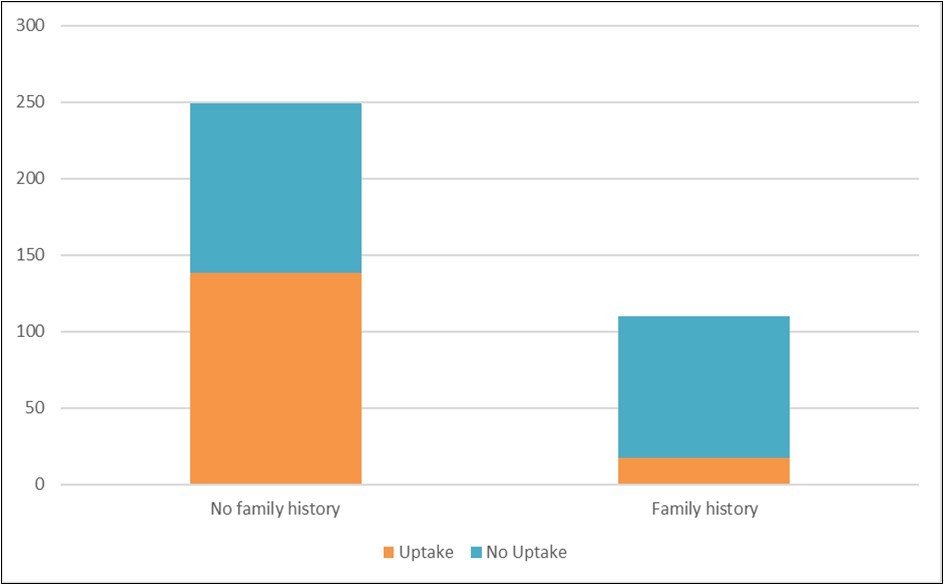
Socio-Demographic Characteristics of Respondents Versus the Uptake of Breast Cancer Screening
(Table 1) showed that there was no significant relationship between the age of respondents and their uptake of breast cancer screening (p = 0.283).
Table 1. Socio-Demographic Characteristics of Respondents versus uptake of Breast Cancer Screening| Socio-Demography | Uptake of breast cancer screening | χ2 | p-value | ||
| Yes (%) | No (%) | Total (%) | 3.883 | 0.283 | |
| Age(yrs.) | |||||
| 20-29 | 21 (13.5) | 18 (8.8) | 39 (10.8) | ||
| 30-39 | 76 (49.0) | 101 (49.3) | 177 (49.2) | ||
| 40-49 | 36 (23.2) | 62 (30.2) | 98 (27.2) | ||
| 50& Above | 22 (14.2) | 24 (11.7) | 46 (12.8) | ||
| Level of Education | 13.507 | 0.017* | |||
| SSCE | 1 (0.6) | 4 (1.0) | 5 (1.4) | ||
| OND | 7 (4.5) | 28 (13.7) | 35 (9.7) | ||
| HND | 43 (27.7) | 44 (21.5) | 87 (24.2) | ||
| BSc. | 57 (36.8) | 66 (32.2) | 123 (34.2) | ||
| MB;BS | 18 (11.6) | 15 (7.3) | 33 (9.2) | ||
| Postgraduate | 29 (18.7) | 48 (23.4) | 77 (21.4) | ||
| Number of Children | 4.334 | 0.239 | |||
| 0 | 37 (23.9) | 52 (25.4) | 89 (24.8) | ||
| 1-2 | 63 (40.6) | 65 (31.7) | 128 (35.7) | ||
| 3-4 | 48 (31.0) | 82 (40.0) | 130 (36.2) | ||
| 5 & Above | 6 (3.9) | 6 (2.9) | 12 (3.3) | ||
| Staff designation | 0.153 | 0.754 | |||
| Clinical staff | 19 (40.4) | 28 (59.6) | 47 | ||
| Non-clinical | 136 (43.5) | 177 (56.5) | 313 | ||
The table also shows that there is a significant relationship between the education level of respondents and respondents’ uptake of breast cancer (p = 0.017). This shows that the uptake of breast cancer screening is associated with the level of education.
As regards the association between the number of children owned by respondents and their uptake of breast cancer screening services, the result on Table 1 shows that the uptake of screening programmes was statistically independent of the number of children owned by the respondent (p = 0.239).
Awareness of Breast Cancer Versus Uptake of the Screening Programme
As regards the knowledge of breast cancer and the uptake of the screening programme, there is a higher proportion of the respondents, 352 (97.8%) who have had information on breast cancer but did not take up its screening services especially the mammography. This difference though, was not statistically significant (p =0.190).
Family History of Breast Cancer Versus Uptake of the Screening Programme
As regards the family history of breast cancer and the uptake of the screening programme shown in Figure 4 below, a greater number of respondents who had a family history of breast cancer did not go for any screening. This relationship was statistically significant (p <0.001).
Knowledge of Importance of Early Detection versus the Uptake of Breast Cancer Screening
(Table 2) shows a test of significant between knowledge of the importance of early detection of breast cancer on uptake of breast cancer screening services. The result shows that uptake of breast cancer screening services was dependent on knowledge of the importance of early detection of breast cancer (p < 0.001).
Table 2. Knowledge of Importance of Early Detection versus uptake of breast cancer Screening| Knowledge of Importance of Early Detection | Uptake of breast cancer screening | χ2 | p-value | ||
| Yes (%) | No (%) | Total (%) | |||
| Yes | 139 (50.4) | 137 (49.6) | 276 (76.9) | 29.968 | <0.001 |
| No | 10 (15.4) | 55 (84.6) | 65 (18.1) | ||
| I don’t Know | 5 (27.8) | 13 (72.2) | 18 (5.0) | ||
Majority of the respondents, 276 (76.9%) had good knowledge of the importance of early detection of breast cancer, its management, and its screening (139, 50.4%). Out of 65 (18.1%) respondents who had poor knowledge on the importance of early detection of breast cancer and its management and the 18 (5.0%) who had poor knowledge of the importance of early detection of breast cancer on its management, only 10 (15.4%) and 5 (27.8%) had breast cancer screening respectively.
Attitude to Breast Cancer Screening Versus the Uptake of BSE, CBE, and Mammography
(Table 3) shows the relationship between attitudes of the respondents on uptake of different forms of breast cancer screening which include Breast Self-Examination, Clinical Breast Examination, and mammography. The result reveals a high uptake for BSE 146 (94.8%) and CBE 92 (61.3%) among respondents who had a positive attitude to breast cancer screening, but a low uptake for mammography, 22 (14.6%).
Table 3. Attitude towards breast cancer screening versus uptake of BSE, CBE and Mammography| Attitude towards screening | Uptake of BSE | Uptake of CBE | Uptake of Mammography | ||||||
| Yes | No | Total | Yes | No | Total | Yes | No | Total | |
| Negative | 78(82.1) | 17(17.9) | 95(38.2) | 47(64.4) | 26(35.6) | 73(32.7) | 21(23.1) | 70(76.9) | 91(37.6) |
| Positive | 146(94.8) | 8(5.2) | 154(61.8) | 92(61.3) | 58(38.7) | 150(67.3) | 22(14.6) | 128(85.4) | 151(62.4) |
| Total | 224(90.0) | 25(10.0) | 249(100.0) | 139(62.3) | 84(37.7) | 223(100.0) | 43(17.8) | 199(82.2) | 242(100.0) |
| χ2= 10.492P = 0.002* | χ2= 0.195P =0.769 | χ2= 3.343P = 0.108 | |||||||
The study further test if respondents ‘uptake of BSE, CBE and mammography was dependent on their attitude towards breast cancer screening. The result shows that respondent’s uptake of BSE was dependent on their attitude (p = 0.002), while their uptake of CBE (p = 0.765) and mammography (p = 0.108) was independent of their attitude.
Determinants of Breast Cancer Screening Uptake
(Table 4) shows the result of the logistic regression performed to ascertain the effects of socio-demographic factors, attitude, and awareness of Breast cancer on the likelihood that respondents will go for breast cancer screening. The model explained 18.5% (NagelkerkeR2) of the variance in breast cancer screening uptake and correctly classified 66.2% of cases.
Table 4. Determinants of Breast Cancer Screening uptake| UptakeDeterminants | variables | Coefficient | Standard error | Significance | Odds Ratio |
| Barrier | fear of losing spouse | -20.573 | 12498.497 | 0.999 | 0.000 |
| Age of respondents | 20-29 | 1.000 | |||
| 30-39 | 0.511 | 0.431 | 0.236 | 1.667 | |
| 40-49 | 0.833 | 0.495 | 0.093 | 2.300 | |
| 50 and above | 0.382 | 0.548 | 0.486 | 1.465 | |
| Number of children | 0 | 1.000 | |||
| 1-2 | -0.321 | 0.333 | 0.335 | 0.726 | |
| 3-4 | 0.196 | 0.361 | 0.586 | 1.217 | |
| 5 and above | -0.278 | 0.772 | 0.718 | 0.757 | |
| Education | Completed secondary | 1.000 | |||
| Ordinary diploma | -0.429 | 1.261 | 0.734 | 0.651 | |
| Degree | -0.675 | 1.257 | 0.591 | 0.509 | |
| Postgraduate | -0.561 | 1.275 | 0.660 | 0.570 | |
| Attitude | Positive | 1.000 | |||
| Negative | -1.260 | 0.264 | <0.001* | 0.284 | |
| Awareness | No | 1.000 | |||
| Yes | -20.248 | 18597.952 | 0.999 | 0.000 |
Clear observation on Table 4 shows that attitude has a statistically significant correlation with uptake p ≤ 0.001. This implies that respondents with a negative attitude are less likely to take up breast cancer screening services (coefficient is negative). Those of age, number of children, education, barriers, and awareness were not statistically significant at p > 0.05.
Discussion
Discussion of Findings
This study examined the knowledge, attitude and factors that affect the uptake of breast cancer screening among female health care workers in a tertiary health institution, Southwest, Nigeria. Even though the participants were a sample from among the female staff of the health institution, the sample, as a cross-sectional pool, should reflect what could be expected of the entire female staff.
Knowledge of Screening
The findings from this study highlight the major factors affecting the uptake of breast cancer screening among the respondents. The study demonstrated that the majority of the respondents have heard about breast cancer. These may be because the respondents were hospital staff which cannot be compared with a lower rate of about a third among tertiary school female student’s population in Ibadan and women in a local community in the same environment. 12, 13. This appears to be a problem of developing countries as studies done in Tunisia and Jamaica in 2007 14, 15 showed a similar pattern of the low level of awareness.
Women in developed countries also appear to be more aware of cancer of the breast and the screening programmes as indicated in a study done among Cambodian, Laotian, Thai, and Tongan women which reported above three-quarters of their women with good knowledge on Breast cancer screening 16.
The level of knowledge of the availability of a screening programme for breast cancer was found to be high in this study. This also may reflect the respondents being health staff. Generally, the level of knowledge was found to be low for most developing countries and among the non-health workers. 17, 18.
About half of the respondent's sources of information on cancer and screening were mainly from health workers. Surprisingly, this low proportion may reflect the low drive for information dissemination among the health workers on cancer screening despite high knowledge. This is unlike in the developed areas where the health workers have a mandate to ensure the provision of more effective health education and information about prevention and screening to be able to elicit the fears, prejudices and priorities of patients in these areas that may serve as barriers to uptake of the programmes 19.
In this study, the respondents have a fair understanding of the symptoms associated with breast cancer in which painless lump in the breast and bloody nipple discharge were highly considered.
The most common risk factors for breast cancer mentioned include hereditary, painless breast lump, and advancing age for breast cancer. This finding is also similar to the finding in a study done among Cambodian, Laotian, Thai, and Tongan Women 16. In this study, about one-fifth of the respondents could not identify any risk factor for breast cancer.
The knowledge of risk factors is an important element in the prevention of breast cancer. Knowing the modifiable risk factors can make a woman avoid them and hence prevent disease occurrence. Surprisingly, one-fifth of the respondents still believe in the evil spirit and magic being a risk factor for breast cancer.
Women's knowledge on the importance of screening for breast cancer to detect premalignant lesion was also good, only a few were not sure of screening importance. The majority identified BSE as the breast cancer screening method, however, some also recognized CBE and mammography. This pattern is also seen in the similar studies done among health workers in Tunisia and some developed countries 20, 21. Among the respondents, about half believed that any woman of age 18 years and above is eligible for screening.
Attitude Towards Screening
This study shows a good attitude of the respondents to seek medical help when noticed a lump or other associated symptoms though some will allude to pray unto God.
This study also looked at the respondent’s attitude to breast screening programmes. Overall, more than half of the respondent had a positive attitude towards the screenings.
Perception of susceptibility to the development of breast cancer was found to be another factor that can affect screening behaviour. Less than one-quarter of the respondents wrongly expressed lack of personal susceptibility to cancer and therefore believed they didn't need to have any screening done.
The Practice of Screening Programmes
This study also looked at the practice of screening programmes among the respondents. In this study, 94%, 58% and 11% of the respondents had practised BSE, CBE and mammography before while only third of respondents above 40 years old have had mammography done. This pattern of low uptake of mammography is usually observed across African countries including among the female health workers despite their good knowledge and also among Vietnamese women 16 and 22.
There were huge differences when comparing the practice in African countries to those in developed countries. In the UK, multiple strategies were in place to capture all eligible women for the screening programme despite the high uptake level 23. In this study, the majority of women in the age group 30-39 years uptake the screening more unlike the younger women in the developed countries, who tend to be screened earlier based on the high level of awareness and the availability standard national programmes on screening. However, the small proportion of women in the age group 20-29 years taking up the screening for breast cancer could also be due to common belief that breast cancer is commoner in older women except for people with positive family history.
Even though there was no significant association between age and awareness of breast cancer, however, respondents at all ages practice BSE while the least practised is mammography even among the age group above 40 years which is unlike some studies where increase uptake was reported among this group 18, 21.
The relationship between marital status and uptake of BSE was not significant (p> 0.05).
Factors Affecting the Uptake of the Screening Programmes
Barriers to the uptake of breast cancer screening have been shown to exist in many countries. The greatest barriers identified against breast cancer screening uptake include none affordability/accessibility, shyness (because of familiarity with the screener) and unavailability of female doctors most of the times. Other factors include careless attitude, fear of cancer and other more pressing family problems. Similar barriers are common to several local and hospital-based studies even in this environment 12, 24, 25.
These findings identify the need of providing adequate information about the importance of breast cancer screening to the health workers in different department to eliminate these barriers. It is therefore obvious that a concerted effort is needed to actively remove these barriers by repeated education, training and re-training strategies to improve their uptake and level of advocacy in campaigning for screening among their patients and clients.
The correlations between the uptake of the breast cancer screening and age are significant with the uptake of mammography (p < 0.0001) and with various factors preventing utilization of screening programmes (p = 0.016).
Conclusions
The result of this study provides a comprehensive picture of the knowledge, attitude and practise of the screening for breast cancer, including the locally available screening procedures, various barriers to uptake of the screening programmes and the barriers to the utilization of the locally available screening procedures. Various factors identified in this study that affect the screening programme are modifiable. This could be addressed through multiple channels which may include detailed and regular sensitization and awareness programme for all staff on epidemiology, risk factors, symptoms and management of common cancers. Most especially, special emphasis should be made on the available screening programmes and the importance and necessity of uptake with a primary aim of addressing the barriers.
Recommendations
Due to the poor uptake of screening programmes among a tertiary health institution female staff despite the local availability of the screening programme and several modifiable barriers identified in this study, the following will be recommended
The management of medical institutions should embarked on a regular hospital-wide grand round on the importance of screening, awareness of available local screening programmes and the need for every staff to actively campaign and ensure that majority of the patients and clients encounter are encouraged for screening (see and screen policy).
There should be active awareness on all the locally available screening programmes within the medical institutions by the information and IT units of the hospital which will be in form of posters, billboards, handbills, in calendars, text messages and electronic board display.
The hospital management should include locally available screening programmes in the routine pre-employment screening tests especially for women for all the newly employed staff
Policies regarding regular breast cancer screening for all women both locally and nationwide should be formulated and enforced.
References
- 1.Jedy-Agba E, M P Curado, Ogunbiyi O, Oga E, Fabowale T et al. (2012) Cancer incidence in Nigeria: A report from population-based cancer registries.Cancer Epidemiol[Internet]. 36(5), 271-8.
- 2.Akram M, Iqbal M, Daniyal M, Khan A U. (2017) Awareness and current knowledge of breast cancer. Biological Research.
- 3.Billette D, Agathe E, Garnier C, Ancelle-Park A, Ferley R. (2007) Evaluation of a combined screening programme for breast, cervical and colorectal cancers in. , France.Eur J cancerPrev[Internet] 16(1), 26-35.
- 4.. Barratt, A., Mannes, P., Irwig, L., Trevena, L., Craig, J.,et.al,.(2002). Cancer screening. Heggenhougen K, editor.N Z Med J[Internet]. BMJ Group 111(12), 899-902.
- 5.O S Arulogun, Maxwell O O. (2012) Perception and utilization of cervical cancer screening services among female nurses in University College Hospital, Ibadan. , Nigeria.PanAfrMed J 11, 69.
- 6.O A Ayinde, A O Omigbodun, Ilesanmi A O. (2004) Awareness of cervical cancer, Papanicolaou’s smear and its utilisation among female undergraduates in Ibadan.AfrJReprodHealth. 8(3), 68-80.
- 7.C O, Aniebue U. (2011) Why Southeastern Nigerian Women Who Are Aware of Cervical Cancer Screening Do Not Go for Cervical Cancer Screening.Int JGynecolCancer[Internet]. 21(7), 1282.
- 8.Al-Wassia R K, Farsi N J, Merdad L A, Haj S Patterns. (2017) knowledge and barriers of mammography use among women in Saudi Arabia.Saudi Med.
- 9.Al-Zalabani A H, Alharbi K D, Fallatah N I, Alqabshawi R I. (2018) . Al-Zalabani AA,et.al,.Breast Cancer Knowledge and Screening Practice and Barriers Among Women in Madinah, Saudi Arabia.J Cancer Educ .
- 10.Dodo A M, Sykes P, Powell C. (2016) Exploring the barriers to breast and cervical cancer screening in Nigeria: A narrative review. African Journal of Reproductive Health.
- 11.. Cancer In Africa IARC Scientific Publication No 153 Parkin, D.M., Hamdi-Chérif, M., Sitas, F., Thomas, J.O., Wabinga H. (2003). editor. IARC Publications - Cancer Epidemiology .
- 12.Asuzu C, Inegbeniki D. (2011) Assessing the cancer screening behaviours of female healthcare workers in the University College Hospital (UCH):. , Ibadan.PsychoOncology 20, 158.
- 13.Asuzu C, Unegbu J. (2009) Knowledge, attitude and behaviour of university of ibadan women toward cancer of the cervix and its prevention.PsychoOncology. 18, 99.
- 14.Hsairi M, H B Gobrane, N B Alaya, Bellaaj R, Achour N. (2007) Knowledge and attitudes of medical students at the end of their curriculum, towards breast and cervical cancer screening.SantePublique(Paris)[Internet]. 19(2), 119-32.
- 15.Bessler P, Aung M, Jolly P. (2007) Factors affecting uptake of cervical cancer screening among clinic attendees in Trelawny. , Jamaica.Cancer Control 14, 396-404.
- 16.Dang J, Lee J, J H Tran. (2010) Knowledge, Attitudes, and Beliefs Regarding Breast and Cervical Cancer Screening among Cambodian, Laotian, Thai, and Tongan Women.J cancer Educ[Internet]. 25(4), 595-601.
- 17.Lin S. (2008) Factors influencing the uptake of screening services for breast and cervical cancer in. , Taiwan.J R SocPromotHealth[Internet] 128(6), 327-34.
- 18.Akinyemiju T F. Department of Epidemiology, University of Michigan School of Public Health (2012) Socio-economic and health access determinants of breast and cervical cancer screening in low-income countries: analysis of the World Health Survey.PLoSOne. , Ann Arbor, Michigan, United, States of America. [email protected]; 7(11), 1-5.
- 19.Bowling A. (1989) Implications of preventive health behaviour for cervical and breast cancer screening programmes: a review.FamPract. 6(3), 224-31.
- 20.S El Mhamdi, Bouanene I, Bouslah A, Sriha A, K B Salem et al.Breast and cervical cancer screening: Knowledge, attitudes and practice of health personnel in the region of Monastir (Tunisia).Trop Med Int Heal[Internet]. 16, 318.
- 21.Martín-López R, Hernández-Barrera V, Andres A L De, P C Garrido, Miguel De. (2010) Breast and cervical cancer screening in Spain and predictors of adherence.Eur. , J cancerPrev[Internet] 19(3), 239-45.
- 22.Abu-Helalah M A, Alshraideh H A, AAA Al-Serhan, Kawaleet M, Nesheiwat A I. (2015) Knowledge, barriers and attitudes towards breast cancer mammography screening in Jordan.Asian Pacific J Cancer Prev.
- 23.D P Weller, Campbell C. (2009) Uptake in cancer screening programmes: a priority in cancer control.Br. , J Cancer[Internet]. Nature Publishing Group 101, 55-9.
Cited by (2)
This article has been cited by 2 scholarly works according to:
Citing Articles:
Texila international journal of public health (2022) OpenAlex
Texila international journal of public health (2022) OpenAlex
