Knowing, Proposing and Acting: Epistemological Aspects of Medical Practice in the New Millennium.
Abstract
In this work, it is analysed how the medical practice is imbued with Cartesian rational thought as well as empiricist thought and it is stated that medicine is an art and is science. It is proposed that the object of knowledge of the medical practice is not the concept of disease but health. It is from the concept of health and normality that medical taxonomy labels individuals as sick. This taxonomy is frequently re-evaluated and reorganized by scientific societies. This sometimes occurs according to new knowledge, but this categorization may also be questioned due to direct intervention or indirect pressure related to interests, especially economic, that are sometimes not clearly visible. Accordingly, an ongoing discussion is needed to keep the medical practice neutral against struggles of interest derived from the health industry. These topics must be considered and debated in medical schools including undergraduate and postgraduate programs.
Author Contributions
Academic Editor: Alaa Ali Mohamed Elzohry, Lecturer of Anesthesiology and Pain Management South Egypt Cancer Institute Assiut University.
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2018 Rafael Vargas
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Introduction
Within any scientific discipline, there are three fundamental questions that are articulated in epistemology. What area of reality does the discipline in question know? How do you know this reality? What is known scientifically for that discipline? These three questions apply to all areas of human knowledge, including medicine, and allow us to define scopes, actions, and limits1,2. Medical practice is imbued with Cartesian rational thought as well as empiricist thought and for many years has been stated that medicine is an art and is science3.
“What Area of Reality does Medicine Know?” - Objective of Medical Practice
For the first question, “what area of reality does medicine know?”, there is no clear answer. Although for society, including health professionals, the objective of the medical practice is tending to patients and their illness, the departure point and the axis on which the medical practice fluctuates in reality is the concept of health and normalcy. The area of reality that the clinician knows is the occasional state of a person's health insofar as he or she is susceptible to becoming ill or suffers a disease and is therefore qualified for a medical intervention, either preventive or curative, that is performed through a medical prescription. Establishing the health status of an individual at a given time is therefore the primary objective of medical practice 4, 5, 6.
The concept of health has evolved and changed periodically throughout history with accumulated knowledge and especially with the emergence of scientific societies that establish norms, revise them, eliminate them and / or modify them according to the progress of medical-scientific knowledge about health and disease7. These decisions can greatly impact the epidemiological profile of society. We can think, for example, about the criteria for dyslipidaemias diagnosis. Changing the values of lipids that are considered normal can cause a large part of the world population to be included or excluded8.
Currently, there are various definitions of health, although there is no consensus on the matter. The most accepted definition is one that presents health as the complete physical, mental and social well-being of the individual and not simply the absence of the disease9. Each of these elements that establish the concept of health, including physical, mental and social elements, are properly defined, classified, standardized and regulated, although some authors have shown that a change towards this holistic concept is not easy to apply in the medical practice10,11.
Any element that does not comply with such patterns is beyond feasible, acceptable patterns, and it is considered "abnormal." This discrepancy has obviously created a series of controversies and discussions in the biological field in which genetics, in addition to environmental, cultural, and other factors, can give rise to a series of morphophysiological variations and diversities that can be considered normal without being common11. Given the propensity in the medical field to organize and classify, many individuals are categorized and labelled as specific syndromes or diseases. This tendency to diagnose and / or overdiagnose has permeated other areas of society, which generates a tendency to medicalize life, each of its stages and even natural physiological processes12. An example of this is the increasingly important presence of medicine in fields as diverse as sports, where high-performance athletes and amateurs are inundated with concepts related to hydration, nutrition, analgesia, and anabolic processes, among others. Additionally, natural physiological phenomena, such as sleep, rest, childhood, adolescence, menstruation, sexual activity, pregnancy, childbirth and ageing, are increasingly managed from the medical point of view. This approach has led to new and modern diagnoses, such as premenstrual tension syndrome, sexual dysfunction, diverse pregnancy risks, chronic fatigue syndrome, post-holiday blues, post-Christmas blues or post-travel depression syndrome. This medicalization determines patterns of behaviour in the social domain, where a human conglomerate, whether it is a family, ethnic group or society in general, can consider an individual abnormal who does not follow the behaviours of the masses. This possibility is supported by concepts that come from medical knowledge but that are distorted by the dissemination of this information through the mass media. This form of controversy and conflict about what is considered normal and what is pathological can be related to various aspects of humanity, but perhaps one of the most frequent aspects (and the one that has generated the most discussion) is related to the brain, the mind and the diagnosis of psycho-social diseases, such as mental illnesses13. It is in this field where concepts of normality and abnormality are frequently questioned and debated. It is in this field where the incorporation of new diagnoses and the proposal of new therapies generate more tension, give rise to ruptures, new trends and new schools14. At the end of the 1960s, this type of debate was evident because it was a time in which diverse social, economic and political factors converged that generated questions at all levels of society. In the field of medicine, the nonconformity generated by rigid theories and practices of classical psychiatry favoured the development of a movement that questioned those practices and generated an anti-psychiatry movement in response15,16. All of this implies that the concept of health and / or illness is intimately linked to socio-historical moments and the forms of perception of reality that predominate in that moment. In this case, all that is valid from the medical point of view today may be totally distorted in the light of new knowledge tomorrow. However, we can affirm that in answer to the question, “Which area of reality is key to know for medical practice?” the answer is the health of the individual.
“How is this Reality known?” - Methods in Medical Practice
For the next question, “How is this reality known?”, we can see how the approach to the individual health status is achieved based on technical-operative knowledge, which is applied throughout medical practice. This approach comprises various phases that constitute the patient's medical history or medical record and that include anamnesis, physical examination, hypothesis proposals, and confirmation of the hypothesis, diagnosis and treatment.
It is important to note that in medical practice, the clinician tries to know the reality of another person following a process of thought strongly impregnated with Cartesian rationalism17, 18, 19. We can clearly see within this activity three key elements that are differentiated within the process of rationalist knowledge: a thinking subject (doctor), a thought object (patient) and an act of thought (clinical judgement).
Regarding the method of knowledge in medical practice, the requirements and characteristics that a valid method must have to reach a truth are met. In this method, the entire process of research is repeated. This movement leads to maximum simplification, which is achieved through the exploration of the patient to obtain signs and symptoms. This approach proceeds to establishing rigorous associations between these data, which is achieved using various methods. First, there is a deductive method when the diagnostic possibility is clear and unique. Second, there is a probabilistic method when the data point to a specific pathology without absolute certainty. Third, there is a falsification method when differential diagnoses are used to compare the main diagnoses with alternative diagnoses (Figure 1). With these methods, the clinician tries to generate an approximate model of perceived reality that is capable of being adjusted to existing theoretical models. In recent years, medical practice has focused on medical practices that are based on clinical evidence. In this model, pre-existing theoretical models are used, and recent or current information must be gathered to support the diagnostic or therapeutic decisions that are made20,21.
Figure 1.Medical practice process. Rational and empirical points of view participate in all clinician-patient relationships. However, rational thought implies the simplification and association of ideas and is dominant during the first step of clinical examination. Empirical thought is linked to evidence; this type of thought is necessary to form hypotheses, achieve a diagnosis and develop intervention steps.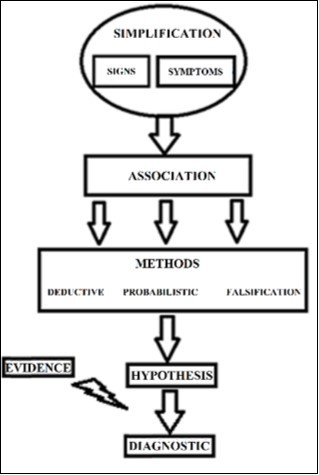
Along with this technical analysis and an approach to determine the reality of another person, clinicians can order a series of technical resources and aids. These resources include laboratory tests, imaging exams, and physiological tests. These para-clinical tests allow clinicians in many cases to clarify the diagnosis, but they cannot determine it alone22. This affirmation allows us to deduce that a medical practice supported exclusively in one of these stages or in any of these processes is weak and methodologically incorrect. However, due to the technical and economic interests that push for increasing technology use in medical practice, diagnoses are often supported only in the medical arsenal surrounding the patient. Again, it is evident that technology use in medicine has permeated aspects of common life. Some examples include sports practices that have been changed by various types of instrumentation that allow individuals to programme their level of physical activity, which allows them to monitor their physiological variables permanently and suggest what meals they must to consume according to their metabolic expenditure. In general, great advances in technology and the miniaturization of many devices have allowed daily use of devices that measure and evaluate every moment of our lives, both in wakefulness and during sleep and in sick individuals as well as in healthy individuals.
In conclusion, the answer to this second question, “How is reality known?”, is through an adequate rational and methodical medical practice that can be complemented with paraclinical tests and supported by scientific evidence.
“What is known Scientifically for Medicine?” - Scientific Basis of Medical Practice
To the third question, “What is known scientifically for medicine?”, there has always been a debate about whether medicine is an art or science23. It is stated that medicine is an art and is a subjective act that depends on intuitive, emotional aspects and on the empathy between doctors and patients. However, it is also a science because it is an objective act in which the clinician applies knowledge, techniques and interventions that have been validated and previously published in prestigious journals, which are recognized by the discipline and the bulk of the scientific community (Figure 2).
Figure 2.Medical knowledge and medical practice. Medical knowledge is inserted from all sides of clinical practice and determines the success or failure of maintaining or recovering a patient’s normal health condition.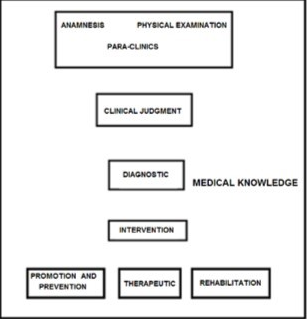
Medical Practice and Objectivity
It is argued that medicine is science more than art. The scientific basis of medical practice is supported by the fact that once a patient's data are obtained, they are examined based on biological models, natural laws, and algorithms that were previously established. The aim of the scientific basis is to tie the disorder to previous thinking to reach a diagnosis, which is the fundamental basis for medical intervention24. We see a strategy of establishing objective knowledge that establishes universal and necessary relationships between clinical phenomena. These relationships, framed within a series of laws and models, allow clinicians to propose possible outcomes of the evolution of a state or to predict effects, and all of these aspects are subject to experimental control through therapeutic activity. The establishment of such objective knowledge allows clinicians to give medical practice scientific characteristics25.
Medical Practice and Subjectivity
In medical practice, the experience of the doctor enriches the practice of the profession, which implies that there is a highly subjective component of the activity since experience is determined by aspects such as the individual’s environment, personal motivation, and commitment to society. All these factors determine whether a clinician arrives quickly and clearly at a diagnosis and an effective treatment that allows an individual to recover or maintain his or her state of health. However, another aspect that influences both the doctor and the patient is the historical-social context in which the relationship occurs. This context includes aspects such as the state of science and medical knowledge, assessment and position of a social group or of society with respect to certain types of diseases (the Black Death, Hansen's disease, syphilis, AIDS, etc.), the social value of the sick individual and the position of the individual in the family and society. All of these factors determine the scientific nature of medical knowledge and its validity23,25.
Medical Practice and Diagnostic Certainty
One of the fundamental elements to support clinical diagnosis is the reliability of paraclinical supports. These supports include laboratory tests (biopsies, analysis of body fluids, bacteriological tests, etc.), imaging tests (endoscopies, X-rays, tomography, PET, etc.) or physiological tests (stress tests, haemodynamic studies, electrophysiological studies, etc.). The trustworthiness of the doctor-patient relationship will add factors, such as the validity of the analysis of an isolated organic segment of an entire organic macrocosm in pathological analyses. This implies answering the question of whether one can know the whole from one of its parts. Will tissue behaviour be equal to being isolated amid totally strange chemical substances when it belongs to an integral organism? What validity can an individual's reading have on a fragment of reality of a being that he vaguely knows?8.
However, the technical failures that occur in the control and measurement equipment, the lack of maintenance and calibration, and the use of these equipment by untrained or inexpert personnel can generate erroneous data, giving rise to inaccurate interpretations and misdiagnoses. Even if an adequate procedure is performed in a clinical exercise, supported by a series of serious and reliable paraclinical examinations and leading to a clear and indubitable diagnosis, the problem of the narrow therapeutic capacity of current resources is added. There are diverse elements, substances and actions that are used to control (not always cure) a series of pathologies; however, these elements must be administered once a clear diagnosis is made to avoid undesirable responses in individuals. Although the diagnosis could be accurate and the therapy effective, there is always an uncertain point: biological variability and the patient’s responses before the curative element is administered and / or changes in the behaviour of an exogenous element. These are adverse reactions, side effects, and idiosyncratic reactions that can cause disorders that in many cases are lethal for the patient. There is also concern that despite careful and judicious clinical exercise as well as sufficient paraclinical support, inaccurate or erroneous diagnoses could be made that could lead, most likely, to therapeutic behaviours that are not harmful, or are at least innocuous, which may imply a progressive and irreversible progress of the pathology in question26,27.
Medical Practice and Chain of Trust Agreements
Although here there is no reflection that follows the characteristic patterns of a proper philosophical reflection, since the physician moves within the probable, the steps that are carried out to clarify signs and symptoms are permeated with the scientific method, including observation, order and disposition to reach the truth. This is a truth that is probably volatile and temporal (the diagnosis of a disease made two centuries ago is probably not the same when evaluated by today's doctor) and depends on the non-rupture of a labile chain of trust that ties the participants of medical practice. A doctor trusts the word of others (patient, family). The patient trusts the wisdom and the doctor´s skills. Both rely on the skills and technical capacity of a third party that processes and analyses samples to send a report that makes the diagnosis possible (technicians and associate professionals). The doctor also trusts what is achieved by science and technology through thousands of studies and experiments (medical knowledge), which allows him to preserve or recover an ideal state of health in the patient28. The patient relies instinctively on the same things. Any failure in this chain of trust can ruin the medical practice. This disruption can cause the loss of credibility for medicine and force the patient to seek refuge in other medical systems that offer what apparently allopathic medicine cannot offer: security, trust, and hope, among other things29,30.
Conclusion
The basis of medical knowledge is the concept of health. It is from the concept of health and normalcy that medical taxonomy emerges, which labels the individual a sick individual. This taxonomy is frequently re-evaluated and reorganized by scientific societies. Sometimes the re-evaluation is based on new knowledge, whereas other times this reorganization of the classification of diseases is questioned when it is evident that it is carried out by interventions or pressure exerted by individual groups, which could be patient associations, health institutions or economic corporations that defend particular interests. Therefore, an ongoing discussion is needed to guarantee that medical practice remains neutral in the face of the strong interests of health-related businesses. All these aspects around medical knowledge and the relationship with medical practice must be considered and debated in medical schools during undergraduate and postgraduate medical training.
Disclosures
I confirm that I do not have any conflicts of interest in relation to this article. No ethical issues are involved.
References
- 1.Weatherall D J. (2004) Philosophy for Medicine. , Journal of the Royal Society of Medicine 97(8), 403-405.
- 2.Tosam M J. (2014) The role of philosophy in modern medicine. , Open Journal of Philosophy 4(01), 75.
- 3.Lanier W L, Rajkumar S V. (2013) Empiricism and rationalism in medicine: can 2 competing philosophies coexist to improve the quality of medical care?. In Mayo Clinic Proceedings 88(10), 1042-1045.
- 4.Hesslow G. (1993) Do we need a concept of disease?. , Theoretical Medicine and Bioethics 14(1), 1-14.
- 5.Lennox J G. (1995) Health as an objective value. , The Journal of medicine and philosophy 20(5), 499-511.
- 6.Mordacci R. (1995) Health as an analogical concept. , The Journal of medicine and philosophy 20(5), 475-497.
- 9.Azevedo M A. (2015) Health as a clinic-epidemiological concept. , Journal of Evaluation in Clinical Practice 21(3), 365-73.
- 10.Engel G L. (1977) The need for a new medical model: a challenge for biomedicine. , Science 196(4286), 129-136.
- 11.Alonso Y. (2004) The biopsychosocial model in medical research: the evolution of the health concept over the last two decades. Patient Education and Counseling. 53(2), 239-244.
- 12.W van Dijk, Faber M J, Tanke M A, Jeurissen P P, Westert G P. (2016) Medicalisation and Overdiagnosis: What Society Does to Medicine. , International Journal of Health Policy and Management 5(11), 619-622.
- 13.Boorse C. (2013) On the distinction between disease and illness. In Meaning and Medicine. Routledge 30-41.
- 14.Wakefield J C. (1992) The concept of mental disorder: on the boundary between biological facts and social values. , American Psychologist 47(3), 373.
- 16.Harari E. (2001) Whose Evidence? Lessons from the Philosophy of Science and the Epistemology of Medicine. , Australian and New Zealand Journal of Psychiatry 35(6), 724-730.
- 17.Shapin S. (2000) Descartes the doctor: Rationalism and its therapies. , The British Journal for the History of Science 33(2), 131-154.
- 18.Newton W. (2001) Rationalism and empiricism in modern medicine. Law and contemporary problems. 64(4), 299-316.
- 19.Rodríguez M D, Hernández A G, González A C, Pi O F. (2010) Descartes’ influence on the development of the anatomoclinical method. , Neurología (English Edition) 25(6), 374-377.
- 20.Shryock R H. (1969) Empiricism Versus Rationalism in American Medicine. In Proceedings of the American Antiquarian Society 79(1), 99.
- 21.Newton W. (2001) Rationalism and empiricism in modern medicine. Law and contemporary problems. 64(4), 299-316.
- 22.Walter E. (1985) Testing and Estimating the Sensitivity and the Specificity of Diagnostic Procedures. In Methodical Problems in Early Detection .Springer,Berlin,Heidelberg. Programmes 116-122.
- 23.Saunders J. (2000) The practice of clinical medicine as an art and as a science. , Medical Humanities 26, 18-22.
- 24.Jankowska D, Milewska A J, Górska U. (2010) Applications of logic in medicine. Studies in Logic, Grammar and Rhetoric 21(34), 7-24.
- 25.Cunningham T V. (2015) Objectivity, Scientificity, and the Dualist Epistemology of Medicine. In: Huneman. Disease and Evidence. History, Philosophy and Theory of the Life Sciences,Springer,Dordrecht 7.
- 26.Hodgkin P. (1996) Medicine, postmodernism, and the end of certainty. , BMJ: British Medical Journal 313(7072), 1568.
- 27.Gillett G. (2004) Clinical medicine and the quest for certainty. , Social Science and Medicine 58(4), 727-738.
