Abstract
Overview:
Dementia is a serious brain disease that impacts negatively in several areas of patient’s functioning. Depression has a strong link with dementia and is part of the behavior and psychological symptoms (BPSD). Behavior management for depression is recommended as a first-line psychological treatment for dementia patients. However, there are no systematic reviews examining the efficacy of behavior management for depression in dementia.
Objective:
To examine the efficacy of behavior management (BM) for depression in dementia patients.
Methods:
Five electronic databases were searched (1999 to 2015) for randomized controlled trials (RCTs) which were selected according to eligibility criteria. Data was pooled, quality assessment was completed, and a meta-analysis was performed.
Results:
This review included ten randomized controlled trials. In the four studies where behavior management was a focused intervention, no significant treatment effect was observed (standardized mean difference SMD -0.20; 95 % CI -0.96 to 0.56). In the remaining six studies in which behavior treatment was involved as a component, the analysis showed a trend favored the intervention, but it was not significant (SMD -0.12; 95 % CI -0.25 to 0.01).
Conclusion:
There is no evidence for behavior management alleviating depression in dementia patients. Future research examining the efficacy of specific behavior management techniques for milder forms of dementia and multimodal interventions are recommended.
Author Contributions
Academic Editor: Ian James Martins, Edith Cowan University
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2018 Win K. Thu, et al.
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Introduction
Dementia is a chronic progressive brain disease characterized by impairments of cognitive function which usually accompanied by deterioration in emotional control, social behavior, and/or motivation (World Health Organization WHO, 2015)22. The number of people suffering from dementia has been increasing proportionately as the global population ages. A review by Alzheimer’s Disease International estimated that the global prevalence of dementia in 2015 was 46.8 million, and this figure would project to 74.7 million in 2030 (Prince et al., 2015).15
Besides the decline in cognitive functioning, most dementia patients also suffer episodic patterns of behavior and psychological symptoms of dementia (BPSD) throughout the illness (Kales, Gitlin & Lyketsos, 2015)7. BPSD is defined as “symptoms of disturbed perception, thought content, mood or behaviors that frequently occur in patients with dementia” (Finkel, Costa e Silva, Cohen, Miller, & Sartorius, 1997)4. Depression is a feature of BPSD, Zubenko et al. (2003)23 found the prevalence of depression ranged from 22.5% to 54.4%. Similarly, in a five-year prevalence study of neuropsychiatric symptoms of dementia in a community setting, the point prevalence of depression at baseline and last three visits varied between 29 to 47%. Seventy-seven percent of dementia patients suffered from depressive symptoms during the study period (Steinberg et al., 2008)17.
Depression is regarded as both a risk factor and a consequence in relation to Alzheimer’s disease (Taylor, Paton, & Kapur, 2015)18. Diagnosis, treatment and provision of care for the dementia patients with depression are challenging. Depression is difficult to diagnose in dementia patients because these patients are less likely to report their symptoms due to the presence of memory impairment and language difficulties; and also, because of the presence of agitation, weight loss, sleep disturbance and apathy in advanced dementia may mimic depressive symptoms (International Psychogeriatric Association IPA, 2012)6. The presence of depressive symptoms negatively impacts dementia patients by diminishing the quality of life and may result in early hospitalization and increased mortality. It also impacts caregiver well-being by increasing the burden of care (IPA, 2012; Ornstein & Gaugler, 2012; Pattanayak & Sagar, 2011)6,12,13.
Pharmacological treatment of depression in dementia is challenging due to lacking efficacy data and clinical controversies on the use of antidepressants. Although a systematic review found an improvement in depression scores with clomipramine (a tricyclic antidepressant) and sertraline (a selective serotonin reuptake inhibitor-SSRI) the authors stated that the findings were difficult to generalize due to small sample size of the studies reviewed (Bains, Birks, & Dening, 2009)2. Moreover, tricyclic antidepressants are not prescribed commonly in the clinical practice for the elderly because of potential side effects. Similarly, a systematic review of dementia guidelines supports the use of SSRI (e.g., sertraline, citalopram) in dementia patients with depression (Azermai et al., 2011)1. However, the recent Maudsley Guidelines (2015), states only that “use of SSRIs may be justified in some cases, and the effect is modest at best and supporting evidence is weak”. (Taylor, Paton, & Kapur, 2015)18
A wide range of non-pharmacological interventions such as multisensory stimulation, music therapy, BM, bright light therapy and psychotherapies are practiced to prevent or manage BPSD with varying degree of evidence. A systematic review of dementia guidelines recommended the use of the non-pharmacological interventions as first line therapy to treat BPSD (Azermai et al., 2011)1. A controlled trial of behavior therapy has been shown to result in a significant improvement in symptoms of depression in behavior treatment group compared with the waiting list control and with typical care in the early stages of Alzheimer (Teri, Logsdon, Uomoto, & McCurry, 1997)20. Similarly, a randomized controlled trial of a multimodal intervention stated that the combination of the exercise program in Alzheimer’s patients and caregiver training of BM resulted in improvement of depression (Teri et al., 2003)19,34. In the same way, Scottish Intercollegiate Guidelines Network – SIGN (Network SI, 2006)16 and the systematic review of dementia guidelines by Azermai et al. (2011)1 also recommend music and BM to treat depression in dementia patients.
Although there are many systematic reviews and dementia guidelines recommending the use of BM as one of the first line non-pharmacological interventions for the management of BPSD in general, there is only a limited number of studies focusing on the reduction of any behavior and psychological symptom (e.g., depression, wandering). To our knowledge, there had been no systematic review investigating the efficacy of BM for depression in dementia patients. This systematic review is aimed at evaluating the efficacy of BM for depression in dementia patients.
Methods
Study Protocol
The study protocol was reviewed by two Ph.D. level researchers (third and fourth authors) and approved by the University of Queensland Medical and Human Research Ethics Committee.
Inclusion Criteria
Types of Studies
Randomized controlled trials that included BM delivered to dementia patients compared with control conditions or usual care, and that assessed depression as an outcome measure using validated measuring instruments were included in this review. Usual care might include routine psychosocial supports, routine medical care for dementia, medication for physical conditions, family education, and other support.
Types of Participants
Participants included in this review were all types of dementia patients (e.g., Alzheimer’s, vascular, dementia with Lewy body, frontotemporal dementia and others) in any setting (e.g., home, residential housing). Dementia could be diagnosed either clinically by psychiatrists or physicians; by using available diagnostic classification systems (e.g., International Classification of Diseases ICD, Diagnostic and Statistically Manual of American Psychiatric Association DSM); or by using cognitive function assessment scales (e.g., Mini-Mental State Examination – MMSE, Clinical Dementia Rating Scale - CDR).
Types of Intervention
Behavior management is a structured and systematically applied and time-limited intervention, usually provided by caregivers under an expert supervision (Network SI, 2006)16. For the purpose of this review, behavior management included behavior therapy, behavior intervention, behavior modification and functional analysis (Kasl-Godley & Gatz, 2000; McGee & Bratkovich, 2011; Network SI, 2006)8,16. Behavior management applies learning principles and aims to reduce the occurrence of undesirable behaviors or to increase desirable behaviors. A baseline for target behavior change is usually identified through functional analysis where the undesirable behavior, its antecedents and consequences are observed and managed (Kasl-Godley & Gatz, 2000). Usual procedures include contingency principles (e.g., positive and negative reinforcement, punishment and extinction); indirect contingency management (e.g., verbal control, distraction and environmental modification); behavioral rehearsal and relaxation training (Kasl-Godley & Gatz, 2000; McGee & Bratkovich, 2011)8. In the reviewed studies BM also included increasing pleasant events as well as problem-solving strategies to alter the contingencies that related to depression and associated behavior disturbance (Teri et al., 1997)20. Among the reviewed studies BM was delivered as a sole intervention or as part of a number of interventions. In most studies caregivers also provided BM under an expert supervision. In these studies caregiver training supported therapist intervention and included problem-solving, coping strategies and using reinforcement to manage behavior associated with low mood. BM was often used in conjunction with basic cognitive strategies such as the identification of negative thoughts, and simple cognitive restructuring. It was not possible to fully differentiate separate effects for the BM and cognitive techniques; however, there was no difference in effectiveness for BM only compared to BM with simple with cognitive techniques.
Types of Outcome Measures
The primary outcome was the measurement of severity or frequency of depressive symptoms in dementia patients (e.g., Cornell scale for depression in dementia, Geriatric depression scale).
Exclusion Criteria
Studies were excluded if: they were not randomized controlled trials (e.g., observational studies, case studies); participants were not suffering from dementia; if any interventions other than BM were used (e.g., light therapy, pharmacological interventions); had no depression outcome measures; no interpretable outcome data; or a low score on the methodological quality rating by Physiotherapy Evidence Database PEDro scale (Physiotherapy Evidence Database PEDro, 1999)14.Concurrent use of other interventions (e.g., medications for physical conditions, routine psychosocial supports) was regarded as acceptable and not used as a criterion for exclusion.
Search Methods for Identification of Studies
Systematic searching of randomized controlled trials (RCTs) included literature published between January 1999, which was the time at which the term and definition of BPSD was adopted by International Psychogeriatric Association (IPA, 2012)6 to the 30th August 2015. The search was conducted on five electronic databases: PubMed, Cochrane Library, EMBASE, CINHAL and PsycINFO.
By applying the Medical Subject Headings (MeSH), subheadings, keywords, and word variations search strategies, the search terms in PubMed and the other databases were “(dementia OR Alzheimer's disease OR neurocognitive disorders) AND (behavio* and psychological symptoms of dementia OR neuropsychiatric symptoms OR behavio* that challenge OR challenging behavio* OR bpsd) AND (depression OR depressive symptoms) AND (behavio* management OR behavio* therapy OR behavio* intervention OR behavio* modification OR functional analysis).” The search limits were the study type: randomized controlled trial; publication types: peer-reviewed journal articles with abstract; studies with only human subject; and published in English.
Data Collection and Analysis
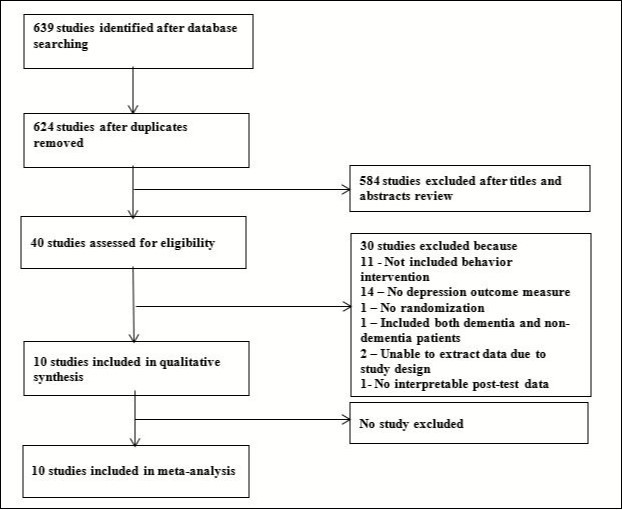
Selection of the Studies (See Figure 1)
A total of 639 studies was initially identified (624 after removing duplicates) from searching the five electronic databases. The first two authors separately reviewed the titles and abstracts of these studies against the selection criteria screen which yielded 40 studies. The 40 studies where then assessed against the full selection criteria where eleven studies fulfilled eligibility criteria which yielded 10 suitable studies. The chosen 10 studies where then rated separately rated by the first two authors to assess quality using the PEDro scale. The PEDro scale is an 11-item scale for the appraisal of methodological qualities of randomized controlled trials. Each item scores 1 point for “yes” and zero for “no or unclear” answers, with a total score ranging from 0 - 11 points. Studies with PEDro scores of six and above were assumed as having adequate internal validity and included in this systematic review. In the case of disagreement in the quality rating, a third author was consulted, and a decision was taken in agreement by all three raters. Finally, a quantitative synthesis (meta-analysis) was performed over the selected studies (n=10).
Data Extraction, Quality Assessment, and Analyzes
Data extraction from included studies was done using Excel spreadsheets. Details of the methodology, background demographic variables, baseline depression and dementia status, intervention and control methods, duration and dosage of interventions, and of depression outcome measures were extracted from the studies. If the depressive outcome was assessed more than one time, the result of the assessment that was taken at time immediate or closest to the termination of the intervention was chosen.
Data management and analyzes were performed using Microsoft Excel (2010 version) and MetaXL Version 3.0 software (EpiGear International Pty Ltd, Queensland, Australia 2011-2015). For comparisons between treatment and control groups, standardized mean differences (SMD) for pre-post studies with 95% confidence intervals (CIs) were calculated. Statistical heterogeneity was assessed using Chi-squared and I2 statistics (Higgins & Green, 2008)5. A random effect model was used to pool treatment effect. Sensitivity analysis was also performed to test the effects of outlying studies on the heterogeneity.
Results
Description of Studies
Included Studies (See Table 1)
Table 1. Characteristics of Included Studies.| Studies | Design | No | Baseline depression scores of treatment group (SD) (Measures) | Dementia severity | Types of Intervention | Setting | Duration | Dosage/session | |||||||||||||
| Treatment | Control | ||||||||||||||||||||
| Behavior Management Alone Group | |||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Kiosses 201528 | RCT | 74 | 21.08 (3.74)(MADRS) | Mild to moderate | Problem adaptation therapy | Attention control (Supportive therapy) | Community | 12 weeks | 12 | ||||||||||||
| Lichtenbeg 200530 | RCT (pilot study) | 20 | 13.1 (7.0) (CSDD) | Moderate to severe | Involving in pleasant events | Usual care (not specified in detail) | Nursing home | 3 months | 39 | ||||||||||||
| Marriott 200031 | Single blind RCT | 28 | 7.3 (4.6) (CSDD) | Moderate to severe | Caregiver education, stress management, coping skills training for problem behaviors | Two control groups: inter-view control and no interview control groups (No interview group was selected for comparison) | Community | 28 weeks | 14 | ||||||||||||
| Stanley 201333 | RCT (pilot study) | 32 | 9.4 (7.19) (GDS30) | Mild to moderate | Peaceful Mind program: Cognitive and behavior intervention for anxiety | Usual care (assessment, diagnostic feedback) | Community | 6 months | 20 | ||||||||||||
| Multimodal Group | |||||||||||||||||||||
| Burgener 200825 | RCT (pilot study) | 43 | 2.9 (3.4) (GDS15) | Mild to moderate | Combined Taiji exercise, cognitive behavior therapy, supportive group | Attention control (Delayed treatment) | Community | 20 weeks | 80 | ||||||||||||
| Callahan 200626 | RCT (Blocked randomization) | 153 | 4.4 (4.9) (CSDD) | Moderate | Functional analysis based collaborative care | Augmented usual care (education on dementia care and legal and financial advice) | Community | 1 year | 12 | ||||||||||||
| Chapman 200727 | Randomized partial cross over design | 118 | 0.11 (0.14) (CSDD) | Moderate to severe | Advanced Illness Care Team (AICT) approach: Combined behavioral, psychological, medical care and meaningful activities | Usual care (medication management, monitoring, physical and social activities) | Nursing home | 8 weeks | 5 | ||||||||||||
| Kurz 201229 | RCT | 201 | 8.54 (4.83) (GDS30) | Mild | Cognitive rehabilitation for patients and problem solving and coping skills training for caregivers | Standard medical care (may involve occupational therapy, physiotherapy,carer support or medication) | Community | 12 weeks | 12 | ||||||||||||
| Samus 201432 | RCT (pilot study) | 303 | 6.5 (4.8) (CSDD) | Mild to severe | management of unmet needs for patients with training of caregivers for problem solving skills | Augmented usual care (guidance and materials for care need assessment) | Community | 18 months | 18 | ||||||||||||
| Teri 200334 | RCT | 154 | 5.7 (3.9) (CSDD) | Moderate to severe | Combined exercise training to patients and behavior management training to caregivers | Routine medical care (acute medical and crisis intervention, education, advice) | Community | 3 months | 18 | ||||||||||||
The 10 randomized controlled trials (See References) represented a total of 1125 participants of which four studies (Burgener 2008, Lichtenberg 2005, Samus 2014 and Stanley 2013)25,30,32,33 were pilot studies (N = 398). The intervention arm of included studies had a total of 527 participants, and the control arm had 598 participants. Sample sizes ranged from 20 to 303 across the ten studies: four studies had <50 participants at baseline, one had <100, three had between 100-200 participants and two had > 200 participants at baseline. Eight studies were carried out in the United States, one in the United Kingdom and one in Germany. Apart from two studies (Chapman 2007 and Lichtenberg 2005)27,30 developed in residential care settings, eight studies were conducted in community settings. With the exception of (Lichtenberg 2005)30, the other studies described detailed demography of participants. In these nine studies, participants had their mean ages ranged from 72.4 to 88, and 57% were female. Four depression outcome measures were utilized in the included studies: Cornell Scale for Depression - CSDD (n=6), Geriatric Depression Scale – GDS 15 (15 item version) (n=2), GDS 30 (30 item version) (n=2), and Montgomery Asberg Depression Rating Scale - MADRS (n=1). The (Lichtenberg 2005)30study used both CSDD and GDS 15 and only the data for CSDD was used for the purposes of this review. With regard to participant severity of depression (Kiosses, 2015; Lichtenberg, 2005)28,30mean depression scores of participants at baseline assessment were MADRS score 21.08 (SD 3.74) and CSDD score 13.1 (SD 7.0) indicating that participants in these two studies were depressed at baseline. In the other eight studies, mean depression scores at baseline varied with the majority being mild cases. The severity of dementia at baseline assessment for the 10 studies were mild (n=1), moderate (n=1), mild to moderate (n=3), mild to severe (n=1), and moderate to severe dementia (n=4).
Characteristics of Interventions and Control Conditions (See Table 1)
Out of 10 studies, four studies (Kiosses 2015, Lichtenberg 2005, Marriott 2000 and Stanley 2013)28,30,31,33 applied problem adaptation therapy, involving in pleasant activities, caregiver coping skills training, and cognitive-behavior therapy (CBT) for depression and anxiety respectively. In the other six studies BM was part of multimodal intervention (See Table 1). The duration of intervention ranged from eight weeks to 18 months in which groups received between five to 80 sessions of BM. Interventions were targeted on depression coupled with one or more symptoms of agitation, pain, functional ability and disturbing behavior in three studies (Chapman 2007, Kiosses 2015, Lichtenberg 2005)27,28,30 while the remaining seven studies focused on mood and other outcomes, e.g., anxiety, cognitive function and disability. Usual care control conditions were described as attention control (n=2), usual care (n=3), augmented usual care (n=2), standard or routine medical care for dementia (n = 2), and no intervention control (n=1).
Quality and Risks of Bias in the Included Studies (See Table 2)
All studies scored 6 and above in the Pedro Scale, and were judged as having a low risk of bias as well as using randomization designs. Except for (Lichtenberg 2005)30, all studies stated specific eligibility criteria for participants. Few studies (n=2) described allocation concealment. Regarding blinding, only one study (Callahan 2006)26 described for therapist and subject blinding; but most studies (n=8) blinded the assessors. Six studies had more than 85% follow-up of at least one key outcome. Concerning the attrition bias, seven studies described that they made intention to treat analyzes (ITT) while two other studies (Chapman 2007 and Lichtenberg 2005)27,30 had all of their participants involved in the post-intervention assessment and, therefore, did not need to perform ITT. All studies described intervention protocols, guidelines or manuals for treatment fidelity and adherence purposes, nevertheless other factors affecting outcomes, such as differences among therapists, were not controlled.
Table 2. Quality Assessment of Included Studies by PEDro Scale| Studies | Specification of eligibility criteria | Random allocation | Concealed allocation | Prognostic similarity at baseline | Subject blinding | Therapist blinding | Assessor blinding | Greater than 85% follow up of at least one key outcome | Intention to treat analysis | Between group statistical comparison for at least one key outcome | Point estimates and measures of variability provided for at least one key outcome | Total |
| Kiosses 201528 | 1 | 1 | 0 | 1 | 0 | 0 | 1 | 1 | 1 | 1 | 1 | 8 |
| Lichtenberg 200530 | 0 | 1 | 0 | 1 | 0 | 0 | 1 | 1 | 0 | 1 | 1 | 6 |
| Marriott 200031 | 1 | 1 | 0 | 1 | 0 | 0 | 1 | 1 | 1 | 1 | 1 | 8 |
| Stanley 201333 | 1 | 1 | 0 | 1 | 0 | 0 | 1 | 0 | 1 | 1 | 1 | 7 |
| Burgener 200825 | 1 | 1 | 0 | 1 | 0 | 0 | 0 | 0 | 1 | 1 | 1 | 6 |
| Callahan 200626 | 1 | 1 | 1 | 0 | 1 | 1 | 1 | 0 | 1 | 1 | 1 | 9 |
| Chapman 200727 | 1 | 1 | 0 | 1 | 0 | 0 | 0 | 1 | 1 | 1 | 1 | 7 |
| Kurz 201229 | 1 | 1 | 1 | 0 | 0 | 0 | 1 | 1 | 1 | 1 | 1 | 8 |
| Samus 201432 | 1 | 1 | 0 | 1 | 0 | 0 | 1 | 0 | 1 | 1 | 1 | 7 |
| Teri 200334 | 1 | 1 | 0 | 1 | 0 | 0 | 1 | 1 | 1 | 1 | 1 | 8 |
Efficacy of Behavior Management on Depression (See Table 3, Figure 2 and Figure 3)
After pooling of treatment effect data, the quantitative analysis (meta-analysis) yielded the following results. In subgroup analysis, the four studies that used BM as an independent intervention showed no significant treatment effect on depression (SMD -0.20; 95% CI -0.96 to 0.56; N = 154). Sensitivity analysis was undertaken due to considerable heterogeneity (p = 0.00; I2 =80%) with the removal of an outlying study (Kiosses 2015)28, no heterogeneity resulted (p = 0.93; I2 = 0) (SMD 0.16; 95% CI -0.28 to 0.60).
In the other six studies where behavior treatment was a component of a multimodal intervention, the analysis showed a trend favored the intervention, but it was not significant (SMD -0.12; 95 % CI -0.25 to 0.01; N = 971). There was no heterogeneity among these multimodal intervention studies (p = 0.79; I2= 0%). Only one study (Kiosses 2015)28used problem adaptation behavior therapy which showed a significant positive result (SMD -1.13; 95% CI -1.62 to -0.64).
Table 3. Comparison of Depressive Outcome Scores at Post- Intervention Period between Behavior Management and Usual Care Groups.| Study | Intervention | Control | Standardized mean difference (95% CI) | ||||
| N | Pre-post mean difference | SD | N | Pre-post mean difference | SD | ||
| Behavior Management Alone Group | |||||||
|---|---|---|---|---|---|---|---|
| Kiosses 201528 | 37 | -10.00 | 3.74 | 37 | -6.00 | 3.26 | -1.13 (-1.62 to -0.64) |
| Lichtenberg 200530 | 9 | -0.20 | 7 | 11 | -1.40 | 5.80 | 0.18 (-0.70 to 1.06) |
| Marriott 200031 | 14 | -0.10 | 4.6 | 14 | -0.30 | 2.70 | 0.05 (-0.69 to 0.79) |
| Stanley 201333 | 16 | -1.20 | 7.19 | 16 | -2.90 | 6.46 | 0.24 (-0.45 to 0.94) |
| Multimodal Group | |||||||
| Burgener 200825 | 24 | 0.40 | 3.4 | 19 | 0.90 | 2.90 | -0.15 (-0.76 to 0.45) |
| Callahan 200626 | 84 | -0.90 | 4.9 | 69 | 0.40 | 5.90 | -0.24 (-0.56 to 0.08) |
| Chapman 200727 | 57 | -0.02 | 0.14 | 61 | -0.01 | 0.08 | -0.09 (-0.45 to 0.27) |
| Kurz 201229 | 100 | -1.23 | 4.83 | 101 | -0.41 | 5.47 | -0.16 (-0.44 to 0.12) |
| Samus 201432 | 110 | 0.40 | 4.8 | 193 | 0.30 | 4.60 | 0.02 (-0.21 to 0.26) |
| Teri 200334 | 76 | -0.50 | 3.9 | 77 | 0.40 | 4.50 | -0.21 (-0.53 to 0.11) |
Figure 2. Forest Plot of Comparison: Behavior Management versus Usual Care (Behavior Management Alone Group) 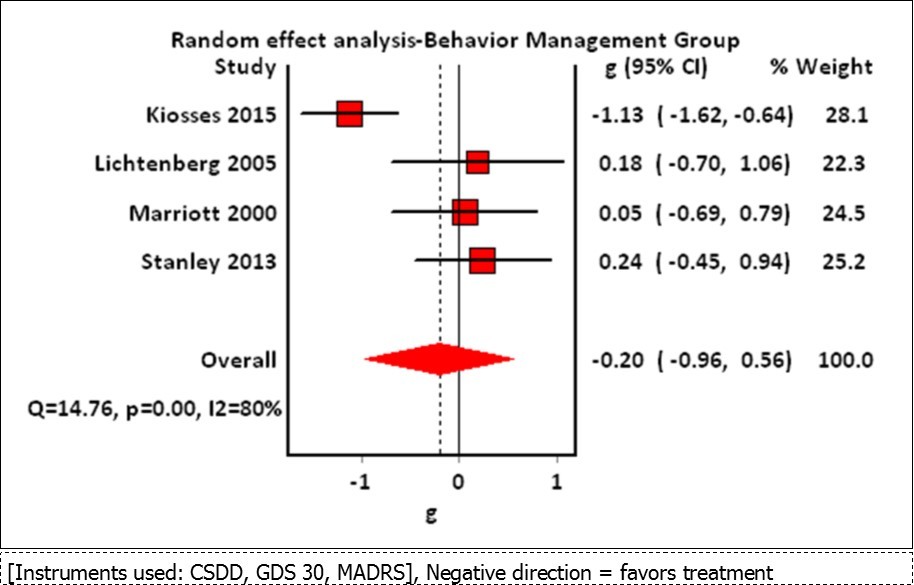
Figure 3. Forest Plot of Comparison: Behavior Management versus Usual Care (Multimodal Intervention Group)
Discussion
The information from this meta-analysis suggested that BM lacked efficacy in reducing depression in dementia patients. However, ( Kiosses 2015)28 found an effect for BM for participants with mild to moderate dementia in a community setting. It is possible that BM has some efficacy for people with milder severity of dementia compared to those with advanced symptoms. The intervention used was problem adaptation therapy involving both patients and importantly caregivers. Multi-modal interventions modify the patient environment which may assist mood without requiring a high level of individual understanding and engagement with BM. The four studies in which BM was provided as a focused intervention yielded no significant treatment effect of the intervention on depression. (see Table 1) Interventions were exclusively focused on depression in only two studies (Kiosses 2015 and Lichtenberg 2005)28,30 where participants demonstrated higher mean depression scores at baseline assessment. The (Lichtenberg 2005)30 pilot study was undertaken in a residential care setting where participants had moderate to severe dementia. The intervention aimed to increase involvement in pleasant events and demonstrated no significant results. For the remaining two studies in this group of which one was a pilot, targeted symptoms in addition to depression and also was non-significant. However, there is a risk that pilot studies might not indicated a true effect for BM because of small sample sizes and might better represent the features of the specific participants studied.
There remains a question as to how depressed participants actually were in these studies. Baseline depression assessments in eight studies (92% of the total sample population) showed mean depression scores within mild to subclinical ranges, and in a few studies, e.g., Chapman 2007)27, baseline mean depression scores lay at the bottom of the respective rating scales. It might be the case the participants were not depressed enough to demonstrate significant change over the duration of BM. Depression research suggest higher symptoms score are more likely to significantly reduce as a result of intervention compared to low scores which result in a floor effect. It is also questionable if the depression rating scales used in these studies would detect atypical presentations of depression in the advanced dementia patient groups. In detecting depression in Alzheimer’s disease, Müller-Thomsen, Arlt, Mann, Maß and Ganzer (2005)10 recommended the use of CSDD and MADRS, and stated the GDS was not an adequate for the detection of depression in this population because of sensitivity issues.
A considerable proportion of participants had severe dementia. The presence of declining language functions and increasing resistance to care in advanced dementia patients could limit adherence and cooperativeness with care, which might consequently reduce treatment effect. The prevalence of resistance to care might increase eightfold in patients with the most severe stage of dementia in comparison with patients with mild dementia (Volicer, Bass, & Luther, 2007)21. Due to the limited amount of published data that met the inclusion criteria a degree of heterogeneity between studies was tolerated. The limitation was related to the focus of the interventions with two studies targeted for depression only and one study of the multimodal group.
While meeting the criteria for BM, the interventions reviewed were based on different theoretical models, for example, behavior programming model in (Lichtenberg 2005)30, stress vulnerability family coping skills model in Mariott 2000, and unmet need model in Samus 2014;)32 it was delivered in different settings (e.g., family care and residential care). This heterogeneity was unavoidable due to the limited amount of literature available for this review. As a result it might have affected the comparability of outcomes. However, what appears reasonably robust in terms of findings is that the different approaches did not yield significant differences in effect which demonstrated them all as equally non-effective.
Another caveat could be the use of variable control conditions. Participants in the control groups were receiving some forms of usual service from their respective dementia care facilities. The intensities of treatment and services they received were varied due to a diversity of the control condition (from no intervention control to augmented usual care) which might have influenced the results of treatment.
The limitations of the literature found for this review reflects a disparity between the amount of research in the area of psychosocial interventions for depression in dementia patients, and the epidemiological importance of the problem. The Teri et al. (1997)20 study resulted in both the SIGN (Network SI, 2006)16and National Collaborating Centre for Mental Health – NICE-SCIE guidelines (NICE-SCIE D, 2006)11 suggested that BM may reduce depression in dementia patients living in the community with caregiver however there was a lack of empirical evidence for different stages of dementia. The findings of this review found no supporting data for the Teri et al. (1997)20 proposition.
Conclusion
The findings of this systematic review indicate a lack of efficacy for BM for depression in dementia patients. However, the finding of a possible non-significant trend towards multimodal interventions that include BM warrants further investigation. Some of the data suggests may have some efficacy for depression in mild dementia. However, this proposition requires further investigation.
Directions for Future Research
Dementia and depression is a clinical problem with increasing prevalence, impact on quality of life and increasing the burden on health systems and examining any benefit for psychological treatments such as BM is a priority area for research. Future research should focus on standardised BM and homogeny in design to additional interventions, treatment targets, setting, and severity of dementia, length of treatment, control conditions and follow up. It may be productive to focus research attention on mild dementia in the first instance where the evidence is suggestive there may be some benefit.