Abstract
The world is countering an unexpected wide spread of Covid-19 virus. Among the procedures used to prevent spreading the virus are classical and modern sterilization methods. In this paper, we combine the use of ultraviolet emissions, as a modern method, with the infrared emissions that generates high temperature, as a classical method, to design and implement a sterilization oven. Ultraviolet emissions have the ability to destroy the RNA of the virus while the infrared emissions destroy the virus membrane. Test was performed on indicators contains +ve gram rod bacteria which is stronger than the Covid-19 virus in high temperature and UV emission tolerant. Results showed that the UV emissions killed the microorganism in 15 minutes. However, combination between the UV and IR emissions in a sterilization oven succeeded to kill the under test microorganism in five minutes. The combination between the two sources of emission guarantees an effective sterilization process against bacteria, fungus, and viruses. Moreover, it speeds up the sterilization process time.
Author Contributions
Academic Editor: Eduardo Rodrigues, Federal University of Mato Grosso, Faculty of Medicine, Cuiabá, MT, Brazil.
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2020 Mohamed Shehataa, et al.
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Introduction
The worldwide nowadays is countering a contemporary disaster by all accounts which is the spread of Corona virus, known as Covid-19 virus. The first case of Corona virus was reported in 1960. Since this time, infected cases were mostly designated as cold flu. After a while, the world faced the fact that some versions of this virus cannot be just treated in home and some patients had to receive the cure in the intensive care rooms. The first appearance of Covid-19 virus was reported in Wuhan market, China on the 7th of January 2020 1. The symptoms were more serious and the world started to take serious actions to prevent spreading the virus. Scientists started studying the spread of the virus using statistical analysis tools to estimate the spread histogram trying to predict the spread peaks of the pandemic for each country. Although a correlation between human mobility and spreading the virus, it was difficult to predict the future spread parameters for the presented models 2. Humanity must move forward to prevent spreading the virus by all available methods.
Medical crows used the sterilization methods to sterilize medical equipment and objects in hospital rooms. Classical sterilization techniques such as steam under pressure and hot air are used whenever they are available 3. However, these methods may not be effective in cases such as sterilizing open area or objects that can be damaged by high pressure and temperature. One different method is used to prevent spreading the Covid-19 virus which is sterilization using irradiation methods. Gamma irradiation is used to sterilize hospital supplies and food products without changing the organic properties 4. However, Gamma ray generation systems are not simple and expensive. Another method which is less in cost and simple in implementation is sterilizing using Ultraviolet (UV) rays 5. The UV radiations penetrates the microorganisms’ membrane and damages the DNA of the cell preventing them from reproducing. Its effect was studied on bacteria, viruses, and fungus and it showed promising results. The advantages of using UV emissions are: prevent using toxic chemicals in sterilization process, no residual effect, user friendly with simple precautions, shorter sterilization time, and needs small space to be installed 6. That is why the UV radiation was used to sterilize grains surface without changing the quality of the food 5.
UV emissions are divided to three sub-bands according to its wavelengths: UV-A from 320 to 400nm, UV-B from 290 to 320nm, and UV-C from 100 to 290nm 7. UV-C has the most powerful effect on the virus that can damage its DNA and prevent its reproduction. Time of exposure and doses control the efficiency of the sterilization process and it shall be predetermined carefully. Using UV-C radiations combined with other classical sterilization processes such as manual cleaning surfaces decreased the bacterial population at least 70% 8, 9. Figure 1(a) shows a sample of virus, Figure 1 (b) shows the effect of the UV emissions on the virus, Figure 1 (c) shows the effect of the IR, and Figure 1 (d) shows the effect of both UV and IR emissions combined on the virus membrane and its RNA 10.
Figure 1. Comparison of damage induced by UV and IR emissions (a) control sample (b) UV treated sample (c) IR treated sample (d) UV and IR combined treated sample 10.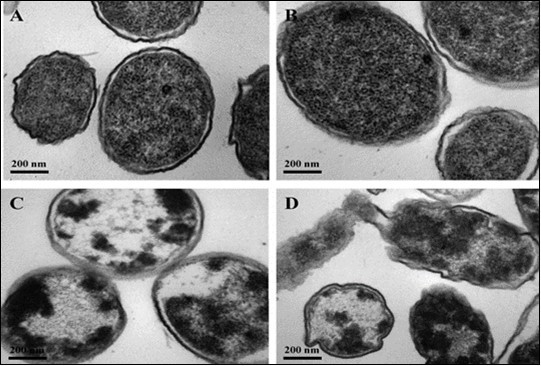
It was proved that Covid-19 virus dies in in a temperature more than 70C0. The high temperature can be considered as a sterilization classical method. Infrared (IR) emissions can be used to generate these high temperatures 11. From the point of view of mixing classical and advanced sterilization methods, the IR and UV-C emissions can be used together to increase the probability of killing Covid-19 virus.
In this paper, a combination between the UV-C radiations and Infrared emission source to generate high temperature is used to sterilize objects in hospitals and in home. The apparatus benefits from UV-C capability to damage the virus RNA and increases the destruction performance by increasing the medium temperature. Section II presents the methods. Section III presents the results and section IV presents the discussion and section V presents the conclusions.
Methods
Allenvelope viruses like Covid-19 are composed of protein membrane protecting the nucleic acid genome. Virus can be killed by destroying the outer membrane or the viral ribonucleic acid (RNA). The effect of medical disinfectants, UV, and high temperature on hepatitis C virus (HCV) was studied and analyzed 12. The medical disinfectants like alcohol destroys the viral envelope membrane. However, UV and high temperature destroy the RNA. Also, the temperature may destroy its envelope membrane 12. UV has the same effect on Covid-19 virus and UV sterilizers can be used to kill the virus 13. In this paper, a combination between UV and IR was directed to implement a sterilization device which has the ability to destroy the virus membrane and its nucleic acid genome.
The relationship between the suggested UV suitable dose to kill the virus and the UV lamb irradiance can be determined from the following equation 14:
D=EtXI ….(1)
where, D is the exposure dose in J/m2, Et is the exposure time in seconds, and I is the irradiance in W/m2. If the irradiance is related to a dose that refers to 90% disinfection rate of the total population of the microorganism, the exposure dose is defined as D90. This disinfection rate dose can be calculated from the following equation 14:
 …..(2)
…..(2)
where, k is the UV rate constant for the resistant population in m2/j. The average k constant for Corona virus is equal to 0.377 14. Then,
 .
.
One of the famous UV lambs that are available in the market is G20T10 UV category lamps that can be purchased on shelves from the international market. This type of lamps has an irradiance rating equal to 41 μW/cm2| 14. The exposure time Et in a sterilization oven can be calculated from Eq. 1 as follows:
 …...(3)
…...(3)
These calculations are for objects in dry air. For liquids, it is harder. The D90 is around 25J/m214. Sterilization process cycle needs an exposure time around 1 minute. Two G20T10 UV lamps were installed in the implemented oven that guarantees subjecting the targeted objects to a dose over the required sterilization dose. Two IR lamps were installed in the oven to increase the probability of killing the virus 8. Figure 2 shows the implemented apparatus.
Results
The sterilization process was tested using Browne biological indicator produced by JST medical Ltd. company, Napier 15 that contains a rod-shaped gram-positive bacteria. The indicator tube contains a stated population of bacteria inside a transparent plastic culture tube. Biological indicators contains highly resistant bacterial spores that if it is destroyed, it is assumed that any other organisms has also been killed 16. Figure 3 shows the used biological indicator.
Figure 3. The used biological indicator.
The test was performed using eight indicators in seven separate experiments and one indicator was left to check the accuracy of lab test for the bacteria growth. Two indicator were subjected to the IR emissions inside the sterilization oven once for 5 minutes and the other for 15 minutes. Another two were subjected to the UV emissions for 5 and 15 minutes. One was subjected to the combined UV and IR emissions for 5 minutes. One was put inside a cotton mask and subjected to a combination between UV and IR emissions for 15 minutes, and one was put inside a white paper envelope and subjected to a combination between UV and IR emissions for 15 minutes. After that, the crushable glass ampule that contains the culture medium was crushed in a medical lab and put in suitable bacteria growth medium for two days. Table 1 shows the results for each experiment.
Table 1. Experiment results| No. | Source of radiation | Exposure time (minutes) | Sterilization object | Lab result |
| 1 | - | - | Bacteria indicator tube | Positive for Geobacillus stearothermophilus |
| 2 | IR | 5 | Bacteria indicator tube | Positive for Geobacillus stearothermophilus |
| 3 | IR | 15 | Bacteria indicator tube | Positive for Geobacillus stearothermophilus |
| 4 | UV | 5 | Bacteria indicator tube | Positive for Geobacillus stearothermophilus |
| 5 | UV | 15 | Bacteria indicator tube | No growth |
| 6 | UV+IR | 5 | Bacteria indicator tube | No growth |
| 7 | UV+IR | 15 | Bacteria indicator tube inside cotton mask | Positive for Geobacillus stearothermophilus |
| 8 | UV+IR | 15 | Bacteria indicator tube inside white envelope | Positive for Geobacillus stearothermophilus |
The results showed that the bacteria were not be able to grow in population with experiment number 5 and 6. The UV and IR emissions in the other experiments failed to kill the bacteria. The IR radiation for 5 and 15 minutes is not enough to affect the bacteria membrane and destroy it. The UV emissions for 15 minutes alone was able to destroy the bacteria DNA. However, it failed to destroy it in 5 minutes. But, the combination between UV and IR emission succeeded to kill the bacteria in 5 minutes.
Discussion
The test was performed on gram-positive rod bacteria, which is stronger than Covid-19 virus. The combination between UV and IR emission succeeded to kill the bacteria in a period of time less than that is required for UV only to do the same effect. When the bacteria indicator tube is not subjected to direct UV emissions, the combination between UV and IR emissions failed to kill the bacteria. This means that the combination between UV and IR emissions in sterilization oven can be used to kill bacteria, virus, and fungi on surfaces subjected to direct UV emissions. This method of sterilization is not effective for indirect contact with the UV emission source. For example, medical tools with groves is not suggested to be sterilized in this oven.
One of the new findings in this research is that the IR emissions accelerates the sterilization process. The sterilization process cycle time was reduced three times when the IR was combined with the UV emissions. The IR radiations can be used alone with longer sterilization process cycle time and higher temperature (more than 135C0). But, it is not preferred because objects may be affected functionally by the high temperatures, in addition, the longtime means less objects to be sterilized.
Conclusion
In this paper, a sterilization oven for Covid-19 is presented. The sterilization process depends on combining between the use of ultraviolet and infrared emissions. The oven was tested by putting eight transparent biological indicator inside it separately for 5 and 15 minutes in different seven experiments. The indicators was tested in the lab to study the bacteria growth. The oven stopped its growth successfully when the UV and IR emissions were combined for 5 minutes. The combination between the two radiation sources speed the sterilization process. However, the object surface shall be subjected to direct UV emissions.
On behalf of all authors, the corresponding author states that there is no conflict of interest
Acknowledgements
This research is supported in part by the air defence research and development center, Cairo, Egypt and the bacteria growth was tested in Alborg lab by Dr. Ghada Abd El Tawab, M.D. Clinical & Chemical Pathology, Faculty of Medicine, Al Azhar University.
