Abstract
Syphilis is caused by the bacterium Treponema pallidum and is transmitted from human to human through sexual contact. Congenital syphilis (CS) occurs when the mother transmits the infection to the fetus. Clinical manifestations of CS include anemia, hepatosplenomegaly, blindness, deafness, meningitis, and deformities in bone structure. The number of cases of CS have increased over the past decade in the United States according to the CDC. A study was conducted correlating the number of Medicaid enrollees in 2020, the number of uninsured persons in 2020, and the number of cases of COVID-19 in 2020 to cases of CS in the United States in 2021. A Spearman rank correlation analysis was done using SPSS. Results were statistically significant for all three pairs of variables with positive correlations; Medicaid enrollment and CS cases (r = 0.735, P<.05), uninsured persons with CS cases (r = 0.713, P<.05), COVID-19 cases and CS cases (r = 0.689, P<.05). Reasons for the increase in CS cases are multifactorial, including variations in state laws regarding syphilis screening in the prenatal period, differences in provider processes for persons on Medicaid, persons uninsured, and restrictions to accessing healthcare providers during the COVID-19 pandemic. Future studies should include questionnaires and interviews with women on their experiences during prenatal visits in regards to syphilis screening, particularly women covered by Medicaid, and surveys completed by healthcare providers to gain insight and to identify factors that affect a woman not being tested for syphilis during her pregnancy.
Author Contributions
Academic Editor: Rahul Hajare, Indian Council of Medical Research, New Delhi
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2023 Virginia C. Hughes
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Introduction
Congenital syphilis (CS) is an infection transmitted from mother to child during pregnancy and is caused by the spirochete Treponema pallidum. Infection may result in stillbirth or miscarriage, and a plethora of health issues for the developing newborn including severe anemia, hepatomegaly, splenomegaly, blindness, deafness, meningitis, and deformities in bone structure. Over the past decade, there has been an upward trend in the number of cases of CS as reported by the CDC. For example, the number of reported CS cases increased by 261 percent from 2013 to 20181. The CDC recommends syphilis screening at the first prenatal visit with retesting at 28 weeks gestation, and at delivery if the woman is considered at high risk for syphilis; including a history of drug misuse, Sexually transmitted infections (STIs) during pregnancy, multiple partners, a partner with an STI, homelessness, or lack of prenatal care2. The fifty states and the District of Columbia voluntarily report cases of CS to the National Notifiable Diseases Surveillance System (NNDSS) which has defined CS as a condition that affected stillbirths and infants born to mothers with untreated or inadequately treated syphilis regardless of signs in the infant, or a condition affecting an infant with clinical evidence of CS including direct detection of Treponema pallidum or a reactive nontreponemal syphilis test with signs on physical examination, radiographs, or cerebral spinal fluid. Administration of a penicillin-based regimen to pregnant women ≥30 days before delivery, appropriate for the stage of infection, is considered sufficient treatment3
Barriers to syphilis screening among pregnant women have been linked to the type of insurance (e.g. Medicaid vs private insurance), lack of transportation to the physicians' office or clinic, delays in testing, and issues related to the COVID-19 pandemic. This study focuses on three factors in association with CS cases: Medicaid enrollment, persons uninsured, and COVID-19 cases. Medicaid has been in existence since 1965 and provides health assistance for persons with low income. This program provides healthcare coverage to more than 25 million women in the United States, and moreover represents the largest single payer of pregnancy-related services.4 Syphilis rates among Medicaid participants are six times as high as those with private insurance and twice as high as those that are uninsured or self-pay persons5. The high rates of syphilis may be explained by what individual states provide regarding screening and clinician practices. Persons that are uninsured may choose to disregard screening recommendations due to financial challenges or ascribing screening a low priority. Regarding the COVID-19 pandemic studies have shown an increase in cancellations and/or delays in prenatal care visits. During the COVID-19 pandemic, pregnant women may have been apprehensive to undergo screening not wanting to expose themselves to the virus. This study correlates Medicaid, uninsured persons, and COVID-19 data to cases of CS in 2021.
Materials and Methods
A Spearman rank correlation analysis was conducted utilizing data from the CDC on cases of CS in all states except for Maryland. The District of Columbia was included in this study. The unit of analysis was the state, and the dependent variable was CS cases. Independent variables included COVID-19 cases in 2020, Medicaid enrollment in 2020, and persons uninsured in 2020. Medicaid enrollment data and COVID-19 cases were accessed from the CDC for the year 2020. Data representing persons who were uninsured was accessed from HHS-ASPE (Health and Human Services Assistant Secretary for Planning and Evaluation) for the year 2020. Because the data were not normally distributed, a Spearman's rank correlation was performed using SPSS (v.26). Raw data were transformed into ranked data using SPSS.
Results
Spearman rank correlation studies revealed statistical significance and positive correlations across all variables. CS cases paired with COVID-19 cases yielded a correlation coefficient of 0.689, P<.05 (Figure 1); CS cases paired with Medicaid enrollment yielded a correlation coefficient of 0.735, P<.05 (Figure 2); CS cases paired with uninsured persons yielded a correlation coefficient of 0.713, P<.05 (Figure 3).
Figure 1. Spearman rank correlation analysis of CS cases with COVID-19 cases (r = 0.689, P<.05).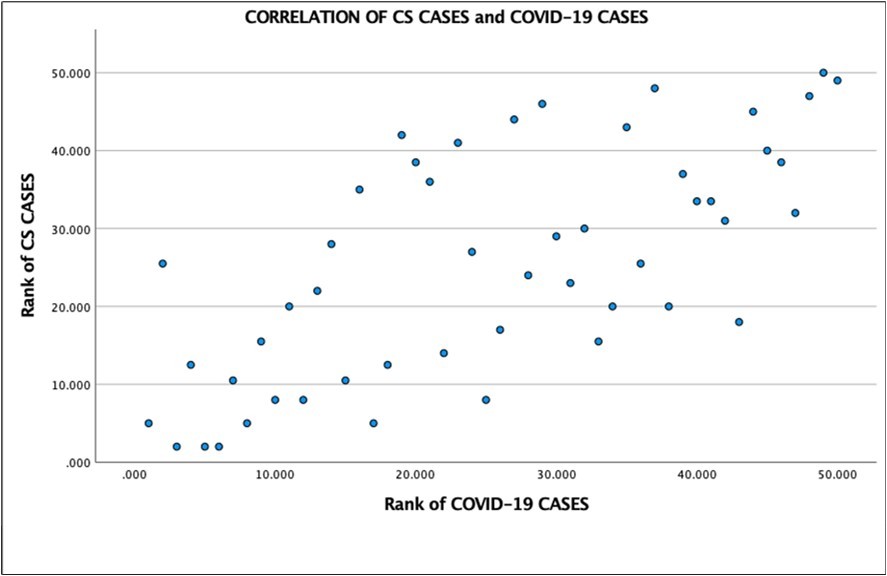
Figure 2. Spearman rank correlation analysis of CS cases with Medicaid enrollment (r = 0.735, P<.05).
Figure 3. Spearman rank correlation analysis of CS cases with uninsured persons (r = 0.713, P<.05).
Discussion
This study provided insight into associations with CS cases in 2021 involving COVID-19 cases, Medicaid enrollment, and the number of persons without health insurance. Data from 2020 for the three independent variables were hypothesized to have an impact on the 2021 CS cases. All correlations proved to be statistically significant and all were positive correlations, which can be interpreted as increases in COVID-19, Medicaid enrollment, and persons uninsured tend to yield increases in the number of CS cases. Higher numbers of CS cases have been seen in southern states. Toward this end, Lanier et al6 studied prenatal syphilis screening from 2017 to 2019 among Medicaid beneficiaries in Georgia, Kentucky, Louisiana, North Carolina, South Carolina, and Tennessee. The percentage of women with a syphilis test at any point during pregnancy ranged from 56 to 91 percent, and from 78 to 90 percent during the first trimester across six states. The total number of women tested in the first trimester was 179,552 compared to 346,500 in the prenatal period. Demographically, researchers found non-Hispanic White women exhibited a higher percentage of first-trimester testing (34 to 74 percent) than non-Hispanic Black women (31 to 69 percent); this pattern was reversed in third-trimester testing (7 to 72 percent, 10 to 72 percent, respectively). The authors asserted that healthcare strategies implemented among the six states in regard to screening women for syphilis in the first trimester were not successful given the data. State-wide public information campaigns are needed to better ensure early detection and treatment among women to prevent CS. In 2023, the same six states were studied by the CDC in addition to the state of Alabama7. The CDC interviewed women to assess their experiences with Medicaid and procuring adequate pre-natal care with regard to syphilis screening. Semi-structured interviews were conducted via videoconferencing from February to August 2021. Questions posed to participants related to immigrants access to Medicaid, state expansion and access to syphilis testing before and during pregnancy, and improving access to pregnant women. The findings indicated that men are more likely than women to be uninsured in non-expansion states that have not expanded eligibility for Medicaid, resulting in increased infection or reinfection of pregnant women. Of the seven states studied, only Louisiana and Kentucky have expanded their Medicaid programs. The study also revealed that women who qualify for Medicaid during their pregnancy are devoid of coverage after the postpartum period; the overall rate of postpartum uninsurance is three times higher than in Medicaid expansion states. Lapses in insurance coverage during the postpartum period may prompt women to delay recommended screening for syphilis. Alabama and Georgia are the only states that extended coverage past the 60-day postpartum period. It was articulated by an interviewee that many pregnant women in non-expansion states may not be aware they are eligible for testing or simply choose not to be bothered with the complex application process. Late initiation of prenatal care due to lack of health care coverage has been identified as a major contributing factor to the late diagnosis of maternal syphilis and resultant CS cases. Georgia, Kentucky, North Carolina, and Tennessee offer presumptive eligibility for pregnant women while their applications are pending; however, some physicians refuse to see pregnant women until they are deemed eligible for Medicaid. Immigrants also face challenges in having access to prenatal care. There is a five-year waiting period for immigrants to be eligible for Medicaid leaving women to utilize Emergency Medicaid, which covers labor and delivery services but not prenatal care. Immigrants also have difficulty navigating the application process, policies, and language in laws. Interviewees also commented that mothers and babies leave the hospital before syphilis testing is completed which can result in a lack of follow-up and treatment in positive cases. Lastly, interviewees stated that the COVID-19 pandemic greatly impacted prenatal care in moving from in-person to virtual doctor visits; pregnant persons without required technological resources or internet access may not have met with a clinician to discuss prenatal care including screening for syphilis.7
The COVID-19 pandemic had a dramatic effect on people having access to their healthcare providers, be it medical, dental, optometry, or other services. Routine antenatal care for women is essential in identifying high-risk pregnancies and detection of diseases. Restrictions women faced in meeting with their healthcare provider included limitations of public transportation, fear of contracting COVID-19 given the high rate of transmission as well as the spread of the virus from asymptomatic persons. While telehealth services increased greatly during the pandemic,8, 9 this option was futile for pregnant women who were in need of ultrasound examinations, blood testing, and other diagnostic tests that require an in-person visit. Lee conducted a cross-sectional study using the Pregnancy Risk Assessment Monitoring System (PRAMS) from October 2020 to June 2021 where pregnant women participated in a survey answering COVID-19-related questions pertaining to canceled or delayed appointments, and in addition binary variables were also explored10. These included facility closure, loss of health insurance, family care, and lack of transportation. Independent variables included demographic information, health conditions, and pregnancy-related histories. Results showed that out of 11,427 participants, 32.5 percent in 2020 and 28.8 percent in 2021 canceled or delayed prenatal care. Factors that were statistically significant included race (Hispanics were more likely to cancel or delay appointments than other groups), lack of transportation, education, depression, and notably type of insurance, where persons on Medicaid were more likely to cancel or delay visits compared to women with private insurance. In another cross-sectional study conducted by Lee, females showed 1.29 times greater risk of delayed and forgone care than their male counterparts which may have led to lapses in syphilis screening on a large scale11.
State legislators have a salient role in syphilis screening in the prenatal period by passing laws requiring clinicians to test for syphilis. However, these laws vary in regard to time period of testing and penalties for clinicians who do not adhere to guidelines. As depicted in Table 1, the majority of states require screening at the first prenatal visit. Arizona, Arkansas, Connecticut, Delaware, the District of Columbia, Florida, Georgia, Illinois, Louisiana, Maryland, Michigan, Nevada, New Mexico, North Carolina, and Texas, require testing in the third trimester, and Alabama, Arizona, New Jersey, New Mexico, North Carolina require testing at delivery. Alabama, Indiana, Missouri, Pennsylvania, and Tennessee only require testing in the third trimester if the woman is deemed to be at high risk, and Florida, Georgia, Louisiana, Maryland, Michigan, and Missouri only require testing at delivery if the woman is at high risk. Hawaii’s law stipulates syphilis testing during the period of gestation or at delivery; Maine, Minnesota, and Kentucky requires screening but does not stipulate time points for testing. States devoid of laws on syphilis screening in the prenatal period are Mississippi, North Dakota, and Wisconsin. Clinicians that violate laws in Alaska, California, Colorado, Idaho, Missouri, Montana, Rhode Island, South Carolina, and West Virginia can be charged with a misdemeanor that may carry a fine; in the state of Virginia, the clinician's professional license can be revoked if laws are not followed. States that honor a woman’s religious beliefs on refusing syphilis screenings include Alaska, Arkansas, California, Colorado, Connecticut, Delaware, Florida, Georgia, Illinois, Iowa, Louisiana, Maryland, Michigan, Montana, Nevada, Ohio, Oklahoma, South Carolina, Tennessee, and Utah. The limitation of this study is not including the state of Maryland in the correlation analysis due to the unavailability of CS cases in 2021.
Table 1. Prenatal Syphilis Requirements for States| State | First Visit | Third Trimester | Delivery |
|---|---|---|---|
| AL | √ | ∆ | √ |
| AK | √ | ||
| AZ | √ | √ | √ |
| AR | √ | √ | |
| CA | √ | ||
| CO | √ | ||
| CT | √ | √ | |
| DE | √ | √ | |
| DC | √ | √ | |
| FL | √ | √ | ∆ |
| GA | √ | √ | ∆ |
| HI | |||
| ID | √ | ||
| IL | √ | √ | |
| IN | √ | ∆ | |
| IA | √ | ∆ | |
| KS | √ | ||
| KY | |||
| LA | √ | √ | ∆ |
| ME | |||
| MD | √ | √ | ∆ |
| MA | √ | ||
| MI | √ | √ | ∆ |
| MN | |||
| MS | |||
| MO | √ | ∆ | ∆ |
| MT | √ | ||
| NE | √ | ||
| NV | √ | √ | ∆ |
| NH | √ | ||
| NJ | √ | √ | |
| NM | √ | ||
| NY | √ | ||
| NC | √ | √ | √ |
| ND | |||
| OH | √ | ||
| OK | √ | ||
| OR | √ | ||
| PA | √ | ∆ | |
| RI | √ | ||
| SC | √ | ||
| SD | √ | ||
| TN | √ | ∆ | |
| TX | √ | √ | √ |
| UT | √ | ||
| VT | √ | ||
| VA | √ | ||
| WA | √ | ||
| WV | √ | ||
| WI | |||
| WY | √ |
Conclusion
This study demonstrated statistically significant correlations between CS cases in 2021 and data from 2020 regarding COVID-19 cases, Medicaid enrollment, and the number of persons without health insurance. It is evident that women covered by Medicaid have a higher rate of syphilis that may be linked to factors such as living in a non-Medicaid expansion state, lapses in insurance coverage, not having access to healthcare services due to immigration status, healthcare providers not performing testing in a state devoid of prenatal screening laws, or not performing screening for other reasons. Women may also choose not to have syphilis screening done for religious reasons, and many states as outlined above honor their decision. The majority of states require screening on the first visit but not in the third trimester or at delivery. A woman may test negative in the first trimester but could be infected later on in the pregnancy. Not being tested places her and her child at great risk for a multitude of conditions. State legislators should revisit laws per the recommendations of the CDC placing a greater emphasis on testing throughout pregnancy. There was also a correlation between persons uninsured in 2020 and CS cases in 2021. There may be many reasons why a pregnant woman is uninsured, be it financial stresses, loss of employment, or lapsed coverage. City officials should communicate to women and families without insurance, options for testing at no charge through the state health department to ensure all women get screened and treatment if positive. City officials should also help women and families navigate all options for health insurance coverage including CHIP (Children’s Health Insurance Program), Community-based healthcare options, Short-term Limited duration Insurance (STLDI), Consolidated Omnibus Budget Reconciliation Act (COBRA), the Indian Health Service, and the Health Insurance Marketplace. While the COVID-19 pandemic is in the past, it is insightful to explore the association between number of COVID-19 cases and CS cases for future healthcare crises that may impede a women’s ability to see their healthcare provider during the prenatal period. Congenital syphilis is a sentinel event. Opportunities are missed for preventing syphilis across the United States as outlined in this paper. Future studies should focus on interviewing both women and healthcare providers on factors they perceive as interfering with syphilis screening during the prenatal period, as well as continuing to track the rates of CS in all areas of the United States.