The Additional Diagnostic Value of the Three-dimensional 3D ultrasound and Doppler angiography imaging in the prenatal diagnosis of left isomerism
Abstract
Objective
To highlight the value of 3D ultrasound and Doppler angiography imagingin the prenatal assessment of left fetal isomerism.
Methods
A retrospective offline analysis of volume datasets of 3 fetuses with left atrial isomerism by 3D ultrasound was conducted.
Conclusion
We believe that parasagittal view demonstrating the heart and the abdominal vessels is easy to obtain and interpret, offer a realistic anatomic image, needs no mental reconstruction of spatial relationships and is very beneficial mainly in detecting the situs. We propose to use 3D ultrasound systematically in suspected cases of atrial isomerism, and better understand and interpret fetal anatomy.
Author Contributions
Copyright © 2020 Wael El Guindi, et al.
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Introduction
At very early embryonic stages the embryo appears symmetrical with respect to the midline 1 During gastrulation, this initial symmetry is broken by cascades of gene activation that confer specific properties on the left and right sides of the embryo. This step, symmetry breaking; is essential for proper establishment of a predicable left-right (LR) patterning and placement of the internal organs and associated vasculature. 2, 3. This left-right (LR) asymmetry arise much earlier than the morphological asymmetry of visceral organs and is fundamental to their function and position within the body. 2.
The term situs solitus is used to describe the usual asymmetric positioning of the cardiac atria and the viscera. Defects in LR asymmetric patterning often leads to malformations, including heterotaxy syndromes 4, 5, 6. (derived from the Greek heteros, “other” and taxis, meaning “arrangement meaning other than the usual arrangement”) which is also named situs ambiguous, isomerism, asplenia and polysplenia syndromes. Here, the pattern of spatial organization of the thoracic and abdominal organs demonstrates abnormal arrangement across the left-right axis of the body i.e. neither the normal (situs solitus) nor mirror image arrangement (situs inversus). 7. There is not one specific finding that is pathognomonic for situs ambiguous (heterotaxy) but rather there is a combination of findings seen in situs solitus and situs inversus. 9, 10.
Heterotaxy syndromes are conventionally grouped in two categories defined according to the status of the spleen and the morphology of the atrial appendages, bronchi, and lungs into the subsets of asplenia syndrome or right isomerism, and polysplenia syndrome, also known as left isomerism. 9, 10, 11. The distinction between the two groups is based on the common concurrence of different abnormalities found with this disorder. The polysplenia syndrome is usually observed in patients with bilateral left sidedness, a condition in which both lungs resemble the left lung. The asplenia syndrome may be associated with a bilateral right sidedness, a condition in which both lungs morphologically resemble the right lung. 9, 10, 11, 12. The relation between left isomerism and polysplenia, right isomerism and asplenia is close, but not one to one, a spleen can be found in right isomerism, just as the spleen can be absent with left isomerism.12. This classification may provide a helpful starting point for a mental organization that allow the clinician to predict structural and physiological abnormalities based on patterns but they are not the rule. 12 Due to morphological variability within the cases, there is no single classification that encompasses the wide spectrumof findings found with this disorder. On account of that, some clinicians advocate referring to it as left atrial isomerism followed by a specific description. 13. We present four cases diagnosed in our department in a period of 16 months. With these four cases and a review in the literature, we explore the definitions and characteristics of left atrial isomerism and we provide a new diagnostic tool of fetal situs anomalies.
Materials and Methods
We present 4 cases diagnosed with left atrial isomerism in our department in a period of 16 months. With these 4 cases and a review in the literature, we explore the definitions and characteristics of left atrial isomerism and we highlight the value of 3D ultrasound in the prenatal assessment of atrial isomerism syndromes.
Examinations were performed via Voluson 730 Pro (General Electric, Milwaukee, WI, USA) with a volumetric abdominal transducer (4–8 MHz). Stored cardiovascular volumes were prospectively and subsequently analyzed offline. Volume datasets were evaluated by an independent examiner who was not blinded to the previous diagnoses of cardiac anomalies per 2D ultrasound. Sonography images were then sent via the internet to a diagnosis reference center (Caen Teaching Hospital, France), and prenatal the initial diagnosis was confirmed or revised. A multidisciplinary team—including a pediatric cardiologist, a neonatologist, and a pediatric cardiac surgeon provided comprehensive prenatal counseling to each expectant mother. Neonatal echocardiography was used to confirm the prenatal diagnosis in surviving fetuses.
Results
In our study, three patients had an interruption of the IVC (Figure2 b, c), the first patients had severe cardiac malformation and 2 patients had a persistent left superior vena cava (LPSVC) (Figure 4 a, b). The four patients had ultrasonographic signs for situs ambiguous (left isomerism) and in 3 of them the diagnosis was confirmed by fetopathological examination. The first patient had an unfavorable outcome (pregnancy termination “hydrops foetalis”) and this was linked to severe heart disease. The second case with no sever cardiac malformation delivered at 27+6 weeks’ gestation and child had psychomotor retardation which appears to be related to extreme prematurity. All the three karyotypes were normal, research 22q11 microdeletion was negative. " Double vessel sign " was found in all cases with interruption of the IVC with azygos continuation -VCI. (Figure 3 b, c). Grayscale facilitated the diagnosis of situs (Figure 1). Power Doppler imaging contributed primarily to prenatal diagnosis of vascular anomalies, and it was beneficial in detecting situs (Figure 2). 3D ultrasound and Doppler enhanced the visualization of fetal vessels. Using volumes, meticulous offline evaluation can be performed, enabling the operator to reconstruct fetal anatomy. 2 patients had the stomach in the right side, one of them without congenital heart disease. (Figure 1 d , 3b). Figure 5.
Figure 1.a)Case control, 3D volume of normal situs solitus (28 weeks’ Gestation). The heart and stomach are on the left; the gallbladder is on the right, liver is predominantly on the right side. b,c) Dextrocardia , echo-anatomic correlation. D) Stomach are on the right side , Apex of the heart is on the left.e,f) Liver in the median position (echo-anatomic correlation), appendix and gall bladder ((white asterisk) are on the left side, rectosigmoid is on the right side.g)Nonrotation , the entire small bowel localizing to the right abdomen and colon localizing to the left abdomen. h- Liver in the median position (echo-anatomic correlation with g). i) Grey scale frontal view, showing the characteristic “double-bubble” appearance of the stomach and duodenum, note that the apex of the heart is toward the stomach i.e. left side.j) (echo-anatomic correlation with i) D1 first part of duodenum , S stomach , *** Ladd's bands (cause of obstruction).A). Apes of the heart S: Staomach R: Right L: Lefi Li: Liver . H: Hand denting apex of the heart GB: Gall Bladder.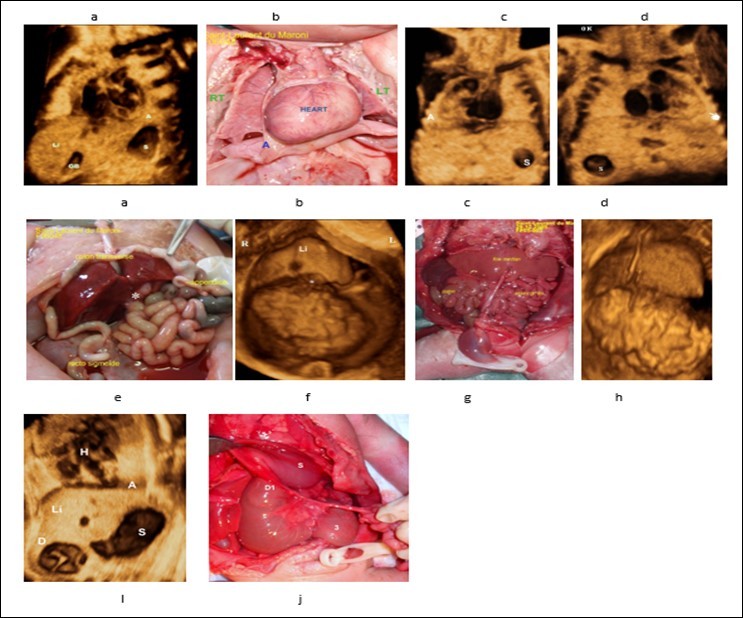
Figure 2.Three-dimensional ultrasound in glass body mode of a parasagittal view
Figure 3.Four-chamber views in four fetuses: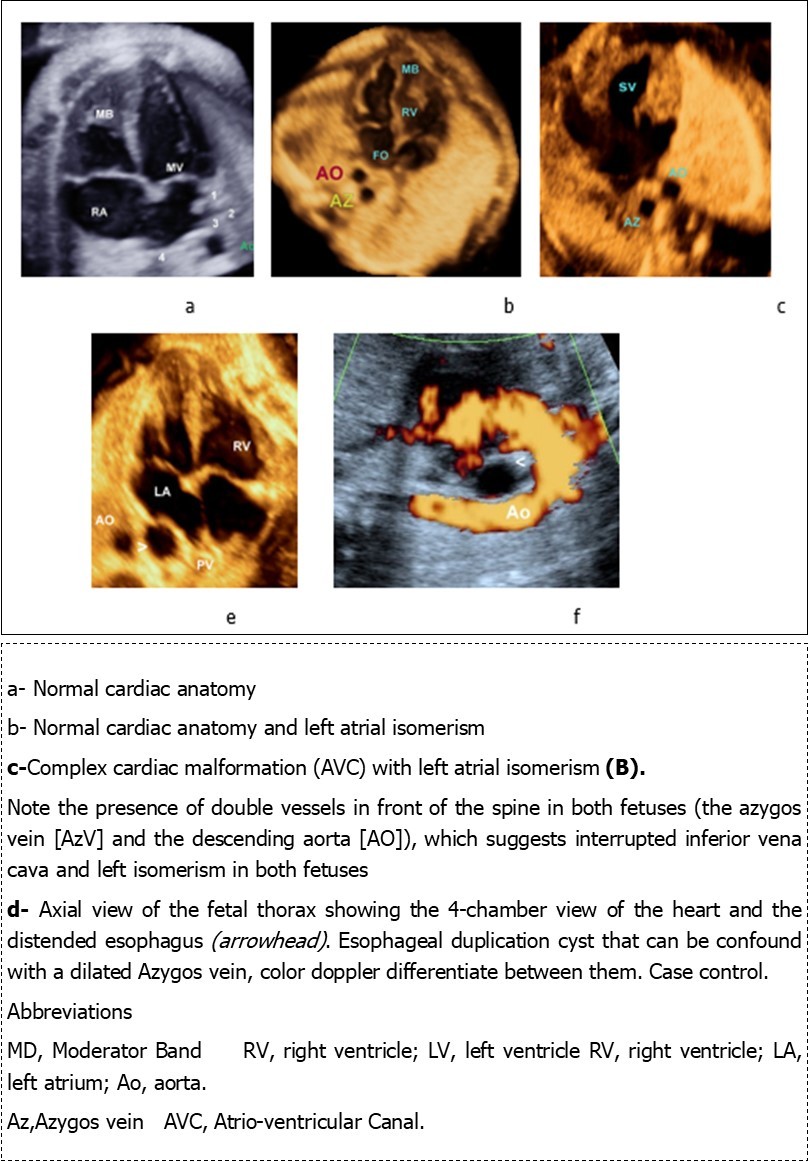
Figure 4.a-Three-vessel-trachea view showing the persistent left superior vena cava located left of the pulmonary artery. b-Persistent left superior vena cava draining into the dilated coronary sinus and to the right atrium, the coronary sinus is aneurysmal. c-Three-dimensional ultrasound in glass body mode showing the Azygos vein and Aorta. d- Anomalous hepatic venous drainage directly into the right atrium. e, f- Aortic coarctation (arrow head), note the presence of coarctation shelf (arrow). Abbreviations: RA: right atrium AO: aorte UV: umbilical vein AP : Pilmonary artery PV: Portal vein DV : Ductud venosus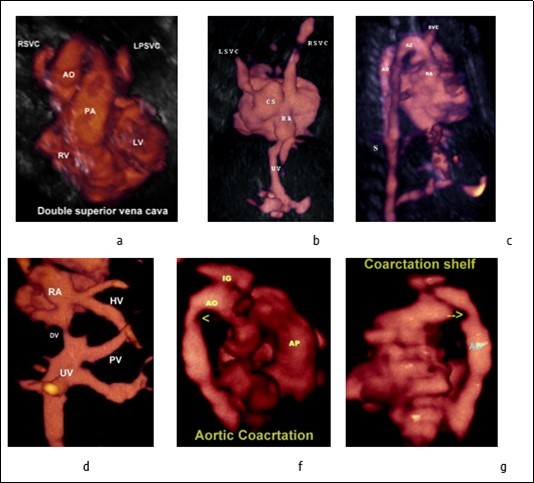
Figure 5.a-Fetopathological examination showing dilated azygos. b- Sagittal image demonstrating the dilated azygos vein and azygos arch connecting to the superior vena cava (*). c-Aortic arche in the same patient, the aortic arche is distinguished from the its branches (arrow heads).e-Coronal planes of the chest and abdomen in a fetus with left atrial isomerism and interrupted inferior vena cava showing the azygos vein (AzV) running parallel and posterior to the descending aorta (on both sides of the spine).f- Fetopathological examination showing azygos and aorta.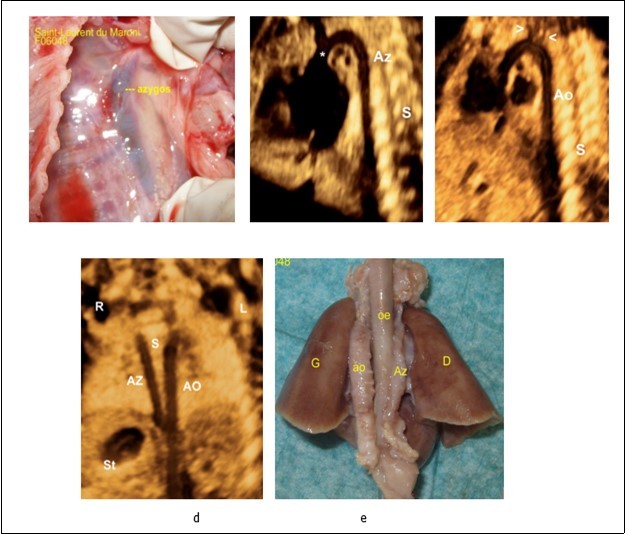
One patient had dextrocardia in which the diagnosis was evoked by by Doppler imaging following localization of the apex of the heart and axis of the left hepatic vein on opposite sides, both left hepatic vein (LHV) and the apex of the heart are in the same side and point to the same direction i.e. downwards, the cardiac apex points to an opposite direction with respect to the spine i.e. away from the spine. (Figure 2d). In levocardia the cardiac apex is oriented away from the spine, on the other hand, in dextrocardia, the cardiac apex is oriented toward the spine (Figure 2). The 4 patients had a liver in the median position , one patient had the appendix appendix and gall bladder ((white asterisk) are on the left side, rectosigmoid is on the right side.(Figure 1 a,b,c,d,f). And another patient had intestinal nonrotation, the entire small bowel localizing to the right abdomen and colon localizing to the left abdomen. (figure g,h). One patient had congenital duodenal obstruction caused by Ladd's bands (Figure 1 I,j)
Abbreviations
A, apex of the heart;
AO, aorta;
AZ, azygos vein;
CS, coronary sinus;
DV, ductus venosus; LHV,
left hepatic vein; LSVC,
left superior vena cava;
PLSVC, persistent left superior vena cava;
PV, portal vein;
PVs: pulmonary veins;
RA, right atrium;
RSVC, right superior vena cava;
SVC, superior,
S: spine. St: stomach.
T, thorax;
UV, umbilical vein.
VCI, IVC: inferior vena cava.
HV: Hepatic vein.
Discussion
The earliest recorded example of a case of asplenia with a malformed heart that of Martin in 1828. 15. Biron Ivemark noted the association of spleen anomalies with some cardiac malformations like atrioventricular canal defects and conotruncal anomalies, he published in 1955 in Acta Paediatrica his landmark paper which included analyses of all cases in the published literature as well as his own 14 cases , this paper was one of the first to recognize the association between splenic status, complex congenital cardiac disease, and abnormal arrangement of the viscera, focusing on the tendency to symmetry, and his name is linked as “Ivemark’s syndrome” with this constellation of anomalies 10, 15, 16. Polhemus recognized that asplenia and polysplenia were associated with complex congenital heart disease. 17. Polysplenia was overlooked as a marker of HS until Moller and his colleagues in 1967 first fully documented the polysplenia syndrome, in their breakthrough paper they correlated their own findings with the literature and showed the relation between polysplenia and bilateral left-sidedness syndrome. 15, 18. Van Mierop et a1. emphasized the association between asplenia and bilateral right sidedness 19, 20. Putschar and Mannion referred to a ‘symmetrical situs’ that sometimes exists, exhibiting symmetrical rightness or leftness on both sides. Although terminology has evolved, this is probably the most eloquent description of isomerism in the historical literature. Van Praagh regrouped these cardiac malformations into 2 groups, those that are more frequent with asplenia (right isomerism) and theses that are more associated polysplenia (left isomerism).
Van Mierop 19 described the concept of the left and right atrial isomerism that was not universally accepted. 22. Van Praagh et al. 24 have pointed out that the concept of bilateral or two right atria and bilateral or two left atria is anatomically unrealistic because atrial chambers as a whole are not entirely isomeric 10 , so this concept of atrial isomerism was refined to the right and left atrial appendage isomerism by McCartney and Anderson 25. Of note, true isomerism of the atrial appendages (considered in isolation) has been demonstrated previously. 26. Therefore, the concept of isomerism of the right and left atrial appendages are therefore more accurate. 10. Left atrial isomerism syndrome is usually observed in patients with bilateral left sidedness. Other common findings are left azygos continuation of the inferior vena cava, gastrointestinal malrotation, biliary atresia and absence of the gallbladder and abnormal cardiac or stomach position. 27, 28.
Absence of the hepatic segment portion of the IVC with azygos continuation into the right or left SVC is referred to as an interrupted IVC and it have been reported as an incidental finding at autopsy as early as 1793 by Abernethy in a 10-month-old infant with polysplenia and dextrocardia. Moller et al 18 emphasized the association, 11 and now it is considered an excellent marker for the presence of left atrial isomerism. a finding that occurs in about 80%. Therefore, a careful examination of the IVC should be performed in the suspected heterotaxy patient. 24, 28. In this condition, the venous drainage from the lower extremities reaches the superior vena cava via the azygos vein (azygos continuation) or via the hemiazygos vein (hemiazygos continuation) emptying into either a right-sided superior vena cava or into a persistent left superior vena cava. It can be recognized by the observation of the aorta and the (dilated) azygos vein on its right or left side (hemiazygos) either in the upper abdomen or at the level of the four-chamber view 31. Sheley et al 29 described it as the ‘double-vessel sign’ (Figure 3) and found it in all eight fetuses with left isomerism that they examined, but also in one false-positive case with right isomerism. If the examiner is aware of this sign, he can easily detect it prenatally on real-time imaging and confirm it using color Doppler. Three of our patients presented this sign (Figure 3), care should be taken not to confound it with other conditions that mimic a ‘double-vessel sign’, for example, esophageal duplication cyst, that can be confound with a dilated azygos vein in 4 chamber view, color doppler can differentiate between the two conditions. (Figure 3 d, f).
Bilateral superior vena cava (SVC) occurs in about 41 % of cases of left atrial Isomerism and in 36 % cases of asplenia or right atrial Isomerism. 11 A (PLSVC) was diagnosed in two patients, with 3D ultrasound and Doppler, we have been able to reconstruct the 3D anatomy of the persistent left superior vena cava draining into the dilated coronary sinus and to the right atrium (Figure 4 b); moreover, reconstructing the 3-vessel view, a fourth vessel (PLSVC) is seen on the left side of the pulmonary artery. (Figure 4 a).). In left atrial isomerism, multiple spleens, from 2 to 16, can be found, usually along the greater curvature of the stomach. 12. Anomalies of midgut derivatives include nonrotation, incomplete rotation, and the rare reversed complete or incomplete rotation. 30
One of our patients had nonrotation with the entire small bowel localizing to the right abdomen and colon localizing to the left abdomen and another patient had incomplete rotation), appendix and gall bladder ((white asterisk) are on the left side, rectosigmoid is on the right side. (Figure 1 e, f)
A mismatch between the position of the fetal stomach and cardiac apex may be one of the first signs indicating atrial isomerism. 27. 2 patients had the stomach in the right side, one of them without congenital heart disease. (Figure 1 d, Figure 3b).
In our previous work 31, we demonstrated that, in parasagittal view, both left hepatic vein (LHV) and the apex of the heart are in the same side and point to the same direction. Thus , the diagnosis of dextrocardia is achieved by Doppler imaging following localization of the apex of the heart and axis of the left hepatic vein, furthermore, in normal position (levocardia) the cardiac apex is oriented away from the spine (Figure 2 a) , on the other hand, in dextrocardia, the cardiac apex is oriented toward the spine (Figure 2 d ) , to the best of our knowledge , this the first study evoking the diagnosis of situs using these parameters (orientation of cardiac apex with regard to LHV and spine). Another example demonstrating the utility of this parasagittal view is shown in (Figure 2 e, f), the LHV is pointing in the opposite direction to the cardiac apex i.e. upwards toward the thorax, a diagnostic clue to diaphragmatic hernia, in this case e diagnosis was confirmed by fetopathological examination. In addition, Grayscale facilitated the diagnosis of situs and confirmed the diagnosis of dextrocardia and right-sided stomach and midline position of the liver (Figure 1).
Any deviation from this standard anatomic position (cardiac apex and LHV are in the same side and point to the same direction i.e. downwards on the other hand cardiac apex points in an opposite direction from the spine), using either Galss body mode or power Doppler or Doppler angiography or greyscale would be necessities further evaluation. For example, (Figure 2 d) the cardiac apex and the LHV are in opposite directions and the cardiac apex points toward the spine, denoting an abnormal cardiac axis (Dextrocardia), thus using this parasagittal view, it is possible to diagnose this abnormality using either Doppler angiography with or without glass body mode.
Table 1. Summary of patients| Case 1 | Case 2 | Case 3 | Case 4 | |
| Heart position | Dextrocardia | Levocardia | Levocardia | Levocardia |
| Stomach | Left | Right | Right | Left |
| IVC | Interruption | Interruption | No | Interruption |
| Interruption of IVC with azygos continuation | Yes | Yes | Yes | Yes |
| Cardiac malformations | AVC- Single atrium (SA)Anomalous hepatic venous drainage directly into the right atrium | LPSVC | AVCAortic coarctationLPSVC | Aortic arche hypoplasiaSingle ventricle |
| Digestive anomalies | Midline liverPolysplenia.Intestinal malrotationAppendix on the right side | Midline liver | Midline liverIntestinal nonalrotation | Midline liverduodenal obstruction from Ladd bands, |
| Caryotype | 46XX | 46XY | 46XY | 46XX |
| Outcome | Pregnancy termination | Delivery at 27+6 weeks | Pregnancy Termination | Pregnancy Termination |
Conclusion
Left atrial isomerism is diagnostically challenging due to complex spectrum of findings. To our knowledge, this is the first study in which atrial isomerism is evoked based on study of the cardiac apex, the LHV and assessment of the vena cava (IVC) in parasagittal view. In structurally normal heart with levocardia, with presence of a normal IVC and a right sided stomach, the chances of having left isomerism would be very low. We believe that parasagittal view demonstrating the heart and the abdominal vessels is easy to obtain and interpret , offer a realistic anatomic image , needs no mental reconstruction of spatial relationships and is very beneficial mainly in detecting the situs and provides an added tool for the diagnosis of other anomalies and we propose to obtain this view , if not routinely, in all cases suspected of situs anomalies. We recommend to use 3D ultrasound and doppler angiography systematically in suspected cases of left atrial isomerism, and better understand and interpret fetal anatomy.
References
- 1.Daniel T Grimes. (2019) Making and breaking symmetry in development, growth and disease Development 146(16).
- 2.Koefoed Karen.Iben Rّnn Veland.(2014). Lotte Bang Pedersen Lars Allan Larsen, and Sّren Tvorup Christensen, Cilia and coordination of signaling networks during heart development. , Organogenesis 10(1), 108-125.
- 3.Chen Q, Shi J, Tao Y, Zernicka-Goetz M. (2018) Tracing the origin of heterogeneity and symmetry breaking in the early mammalian embryo. , Nature Communications 9(1), 1819.
- 4.Liu S, Chen W, Zhan Y.(2019).DNAH11 variants and its association with congenital heart disease and heterotaxy syndrome. Sci Rep 9.
- 5.Onoufriadis A, Paff T, Antony D, Shoemark A, Micha D et al. (2013) UK10K Splice-site mutations in the axonemal outer dynein arm docking complex gene CCDC114 cause primary ciliary dyskinesia. , Am J Hum Genet 92, 88-98.
- 6.Babu Deepak, Roy Sudipto. (2013) Left-right asymmetry: cilia stir up new surprises in the node. , Open Biol 3, 130052.
- 7.Jacobs J P, Anderson R H, Weinberg P M. (2007) The nomenclature, definition and classification of cardiac structures in the setting of heterotaxy. , Cardiol Young 17, 1-28.
- 8.Dilli Alper. (2012) Salih Sinan Gultekin, Umit Yasar Ayaz, Hatice Kaplanoglu, and Baki Hekimoglu. in Medicine Volume 2012 Article ID 1-5.
- 9.Lagrotta Gustavo, Moises Melanie. (2020) Heterotaxy Polysplenia Syndrome in Adulthood: Focused Review and a Case Report.”. , Cureus 12(1), 1-10.
- 10.Ryerson L M, Pharis S, Pockett C. (2018) Left atrial isomerism and Intestinal Rotation Abnormalities. , Pediatrics 142(2), 20174267.
- 11.Ilian A, Motoc A, Balulescu L, Secosan C, Grigoras D et al. (2020) A Case Report of Left Atrial Isomerism in a Syndromic Context. , Genes 11, 1211.
- 12.Patrick W O'leary. (2012) Cardiac Malpositions and Abnormalities of Atrial and Visceral Situs. Heart Disease in Infants, Children, and Adolescents , 8th Ed Lippincott Williams & Wilkins In:David J. Driscoll,Robert E.Shaddy,Timothy F.Feltes, editors, Moss and Adams' 53, 1195-1216.
- 13.Meneghetti Caren. (2014) Gonçalves et al, Heterotaxy syndrome: a case report, Radiol Bras. 47(1), 54-56.
- 14.W El Guindi, Dreyfus M, Carles G, Lambert V, Herlicoviez M et al. (2013) 3D ultrasound and Doppler angiography for evaluation of fetal cardiovascular anomalies. , International Journal of Gynecology & Obstetrics 120, 173-177.
- 15.Mishra Smita. (2013) Heterotaxy syndrome. In :I. B. Vijayalakshmi,P.SyamasundarRao,ReemaChughA Comprehensive Approach to Congenital Heart Diseases ; 10 145-165.
- 16.Ivemark B I. (1955) Implications of agenesis of the spleen on the pathogenesis of conotruncus anomalies in childhood. Acta Paediatr; 44(Suppl 104):. 7-110.
- 17.Polhemus D W, Schafer W B. (1952) Congenital absence of the spleen; syndrome with atrioventricularis and situs inversus; case reports and review of the literature. , Pediatrics 9, 696-708.
- 18.Edwards J E. (1967) Congenital cardiac disease associated with polysplenia . A developmental complex of bilateral" left-sidedness.". , Circulation; 36, 789-99.
- 19.Van Mierop LHS, Wigglesworth F W. (1962) Isomerism of the cardiac atria in the asplenia syndrome. , Lab Invest; 11, 1303-15.
- 20.Van Mierop LHS, Gessner I H, Schiebler G L. (1972) Asplenia and polysplenia syndrome. Birth Defects: Original Article Series;. 1, 74-82.
- 21.Robert H Anderson, Edward J Baker, Daniel J Penny, Andrew N Redington, Michael L Rigby et al.(2010).Paediatric cardiology, Copyright by Churchill Livingstone, an imprint of Elsevier Ltd.,Philadelphia,PA19103-2899,Steven. 460-483.
- 22.S Van Praagh, Kreutzer J, Alday L. (1990) Systemic and pulmonary venous connections in visceral heterotaxy, with emphasis on the diagnosis of the atrial situs:a study of 109 postmortem cases. In: Clark EB, Takao A (eds) Developmental cardiology. Morphogenesis and function. Futura, Mount Kisco. 671-727.
- 23.Soto B, Pacifico A D. (1990) Angiocardiography in Congenital Heart Malformations. Mount Kisco,NY:Futura.
- 24.Robert M Freedom, Yoo Shi-Joon, Mikailian Haverj, William G. (2004) The Natural and Modified History of Congenital Heart Disease;Thomas Gilljam,Robert M. Freedom,and Shi-Joon Yoo , The Syndrome of Isomeric Left Atrial Appendages, Often Associated with Polysplenia, by Futura,an imprint of Blackwell Publishing. 34, 430-434.
- 25.Macartney F J, Zuberbuhler J R, Anderson R H. (1980) Morphological considerations pertaining to recognition of atrial isomerism. Consequences for sequential chamber localisation. , Brit Heart J 44, 657-667.
- 26.Uemura H, Ho S Y, Devine W A. (1995) Atrial appendages and venoatrial connections in hearts from patients with visceral heterotaxy. , Ann Thorac Surg; 60, 561-569.
- 27.Thomas C, Sawyer S N.Prenatal Findings in Left Atrial Isomerism and an Overview of Heterotaxy Syndrome. , Journal of Diagnostic Medical Sonography 34(2), 148-154.
- 28.Agarwal R, Varghese R, Jesudian V. (2020) The heterotaxy syndrome: associated congenital heart defects and management. , Indian J Thorac Cardiovasc Surg
- 29.Nyberg D A. (1995) Azygous continuation of the interrupted inferior vena cava: a clue to prenatal diagnosis of the cardiosplenic syndromes. , J Ultrasound Med; 14, 381-7.
Cited by (2)
This article has been cited by 2 scholarly works according to:
Citing Articles:
W. E. Guindi, M. Youssef, Gabriel Carles, M. Dreyfus, S. Elsayed - Integrative Gynecology and Obstetrics Journal (2021) Semantic Scholar
