Cytomegalovirus Esophagitis: Two Patients with Different Features
Abstract
Two cases of CMV esophagitis presenting with distinct clinical and endoscopic features are presented. Diagnostic clues, histopathology, and antiviral therapy considerations are highlighted, emphasizing vigilance in immunocompromised hosts.
Author Contributions
Academic Editor: DiveyManocha, Upstate Medical University,United States
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2016 Huwi-Chun Chao, et al
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Letter To The Editor :
Esophageal ulcer bleeding due to CMV infection is quite infrequent in clinical practice. We reported two cases presenting with different patterns of esophageal ulcer, which was confirmed as CMV esophagitis. Our report would remind physicians the unusual occurrence of the CMV-related esophageal ulcer bleeding in the intensive care unit patients.
Cytomegalovirus (CMV) usually causes opportunistic infections in immunocompromised patients. Active CMV disease occurred in up to 36% of critically ill patients and may affect their health outcomes 1, 2. We present upper gastrointestinal (UGI) bleeding with different endoscopic features of CMV esophagitis in two patients hospitalized in intensive care units (ICUs) - one immunocompetent patient who stayed in ICU for a critical illness and a second patient with colon cancer who received tegafur/uracil chemotherapy.
Case 1
A 77-year-old woman with diabetes mellitus and coronary artery disease had short of breath in recent days. Cough with sputum, mild chest tightness, and poor appetite were noted. She was admitted to the ICU and sputum cultures yielded carbapenem-resistant Acinetobacter baumannii(CRAB). Antibiotic therapy with doripenem plus sulbactam was given for 10 days. Meanwhile, unstable hemodynamic status and upper gastrointestinal bleeding occurred. Panendoscopic study showed diffuse ulcers of whole esophagus (Figure 1A). The CMV- polymerase chain reaction (PCR) results for blood and stool samples were positive. The CMV antigenemia showed 23 positive cells per 200,000 macrophages. Biopsy of esophageal ulcers revealed some large cells containing eosinophilic inclusion, which was positive in the immunohistochemical staining for CMV. Ganciclovir was added and esophageal bleeding stopped soon. One week later, nevertheless, the patient passed away in the hospital due to worsening CRAB pneumonia.
Figure 1.Endoscopy is showing diffuse ulcers of whole esophagus (1A) and pseudomembranous lesions with irregular yellowish patch along upper and lower esophagus (1B).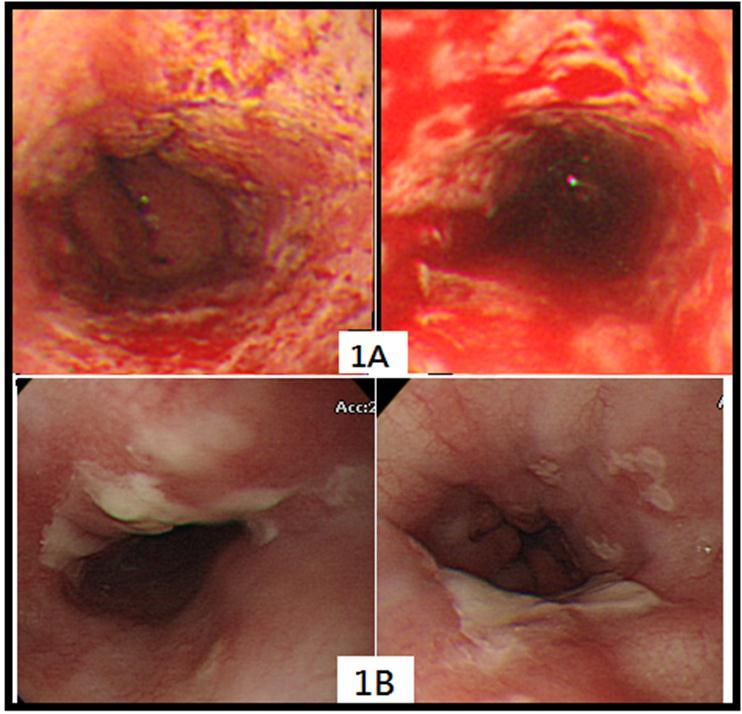
Case 2
A 75 y/o man of diabetes and colon cancer post hemicolectomy had received tegafur / uracil chemotherapy. He suffered from nausea, vomiting and hematemesis for one week. The laboratory data showed leukocytosis and panendoscopy revealed pseudomembranous lesions of the esophagus (Figure 1B). Esophageal biopsy showed CMV infection. The blood and stool CMV- PCR results were positive. A viral load of blood sample was 12,200 IU/mL. After ganciclovir therapy, the esophageal bleeding subsided and he was uneventfully discharged.
CMV diseases have been reported in immunocompromised patients especially with acquired immunodeficiency syndrome and solid organ transplant. Beside, in critically ill patients, CMV infection is associated with prolonged ventilator support, nosocomial infections, prolonged hospital stay and increased mortality 1. Many clinicians neglect CMV colitis in the critically ill patients 3. But there have been a few reports of serious complications, such as massive intestinal bleeding and intestinal perforation in the critically ill immunocompetent patients 3, 4.Therefore, a high level of suspicion for CMV disease is required when diagnosing critically ill patients with gastrointestinal symptoms, and endoscopic biopsies should be taken from all gastrointestinal tract lesions to detect CMV in the cytomegalic inclusion bodies.
The CMV esophagitis is rarely highlighted in critically ill patients. The most common lesions were well-circumscribed ulcers, usually located in the middle to distal parts of the esophagus 5. As we know, the pseudomembranous CMV lesions have been seen in the colitis but not reported in the esophagitis 3. The intensivists should early diagnose the active CMV disease and to assess those patients who might preferably be given antiviral treatment.
Conclusion
We report two cases of esophageal bleeding lesions, which mucosal pathology confirmed CMV esophagitis. Our cases highlight different endoscopic features of CMV esophagitis among non-immunocompromised and immunocompromised patients in the ICUs. Our report would remind physicians the unusual occurrence of esophageal lesions due to CMV infections.
Conflict of Interests
We declare no conflict of interest and financial support regarding this letter.
Ethics Statement
The above study has been granted exemption from review by the Institutional Review Board of Chi-Mei Medical Center (IRB Serial No. 10410-005).
References
- 1.Kalil A C, Florescu D F. (2009) Prevalence and mortality associated with cytomegalovirus infection in nonimmunosuppressed patients in the intensive care unit. , Crit Care Med 37, 2350-8.
- 2.Papazian L, Hraiech S, Lehingue S, Roch A, Chiche L et al. (2016) Cytomegalovirus reactivation in ICU patients. , Intensive Care Med 42, 28-37.
- 3.Chan K S, Yang C C, Chen C M, Yang H H, Lee C C et al. (2014) Cytomegalovirus colitis in intensive care unit patients: difficulties in clinical diagnosis. , J Crit Care,29: 474, 1-6.
