Abstract
Auto transplantation is a fast and economical option when a suitable donor tooth is available for replacement of a tooth considered impossible to treat. The purpose of this case report is to describe methods used for autotransplantation and its advantages for cases with a missing bilateral mandibular firstmolar, as compared with a dental implant, removable partial denture, and other methods of prosthesis. In the present patient who underwent auto transplantation, clinical and radiographic outcomes were considered satisfactory at one and two years postoperatively. Bone healing was observed around the roots of transplanted teeth, which showed good function. In autotransplantation cases, even when the donor tooth has complete root formation, a high success rate can be achieved when the patient is properly selected and treated. Although the chance of root resorption remains because of necrotic pulp and periodontal irritation during manipulation, auto transplantation should be considered as a good treatment modality in feasible cases. Based on the present findings, even though autotransplantation is not common in general dental practice, we consider that it offers a clinically and economically viable alternative as compared to other more complicated prosthetic and dental implant treatments.
The purpose of this report is to show that auto transplantation is a superior treatment method for single molar defects as compared to other prosthetic methods, as the periodontal ligament of the patient can be used and cutting adjacent teeth is avoided. In addition, it is a treatment method that can effectively utilize a wisdom tooth.
Author Contributions
Academic Editor: Abu-Hussein Muhamad, Arab-American University.
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2021 Taichi Kasuga, et al.
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Introduction
Trauma and caries are some of the most common causes of early tooth loss 1, 2. Autotransplantation is a procedure used for transposition of a tooth from an extraction site to another site or a surgically formed recipient site in the same individual 1, 2, 3, 4, 5, 6, 7, 8, 9, 10, 11, and considered to be a viable treatment option for replacing a missing tooth or one that requires extraction due to caries, periodontal disease, endodontic failure, or some other reason 1, 3, 5, 9, 10. The procedure is also indicated for cases with traumatic tooth loss, a tumor, congenitally missing teeth, a cervical root fracture, or teeth with a poor prognosis, as well as patients with developmental anomalies from dental surgery or localized juvenile periodontitis, and also after jaw re construction 1, 6, 10, 12. For patients with congenitally missing or significantly compromised teeth, auto transplantation can provide a long-term, cost-effective, and biological solution when a suitable donor tooth is available 3, 11. Even in the event that an autotransplant tooth does eventually fail, bone and soft tissue conditions are likely to be conductive for subsequent implant treatment 11, 13
There are four types of prosthetics for a missing tooth; bridge, partial denture, implant, and auto transplantation, with the latter performed when a suitable donor tooth is available 3, 14. Different than with use of bridge, there is no need to cut the next tooth. Furthermore, as compared to a partial denture, which requires a removal method, auto transplantation is a fixed method. Thus, chewing efficiency is better with auto transplantation, while it is also less expensive as compared to implants 2, 3, 7
Auto transplantation is considered to be a superior method for restoring missing teeth because of proprioception with the periodontal membrane 12, with other advantages known as well, including cost-effectiveness, as noted above, preservation of proprioception, possibility of a postoperative orthodontic option 14, protection of adjacent teeth, a natural prosthetic rise form from the margin, ability to be used in growing children 1, 15, aesthetics 10, improvements of mastication and pronunciation 1, closure of a maxillary sinus fistula 16, maintenance of the natural shapes of the attached gingiva and interdental papillae 12, and formation of new alveolar bone 5, 7, 8, 13.
Since the 1990s, several studies have examined healing of periodontal tissues and the periodontal membrane, as well as dental root resorption, with the result being a rapid increase in transplant success rate, which has drawn clinical interest. Tsukiboshi reported a 90% survival rate and 82% success rate in 250 cases observed over a period of six years.4
In the present subject, the bilateral mandibular first molars were chosen for extraction due to a vertical root fracture and autotransplantation was selected. Based on the findings of this case report, we report advantages of autotransplantation, including cost-effectiveness 3, avoidance of use of implants, and restoration of the area of occlusal support for bilateral first molars.
Case Presentation
A 27-year-old female patient came to us with discomfort in the right lower jaw (Figure 1). Her primary symptoms were pain in the lower right tooth when biting and discomfort associated with not being able to chew well with the lower left single denture. The patient was married and had one young child, and previously received dental treatment in China, then had returned to Japan for childbirth and early childcare. The patient was a nonsmoker with moderate plaque control and medical history taking revealed no problems. In clinical and radiographic examinations, a root fracture was observed on tooth #46, which had been endodontic ally treated and restored with a full-cast metal crown. Periodontal probing revealed a pocket depth of 8 mm on the buccal center side of the tooth. No pain was detected with percussion and mobility of the tooth was normal. (Figure 1, Figure 2, Figure 3).
Figure 1. Clinical case of right auto transplantation. Panoramic view at initial examination.Tooth #46 was shown to be half decayed and a cystic lesion was found in the mesial root apex. Tooth #36 was lost, while #48 and #38 were present. There was a total of 29 teeth in the oral cavity. 
Figure 2. Pre-treatment X-ray findings. A cystic lesion was found in the mesial and distal roots apex, and root nodule of #46.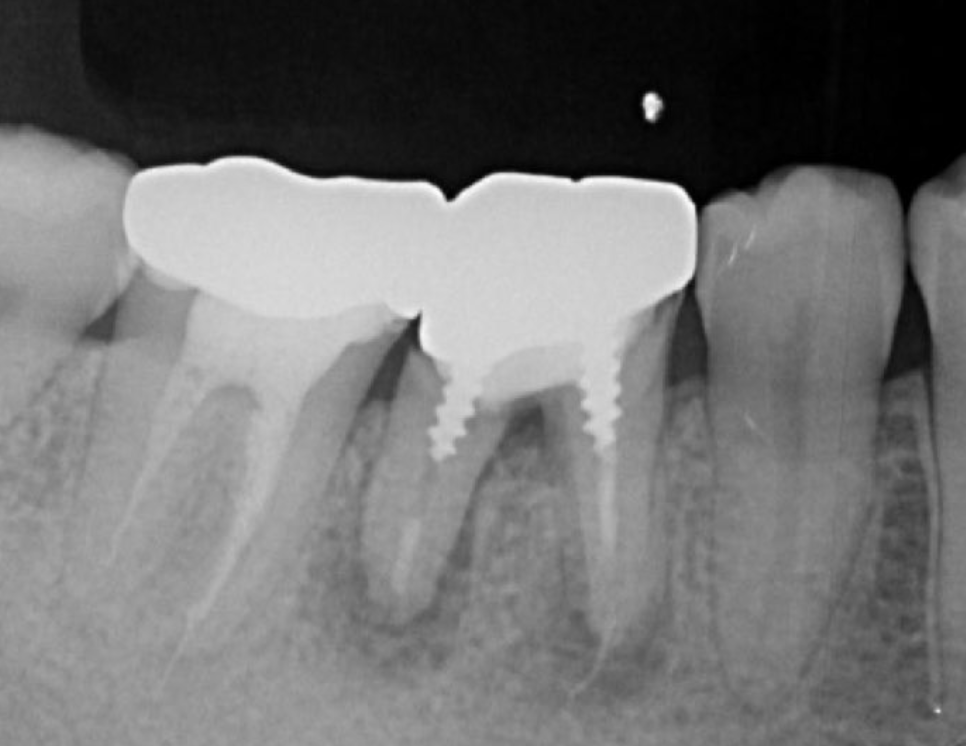
Figure 3. Preoperative intraoral findings. A metal crown was inserted at #46 and bleeding on probing during the periodontal pocket examination was noted.
Following detailed examinations, the situation was explained to the patient and autotransplantation was suggested as preferred treatment. Since a single-rooted wisdom tooth (#48) with no periodontal pathology and a root morphology similar to that of #46 was present, it was determined to be an adequate donor tooth
Full metal crowns were inserted for #46 and #47. Pathological mobility and bleeding on probing were not seen, and the transplanted tooth showed good function.
For this case, a bridge, partial denture, implant, and auto transplantation were each considered to be possible options, with the advantages and disadvantages of each explained to the patient. Her stated desire was for inexpensive treatment, preservation of adjacent teeth, and no denture, because she was not chewing well on the lower left side. In contrast to a bridge, a denture has the advantage of both adjacent teeth not being cut, while advantages of a bridge are that it is fixed and provides improved functionality. Also, in contrast to an implant, it is less expensive. After explaining these points and discussion with the patient, we decided to perform autotransplantation. Panoramic photograph findings showed that #48 had a complete root tooth with stage 7 growth 17, according to the Moorrees classification 18. Informed written consent was obtained from the patient prior to the procedure and treatments were performed according to the Declaration of Helsinki.
To determine adaptability of the donor tooth to the recipient site, the dimensions of both were carefully measured using CBCT images. It was thus determined that the morphology of the tooth root was a single root and the risk of damage to the periodontal ligament during extraction was estimated to be low.
The patient was given amoxicillin/clavulanic acid at 250 mg (Sawacillin Capsules, Japanese Pharmacopoeia, Japan) one hour prior to surgery. Under local anesthesia (GINGICAINE GEL, Hakusui Trading CO., LTD, Tokyo, Japan ), with an inferior alveolar nerve block used for tooth #46 alonb with 2% lidocaine and 1:80000 epinephrine (Dentsply, Tokyo, Japan), that tooth was separated and its fragments were gently extracted with a dental elevator. Granulation tissue was then removed and the socket was prepared with an internal cooling carbide bur. The graft bed was formed using the CT measurements as an index. Abundant rinsing with 0.05% chlorhexidine gluconate and sterile saline (OTSUKA NORMAL SALINE, Otsuka Pharmaceutical Factory, Inc., Tokushima, Japan) was performed to eliminate debris. Tooth #48 was gently extracted with forceps and dental elevators, and meticulously examined, and the absence of fractures was confirmed. Also, the periodontal ligament in the extracted graft tooth was observed and considered to be sufficient, then, after measuring length with a probe, it was stored in saline (Figure 4).
The tooth was immediately placed into the recipient site (Figure 5) and splinted with a methyl methacrylate (MMA)-based adhesive resin cement (Super-Bond C&B, Sun Medical; www.sun-medical.co.jp, Shiga, Japan), as there were some concerns regarding tooth stability. A 4-0 nylon suture (MANI; www.mani.co.jp, Tochigi, Japan) was used for better soft tissue adaptation and occlusal adjustment of the donor tooth was performed to remove any interference. The procedure time was 60 minutes, with time from extraction of the donor tooth until its placement in the recipient site 16 minutes (Figure 6).
Figure 4. Extraction of #48 was performed without damaging the periodontal ligament. Abundant periodontal ligament tissue could be seen.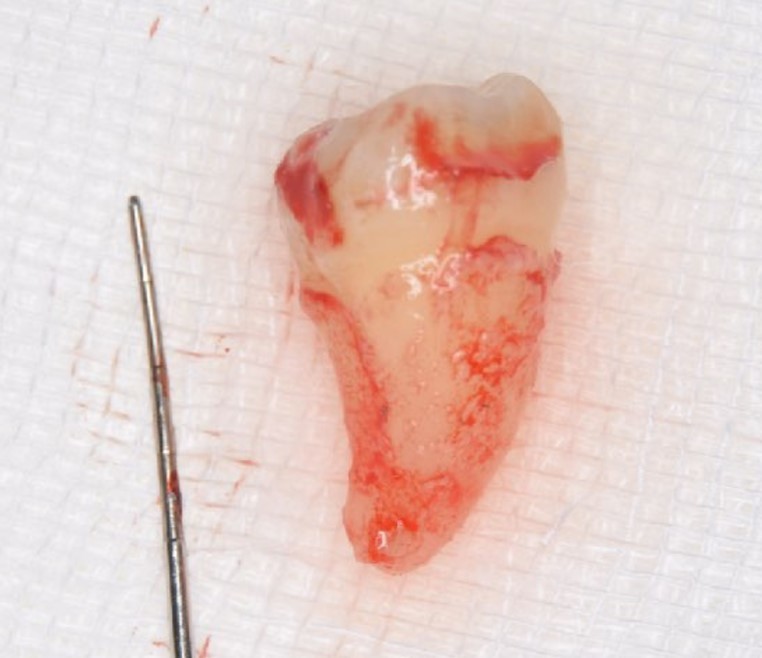
Figure 5. Confirmation of fit of donor tooth in socket. The metal crown for #47 was also detached during tooth extraction.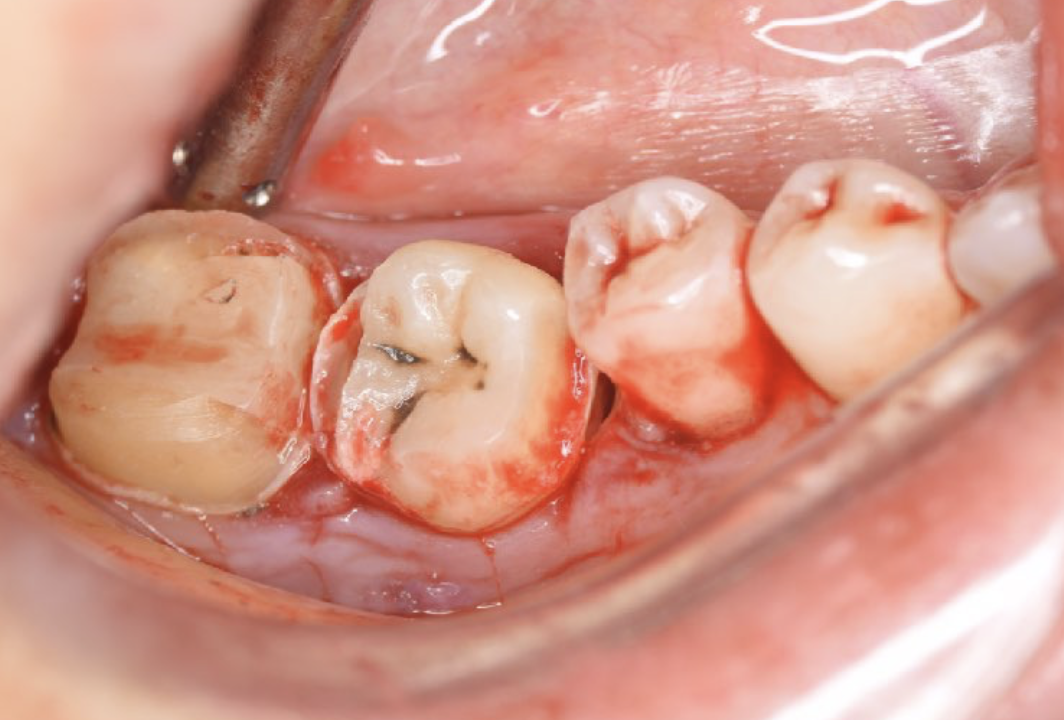
Figure 6. Dental X-ray image obtained after transplantation. 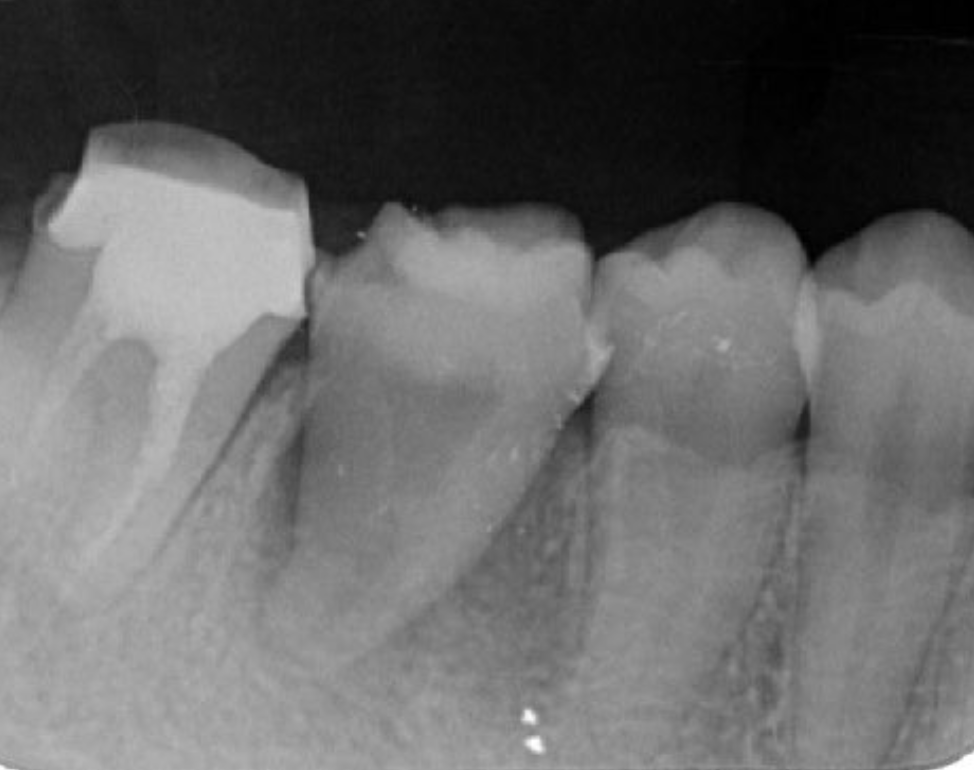
Following surgery, the patient was prescribed amoxicillin/clavulanic acid (Sawacillin Capsules, Japanese Pharmacopoeia, Japan) at 200 mg three times per day for five days as well as an anti-inflammatory analgesic (Loxonin, DAIICHI SANKYO COMPANY, LTD, Tokyo, Japan). She was also instructed to rinse with 0.2% chlorhexidine gluconate (Neosterin-green, Nippon Shika Yakuhin Co.,Ltd. Yamaguchi,Japan) three times per day for one week.
Endodontic treatment was initiated at 14 days after transplantation (8, 17). Root canal treatment for #48 was performed using Ni-Ti files (Pro Taper Next, Dentsply Sirona, Tokyo, Japan) to accommodate the complex morphology of the root canal and for minimal removal of the tooth structure during formation of the access cavity. Root canals were medicated with calcium hydroxide paste and then filled with gutta percha. The splint was also removed four weeks after the operation and a resin core was used as an abutment construction. In an attempt to appropriately modify contact and the crown morphology, a crown prosthesis was made with a full metal crown, with occlusal contact confirmed with use of a temporary crown and easy to visualize markings on occlusal paper. The full metal crown was cemented six months later (Figure 7).
Bone regeneration was confirmed before and after grafting, after root filling, and after placement of the prosthesis, based on X-ray imaging results (Figure 8). There was no pathologic mobility or pain during mastication, and the tooth showed good function. The patient was very satisfied with the treatment results (Figure 9).
Figure 7. Inter-oral photo obtained after treatment. Full metal crowns were inserted for #46, #47. Pathological mobility and bleeding on probing were not seen, and the transplanted tooth showed good function.
Figure 8. Cone beam CT image obtained after transplantation. Bone regeneration around the grafted tooth was confirmed.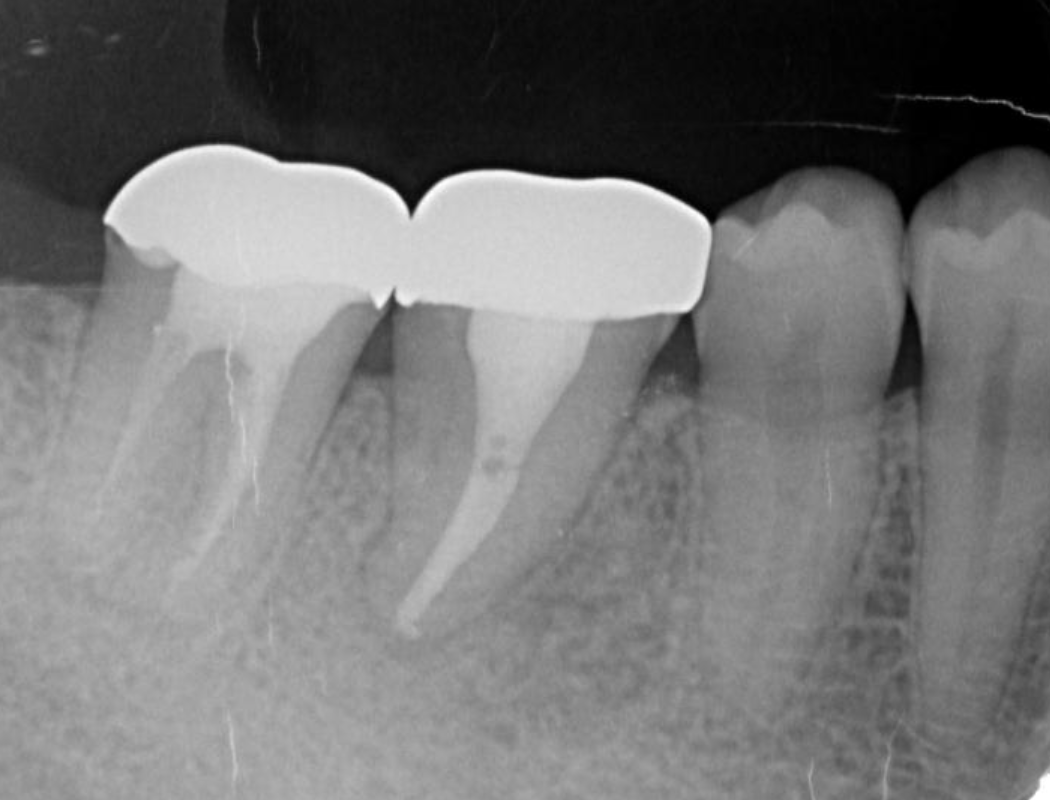
Figure 9. Dental X-ray image obtained two years after transplantation. Bone regeneration around the grafted tooth was confirmed.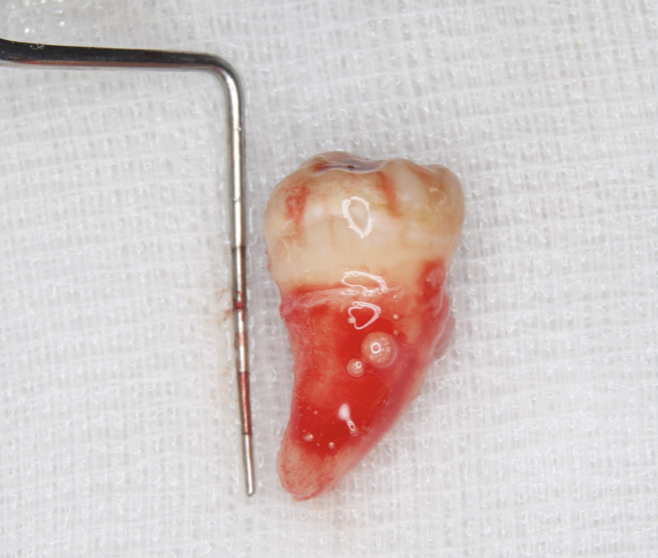
The patient requested auto transplantation in the lower left side jaw equivalent to #36, the tooth that was missing and replaced by a removable partial denture. The basic technique and procedure were the same as previously used for treatment of #48. Prior to the operation for #36, the buccal and proximal crown widths, and root length were measured using CBCT. In such cases, it is considered important to confirm the location of the inferior alveolar nerve, as well as the amount and depth of bone cutting needed by use of preoperative CT findings so as to prepare for treatment and ensure that the donor tooth can be placed smoothly in the socket (Figure 10). A trial application went smoothly, because the tooth was formed so as to be slightly larger than the root from the donor tooth (Figure 11, Figure 12).
Figure 10. Clinical case of left autotransplantation. Extraction of #38 was performed without causing damage to the periodontal ligament, which was found to be abundant.
Figure 11. Dental X-ray image obtained after autotransplantation from #38 to #36. The donor tooth root canal appeared to be blanched.
Figure 12. Intraoral photo obtained after setting the donor tooth into the socket of the recipient.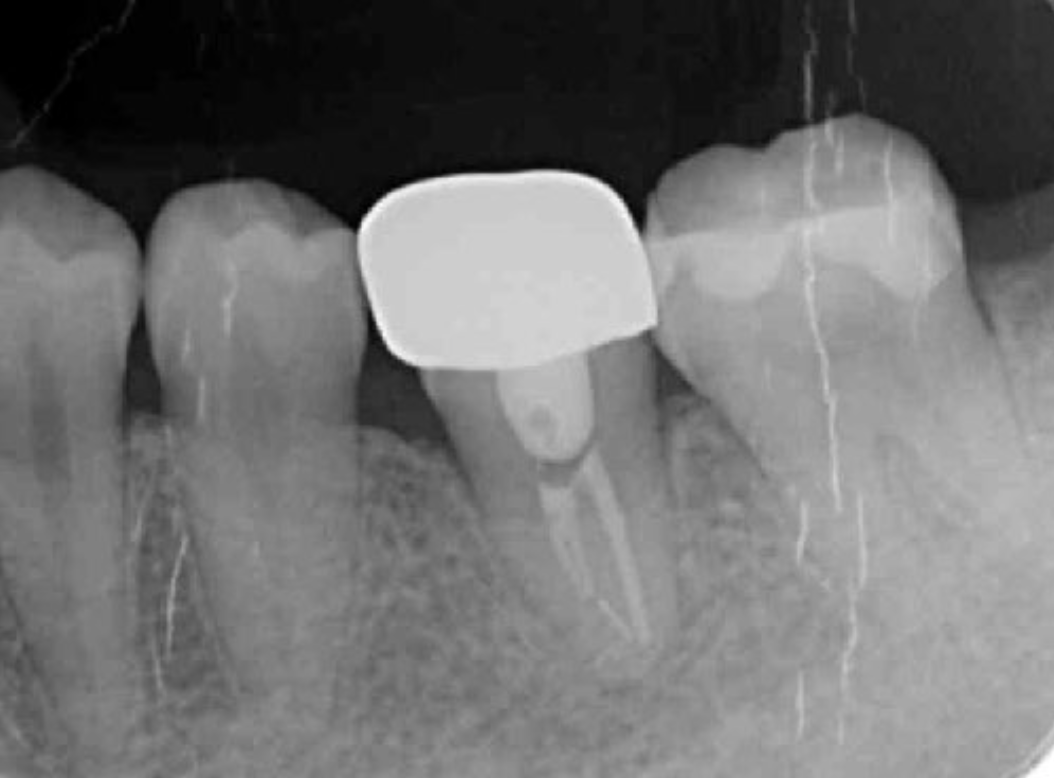
Following the operation, root canal treatment was performed as noted above. Functions including temporary crown occlusal contact and tooth mobility, as well as pocket depth were also checked. All examination results clearly indicated placement of a definitive prosthesis in the patient (Figure 13, Figure 14). At a follow-up examination one year after surgery, progress in this case was determined to be good (Figure 15).
Figure 13. Dental X-ray image obtained after confirmation of definitive prosthesis. Bone regeneration can be seen around the root of the donor tooth. 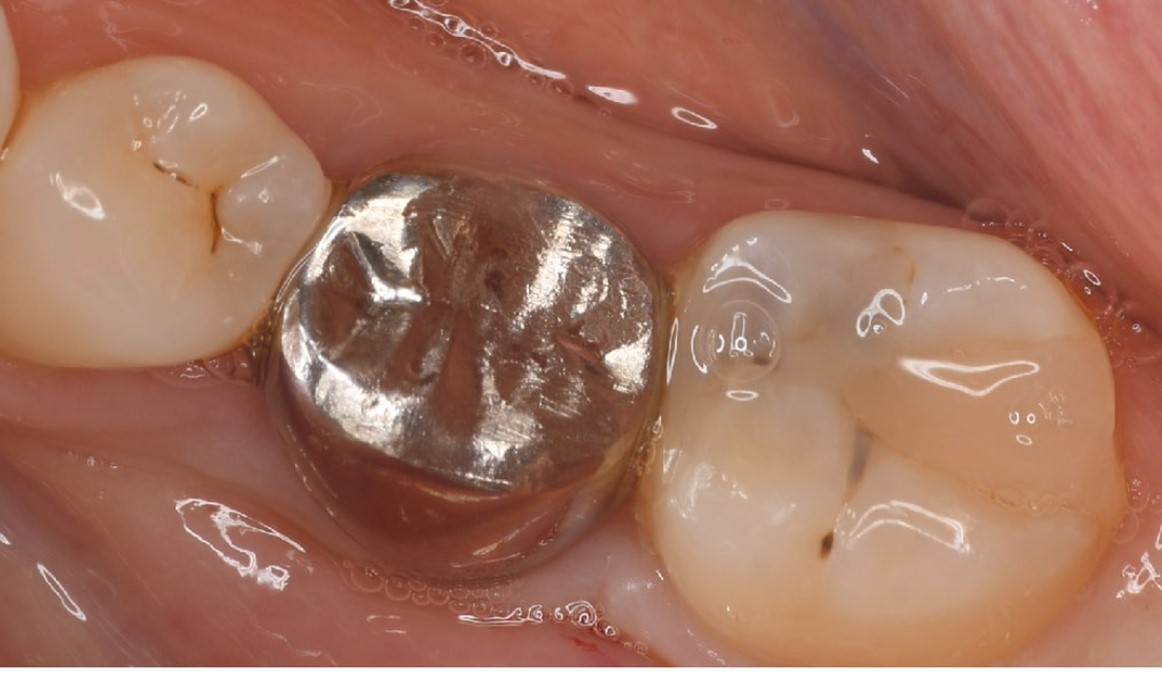
Figure 14. Intraoral photo after placement of definitive prosthesis. 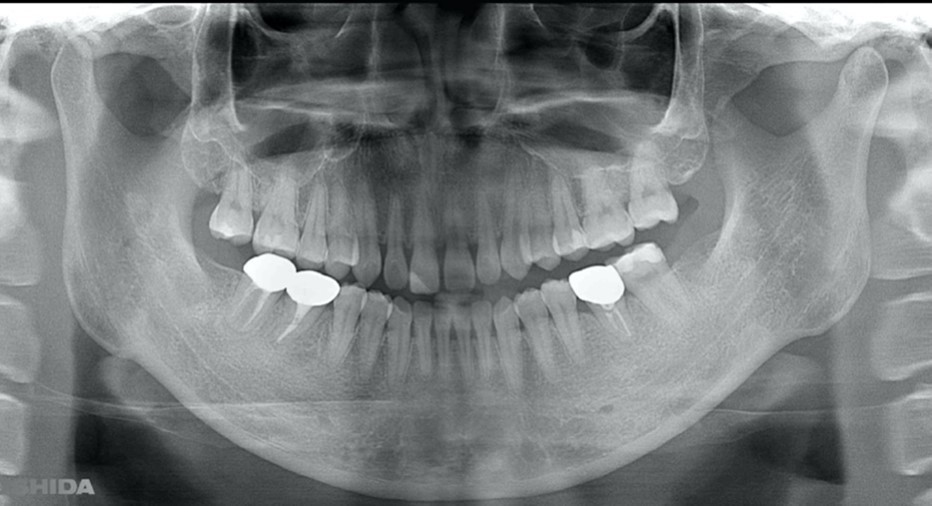
Figure 15. Panorama X ray image obtained one year after procedure for #36. The transplanted teeth demonstrated good function.
The patient actively visited the clinic for maintenance and showed good compliance. Achievement of occlusal recovery using auto transplantation for prosthetic treatment of the missing right and left mandibular first molars fulfilled her wishes, and created a significant improvement in functionality, thus leading to improved quality of life.
Discussion
Teeth are often lost because of complications related to caries. The first permanent molars are most often affected because of early eruption and the complex anatomy of the occlusal surface, though should be restored as soon as possible because they are key to normal occlusion 19. Notably, mandibular first permanent molars are the earliest permanent teeth to erupt and remain in the mouth for a long period, thus the risk of caries and root fracture is high, and they have a high possibility of early loss.
Tooth loss is an oral condition that leads to functional, aesthetic, and social damage, thus has an impact on quality of life 20. Specifically, inclination of adjacent teeth, protrusion of opposing teeth, and decompression of the occlusal plane occur as a result.
Mandibular first molars also serve as a primary functional masticatory site and play an important role as the point where biting force is applied. When missing, functional deterioration is inevitable, with prosthetic treatment always necessary. The presence of non-functional teeth such as wisdom teeth at that time is an indication for auto transplantation, a medical treatment procedure used for replacement of missing teeth that should be considered. As for predictability as well as economic factors, it is worth considering the possibility of grafting as an option before use of a bridge, partial denture, or implant. In the present case, the patient expressed a desire to chew with her own teeth. However, the cost of dental implant treatment was prohibitive and she refused cutting of adjacent teeth for making a bridge type prosthesis. Accordingly, auto transplantation using the non-functional #38 and #48 teeth was considered to be the best treatment option.
Yoshino et al. reported risk factors related to auto transplantation, including maxillary recipient site, periodontitis of a previous tooth, patient age over 40, Eichner classification B1 to C 21 occlusal type, number of remaining teeth less than 25, and skill of the attending surgeon 22, 23. As for those factors, the present patient was 27 years old, the recipient site was a mandibular tooth, the previous tooth was extracted because of root fracture, the number of remaining teeth was 28, and occlusal type was Eichner classification A 21. Therefore, we considered that the risk of losing the donor tooth after the operation was low. In addition, Ong et al. reported the following seven criteria for successful transplantation 11. (a) The patient must be healthy, (b) the donor tooth should have a simple morphology that can be adapted to the graft socket without worsening the occlusion, (c) the root apex must be open more than 1 mm and the root must be 1/2~3/4 grown, (d) patronizing extraction will not destroy the morphology of Hertwig's epithelial sheath, periodontal ligament, or root apex in the growing tooth embryo, (e) the shortest possible time for the donor tooth present outside the oral cavity is vital, within 1 minute if achievable, (f) prepare the donor tooth to fit into the implantation socket using a 3D method when possible, and (g) good oral hygiene must be maintained throughout the oral cavity to avoid post-transplant trauma. Of these, five, excluding (c) and (f), were attained in the present case. Based on these factors, auto-transplantation was thought to be the best alternative.
Implant therapy has become widespread in the field of dentistry, with significant developments obtained over the past several decades, including a large number of related studies published. Jung and coworkers reported that 97.2% of implants supporting single crowns had survived after five years and 95.2% after 10 years. Although survival rate is very high, peri-implantitis has become a primary complication in cases undergoing dental implant therapy. As a result, several dentists and researchers have endeavored to provide methods for prevention of and treatment for peri-implantitis, though consensus regarding proper management has not been established. In other words, the longer an implant remains in the mouth, the greater the risk of peri-implantitis 13. Thus, a delay prior to implant placement in the missing site for as long as possible is necessary.
Auto transplantation has come to be considered a better treatment choice as compared to implant treatment in consideration of gingivitis around the prosthesis 3. Related procedures include extraction of the tooth at the recipient site, preparation of the recipient socket as needed, atraumatic extraction of the donor tooth, minimal extra-oral time, positioning and splinting of the donor tooth, and occlusal adjustment 8, 24. In cases with a mature transplanted tooth, root canal treatment is performed extra-orally or at least two weeks after tooth repositioning 8.
In immature teeth with open apices, revascularization is predictable 8, 25, 26, 27. Successful transplantation depends on use in appropriate situations 5, 9 and patient selection 2, 3, 6, 10, 11. When correct surgical procedures are performed, the survival rate of teeth used for autotransplantation is fairly high 13, 24, while poor oral hygiene, acute infection, or chronic inflammation at the recipient site can lead to delayed healing, with persistent inflammation possibly resulting in transplant failure 10, 28. Furthermore, activity of the remaining periodontal ligament cells in the root of the donor tooth, and shape and location of the graft bed, as well as vascularity of the graft socket are also important points in this regard 6, 29. The success of tooth transplantation depends on the vitality of the periodontal ligament attached to the donor tooth 2, 30, which has been found to decrease with extraoral exposure 12, 19, 31.
The transplantation process begins with a surgical procedure according to the following requirements; the recipient site should be prepared according to the donor tooth shape, time needed for recipient site preparation should be minimized, the number of fitting attempts using the donor tooth should be as few as possible, and extraction of the donor tooth should be gently performed. For realization of an ideal surgical setting, panoramic X-ray and CBCT results (Fig. 1-9) are essential for preoperative diagnosis. In the present case, root completeness, Moorrees classification 18, and donor tooth size were determined based on those results, which allowed us to form an operation plan. Regarding root morphology, a single rather than a compound root is ideal and a single-root tooth that tapers toward the root apex is best, as the risk of damage to the periodontal ligament during extraction is reduced.
A postoperative radiography examination and pulp sensitivity test were performed 24, though pulp healing was not noted 25, 32, 33, partly because the root development status of the tooth was stage 7 according to the Moorrees classification. Since root resorption occurs within 14 days after surgery when the need for blood revascularization is not expected 34, 35, root canal therapy was performed two weeks later 8, 16.
Before the operation, the morphology and direction of the root canal should be simulated so that proper instruments can be easily accessed when performing endodontic treatment on a completed root. In the present case, the root morphology of both donor teeth (#38, #48) was single and bullet type, thus they were thought to most suitable for use as donor teeth.
Watanabe et al. reported that the success of auto transplantation of a tooth with complete root formation is affected by the quality of the root filling 36. Consideration of the difficulty of root canal treatment after auto transplantation .can improve the success rate of root canal fillings, thus we chose to use single-root donor teeth and Ni-Ti files (Pro Taper Next, Dentsply Sirona, Tokyo, Japan) in this clinical case.
As for whether to extract or save a wisdom tooth, there are cases in which the surrounding teeth do not cause any problems. There may be teeth remaining in the mouth that are questionable to save and can be used as donors for transplantation in the future. When there are congenital tooth defects in the mouth, it may be a good idea to inform the patient of the advantages of preserving the wisdom teeth for potential future autotransplantation.
Limitations of the present technique and alter native treatment options should also be discussed. It is hoped that through greater awareness and recognition by dental professionals, autotransplantation will become another viable treatment option for management of compromised teeth in patients with significant remaining growth potential 37.
Conclusion
The three main traditional prosthetic treatments for missing teeth include use of bridges, partial dentures, and implants, with various issues related to each. For the present patient, we performed bilateral auto transplantation for the first molar and consider that other similar cases are also suitable for auto transplantation. With reference to previous reports and studies for meticulous case selection, autotransplantation may be the best treatment option, even for patients with bilateral missing molars.
The purpose of this case report is to show that auto transplantation is a superior treatment method for single molar defects as compared to other prosthetic methods, because the periodontal ligament in the patient is used and cutting adjacent teeth can be avoided. In addition, it is a treatment method that can effectively utilize a wisdom tooth.