Volvulus of the Small Bowel Due to Malrotation During Pregnancy: A Case-Report
Abstract
Volvulus occurring during pregnancy is a rare complication, still potentially lethal nowadays for both the mother and child due to several, early arising complications. We report here a case of small bowel volvulus in a 28 weeks and 4 days, 29 years-old, pregnant woman with a past medical history of appendectomy in her childhood. Patient presented in emergency department with abdominal pain and abnormal hepatic tests. Cholangio-MRI suggested bowel obstruction due to volvulus that was confirmed by gastroscopy (showing the obstruction) and intestinal MRI. Patient was first treated by laparoscopy but, due to a very complicated abdominal status with the presence of several adhesions of the small bowel, surgery was changed to an open laparotomy, which allowed discovery and repositioning of small bowel malrotation and removal of adhesions. Both patient and the foetus were healthy after surgery and the patient was then discharged. In the light of this particularly rare case of small bowel volvulus due to malrotion, we will describe the pathology of bowel obstruction and more particularly volvulus during pregnancy and discuss its diagnosis and treatment.
Author Contributions
Academic Editor: Rongbiao Tang, Ruijin hospital
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2017 Paul E Constanthin , et al
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Introduction
Bowel obstruction occurring during pregnancy (with an incidence between one in 1500 and one in 66’431 (Aftab et al, 2014))1 is a rare complication potentially lethal for both the mother and child. Less than a hundred cases of this pathology have been reported and its causes can be very different, one of them, but not the most frequent, being intestinal volvulus. Intestinal volvulus most frequently interests the sigmoid colon due to its modified position during pregnancy, particularly its displacement during third trimester, but other regions have been reported to be involved. Due to the rarety of this entity and the absence of any specific symptom or laboratory test, early diagnosis, as well as treatment, remains of extremely complicated despite their importance (Aftab et al, 2014)1. We report here a new case of a rare form of small bowel volvulus due to a malrotation in a 28 weeks and 4 days pregnant, 29 years-old female with a past medical history of appendicitis. We then discuss diagnosis of volvulus during pregnancy and its treatment, which both need to be initiated early during patient management to not risk a tragic outcome for both mother and child.
Case-Report
A 28 weeks and 4 days pregnant, 29 years-old female, known for an L4-L5 discopathy and a past history of surgery for appendicitis at the age of 10 (right-positioned appendix, not perforated), consulted with vomiting and abdominal pain in the epigastric region. Eating and drinking had become impossible at that point. Blood tests revealed pathologically elevated white blood cells count (11.4 G/l for a normal value of 4-10 G/l) and elevated hepatic tests. Preeclampsia and HELLP syndrome were ruled out, as were frequent causes for hepatitis (virus, medicines, auto-immunity). Abdominal echography did not reveal any sign of cholecystitis or pancreatitis and testing for urinary cause was negative. The second blood tests revealed a worsening of the hepatic tests, reason why the patient underwent a cholangio-MRI. This test did not reveal any biliary lesion but volvulus was suspected due to apparent intestinal malrotation. Obtruction was confirmed by gastroscopy (without scope) and situated at the level of the jejunum. Final confirmation of obstruction and its position in the abdomen was also obtained through intestinal MRI (see Figure 2A, Figure 2B, Figure 3). During this time, the patient never displayed any gynaecological signs and foetal echography revealed a foetus with cephalic position, weighting 1300g and a posteriorly inserted healthy placenta with a Manning score of 10/10. The patient was referred for surgery. She underwent an exploratory laparoscopy that revealed multiple adhesions of the small intestine. Volvulus of the small intestine was identified just at the level of the duodeno-jejunal angle, situated on the right side of the aorta. Removal of the adhesions was attempted but ended up causing a small lesion of the small intestine, prompting the transformation of the laparoscopy into an open laparotomy. The laparotomy revealed a volvulus of the small intestine with common mesentery, with encircling of the caecum, the last part of the ileum and the beginning of the jejunum by the omentum. Resolution of the volvulus showed absence of intestinal rotation at the duodeno-jejunal angle, confirming the presence of malrotation. Mesentery was repositioned (without Ladd’s procedure) and fixation of the right colon to the right peritoneum was performed. The small intestine, which showed no sign of ischemia, was sutured and adhesions were completely removed. A few hours after the surgery, the patient presented with uterine contractions every two minutes and uterine ultrasonography showed a 33mm cervix. Tocolysis was immediately given with good results and the contractions definitely ceased and did not reappear two days later when treatment was stopped. During her stay, the patient presented with left basal pneumonia that was treated with antibiotherapy. She completely recovered during the following days and was then discharged with no further complication. The rest of her pregnancy went without any other complication and the patient delivered with instrumentation (Kiwi-sucker) at the age of 40 weeks and 0 days due to a suspect cardio-tocogramm and absence of delivery progression. Both baby and mother were healthy and they were then discharged with no further complication
Figure 2A.Axial contrast-enhanced MRI scans show characteristic whirpool appearance of bowel and mesentery wrapping around superior mesenteric artery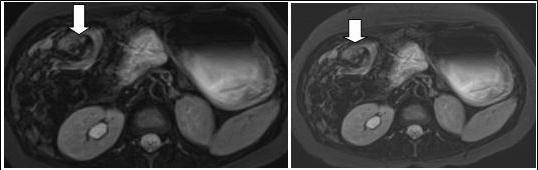
Figure 2B.Axial contrast-enhanced MRI scans show characteristic whirpool appearance of bowel and mesentery wrapping around superior mesenteric artery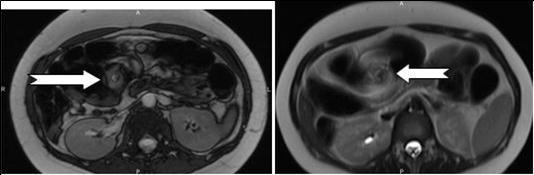
Figure 3.Coronal reformatted image shows contrast agent–filled small bowel on right
Discussion
Intestinal obstruction occurring during pregnancy is a rare (its incidence being between one in 1500 and one in 66’431 (Aftab et al, 2014))1, extremely dangerous complication. In their review of the literature, Aftab et al 1underlined that less than a hundred cases had been reported since the first description of this pathology by Houston in 1830 (Aftab et al, 2014)1. Intestinal obstruction can be caused by many conditions, including congenital or post-operative abdominal adhesions, volvulus, intussusception, hernia, masses of the colon and appendicitis (Aftab et al, 2014; Cong et al, 2014; Shui et al, 2011).1, 4, 12 Volvulus of the sigmoid colon is the most common cause, this being due to its position in the pelvis making it at risk of being pushed upwards out of the pelvis and rendering its mesentery at risk for torsion and secondary vascular insufficiency, this risk being increased during all the pregnancy and particularly the last trimester (Wax et a, 1993; Aftab et al, 2014; Shui et al 2011).14, 1, 12However, the entire gastro-intestinal tract can in fact be at risk for volvulus during pregnancy (Cong et al, 2014).4 The risk is even higher in conditions in which a reduction in the available space is present, like congenital malrotation (Figure 1, Pickhadt et Bhalla, 2002)9, multiple pregnancy or adhesions (Shui et al, 2011)12. Among the other forms of volvulus during pregnancy, midgut volvulus, which comprises small bowel volvulus, presents with the common symptom of small bowel obstruction (Webster et al, 2015)15, which can potentially lead to dramatic consequences for the mother (mortality rate 6-20%) and the foetus (mortality rate 20-26%) (Aftab et al, 2014; Cong et al 2014)1, 4. This particularly bad outcome is mostly due to diagnostic issue. Indeed, typical symptoms of bowel obstruction include nausea, vomiting and abdominal distension, these symptoms being fairly common during normal pregnancy (Aftab et al, 2014; Cong et al, 2014)1, 4. Other signs may include signs of shock, constipation and abdominal pain (Aftab et al, 2014)1. However, many other pathological conditions like preeclampsia or HELLP syndrome may present with those signs and intestinal obstruction by small bowel volvulus may be overlooked. Thus, a complete and thorough physical examination completed by blood tests and imagery should always be considered in front of such a patient. One particular point that should make clinicians extremely cautious is that blood tests can be misleading because non-specific in the case of small bowel volvulus. Our case is particularly interesting in this aspect because blood tests came back as normal except for an elevated white blood cells count and the results of the hepatic tests, which worsened with time, orienting the diagnosis towards the hepato-biliary tract and prompting realisation of a cholangio-MRI. Luckily, this test suggested the right diagnosis and we were able to confirm it with gastroscopy and then with intestinal MRI (to further define small bowel and colon position before the surgery). To our knowledge, this case is the first in which small bowel volvulus presented only with hepatic tests modification and this not only warrants further research in the field but also underlines the difficulty in the diagnosis of this condition.
Figure 1.—Schematic drawings of normal rotation and malrotation (from Pickhart et Bhalla, 2002). A, Drawing shows that normal 270° rotation and fixation of midgut results in familiar positioning of bowel with broad mesenteric attachment (dotted line). B, Drawing shows that malrotation results in malpositioned bowel and narrow base of mesenteric fixation (dotted line), which is prone to midgut volvulus. Abnormal fibrous peritoneal bands of Ladd (curved lines) that attach to right colon predispose to internal hernia in older patients.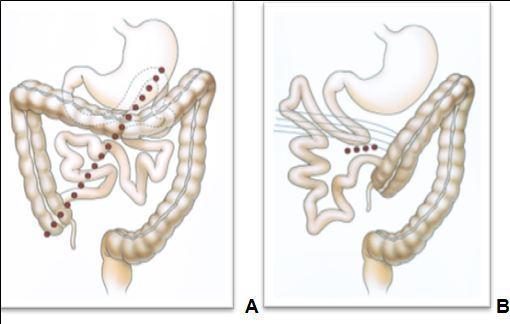
In that aspect, small bowel volvulus should always remain in the differential diagnosis in front of a pregnant woman presenting with abdominal pain during pregnancy, especially one like ours that was known for a previous surgery for appendicitis (a possible reason for the presence of the adhesions). Radiologic diagnosis of small bowel volvulus can be done by several technics. Plain abdominal film can be used, showing sometimes a typical pattern of dilated loops, but more often showing a normal radiological pattern due to a proximal position of the volvulus (with the loops being filled with liquid). Evidences on CT-scan are the presence of dilated bowel loops, intramural gas and the “whirlpool sign” (Cong et al, 2014; Shui et al, 2011)4, 12, but the use of technics exposing the foetus to radiations is debated. However, in their review, Cong et al 4emphasized the fact that those technics (and particularly plain radiography) are considered safe for the mother as well as for the foetus (Cong et al, 2014)4. MRI is also safe and extremely precise in the diagnosis of small bowel obstruction (Vassiliou et al, 2012)13, sometimes also showing the “whirlpool sign” (Kouki et al, 2013)7 and ultrasonography has been reported to be useful in some instances (Cong et al, 2014)4 but it can also remain completely negative. In our case, while cholangio-MRI suggested the diagnosis, final diagnosis was given by intestinal MRI, showing a possible role for this technic in some unusual cases, in which doubts about the diagnosis or about the state of different abdominal structures remain. However, in cases in which clinical symptoms, laboratory and more basic radiological (plain abdominal film of CT-scan) are highly suggestive of this pathology, exploratory surgery should be started at the earliest time possible.
First-choice treatment for volvulus during pregnancy is surgery. While sigmoid volvulus can be treated endoscopically, particularly during early pregnancy (Aftab et al, 2014),1 small bowel volvulus during pregnancy almost always warrants transformation into or immediate laparotomy (Aftab et al, 2014). 1However, due to the time needed for diagnosis, irremediable damages might occur to the intestine and surgeons might need to resect some part of the intestine if gangrene is observed (Baykal et al, 2006)2. Sometimes, the delay for diagnosis will even bring the dramatic outcome that is the death of the mother of the foetus (Gaikwad et al, 2010; Hwang et al, 2014; Nameirakpam et al, 2014)5, 6, 8. Very importantly, mothers that underwent surgery should always be carefully monitored after the intervention because small bowel volvulus has been reported to recur (Yahchouchy et al, 2001)16. Foetal health should also always be monitored and tocolysis should be administered in the case of contractions, as was done in this case. If necessary, delivery of the foetus might be done at the same time as the surgery but it does not always suppress the risk of small bowel volvulus. Indeed, small bowel volvulus can also occur after delivery (Shere et Abulafia, 2001, Coder et al 1976; Ranjan et al, 1993)11,3,10. In our case, we were able to supress contractions with tocolytics and no premature delivery was needed.
In this article, we presented a case of small bowel volvulus during pregnancy that not only confirmed some already known facts about this pathology but also enlightened new ones, notably on the risks of the non-specificity of blood tests. Indeed, in front of a patient with high-level suspicion (due to medical history or symptoms), rapid decision to perform surgery should be taken to avoid tragic outcomes. All in all, our case shows that there is still much to understand about bowel obstruction during pregnancy (and particularly small bowel volvulus) and, in the interest of the patients, diagnosis should be made promptly to prevent the aforementioned dramatic outcomes and we are absolutely convinced that further refinement of the actual diagnosis technics and development of future ones is of paramount importance.
Conclusion
Small bowel volvulus is a rare, potentially lethal complication of pregnancy. Particular attention should be taken in front of any pregnant woman presenting with gastro-intestinal signs and prompt diagnosis and treatment are the key to a positive outcome of such pathology.
References
- 1.Aftab Z, Toro A, Abdelaal A. (2014) Endoscopic reduction of a volvulus of the sigmoid colon in pregnancy: case report and a comprehensive review of the literature. , World J Emerg Surg; 9-41.
- 2.Baykal C, Al A, Ozer S, Hizli D, Gökçin H. (2006) Ileal resection for gangrenous ileal volvulus in a term pregnancy: a case report. Arch Gynecol Obstet;273:. 304-306.
- 3.Coder D M, Schewitz L J, Falls H C.Midgut volvulus following cesarean section. , Obstet Gynecol 1976, 231-233.
- 4.Cong Q, Li X, Ye X. (2014) Small bowel volvulus in mid and late pregnancy: can early diagnosis be established to avoid catastrophic outcomes. , Int J Clin Exp Med;7: 4538-4543.
- 5.Gaikwad A, Ghongade D, Kittad P. (2010) Fatal midgut volvulus: a rare cause of gestational intestinal obstruction. Abdom Imaging;35:. 288-290.
- 6.Hwang S M, Na Y S, Cho Y, You D G, Lee J J. (2014) Midgut volvulus as a complication of intestinal malrotation in a term pregnancy. , Korean J Anesthesiol;67:S98-9
- 7.Kouki S, Fares A, Alard S. (2013) MRI whirpool sign in midgut volvulus with malrotation in pregnancy,JBR-BTR;96:. 360-361.
- 8.Nameirakpam S, Keishing S, Laishram J, S R Devi. (2014) Small Intestine Ischaemia due to Volvulus during Pregnancy. , J Clin DiagnRes;8:ND0 1-2.
- 9.Pickhardt P J, Bhalla S. (2002) Intestinal malrotation in adolescents and adults,AJR;179;. 1429-1435.
- 10.Ranjan V, Boulton J M. (1993) Primary volvulus of the small bowel following normal delivery. , Br J Obstet Gynaecol;100: 860-861.
- 11.Sherer D M, Abulafia O. (2001) Postcesarean small bowel volvulus. Case report and review of the literature. Gynecol Obstet. Invest;51: 69-72.
- 12.Shui L H, Rafi J, Corder A, Mowbray D.Mid-gut volvulus and mesenteric vessel thrombosis in pregnancy: case report and literature review. Arch Gynecol Obstet. , 2011;283 Suppl 1, 39-43.
- 13.Vassiliou I, Tympa A, Derpapas M, Kottis G, Vlahos N. (2012) Small Bowel Ischemia due to Jejunum Volvulus in Pregnancy: A Case Report. Case Rep Obstet Gynecol;2012:. 485863.
- 14.Wax J R, Christie T L. (1993) Complete small-bowel volvulus complicating the second trimester. Obstet Gynecol;82:. 689-691.
Cited by (9)
This article has been cited by 9 scholarly works according to:
Citing Articles:
Case Reports in Obstetrics and Gynecology (2021) Crossref
Case Reports in Obstetrics and Gynecology (2021) OpenAlex
A. Stephens, S. Wagner, B. Pineles, E. Soto - Case Reports in Obstetrics and Gynecology (2021) Semantic Scholar
E. Chong, David S. Liu, Vishnupriya Rajagopal, N. Strugnell - BMJ Case Reports (2020) Semantic Scholar
Obstetrics and Gynecology International (2020) Crossref
Obstetrics and Gynecology International (2020) OpenAlex
E. Chong, David S. Liu, N. Strugnell, Vishnupriya Rajagopal, K. Mori - Obstetrics and Gynecology International (2020) Semantic Scholar
European Journal of Medical and Health Sciences (2020) OpenAlex
European Journal of Medical and Health Sciences (2020) Crossref
D. Shyam, R. Shyam - (2020) Semantic Scholar
Journal Of Digestive Disorders And Diagnosis (2017) OpenAlex
