Abstract
Personal Protective types of Equipment (PPE) are needed for everybody who would be in danger of threatening state; the COVID-19 pandemic raised the need and global demand for PPE, one of the most used and required equipment are gowns, coveralls, and torso protectors; which their shortage of supply raised the cost globally too. This review article gathered the guidelines and recommendations from manufacturers, international organizations, and self-experiments of authors for these utilities. And, provides recommendations on the level of protection needed for each condition.
Author Contributions
Academic Editor: Raul Isea, Fundación Instituto de Estudios Avanzados - IDEA, Hoyo de la Puerta, Baruta.
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2021 Mohammad Meshkini, et al.
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Background
Pandemics and epidemics like lately COVID-19 could challenge the needs and demand' supplies for healthcare workers’ Personal Protective Equipment (PPE). There are different guidelines, protocols, and resources among countries, organizations, and people worldwide. Using coveralls that were mostly seen in the Ebola Outbreak and Zika Virus during the field management, in the later COVID-19 pandemic may be a source of stress for facilities and providers of how many and how much they could provide, however, have the principle like “no visible skin” in mind could lower this stressful condition and achieve better mental and occupational health during crises. Also, training should focus on whether it is indicated to use the protections and what should be done for:
standard protection level (i.e. routine caregiving)
Respiratory protection level (conditions like the COVID-19, air-borne diseases)
Hematologic/fluid protection level (conditions like the Ebola Outbreak, splash and chemical hazards)
Methods and Materials
The primary draft of this article was based on Interim World Health Organization (WHO) and Center of Diseases Control and Prevention (CDC) guidelines and updates or recommendation protocols from textile manufactures and suppliers for gowns and coveralls use, extended use, reuse, and disinfection methods; Also some self-experiences of applying these methods by authors for about 50 days period of COVID-19 incidence in Iran. However, it was not published at that time and has been reviewed after 15 months of clinical experience of methods and revising in some of the recommendations according to the published evidence and self-experiments.
Results
We have reached three general guidelines from WHO about PPE use for healthcare providers 1, 2, 3, also informative web pages and blog posts from local manufacturers and dealers about non-woven fabric like spun-bond and melt-blown which are the fundamentals of these products. However, there were dealers with reusable (i.e. heavy-duty) products that have been assessed for this purpose too. Also, a Cochrane review about breathable and non-breathable fabric showed better tolerance of providers with the same amount of protection in favor of breathable fabric 4. Through the Ebola outbreak WHO provided a useful questionnaire that could be used for addressing the recommendations of this paper or any other PPE guidelines for personnel use 5.
Discussion
All health care workers and who may be in direct or indirect with the blood or body fluid of blood-borne infection must wear protective body-wear that:
Covers all skin and mucus membrane
Should be waterproof and impenetrable to viruses and fluids
empowered if needed to gain more accuracy of protections
recommended to be done under the supervision of a fellow with a checklist to reduce the probability of breach in the donning and doffing of the PPE 6.
Coveralls seems to be introduced while Ebola Outbreak in 2015 and also are known as “Ebola PPE” too; however using gowns may be preferred among health care providers due to the following statements, there is no strong recommendation for or against any of these options, and the comfort of the user is mandatory:
The most crucial in choosing between gown or overall is the comfort of the user during the working shift, ease, and freedom of activity in the wearing.
Gowns may be preferred due to their familiarity among health care providers and better compatibility with donning and doffing them.
In some cultures, it’s not acceptable for women to wear coverall-like body wears, and therefore gowns are tolerable.
Gowns may be better tolerable in heat climate.
In case the coverall’s size doesn’t fit the provider, two gowns may protect the provider’s torso when the first one is putting on like a casual coat and protect the back, then the second one should be done as usual to protect the front.
It’s not recommended to reuse the gowns or aprons in WHO guidelines, which means as they have been contaminated, they should be taken off and done by new body wears. However, note that in case of resource shortage, using heavy-duty products that could be disinfected between patients and at the end of working shifts may be logical.
Either use of heavy-duty and reusable gown, apron or coverall, the headcover or whatever part that would be responsible for protecting the head and face and is donning and doffing through the head, shouldn’t exceed from the nipple line length to reduce the probability of pathogen transmission during doffing the PPE.
And to remind leaning forward while doffing any PPE that is used for head and neck region protection.
Whenever the separate head-cover is not available, a coverall with a hood can be worn after donning the facial and respiratory protectors, which maintains the mucosal protection after taking off the hooded coverall.
A plastic Apron may be used on the gown or coverall to add impenetrable efficacy to the fabric.
The footwear that is used by healthcare providers in the crisis of blood-borne infection site, should be waterproof and washable.
It’s recommended to wear waterproof boots (rubber/gum boots) over shoes due to their optimal protection against pathogens and better protection when the floor is wet.
Boots also can stay in place while the whole working shift time and easily get cleaned or disinfected if needed.
If the provider prefers to use shoes, they should be closed shoes that may seal the dorsum of the foot better; and it’s recommended to put on waterproof covers that their length may cover up to the mid-calf region.
As a full set of PPE is mandatory for all health care workers that may be in direct or indirect contact with blood-borne pathogens; the use of a full set of PPE is not recommended for air-borne diseases and this could be a resource management capability during crisis and resource shortage. Figure 1, Figure 2, Figure 3 demonstrate CDC’s posters for droplet, contact, air-borne precautions signs. Figure 4 shows Point of Care Risk Assessment and Infectious Control by British Columbia.
Figure 1. CDC’s Droplet Precautions Sign
Figure 2. CDC’s Contact Precautions Sign
Figure 3. CDC’s Airborne Precautions Sign
Figure 4. Point of Care Risk Assessment and Infectious Control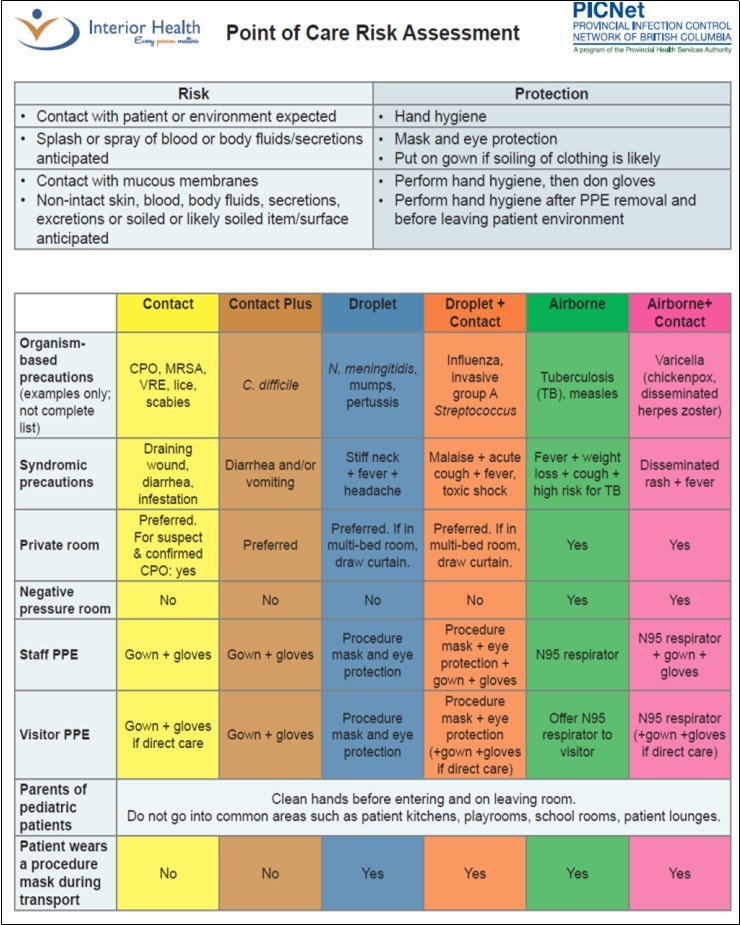
Conclusion and Summary of Studying
Choosing gown or coverall depends mostly on providers’ comfort of use.
Breathable fabric may protect the same as non-breathable also provide better comfort and less heat stress for providers.
The apron may be used on gown or coverall to strengthen its impenetrability.
Doffing all PPE which is worn through head and neck should be provided in a leaning forward position to reduce the risk of eye and mucous contamination.
Foot wear should be impenetrable, seal the dorsum of the foot, and washable; it’s also recommended to use a cover on the foot wear that may extend to the calf and been fixed in place.
In the time of supply shortage, using heavy-duty materials could be logical to both protect the providers and reduce the budget. Also, providers should be aware of indications for contact, droplet, and air-borne precautions.
Acknowledgments
It’s our honor to give the best of wishes to our families, who support us through this pandemic, they are our superheroes and the best of the glory belongs to them. Also, “OpenAccessPub” for all of the support and providing an environment to publish our paper.