Nurses Working with Unlicensed Assistive Personnel: A Phenomenological Study
Abstract
Objective.
To describe the attitudes and behavior of registered nurses in their professional interaction toward unlicensed assistive personnel (UAPs) and to identify areas to develop policy for an effective nursing development and workforce planning.
Background:
One of the challenges health care systems have been addressing is the integration of the UAPs into the nursing care delivery systems.
Study Design:
Aphenomenological study involving registered nurses, staff and managerial positions. Data were collected using an in-depth semi-structured interview.
Findings:
Nurses report an increased task management workload which may lead to a decline in the quality of nursing care. Structural factors that are related to nurses and to UAPs were mentioned as affecting the quality of their professional and collaborative interaction.
Conclusions:
Training nurses to work with UAPs while developing their communication and managerial skills may improve the quality of care and increase their level of satisfaction.
Author Contributions
Academic Editor: Neslihan Lok, Selcuk University faculty of Health Sciences.
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2017 Ronit Calderon-Margalit, et al.
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Introduction
In recent years, the services of unlicensed assistant personnel (UAPs) were introduced into nursing teams in hospitals for the provision of direct nursing care. This development was in response to increasing hospitalization costs and the global nursing shortage combined with patients' expectations of receiving immediate, high-level nursing care 1, 2.
The introduction of UAPs to nursing teams leads to a structural and conceptual change in the nurses’ workload. When delegating some of the nursing duties to UAP, nurses who are educated and trained to be the sole providers of direct nursing care, are required to use other skills in their work including task delegation, supervision and evaluation of the work of their subordinate UAPs.
Global Overview
Most Western countries (Canada, USA, Great Britain and others) have introduced UAPs into their nursing teams. UAPs may appear under various names, such as unlicensed nursing personnel, patient care assistants and patient care aides. There are a variety of work settings in which this role can be found besides hospitals, and there is no uniformity in the scope of practice 1.
Despite the efforts of organizations such as the American Nursing Association (ANA) and the National Council of State Boards of Nursing (NCSBN) to regulate and define the scope of practice of UAPs, there is still ambiguity regarding the responsibilities and accountability of and within the nurse/UAP team in the provision of professional, safe and quality care 1.
Delegation
The nursing literature often uses the terms "delegation" and "delegated authority" to define the professional interaction between a registered nurse and a UAP. By definition, delegation is the act of transferring the authority to perform a selected nursing task to a competent individual, while a registered nurse takes responsibility and accountability for this care 1.
Delegation is now an entry-level nursing practice skill requirement. Still, novice nurses report a lack of knowledge, skills, and attitudes for the delegation decision-making process. Learning delegation skills “on the go” is a common pattern. The literature reports that there is a gap between the expected skill levels and the actual abilities of new graduate nurses relative to delegation 3, 4.
Delegation is a complex managerial skill that strongly affects all parties involved, i.e., the nurses, UAPs and patients 1. To provide quality and safe nursing care for their patients, nurses have to delegate the right task to the right person under the right circumstances with the right direction/communication and appropriate supervision.
The concept of delegation between nurses and UAPs, and the relationship between nurses and UAPs in clinical practice was not broadly studied since the new joint statements issued by the ANA and the NCSBN. Few studies were found in the literature regarding nursing delegation and the relationship between nurses and UAPs. Only few qualitative studies were found on this topic, of which, only one was qualitative in nature 5.
Studies have found that nurses report a lack of knowledge on how to properly delegate activities to UAPs and an insufficient knowledge regarding the UAPs training. Although still responsible for the comprehensive patient care, many nurses expressed frustration with multiple additional responsibilities unrelated to direct bedside care, even if they were assisted during the work by an UAP 6.
Despite the fact that UAPs participate in basic nurses' tasks, nurses have reported disappointment with the lack of time needed for highly professional nursing activities. However, nurses who reported to have good delegation skills were more satisfied with their work, and even reported of having more time to provide professional nursing activities 14.
Poor nursing managerial skills and poor delegation capabilities are reported to be the main cause of negative results or poor relationships between nurses and UAPs 7, 8, 9. Moreover, researchers 5 have found that nurses who reported of being more prepared to use delegation and supervisory skills also conveyed that positive experiences appeared more frequently. However, in the absence of regular direct supervision, more missed care events were reported.
The situation of delegation of tasks from nurses to UAPs is fairly new in Israel. Most Israeli nurses have not had any formal preparation on delegation principles either in nursing school or by specific on-the-job training programs.
Prior to the introduction of the Ministry of Health policy for nurses working with UAPs, the majority of nurses have reported favorable opinions on this issue. However, after the publication of the guidelines, nurses have reported that they expected difficulties both in guiding and in supervising the UAPs' work, as well as in their ability to execute their professional nursing duties 10 respective to other studies 5.
Based on the current international and national research, a better understanding of the collaborative relationship between nurses and UAPs, and what does this mean for nurses in clinical practice is needed. Since the knowledge on this issue is rare, the empirical qualitative approach is a better way to examine and comprehend in-depth the broad meaning of this concept from the nurses’ perspective.
The aim of this study is to describe, recognize and learn aspects regarding the working relationship between nurses and UAPs. This study seeks to explore the following research questions:
Research Questions:
1. What are the nurses' perceptions on working with UAPs?
2. What influence UAPs have on: (A) Quality of nursing care delivered and (B)Working relationships?
3. What are the factors affecting the quality of professional interaction between nurses and UAPs?
Study Design:
Setting:
We used the phenomenological method to describe, identify and learn aspects associated with the working environment of nurses and UAPs. Using the phenomenological methodology, the meaning and significance of the nurses’ experiences when working with UAPs were investigated in detail, since this method is designed to explore personal experience and is concerned with an individual’s personal perception. In-depth interviews with nurses were conducted in two large general hospitals in Jerusalem.
Sampling:
We used a wide purposive sample, representing a wide range of the nurse’s professional roles from different levels of education and responsibility. This sample was designed to provide rich, relevant and diverse data pertinent to the research questions. The study population included six nurses: four nurses at different managerial levels and two staff nurses from the internal medicine, surgical and orthopedic surgery departments. Sociodemographic characteristics are detailed in Table 1.
Table 1. Sociodemographic characteristics| 1 | 2 | 3 | 4 | 5 | 6 | |
| position | supervise nurse | supervise nurse | unit nurse manager | unit nurse manager | staff nurse | staff nurse |
| gender | female | female | female | female | female | female |
| age | 65 | 57 | 38 | 45 | 40 | 28 |
| education | RN MPH | RN-MPH | RN-MPH | RN-BSN | RN-BSN | RN |
| Nursing ex-perience | 45 years | 30 years | 15 years | 20 years | 18 years | 5 years |
Inclusion criteria included nurses who were working regularly with UAPs. Data saturation was achieved based on this sample size. No new issues were raised after the last interview.
Data Collection
Data collection was based on individual interviews in order to ensure conceptual objectivity, enabling an open environment for new ideas without an influence of one nurse to one another. All interviews were conducted by one nurse researcher (IO). Each interview lasted between 60-90 minutes. In-depth and semi-structured interviews were used. The semi-structured questionnaire included the following questions: (1) what do you think about working with UAPs in providing direct nursing care to the patients? Describe your feelings and emotions when working with them; (2) how does the process of working together usually work? (3) Do you think that working with UAPs has changed the nursing work routine? If so, describe how.
Follow-up questions were asked to clarify thoughts, feelings and meanings of what was expressed in order to gain a deeper understanding of their answers. Reflective questions were asked while suggestive questions were avoided. The interviews were audio-reordered for transcription and analysis. Data collection took place in July-August 2014, and continued until saturation occurred (no new themes emerged)..
Validity and Reliability
Rigor was reached by attending to credibility, confirmability and transferability. Credibility and confirmability were enhanced by keeping comprehensive field notes during the data collection and analysis stages, by audio-taping the interviews and transcribing them verbatim, and by implying the investigators’ triangulation where investigators collaborated on analytical decisions. Reflexivity while encoding and re-encoding was made during the data analysis by repeated discussions including all investigators. Transferability of results was enhanced by the heterogeneity of cases in the study, which represent the diversity of staff nurses and nurse managers from both hospitals. Changes in the structure of the study questions were made since findings that accrued during data collection showed some irrelevant issues or issues requiring more intense exploration.
Data Analysis
Data analysis was done according to the Shkedy’s content analysis methodology11. With this method, data repeatedly gathered and learned from the field (interviews with informants), was broken into pieces to remove the data from the chronological context of the interviews. Then segments of data that seemed to pertain to the same phenomena were grouped together to create a preliminary categorization. Repeated processes of narrative analysis, including or excluding items in the categories and discussions between the researchers based on understanding the context of the findings and existing theoretical basis, results in finding relationships and connections in the categories and between them were carried out. Finally, data was organized into main
categories and subcategories in the category "tree": the main categories were organized by horizontal axes (relationship between main categories) and vertical axes (relationship within the categories and subcategories). With this methodology, categorization exposed, provided meaning and led to the construction of a picture that offers an answer for the research question.
The process of coding was manual without the use of software programs. Units of meaning with common ground were organized into preliminary categories and were labeled. Further processing of the data entailed reconstruction of the categories by including and excluding the units of meaning in order to build a main category and sub-categories, as the analytical search for relationships between the categories progressed. Finally, this process revealed from the narrative analysis into a schema of relationships between main categories and subcategories (see Figure 1).
Figure 1.Nurses working with UAP. Themes related to the process.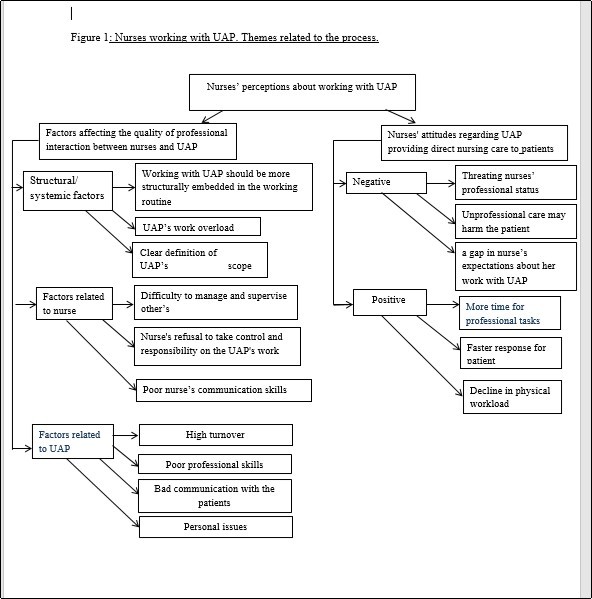
The topics emerging from the nurses’ interviews were organized into two main themes: "nurses’ attitudes while working with UAPs" (sub-themes - "positive" and ‘’negative’’) and "factors affecting the success of the process" (sub-themes - "structural / systemic issues," "factors related to nurse," and "factors related to UAP")
Ethics
The study was approved by the Hadassah Medical Center Ethics committee. Participation in the study was voluntary. Participants were recruited through a brief phone call in which the study, its purposes and its methodology were introduced. Confidentiality was promised. There were no refusals to participate, nor any objections for recording the interviews.
Findings
1. Nurses' Attitudes Regarding Uaps Providing Direct Nursing Care to Patients Under the Nurses' Supervision:
All interviewees saw both positive and negative sides on working with UAPs. On the negative side, they raised concerns related to the decrease in their professional status of nursing since UAPs perform ”tasks that a nurse is supposed to do,”(P6) and the decrease of quality of nursing care provided by unskilled, non-professional staff.
On the positive side, first and foremost, all interviewees indicated a decline in the physical workload imposed on nurses. The expression "another pair of hands" was repeated in almost every interview (P3-6). Even among interviewees that expressed general discomfort with the process of working with UAPs, the overall feeling was that now, when the RN is required to do less physical work, “they are allowed more time to perform more professional tasks."(P5)
The "price" nurses need to pay for this process is to devote more time to managerial and supervisory activities. Many of the nurses felt that these activities took them away from the core of nursing – providing direct nursing care to patients--which deepened the distance between them and the patients:
Some nurses talked about the importance of supervision and monitoring of the UAPs’ work and perceived it as a managerial role: “Every nurse should be a manager ... not only the manager of patient’s treatment; she also has to manage the people she works with."(P4) However, none of the nurses felt that this role was empowering. Some nurses even saw it as a burden, not something that is really part of the process that would promote them in a professional or social aspect: "I feel like, unfortunately, a babysitter"(P5), "I feel like I constantly have to check things - was it done and was it done properly? It takes a lot of my energy."(P6)
A remarkable issue nurses noted as a result of this process is that patients received faster responses to their basic needs. Many mentioned that the response of the UAPs was not necessarily conducted on as a high professional level as it would have been had it been conducted by a nurse.
2. Nurses’ Perception of The Impact Uaps Have on Nursing Care Delivered:
Quality of Nursing Care
Following the incorporation of UAPs in providing direct nursing care to patients, the patterns of providing nursing care have changed. When the working process of nurses and UAPs is clearly defined for both sides, nurses felt that the quality of nursing care is better due to a more rapid response to the patients' needs. Some nurses described the process as "…effective and helpful for the nursing staff and patients".(P1)s
In some cases, nurses reported that the quality of care declined. In their view, the patient expects to see the nurse as the primary caregiver rather than the care provided by nonprofessionals. "This is actually their the patients’ expectation - a nurse should be present, not the UAP. I think they patients feel the quality of care decreases."(P2)
Working Relationships
Nurses noted a significant change in their work processes when they started to work intensely with UAPs. The issue of team work between nurses and UAPs requires "a change in the nurse’s work planning, a change in work habits….these processes are a long term situation, and achieving goals can be made in very small steps."(P3) However, mixed reports were received from the nurses.
One staff nurse working in a department wherein the process of interacting with UAPs is structurally embedded into the nursing workload, said that all of the caretakers were well aware of the routine of working with UAPs. "I build a care program for the patient in advance and explain to the UAP what to do."(P6)
In contrast to this conception, another nurse, working in a department with less structured working processes of nurses and UAPs, expressed a different sentiment:
"Nurses need to remind them UAPs to perform specific nursing care activities, to monitor and supervise their work..... I can't control them all the time!" "I still expect them to have the responsibility to do some of the tasks alone.”(P5)
This problem may occur mainly when there is a gap in expectations between the nurses and UAPs. In contrast to a nurse’s’ work with a physician and other health care professionals in a multidisciplinary health care team, the work with the UAP is completely different. The UAP position, by its definition, is a nonprofessional role and only works under the guidance and supervision of a nurse. The nurses often are not prepared and do not get proper preparation for this kind of working relationship; as a result, they do not fully understand the essential difference: "Working with a n UAP is like working with any other health caretaker; the nurses did not receive any training to work with all of them, so we are not trained to work with UAPs".(P5)
The relationship between nurses and UAPs can be described as ‘’respect and suspect." On the one hand, nurses appreciate the UAPs’ hard work, mainly through their assistance to cope with multiple tasks embedded into the nursing activities. On the other hand, UAPs are expected to take more initiative and to participate in the nursing work routine, so that nurses are able to rely on them in their daily practice. "UAPs will always try to avoid performing little things. I have a great appreciation for UAPs and at the same time, I often have deep concerns."(P4)
3. Factors Affecting the Quality of Professional Interaction between Nurses and Uaps:
Structural/ Systemic Factors Associated with:
Lack of Proper Training for UAPs:
"People that come to work don't know this kind of work… we need to teach them everything: bathing the patient, even how to speak with the patient."(P4)
Unclear UAP role definitions, and permitted performance tasks:
Some nurses noted that there are nurses who are "very comfortable to give instructions"(P3) and "stretch" the limits of authorized UAP tasks: "Some nurses ask UAPs to perform tasks that they are not allowed to do. This serves both the nurses and UAPs who want to feel like professionals”(P6). This lack of role clarity has been mentioned by the nurses as a major factor that could affect patients' safety: "Overall, adverse events and missed care are associated with the UAP’s scope of practice, when they are not properly directed and do things they are not allowed to do"(P2)
High Turnover Among UAPs:
UAPs’ turnover is described by the nurses as a very challenging issue. We must “re-teach the work all the time, re-test issues of trust, and observe level of skills and work quality"(P6).
Factors Related to Nurses:
Difficulties that nurses experience in providing guidance and ensuring constant supervision.
There are nurses who thought that guidance and supervision are not part of their job: "I don’t think I should supervise her/him (UAP). Maybe the nurse manager should do it."(P5) Some felt uncomfortable when controlling the work of others and discomfort from the constant need to guide and supervise: "I'm not comfortable with the fact that I have to remind a person twice my age and tell her what to do and how to do it. Sometimes I need to remind such a person more than once to complete a task ..."(P6)
Poor Nurses’ Communication Skills:
"Sometimes nurses do not talk nicely to UAPs. Some nurses take the position of guidance and supervision to the extreme, and allow themselves to criticize the UAPs’ work in an unpleasant way"(P1)
Factors Related to Non-Professional Personnel:
Since UAPs are mostly employed by Human Resources agencies, nurses cannot control who they are working with: "Now we have good staff here, but sometimes people come who don't know how to work and don't actually want to work. And I'm expected to deal with it and to provide good patient care".(P4)
Discussion
In recent years, the integration of unlicensed assistive personnel (UAPs) as part of the nursing teams in providing direct nursing care to patients has increased throughout hospitals. Non-professional personnel address the complex reality wherein patients’ demands and nurses’ workload is increasing, along with higher nursing professional levels of responsibility. In this new reality, nurses are tasked with an even wider range of responsibilities other than their nursing skills, such as managerial skills in working with UAPs to achieve effective and safe working situations.
Nurses in this study have indicated that the initial nursing role of taking care of patients has changed. The use of more UAPs into hospitals has changed the heath care environment; thus, nurses are required to spend less time with direct care, at the expense of allocating more time to guidance and supervision of UAPs. These findings are similar to those of other studies indicating that the main changes in the nurses’ work responsibilities are associated with the need to use more managerial skills 13, 14. The current study findings support the suggestion that when the roles of the nurse and the UAPs are more clearly defined so that nurses understand the need to delegate and manage the work of others, they report a higher satisfaction level resulting in patients receiving better quality of care 7, 14.
The nurses' perception of their role and responsibility while working with UAPs is not consistent among all the nurses in the study. Although the interviewees indicated a decline in the physical workload imposed on nurses, they mentioned an increase in managerial duties such as the need to supervise other's work. As one of the nurse managers in this study mentioned, “A nurse apparently is a human resources manager. She needs to allocate tasks, supervise and give feedback… It is not only the head nurse’s role, but when working with UAPs the staff nurse needs to have these skills as well".
These findings are in agreement with those of others 15 indicating a lack of uniformity among nurses about understanding the delegation process and their responsibilities when working with UAPs;moreover, we also concur on the nurses’ dissatisfaction and feeling of despair due to the need to supervise other's work and be responsible for the outcomes.
Kelly (2011) includes a lack of sense of authority and low personal confidence in delegating instructions as major barriers to effective delegation. However, according to our interviewees the barriers are: lack of proper training for UAPs and their inappropriate workload, unclear UAP role definitions, difficulties of nurses in providing guidance and ensuring constant supervision, and poor communication between nurses and UAPs. On the other hand, similarly to other findings 15, 2, guidance, control and supervision of the work of UAPs are mentioned as factors necessary for the process. These are also other factors that would lead nurses to be more satisfied when working with UAPs, thus allowing them to devote more time to more complex professional activities 5, 8.
Nurses mentioned the importance of proper communication skills while working with UAPs. This issue appears in almost every study that discusses the work of nurses with UAPs. It has been also linked to the level of nurses’ satisfaction working with UAPs 13, 9. Miscommunication between the two roles contributes to a poor quality of nursing care 7, 16.
According to the findings of other studies 14, 16, an important part of working with UAPs is training. Training programs allow for the establishment of necessary communication and management skills, and the provision of practical tools that are necessary for an effective interaction. Although, nurses in this study (staff and managers) indicated that they did not receive specific training for effective communication, management and delegation skills, they were not fully aware of the need for special training on these issues. As seen in previous studies 14, 16, providing management tools for the nursing team may significantly improve the quality of the nurses’ professional interactions with UAPs and the quality of nursing care.
Study Limitations
This study was performed with a relatively small number of participants. Although we used the purposive sampling to allow for the representation of heterogeneous cases, ultimately, there is also a possibility that different opinions and attitudes exist that were not represented in this study.
This study focuses on RNs’ attitudes of interaction with UAPs. Further investigation of UAPs' feelings and attitudes; and patients’ points of view could contribute to a better understanding of this issue.
Suggestions for Future Research
Since this study was based on the nurses’ perspective, future research is needed to examine the nurse-UAP relationship from the perspective of the UAPs.
Future research is needed to assess the nursing communication and management skills of both novice and experienced nurses.
There is a need to assess nursing outcomes as a result of the communication and the relationship level of the nurses and UAPs (such as: patient satisfaction, quality of care)
Future nursing interventions to improve relationships between nurses and UAPS is needed, accompanied with measures to evaluate the process.
There is a need to assess nursing educational programs of delegation skills on the communication of nurses and UAPs, and on the actual delegation practice in clinical settings.
Implication to Nursing Practice
The perception of the nursing role and nurses' responsibility while working with UAPs is not consistent among all nurses. In order to improve the quality of care given to patients and increase nurses' satisfaction, there is a need to: 1) strengthen the key role of the nurse in the patient care delivery pattern while working with UAPs 2) emphasize nurses' delegation skills 3) reinforce communication skills between nurses and UAPs and 4) designate specific management activities for maintaining the skills of the nurse-UAP team.
References
- 1.. , American Nurses Association & National Council of State Boards of Nursing. Jointstatementondelegation,(2006),https://www.ncsbn.org/Joint_statement.pdf
- 2.The Ministry of Health, Nursing division, Directory No.64(2011)Guidelines for working with UAP. http://www.health.gov.il/hozer/ND89_11.pdf
- 3.Conger M. (1999) Evaluation of an educational strategy for teaching delegation decision making to nursing students. , Journal of Nursing Education 38(9), 419-422.
- 4.Antony M, StandingT. (2008) Delegation: What It Means to Acute Care Nurses. , Applied Nursing Research 21, 8-14.
- 5.White M, Gutierrez A, Davis K, Olson R, McLaughlin C. (2011) Delegation knowledge and practice among rehabilitation nurses. , Rehabilitation Nurse 36, 16-18.
- 6.Kalisch B. (2006) Missed nursing care: a qualitative study. , Journal of Nursing Care Quality 21(4), 306-313.
- 7.Keeney S, Hasson F, McKenna H. (2005) Nurses’, midwieves’ and patient’ perceptions of trained health care assistants. , Journal of Advanced Nursing 50(4), 345-355.
- 8.Rubin G, Rengaran V, Barcikowwsky R. (2009) Barriers to nurse/nursing aide communication: the search for collegiality in a southeast Ohio nursing home. , Journal of Nursing Management 17, 822-832.
- 9.Albagli Haaron, Riva. (2008) Survey on nurses ‘perceptions about working with UAP.http://www.health.gov.il/UnitsOffice/nursing/research/Documents/Research_Abstracts_2010-2014.pdf.
- 10.Shkedi A. (2003) Words which try to Touch: Qualitative Research-Theory and Practice,2nded,Tel-Aviv.
- 11.Kelly P. (2011) Delegation of patient care:. , Essentials of Nursing Leadership & Management,3rded,Cengage Learning
- 12.McLaughlin F, Barter M, Thomas S, Rix G, Coulter M et al. (2000) Comparison of registered nurses in the United Kingdom and the United States:Perceptions of the registered nurse role when working with nursing care assistants/unlicensed assistive personnel. , International Journal of Nursing Practice 6, 46-57.
