Assessment of the Preferred Methods Used by Mothers to Prevent Malaria Infection among Children Under Five Years in the Hohoe Municipality Of Ghana
Abstract
Background:
The use of Long Lasting Insecticide Nets (LLINs) is seen as a major public health intervention and has shown to have both direct and indirect effects on the dynamics of malaria transmission. This report assessed the methods used by mothers to prevent malaria infection among their children under five years in the Hohoe Municipality.
Method:
A cross-sectional survey carried out in February 2017 among 418 mothers with children under five. Data were collected in the form of interviews using questionnaires on the usage of LLIN alone, LLIN with other methods (LLIN+) and use of other methods only (OMs). Chi square test and multinomial logistic regression were used to determine the association between dependent and independent variables.
Results:
Of the 418 mothers, 28.5% used LLIN only, 50.7% used LLIN+ and 20.8% used OMs only to prevent malaria. Mothers aged 30-39 and 40-49 years were 3.87 and 5.55 times more likely to use LLIN only rather than OMs as compared to those aged less than 20 years (AOR=3.87, p=0.019) and (AOR=5.55, p=0.029) respectively. Similarly, mothers aged 30-39 and 40-49 years were 3.08 and 4.02 times more likely to use LLIN+ rather than OMs as compared to those aged less than 20 years (AOR=3.08, p=0.023) and (AOR=4.02, p=0.050) respectively. Mothers who attained a higher level of education were 2.08 times more likely to use LLIN+ rather than OMs as compared to those with no formal education (AOR=2.08, p=0.015). Those who resided in rural areas were 2.00 times more likely to use LLIN only and LLIN+ rather than OMs only as compared to urban dwellers (AOR=2.00, p=0.002) and (AOR=2.00, p=0.013) respectively.
Conclusion:
More than half of the mothers preferred using LLIN+. One out of 3 mothers used only LLIN while one out of 5 used OMs only to prevent malaria. Age, educational level and place of residence were significantly associated with methods used to prevent malaria. There is the need for targeted education on LLINs in order to improve usage among younger mothers and mothers residing in urban areas. Further investigations to determine reasons for using OMs only and also determine the added value of OMs to LLINs in preventing malaria are recommended.
Author Contributions
Academic Editor: Prachi Arora, University of Wisconsin - Madison
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2017 Margaret Kweku, et al
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Introduction
Malaria continues to be a major public health problem globally with high mortality and morbidity in Africa. As at December 2015, the disease accounted for 214 million cases and 438,000 deaths globally with sub-Saharan Africa (SSA) accounting for 88% and 90% of cases and deaths respectively 1. Pregnant women and children are the most vulnerable groups to Malaria 2. Malaria in pregnancy exposes women to an increased risk of severe anaemia, spontaneous abortion, premature delivery or death while subjecting the foetus to the risk of stillbirth or low birth weight 3, 4 . Children are particularly susceptible to the disease due to their poorly developed immune system. Despite the decline in morbidity and mortality, malaria remains the fourth leading cause of under-five mortality in the sub-region 5, 6.
Considering the closeness between mother and child, effective measures put in place to protect the mother from malaria could also protect the child and hence reduce the morbidity and mortality related to malaria 7. In 1992, the World Health Organization (WHO) during its global ministerial conference on malaria in Amsterdam approved a number of control measures, which include early diagnosis and prompt effective treatment, chemoprophylaxis in susceptible groups, reduction of man-vector contact, information, education and communication (IEC), surveillance and research 8.
In order to reduce the burden and mortality of malaria in the region, African leaders committed to implementing strategies of the Roll Back Malaria Initiative (RBM). The commitment was to be realized by 60% coverage of populations at risk with anti-malaria interventions 9. The 60% coverage was subsequently redefined to 80% coverage by 2010 and further raised higher with the introduction of the Global Malaria Action Plan for universal coverage 10. Mosquito nets, treated with insecticides were found as one of the major breakthroughs in the fight against malaria. They were found to give a much higher degree of protection against malaria 11. The use of mosquito nets was one of the primary interventions recommended by WHO Global Programme (WHO/GMP) for effective malaria control 12.
However, reports have shown that caregivers and mothers use other preventive measures in addition to LLIN in preventing malaria. A study conducted in Ekiti, Nigeria revealed that, 28% of the respondents used LLIN alone, others used other malaria preventive methods such as mosquito coil (21%), 21% used gauze wire in windows and 30% used other methods such as mosquito repellent, brooms and burning of cow dung 13.
In Ghana, according to the Ghana Demographic Health Survey (GDHS), overall LLIN ownership was 68.3% with 60.7% ownership in urban and 78.3% in rural settings. The overall usage of LLIN was 46.6% with 35.8% in urban and 56.1% in rural settings. In the Volta Region LLIN ownership was 76.3% and usage was 66.3% 14. No studies have been conducted to show the preferred malaria control measures in the Volta region. This report assessed preferred methods of controlling malaria among mothers with children under five years in the Hohoe Municipality of Ghana.
Study Area
The study was undertaken in the Hohoe Municipality, which is one of the twenty-five administrative Districts/Municipalities of the Volta Region. The Municipality is located in the central part of the Region with a total land surface area of 1,172 km square and consists of 102 communities. It is located at longitude 0 degrees 15 East and 0 degrees 45 East and latitude 6 degrees 45 North and 7 degrees 15 North and lies almost in the heart of the Volta Region. The Municipality has a total population of 167,016 people projected from the 2010 population census. It is bounded by Jasikan District to the North, Northwest by Biakoye District, South by Afadjato South District, West and Southwest by Kpando Municipality and East by the Republic of Togo. There are two main seasons, the wet and dry seasons. The major wet season lasts from April to July and the minor one from September to November. The rest of the year is relatively dry. The average annual rainfall recorded by the Hohoe Municipal Meteorological Department (HMMD) in the Municipality is 1,592 mm with approximately 1,296 mm rain falling between April and October 15. Malaria is hyper-endemic and transmission is throughout the years but with seasonal peaks. The Municipality has been divided into seven (7) sub-Municipalities namely: Akpafu/Santrokofi, Alavanyo, Agumatsa, Lolobi, Gbi-Rural, Hohoe-sub and Likpe. There are 21 health facilities including a Municipal Hospital (1) Health centres (14) and Community-based Health Planning and Services (CHPS) compounds (6). Fifty-seven (57) outreach Child Welfare Clinics (CWCs) and 24 static clinics are carried out every month in the Municipality.
Study Population
The study population was mothers of children aged less than five years (3-59 months) attending Child Welfare Clinics (CWCs) at the time of the survey.
Inclusion Criteria
The inclusion criteria were, mothers with children aged between 3-59 months, resident within the Hohoe municipality for at least 6 months and gave consent to participate.
Exclusion Criteria
The exclusion criteria were, mothers with children aged less than 3 months or above 59 months, not attending CWCs at the time of the survey, not resident within the Hohoe Municipality for at least 6 months and no consent given to participate.
Study Design
A descriptive cross-sectional study was carried out in February 2017, which involved 418 mothers with children under five years. Data were collected in the form of interviews using pre-tested semi-structured questionnaires. Information was obtained on socio-demographic characteristics (age occupation, educational attainment, place of residence and place child was delivered), LLIN ownership and usage and other methods (fan, mosquito repellents, baby net) used in preventing malaria.
Sample Size Determination
The sample size was calculated using a formula 16. The Reliability coefficient (z score) of 1.96 at 95% confidence level, the margin of error (e) of 5. The prevalence of LLIN use among mothers (p) of 50% was substituted into the formula to determine a minimum sample size of 384. Adjusting for non-response rate of 8% gives the total sample size of 415. However, 418 mothers of children aged 3 to 59 months were recruited.
Sampling Method
Selection of Child Welfare Clinics and Study Participants
A sampling frame of all the CWCs (60) within the Municipality was obtained. A simple random sampling method (lottery) was used to select 10 CWCs, which were located within the Hohoe Municipality. The participants were proportionately distributed to the CWCs based on the 2016 clinic attendants. The probability sampling technique (simple random) was used for the selection of the participants in each clinic. The balloting method specifically, sampling without replacement type was used. With this, the expected number of children under-five (participants) needed for each clinic was estimated. This was done by counting the number of under-five children that reported at the CWC in the same period of the previous year (2016) for each clinic. Once the sampling frame for each clinic was obtained and the number of respondents to be interviewed for each clinic known, ‘‘yes’’ and ‘‘no’’ was written on pieces of papers and then folded. The number of ‘‘yes’’ was equal to the number of respondents required per clinic and the number of ‘‘no’’ was equal to the number remaining after subtracting the required number of children from the total number for each clinic. Parents of all children who were eligible, randomly picked one paper. Those who picked ‘‘yes’’ and consented were interviewed. In a situation where the number of children was less than or equal to the number of children required, all those who visited the CWC were enrolled and interviewed.
Data Collection
Pre-tested semi-structured questionnaires were used to collect the data. The questionnaires were administered to mothers of eligible children under five years immediately after they had completed the CWC activities and were exiting the clinic. The exit interview was conducted in a convenient and conducive place, in the English language, and in Ewe for respondents who did not understand or speak English. Information wasobtained from mothers on the demographic characteristics, socioeconomic status, LLIN ownership and usage and other methods used to prevent malaria.
Statistical Analysis
After entry, data were cleaned and validated to ensure quality before they were analysed. Data were entered using EPI DATA 3.1 software. Cleaned data were then exported to STATA version 14.1 for analysis. Simple frequency and percentages were used to determine the prevalence of categorical variables. Chi square test and Multinomial Logistic Regression were used to determine the association between preferred methods (dependent) and independent variables. Statistical significance was considered based on p-value <0.05.
Ethical Issues
Ethical approval for the study was sought from the Ghana Health Service (GHS) Ethics Review Committee (ERC) (GHS-ERC: 13-07-2014). In addition, permission was obtained from the Hohoe Municipal Health Directorate (HMHD). The respondents were assured that the findings from the study and its dissemination would not have their names or any information that could be used to trace them. By this, confidentiality was assured. Special codes were assigned to the participants; this was to ensure that individuals were not identified by their names.
Results
Table 1 shows that a total of 418 mothers (respondents) with their mean age and that of their children was 28.84±6.7 years and 13.8±10.0 months respectively were recruited for the study. Most of the respondents, 46.2% attained primary/Junior High School (JHS), and most, 35.1% were traders. The majority, 86.5% were married/co-habiting, and most, 97.4% were Christians. The main ethnic groups were the Ewes (82.6%), and more than half (51.4%) of the respondents were residing in urban areas. The majority, 71.5% delivered their babies at the hospital.
Table 1. Socio-demographic characteristics of respondents and their children| Characteristics | Frequency N=418 | Percentage (%) |
| Mean age of child (in months) (SD) | 13.8(10.0) | |
| Age (in months) | ||
| <12 | 203 | 48.6 |
| 12-23 | 149 | 35.6 |
| 24-35 | 42 | 10.0 |
| 36-47 | 17 | 4.1 |
| 48-59 | 7 | 1.7 |
| Sex | ||
| Male | 200 | 47.9 |
| Female | 218 | 52.1 |
| Mother’s socio-demographic characteristics | ||
|---|---|---|
| Mean age in years (SD) | 28.84(6.7) | |
| <20 | 28 | 6.7 |
| 20-29 | 206 | 49.3 |
| 30-39 | 153 | 36.6 |
| 40-49 | 31 | 7.4 |
| Educational level | ||
| No education | 65 | 15.5 |
| Primary/JHS | 193 | 46.2 |
| SHS/Tertiary | 160 | 38.3 |
| Occupation | ||
| Unemployed | 79 | 18.9 |
| Farming | 51 | 12.2 |
| Trading | 149 | 35.7 |
| Artisan | 103 | 24.6 |
| Civil servant | 36 | 8.6 |
| Marital Status | ||
| Single | 58 | 13.9 |
| Married/Co-habiting | 353 | 84.4 |
| Divorced | 3 | 0.7 |
| Widowed | 4 | 1.0 |
| Religion | ||
| Christian | 407 | 97.4 |
| Muslim | 11 | 2.6 |
| Ethnicity | ||
| Ewe | 346 | 82.8 |
| Guan | 72 | 17.2 |
| Location | ||
| Urban | 213 | 51.0 |
| Rural | 205 | 49.0 |
| Place of delivery | ||
| Hospital | 299 | 71.5 |
| Health Centre | 52 | 12.4 |
| Home | 67 | 16.0 |
Methods used to Prevent Malaria
Figure 1 shows that of the 418 mothers, the majority, 212 (50.7%) combined LLIN with other methods (LLIN+) to prevent malaria.
Figure 1.Preferred methods used by respondents to prevent malaria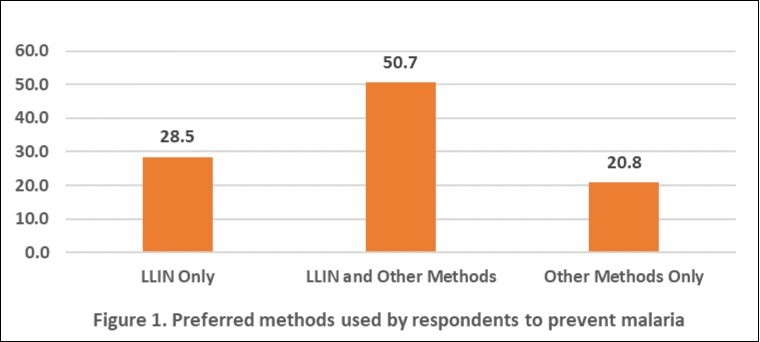
Association Between Socio-Demographic Characteristics of the Respondents and the Odds of Methods Used for Preventing Malaria
Table 2 shows that there was a significant association between level of educational attainment, place of residence and preferred methods used for preventing malaria (χ2=19.76, p=0.001) and (χ2=11.65, p=0.003) respectively.
Table 2. Association between socio-demographic characteristics of mother and preferred methods of preventing malaria| Preferred methods of preventing malaria | |||||
| Characteristics | LLIN only n=119 n( %) | LLIN+ n=212 n( %) | OMs only n=87 n( %) | Total (N) | χ 2 (p-value) |
| Mother’s age(years) | |||||
| < 20 | 6(21.4) | 11(39.3) | 11(39.3) | 28 | 9.79(0.134) |
| 20-29 | 55(26.7) | 104(50.5) | 47(22.8) | 206 | |
| 30-39 | 47(30.7) | 81(52.9) | 25(16.3) | 153 | |
| 40-49 | 11(35.5) | 16(51.6) | 4(12.9) | 31 | |
| Education | |||||
| No education | 14(21.5) | 38(58.5) | 13(20.0) | 65 | 19.76(0.001) |
| Primary | 73(37.8) | 77(39.9) | 43(22.3) | 193 | |
| SHS/Tertiary | 32(20.0) | 97(60.6) | 31(19.4) | 160 | |
| Occupation | |||||
| Unemployed | 25(31.7) | 37(46.8) | 17(21.5) | 79 | 8.00(0.433) |
| Farming | 15(29.4) | 26(51.0) | 10(19.6) | 51 | |
| Trading | 44(29.5) | 82(55.0) | 23(15.4) | 149 | |
| Artisanship | 29(28.2) | 47(45.6) | 27(26.2) | 103 | |
| Civil servants | 6(16.7) | 20(55.6) | 10(27.8) | 36 | |
| Marital status | |||||
| Single | 14(24.1) | 25(43.1) | 19(32.8) | 58 | 10.54(0.103) |
| Married/co-habiting | 101(28.6) | 186(52.7) | 66(18.7) | 353 | |
| Divorced | 2(66.7) | 0(0.0) | 1(33.3) | 3 | |
| Widowed | 2(50.0) | 1(25.0) | 1(25.0) | 4 | |
| Religion | |||||
| Christianity | 117(28.8) | 206(50.6) | 84(20.6) | 407 | 0.68(0.712) |
| Islam | 2(18.2) | 6(54.5) | 3(27.3) | 11 | |
| Ethnicity | |||||
| Ewe | 91(26.3) | 178(51.4) | 77(22.3) | 346 | 5.53(0.063) |
| Guan | 28(38.9) | 34(47.2) | 10(13.9) | 72 | |
| Location | |||||
| Urban | 47(22.1) | 111(52.1) | 55(25.8) | 213 | 11.65(0.003) |
| Rural | 72(35.1) | 101(49.3) | 32(15.6) | 205 | |
| Socioeconomic status | |||||
| Low SES | 80(30.4) | 126(47.9) | 57(21.7) | 263 | 2.3(0.316) |
| High SES | 39(25.2) | 86(55.5) | 30(19.3) | 155 | |
| Place of delivery | |||||
| Hospital | 85(28.4) | 147(49.2) | 67(22.4) | 299 | 3.22(0.520) |
| Health centre | 12(23.1) | 31(59.6) | 9(17.3) | 52 | |
| Home | 22(32.8) | 34(50.7) | 11(16.4) | 67 | |
Table 3 shows that respondents aged 30-39 and 40-49 years were 3.87 and 5.55 times more likely to use LLIN only rather than other methods as compared to those aged less than 20 years AOR=3.87 (95% CI: 1.25 11.99) p=0.019 and AOR=5.55 (95% CI: 1.19 25.89) p=0.029 respectively. Respondents aged between 30-39 and 40-49 years were 3.08 and 4.02 times more likely to use LLIN+ rather than OMs only as compared to those aged less than 20 years AOR=3.08 (95% CI: 1.16 8.15) p=0.023 and AOR=4.02 (95% CI: 0.99 16.28) p=0.050 respectively. Mothers who attained SHS/Tertiary educational level were 2.08 times more likely to use LLIN+ rather than OMs only as compared to those with no formal education AOR=2.08 (95% CI: 1.15 3.76) p=0.015.
Table 3. Association between socio-demographic characteristics and the odds of preferred method for preventing malaria| Preferred methods for preventing malaria | |||||
| Unadjusted Multinomial Logistic Regression | Adjusted Multinomial Logistic Regression | ||||
| Characteristics | LLIN only COR (95% CI) p-value | LLIN+ COR (95% CI) p-value | LLIN only AOR (95% CI) p-value | LLIN+ AOR (95% CI) p-value | |
| Mother’s age(years) | |||||
| < 20 | |||||
| 20-29 | 2.14(0.74, 6.24) 0.161 | 2.21(0.90, 5.46) 0.085 | 2.32(0.78, 6.89) 0.130 | 2.10(0.83, 5.30) 0.118 | |
| 30-39 | 3.45(1.14, 10.42) 0.028 | 3.24(1.25, 8.36) 0.015 | 3.87(1.25, 11.99) 0.019 | 3.08(1.16, 8.15) 0.023 | |
| 40-49 | 5.04(1.11, 22.96) 0.037 | 4.00(1.01, 15.87) 0.049 | 5.55(1.19, 25.89) 0.029 | 4.02(0.99, 16.28) 0.050 | |
| Educational Attainment | |||||
| No education | |||||
| Primary/JHS | 0.63(0.27, 1.47) 0.290 | 1.63(0.78, 3.39) 0.189 | 0.68(0.29, 1.63) 0.391 | 1.71(0.81, 3.63) 0.160 | |
| SHS/Tertiary | 0.61(0.33, 1.130 0.110 | 1.75(1.01, 3.03) 0.047 | 0.79(0.41, 1.54) 0.488 | 2.08(1.15, 3.76) 0.015 | |
| Occupation | |||||
| Unemployed | |||||
| Farming | 1.02(0.37, 2.80) 0.969 | 1.19(0.47, 3.02) 0.707 | |||
| Trading | 1.30(0.59, 2.89) 0.517 | 1.64(0.78, 3.42) 0.190 | |||
| Artisanship | 0.73(0.32, 1.64) 0.446 | 0.80(0.38, 1.68) 0.556 | |||
| Civil servants | 0.41(0.12, 1.33) 0.138 | 0.92(0.35, 2.38) 0.862 | |||
| Marital status | |||||
| Single | |||||
| Married/co-habiting | 2.08(0.97, 4.43) 0.058 | 2.14(1.11, 4.14) 0.024 | |||
| Divorced | 2.71(0.22, 33.0.5) 0.433 | 0.03(0.01, 2.87) 0.987 | |||
| Widowed | 2.71(0.22, 33.01) 0.433 | 0.76(0.04, 12.95)0.850 | |||
| Religion | |||||
| Christianity | |||||
| Islam | 0.48(0.08, 2.93) 0.425 | 0.81(0.20, 3.34) 0.777 | |||
| Ethnicity | |||||
| Ewe | |||||
| Guan | 2.37(1.08, 5.18) 0.031 | 1.47(0.69, 3.13) 0.316 | |||
| Place of residence | |||||
| Urban | |||||
| Rural | 2.63(1.48, 4.65) 0.001 | 1.56(0.94, 2.61) 0.087 | 2.00(1.39, 4.67) 0.002 | 2.00(1.16, 3.47) 0.013 | |
| Socio-economic status | |||||
| Low SES | |||||
| High SES | 0.93(0.52, 1.66) 0.797 | 1.29(0.77, 2.18)0.327 | |||
| Place of Delivery | |||||
| Hospital | |||||
| Health centre | 1.05(0.42, 2.64) 0.916 | 1.57(0.71, 3.48) 0.267 | |||
| Home | 1.58(0.71, 3.48) 0.260 | 1.41(0.67, 2.94) 0.363 | |||
Respondents residing in rural areas were 2.00 times more likely to use LLIN only rather than other methods only as compared to those who resided in urban areas (AOR=2.00 (95% CI: 1.39 4.67) p=0.002). Similarly, mothers who resided in rural areas were 2.00 times more likely to use LLIN+ rather than OMs only as compared to those who resided in urban areas (AOR=2.00 (95% CI:1.16 3.76) p=0.013).
Discussions
This study assessed methods used by mothers to prevent malaria infection among children under five years in the Hohoe Municipality of Ghana. The current study revealed that the use of LLINs only by mothers to prevent malaria was 28.5%. This is in agreement with what was reported from Ekiti, Nigeria which also found only 28% respondents using only LLINs to prevent malaria 13. It was also found that older mothers aged between 30-39 and 40-49 years were 3.87 and 5.55 times more likely to use LLINs only rather than OMs as compared to mothers aged less than 20 years (p=0.019) and (p=0.029) respectively. Mothers who resided in rural areas were 2 times more likely to use LLINs only rather than other methods as compared to mothers in urban areas (p=0.002). The possible reasons why older mothers used LLINs only could be that they might have obtained more information on the use of LLINs during their previous pregnancies and might have used LLINs with their children before and experienced the effectiveness of the nets.
This current study also found that 50.7% of mothers combined LLINs with other methods and older mothers aged between 30-39 and 40-49 years were 3.08 and 4.02 times more likely to combine LLIN with and other methods rather than OMs only as compared to mothers aged less than 20 years (p=0.023) and (p=0.050) respectively. Mothers in this study preferred using a combination of LLIN with other methods because they might have the perception that LLINs alone cannot give them maximum protection since they are not always sleeping except in the night. However, mosquitoes are seen around the homes in the evenings when they are not sleeping. This may compel them to use other methods to complement the LLIN. Another reason could be that mothers may not use LLINs all the time because sometimes the net may be washed and not be hanged or may not use it because of heat and may use OMs to complement LLIN.
The current study also found that mothers with a higher (SHS/tertiary) educational attainment were 2.08 times more likely to use a combination of LLIN while other mothers preferred using LLIN and other methods rather than OMs only as compared to those with no formal. It is possible that mothers with higher educational attainment could read and understand information and instructions on the use of LLIN and adverts on other methods and are therefore attracted to using other methods.
The current study found that mothers who resided in rural areas were 2 times more likely to use LLINs only as well as 2 times more likely to combine LLIN with other methods as compared to those in urban areas (AOR=2.00, p=0.002) and (AOR=2.00, p=0.013) respectively. The GDHS, (2014) also reported that 56.1% of children under five years residing in rural areas used LLINs as against 35.8% urban areas 14. The difference in usage could have been as a result of the nature of buildings found in rural and urban areas. Mothers in urban areas may living in houses with trap doors, wire gauze mess, fans and even air conditioners, which may make them feel protected against malaria, hence the disparity in usage. Another reason for the lower usage of LLINs in urban areas could be due to a lot of advertisement on the radio television, bill boards and posters on the effectiveness of other methods in preventing malaria. Other methods such as mosquito coil, repellents and paints are readily available in the shops and markets in urban areas and are not expensive. Therefore, mothers could be attracted to using them.
Even though LLINs are distributed free of charge to pregnant women and children under five years and the coverage in the Hohoe Municipality is above 95% reported by Kwekeu et al, (2017) (Unpublished), this current study found that 20.8% of mothers used OMs only to prevent malaria. This was found to be higher among younger mothers less than 20 years and mothers with no formal education and those residing in urban areas. The possible reason could be that younger mothers may not have experienced the effectiveness of LLINs before. Those with no formal education may be aware of the importance of LLINs. It is also possible that mothers in urban areas may have the LLINs but because they have other methods which they think are equally effective, the LLIN is not being used.
Limitations of the Study
Limitations of this study included the fact that the study was done for only one month and the results may not reflect what happens throughout the year. Also, Information on the preferred method to prevent malaria may not be accurate because it was only collected from the respondents but not observed.
Conclusion and Recommendations
This study has revealed that the proportion of mothers who used LLINs alone for preventing malaria was low. One out of 3 mothers used LLINs only while more than half of mothers preferred using a combination of LLINs with other methods. Despite the free distribution of LLINs at the antenatal care and CWC with a coverage of over 95%, one out of 5 mothers use OMs only to prevent malaria. Older mothers, higher educational attainment and place of residence were significantly associated with methods used to prevent malaria. This could be a reflection of how LLINs are used in Ghana. Targeted educational interventions on LLINs in order to improve usage among younger mothers and mothers residing in urban areas would be required. Further studies are needed to find out reasons for using OMs only and also the reasons for the combination of LLIN with other methods. There is also the need to determine the added values of OMs to LLINs in preventing malaria.
List of Abbreviations
LLIN: Long Lasting Insecticide Treated Net, LLIN+: Long Lasting Insecticide Treated Net plus other methods, OMs: Other methods, GDHS: Ghana Demographic Health Survey; GMP: Global Malaria Programme, RBM: Roll Back Malaria, GHS: Ghana Health Service, ERC: Ethical Review Committee, WHO: World Health Organization; CWCs: Child Welfare Clinics, GHS-ERC: Ghana Health Service-Ethics Review Committee, GHS: Ghana Health Service, LLINs: MoH: Ministry of Health, MCP: National Malaria Control Program, JHS: Junior High School, SHS: Senior High School. HMMD: Hohoe Municipal Meteorological Department, HMHD: Hohoe Municipal Health Directorate. SPH: School of Public Health, UHAS: University of Health and Allied Sciences, SES: Socio-Economic Status.
Availability of Data and Material
Available upon request
Funding
None
Authors' Contributions
MK conceived the study. MK and WA, WT, RO, MA did the data analysis and wrote the methods section. MK, MA, WT, PP and ET were responsible for the initial draft of the manuscript. All authors reviewed and approved the final version of the manuscript.
Acknowledgements
We are grateful to the staff of the School of Public Health (SPH) of the, University of Health and Allied Sciences (UHAS). We are also grateful to Dr Felix Doe and the staff of the Hohoe Municipal Health Directorate (HMHD). We would like to thank the staff at the CWCs, interviewers and the mothers and their children under five years who participated in the study.
References
- 2.Wagbatsoma W A, Aigbe E E. (2010) . , ITN UTILIZATION AMONG PREGNANT WOMEN ATTENDING ANC IN ETSAKO WEST LGA, EDO STATE, NIGERIA.Nigerian Journal of Clinical Practice,13(June) 144-148.
- 3.Okpere E E.Enabudoso EJ, Osemwenkha AP.(2010)Malaria in pregnancy.Nigerian. , Medical Journal 51, 109-13.
- 4.Tobin-West C I, Kanu E N. (2016) Factors Influencing the Use of Malaria Prevention Methods Among Women of Reproductive Age in. , Peri-urban Communities of Port Harcourt City, Nigeria.https://doi.org/10.4103/1117-1936.1801. Nigerian Postgraduate Medical Journal 23, 6-11.
- 5.Murray C J, Rosenfeld L C, Lim S S, Andrews K G, Foreman K J. (2012) Global malaria mortality between1980and2010:a systematic analysis. , Lancet 379, 413-431.
- 7.Bisong C E, Dongmo C M. (2013) Utilization of malaria prevention methods by pregnant women in Yaounde. https://doi.org/10.11604pamj.2013.15.89.2324.Pan-African Medical Journal,8688 1-7.
- 8.World Health Organization.. Global Ministerial Conference on Malaria held in 1992. Amsterdam. World Health Organization , Geneva .
- 9.Chuma J, Okungu V, Ntwiga J, Molyneux C. (2010) Towards achieving Abuja targets: identifying and addressing barriers to access and use of insecticides treated nets among the poorest populations in Kenya. BMC Public Health. 10-137.
- 10. (2008) World Health Organization. Roll Back Malaria. The Global Malaria Action Plan for a Free Malaria World. Roll Back Malaria Partnership.
- 11.Ozims S J, Eberendu I F. (2014) Awareness, Ownership and Utilization of Long Lasting Insecticide-Treated Net (LLIN) among Pregnant Women Attending Antenatal Clinic. in Imo State University Teaching Hospital , Orlu , Imo State. InternationalJournal of ResearchInMedical and Health Sciences.4(8); 14-21.
- 12.Afoakwah C, Nunoo J, Andoh F K.Effect of insecticide-treated bed net usage on under-five mortality in northern Ghana.https://doi.org/10.1186/s12936-015-0827-8. , Malaria Journal 14(1), 309.
- 13.Oluwasogo A O, Henry O S, Abdulrasheed A A, Olawumi T A, Olabisi E Y. (2016) . Malaria Control and Elimination Assessment of Mother’ s Knowledge and Attitude towards Malaria Management among Under Five ( 5 ) Years Children in Okemesi – Ekiti,Malaria ControlandElimination,5(2),1–6.https://doi.org/10.4172/2470-6965/1000142 .
