Food Intake Pattern of Obese Older Patients with Successful Weight Loss and Weight Maintenance on the Basis of Food Energy Density
Abstract
Objective:
Detailed reports in changes of eating habits especially in elderly subjects with successful weight loss and maintenance are virtually unknown. In this paper we have analyzed the eating habits of 104 obese patients (BMI 37.8±0.3 kg/m2, age range 65 and 84 years) who lost 11.5±0.3kg over an average follow-up period of 37.5±0.5 months.
Design:
Patients recorded food intake over a period of 12 days before and 12 days after changes of eating habits. Dietary counseling was based on food energy density (ED) with the aim to maintain food quantity as much as possible for adequate satiety in conjunction with a reduction of energy intake. Individual eating habits should be preserved as much as possible.
Results:
Average daily energy intake of solid food was reduced by 267kcal, food intake by 114g and ED by 0.10 kcal/g, respectively. Liquid calories were reduced by 79 kcal/d. Lower daily energy intake was the result of a reduction of medium and high ED food items compensated for by a greater intake of low ED food items. Changes of macronutrients comprised substantially lower carbohydrate and fat intake with minimal reduction of protein. From 28 different food groups 9 were reduced significantly (bread, butter, marmalade, cheese, meat products, fast food, fruit and chocolate) while 3 were increased (eggs, curds, ham). The relative contributions of the various food groups to daily energy intake remained fairly similar indicating that individual preferences were largely maintained.
Conclusion:
The data demonstrates that in elderly subjects with severe obesity an individual change of eating habits can lead to successful long-term weight loss with improvement of carbohydrate metabolism. This will contribute to increased mobility and to improved quality of life. This method which is based on the energy density of food items is a simple measure to reduce energy intake while ensuring long-term adherence.
Author Contributions
Academic Editor: Ehimen Aneni, Baptist Health South Florida
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2015 Volker Schusdziarra, et al.
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Introduction
In most industrialized countries the prevalence of obesity in older persons has been rapidly increasing1, 2, 3, 4. This leads to increasing health care costs due to related co-morbidities (e.g. diabetes mellitus, osteoarthritis) and higher risk of disability5. The shifting balance between muscle mass and fat mass in older individuals, which is accompanied by a decline of muscle strength and muscle function predisposes them towards a deterioration of functionality6. This age-associated physiological phenomenon will be aggravated in those that are considered to be sarcopenic obese when obesity is combined with low muscle mass and low muscle strength7.
In recent years it has been shown that successful weight management which included dietetic advice and exercise could improve functionality in obese older persons 8, 9. However, long-term effects of these programs have not yet been documented.
At present weight-maintenance must still be considered to be a major obstacle, since most treatment modalities have shown rapid regain in younger adults, either during treatment or after its termination10, 11, 12, 13, 14 As weight cycling might induce a detrimental decrease of functionality in older persons weight maintenance has to be achieved in this population as otherwise the benefits of weight loss with regard to function will be offset15.
Various concepts of dietary intervention have been advocated such as reduction of fat (low fat) or carbohydrate (low-carb) intake16, 17. Furthermore, an increase of the protein/carbohydrate ratio in conjunction with either a low-fat or normal fat regime has shown favorable effects 18, 19. Several studies have demonstrated that any change of the macronutrient ratio leads to a similar weight reduction9, 10, 20, 21, 22. In addition, behavioral interactions have been shown to be important for successful weight loss23, 24.
In recent years, the important role of food energy density (ED) for acute energy intake has been recognized. ED refers to the amount of energy in a given mass of food (kcal/g) and depends primarily on fat and /or water content of food. ED reflects best the relationship between the satiating capacity of a food item and its contribution to energy intake 25, 26, 27, 28, 29, 30, 31. Moreover, it has been shown that ED is a good basis for weight reduction concepts. Several studies over a period of 6-12 months have shown a good weight reduction by supplementation of snacks with low ED (soup, vegetable, fruit or milk products)32, 33, 34.
We have recently shown that an individually tailored change of eating habits without any rigid dietary prescriptions concerning limitations of energy intake, macronutrient ratios or dietary fiber intake is associated with successful weight loss and its maintenance35.
In this context it is of interest to examine the change of eating habits of those subjects who successfully lost weight and who were able to maintain this weight loss over a prolonged period of time. For this purpose in the U.S. the National Weight Control Registry has been established which analyzes the eating habits of patients who were able to maintain their initial weight loss for at least another year 36, 37, 38, 39. In these patients however, the eating habits prior to treatment have not been recorded so that an intraindividual analysis is not possible and only post-treatment cross-sectional data are available.
In this paper we report the eating habits of 104 patients with an age ≥65 years before and after weight-loss and maintenance on the basis of food energy density.
Methods
The analysis used in this paper is based on the dietary records of 104 obese patients with an age of ≥ 65 years. Basic requirements for inclusion were weight loss and maintenance of at least 5% over a period of at least 12 months. The demographic characteristics of all patients are shown in Table 1. They have been in contact with the outpatient clinic of the department of nutritional medicine since January 2003 with the intention of losing weight. Excluded were mentally disabled subjects, those with body mass index ≤25 kg/m2 and those with type 1 diabetes mellitus. Patients could refer themselves or could be referred by their physician. The duration of treatment was principally unlimited and the treatment costs were covered by the German health insurance system. The recommended interval between counseling sessions was initially 4-5 weeks and depended thereafter on the clinical course of each patient.
Table 1. Baseline characteristics of all patients (mean ± SD)| All | Women | men | |
| Number | 104 | 69 | 35 |
| Age | 70.6±1.02 | 70.0±1.66 | 71.6±1.77* |
| BMI | 37.8±3.06 | 37.6±3.3 | 38.3±3.55 |
| kcal/day solid food | 1381±186.6 | 1371±187.7 | 1402±185.2 |
| kcal/day liquids | 207±88.7 | 201±83.1 | 220±93.5 |
| gram/day solid food | 1018±126.5 | 1023±126.3 | 1010±127.2 |
| ED kcal/gram | 1.40±0.4 | 1.37±0.17 | 1.45±0.45* |
| kcal/day total | 1517±198.9 | 1504±196.0 | 1654±205.9 |
| Patients with type 2 diabetes no (%) | 59 (56.7) | ||
| Medications no (%) | |||
| Antihypertensive therapy | 71 (68.3) | ||
| ß-blocker | 21 (20.2) | ||
| Lipid lowering therapy | 15 (14.4) | ||
| Oral antidiabetic therapy | 38 (36.5) | ||
| Insulin treatment | 21 (20.2) | ||
| Antipsychotic and anti depressant therapy | 6 (5.8) |
Dietary intervention
The aim of our treatment concept is to change eating habits towards hypocaloric nutrition in conjunction with adequate satiety whilst preserving of as many of the most favored dishes and food items as possible with the expectation of improving long-term adherence to an individually tailored food intake. Prior to the start of dietary counseling all patients had to complete a food diary over 12 consecutive days to get as much information as possible about the “old” eating habits. They were instructed to record in as detailed a manner as possible every item they either ate or drank, the time of consumption, the amount they ate by weighing with a scale as often as possible and how the food was prepared. To increase the motivation to accurately report their habitual food intake patients were told that an accurate recording of their usual intake would improve individually adapted changes of their personal eating habits during subsequent therapy. They were told that the most preferred food items of their usual diet would remain unchanged as much and as long as possible to prevent underreporting, particularly the underreporting of snacks with high ED.
The patients were informed that record keeping could produce a change in nutrient intake and they should not try to alter their usual eating habits since this could lead to less effective recommendations during subsequent dietary counseling. All patients were handed out a booklet with examples of characteristic portion sizes should they eat out.
During the first counseling session suggestions were made to substitute low ED for high ED food items. For support patients had a booklet with the ED of approximately 1500 food items divided into 37 food groups 40. Within each group, the items are listed in an ascending order of their ED. Low ED food (≤1.5 kcal/g) is marked green, medium ED (1.51-2.49 kcal/g) yellow, and high ED food (≥2.5 kcal/g) red.
Patients were told to eat a sufficient amount of low ED food to feel satiated. Medium and high ED food was thought to satisfy taste as well as sensory and cognitive cues. No dietary prescription was made for energy or macronutrient intake. Further recording of food was recommended to reinforce the learning process of becoming acquainted with the new eating habits. In addition patients were encouraged to increase their physical activity but without any specific recommendations concerning duration and intensity.
The treatment of the patients was in accordance with the declaration of Helsinky and the guidelines of the ethical committee of the Technical University of Munich.
Data analysis
Dietary protocols were calculated with the scientific program PRODI 5.5. Expert (Kluthe, Freiburg, Germany). Energy containing beverages were considered separately, so that the reported ED is based on weight and energy content of solid food only as reported recently in several detailed studies 41, 42, 43. Macronutrients are expressed in absolute values (g) and as percent of total solid food energy intake.
The data are expressed as mean ± standard deviation (SD), unless stated otherwise. For statistical analysis t-test for paired data (comparison within groups) was employed. Where appropriate, correction for multiple comparisons according to the procedure of Bonferroni was made. Values of p<0.05 were considered significant. All data were analyzed by using SPSS (version 17.5).
Results
104 elderly patients were evaluated with an age range between 65 and 84 years. Mean follow-up time of the patients was 37.5±8.2 months (min-max: 15-108 months). During this period the intitial weight decreased from 106.5±9.2 to 95.0±7.1 kg at follow-up (BMI: 37.8±3.1 to 33.8±2.0 kg/m2) (p<0.001). The average number of visits for dietary counseling was 14.3±8.2. In the 59 patients with type 2 diabetes mellitus HbA1c was reduced from 7.7±2.3 to 6.4±1.5 % (p<0.001).
The analysis of food intake was based on 1248 dietary records before start of treatment and 1248 protocols at the time of follow-up.
Food intake was reduced by 114 g from 1018±126.5 to 905±135.6g/day (p<0.0001). Energy intake by solid food was reduced from 1381±186.6 to 1114±163.2 kcal/day (p<0.0001). This reduction of 267 kcal was accompanied by a further reduction of 79 kcal in form of liquid calories (207±86.7 to 127±67.3 kcal/day, p<0.0001). The intake of total energy (solid and liquid) changed from 1517±198.9 to 1183±172.4 kcal/d (p<0.001). Energy density was reduced from 1.40±1.0 to 1.30±1.0 kcal/g (p<0.0001) and the number of meals from 3.8 to 3.5 meals per day (p<0.001), with significant reductions of breakfast, afternoon snack and dinner while morning snack and lunch frequency remained unchanged.
The changes of macronutrient intake are shown in table 2. The absolute intake decreased significantly for all three macronutrients. The relative change for carbohydrate was -25%, followed by fat intake (-22%) while protein changed only slightly with -6%.
Table 2. Changes of daily macronutrient intake in absolute values and as percent of daily energy intake (mean ± SD).| carbohydrate | fat | protein | ||||
| before | after | before | after | before | after | |
| g/day | 143±22.4 | 108±18.4* | 59±11.2 | 46±10.2* | 66±10.2 | 62±10.2* |
| % kcal | 42.4±5.1 | 39.6±4.1* | 38.3±5.1 | 27.8±5.1* | 19.7±3.1 | 23.1±3.1* |
The relative contribution to daily energy intake was reduced substantially for fat (-10.5%) and only little for carbohydrates (-2.8%) while the relative contribution of protein was raised by 3.4%. Daily fiber intake was reduced from 15.6±3.1 to 12.2±3.1 g/day (p<0.0001).
Figure 1 shows the contribution of food items with low, medium and high ED to daily food quantity and energy intake. At baseline almost 70% of the daily food intake came from low ED food, which was significantly increased while medium and high ED food intake showed a small but significant reduction. Energy intake by low ED food increased significantly by 10% after change of eating habits which was paralleled by a small reduction of medium ED food and an 8% reduction of high ED food items (Figure 1).
Figure 1.Contribution of food items with low, medium and high ED (kcal/g) to daily food quantity (% g) and energy intake (% kcal) before treatment (pre) and at follow-up (post). Mean ± SEM. *=significantly different from the pretreatment period, p<0.0001 or less.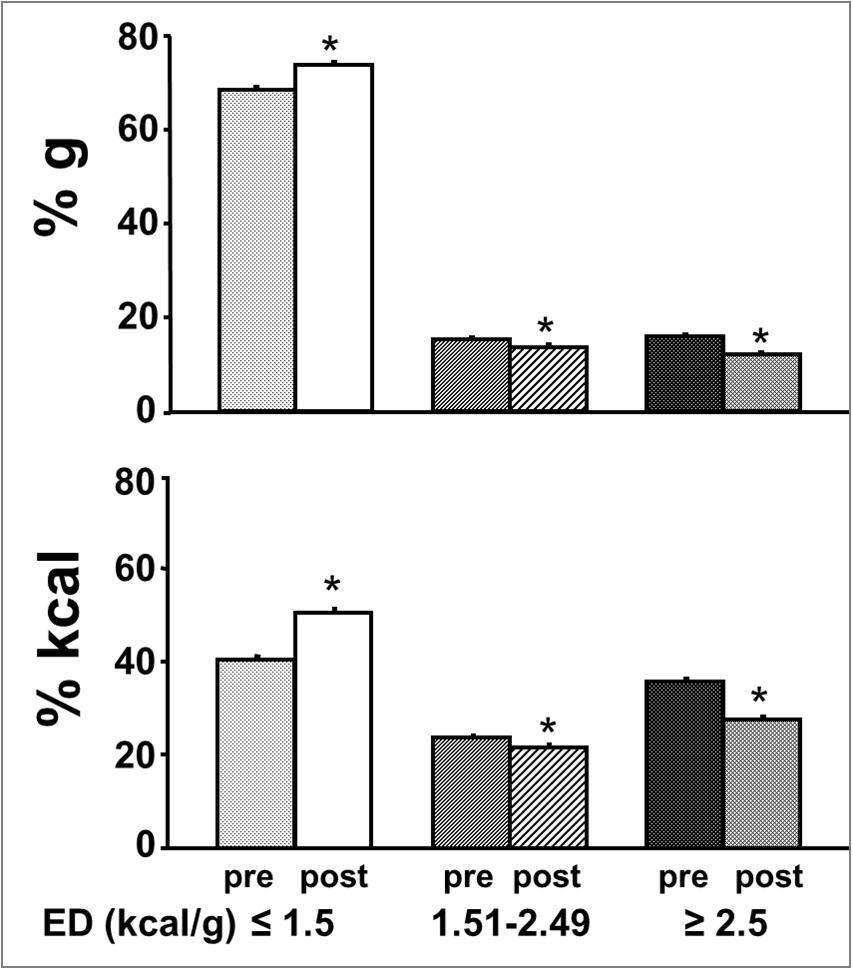
The preferential consumption of low ED food items decreases average daily ED as expected but it is not associated with hypocaloric nutrition as shown in Figure 2a. The increase of low ED food by almost 900g was associated with a significant reduction of ED from 1.92± 0.71 to 1.06±0.31 kcal/g (p<0.0001) and a significant increase of total daily food quantity by 670g (p<0.001) indicating a reduction of medium and high ED food by 209g. This however, does not lead to a reduction of energy intake below the average daily intake of 1381 kcal.
Figure 2b demonstrates that a reduction of high ED food intake is necessary for hypocaloric energy intake. The changes of high ED food intake do not affect total daily food quantity due to parallel reduction of lowered medium ED food.
Figure 2a Change of daily energy intake (kcal/d) in relation to an intraindividual increase of the consumption of low ED food items.*= p<0.05 or less versus each individuals’ 12 days average intake.
Figure 2b Change of daily energy intake (kcal/d) in relation to an intraindividual increase of the consumption of high ED food items.*= p<0.05 or less versus each individuals’ 12 days average intake.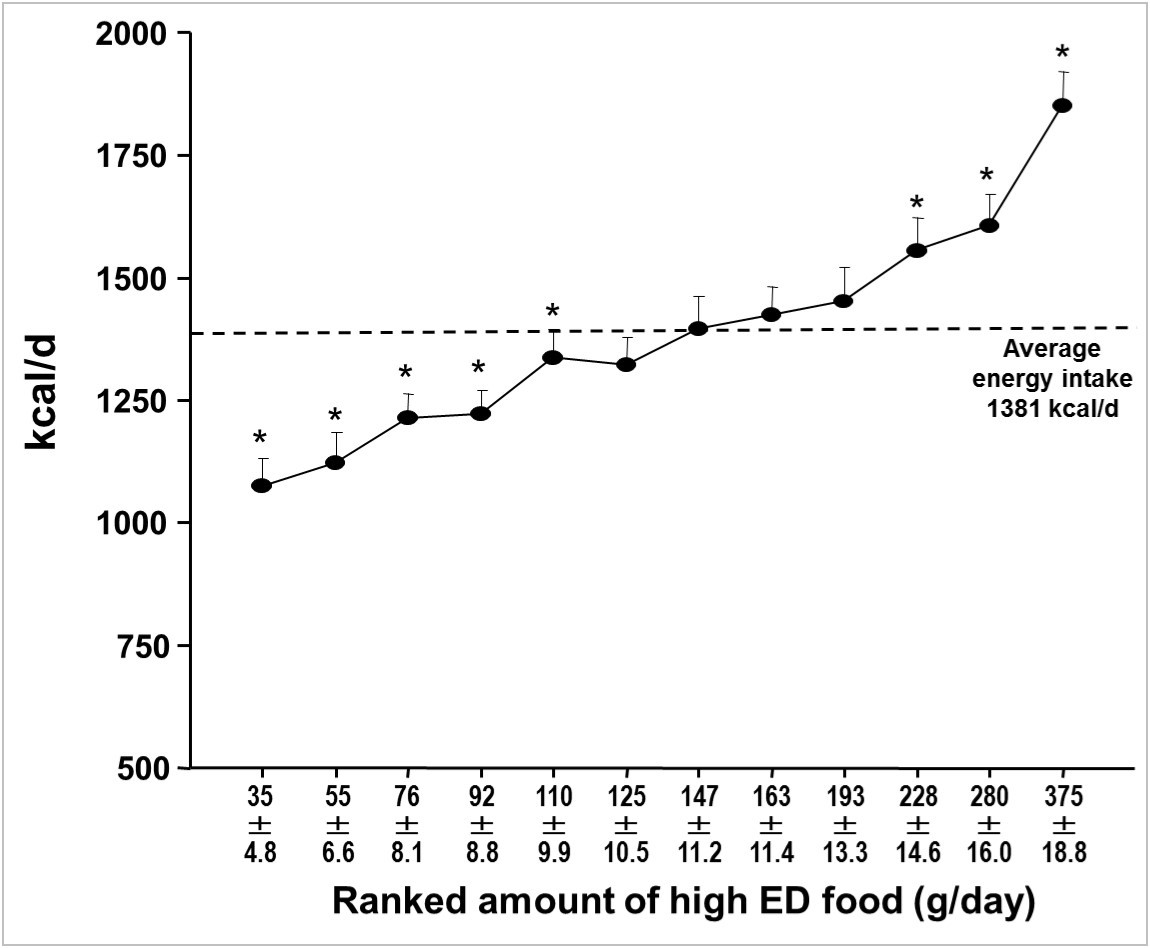
food groups
Major contributions to energy intake prior to treatment came from bread, meat products, carbohydrate accompaniments, cake, cheese, meat, and fruit (Table 3). These 7 food groups accounted for 63% of daily energy intake (Table 4).
Table 3. Energy intake (kcal/day), food quantity (g/day) and frequency of consumption by the various food groups before and after change of eating habits (mean ± SD);| kcal/day | gram/day | % frequency | ||||
| before | after | before | After | before | after | |
| Bread | 260±6.0 | 178±5.1* | 113±2.6 | 78±2.2* | 93.2 | 84.8* |
| Dessert | 17±2.9 | 17±2.3 | 11±1.9 | 11±1.6 | 7.0 | 7.6 |
| Eggs | 20±1.7 | 28±2.2* | 13±1.2 | 19±1.5* | 20.3 | 25.1* |
| Stews | 25±3.7 | 24±3.3 | 25±3.7 | 24±3.3 | 8.7 | 9.4 |
| Ice cream | 5±1.4 | 7±1.8 | 2±0.6 | 3±0.8 | 3.1 | 3.6 |
| Fastfood | 22±4.4 | 8±2.4* | 9±1.8 | 3±1.0* | 4.1 | 2.5 |
| Delicatessen | 60±6.2 | 54±5.8 | 29±3.0 | 27±2.8 | 16.3 | 15.5 |
| Fish | 28±2.6 | 27±2.7 | 23±2.2 | 23±2.3 | 19.8 | 18.2 |
| Meat | 91±4.9 | 99±4.9 | 70±3.8 | 77±3.8 | 40.8 | 45.9* |
| Meat products | 138±8.3 | 103±8.4* | 48±2.9 | 37±3.0* | 48.7 | 36.2* |
| Cake | 101±6.7 | 56±4.7* | 31±2.1 | 18±1.5* | 32.4 | 21.8* |
| Yogurt | 37±2.7 | 35±3.2 | 38±2.7 | 36±3.2 | 26.0 | 20.2* |
| Cheese | 99±5.4 | 70±4.2* | 28±1.5 | 22±1.2* | 52.7 | 43.4* |
| Carb.accomp. | 106±4.6 | 97±4.2 | 97±4.1 | 88±3.8 | 51.6 | 50.5 |
| Marmalade | 24±1.4 | 17±1.4* | 7±0.4 | 5±0.4* | 40.8 | 27.3 |
| Cereals | 22±3.8 | 15±2.4 | 7±1.2 | 5±0.8 | 11.4 | 10.9 |
| Fruit | 81±3.2 | 65±3.1* | 162±6.3 | 131±6.2* | 67.1 | 56.1* |
| Oil | 10±1.2 | 8±0.9 | 1±0.1 | 0.9±0.1 | 12.1 | 10.7 |
| Proc. potatoes | 8±2.5 | 10±2.5 | 3±1.0 | 4±1.0 | 3.4 | 3.6 |
| Curd | 20±2.4 | 39±2.9* | 20±2.4 | 39±2.9* | 21.6 | 32.7* |
| Cream | 3±0.9 | 2.5±0.6 | 1±0.4 | 1±0.2 | 3.4 | 3.2 |
| Vegetables | 36±1.3 | 33±1.3 | 181±6.5 | 168±6.3 | 75.2 | 73.9 |
| Ham | 26±2.2 | 35±2.4* | 20±1.7 | 27±1.8* | 31.9 | 41.5 |
| Sauces | 4±0.6 | 5±0.6 | 5±0.7 | 6±0.8 | 12.7 | 12.0 |
| Butter | 57±2.7 | 23±1.9* | 9±0.4 | 4±0.3* | 53.5 | 27.0* |
| Soup | 31±3.0 | 29±2.8 | 52±5.0 | 48±4.7 | 16.0 | 14.9 |
| Chocolate, nuts | 50±4.0 | 25±2.9* | 11±0.8 | 5±0.6* | 28.2 | 16.1* |
| Sugar | 0.5±0.2 | 0.2±0.1 | 0.1±0.04 | 0.04±0.02 | 1.0 | 0.4 |
| % kcal | % gram | |||
| before | after | Before | after | |
| Bread | 19.6±4.18 | 16.9±5.1* | 12.2±3.1 | 10.2±4.1* |
| Dessert | 1.2±2.0 | 1.5±2.0 | 1.1±2.0 | 1.3±2.0 |
| Eggs | 0.7±1.0 | 2.7±2.0* | 1.4±1.02 | 2.3±2.0* |
| Stews | 1.7±2.0 | 2.3±3.1 | 2.3±3.1 | 2.6±4.1 |
| Ice cream | 0.3±1.0 | 0.5±1.0 | 0.2±0.5 | 0.3±1.0 |
| Fastfood | 1.3±3.1 | 0.6±2.0* | 0.8±2.0 | 0.4±1.0* |
| Delicatessen | 3.9±4.1 | 4.3±5.1 | 3.0±3.1 | 3.3±4.0 |
| Fish | 2.1±2.0 | 2.7±3.1 | 2.4±2.0 | 2.7±3.0 |
| Meat | 7.0±4.1 | 9.5±5.1* | 7.0±4.1 | 8.3±4.1* |
| Meat products | 8.8±5.1 | 7.5±5.1 | 4.9±3.1 | 4.0±3.1* |
| Cake | 6.5±4.1 | 4.5±4.1 | 3.2±2.0 | 2.2±3.0* |
| Yogurt | 2.9±2.0 | 3.1±3.1 | 3.8±3.1 | 3.7±2.0 |
| Cheese | 6.9±3.1 | 6.2±4.1 | 3.0±2.0 | 2.5±2.0* |
| Carb. accomp. | 8.2±4.1 | 9.1±4.1 | 9.5±4.1 | 10.0±5.1 |
| Marmalade | 1.8±1.0 | 1.5±1.0 | 0.8±4.1 | 0.6±1.0 |
| Cereals | 1.4±2.0 | 1.3±2.0 | 0.6±1.0 | 0.5±1.0 |
| Fruit | 6.3±3.1 | 5.9±3.1 | 15.0±6.1 | 12.7±5.1 |
| Oil | 0.7±1.0 | 0.6±1.0 | 0.1±0.2 | 0.1±0.1 |
| Proc. potatoes | 0.5±1.0 | 0.8±2.0 | 0.4±1.0 | 0.5±1.0 |
| Curd | 1.6±2.0 | 3.5±3.1* | 1.9±0.2 | 3.9±3.1* |
| Cream | 0.2±0.6 | 0.2±0.6 | 0.1±0.4 | 0.1±0.3 |
| Vegetables | 3.2±1.0 | 3.3±1.0 | 17.5±6.1 | 17.5±6.1 |
| Ham | 2.0±2.0 | 3.3±2.0* | 1.9±2.0 | 3.2±2.0* |
| Sauces | 0.3±0.5 | 0.5±0.5 | 0.5±0.7 | 0.7±1.0 |
| Butter | 4.3±2.0 | 2.3±2.0 | 1.1±0.4 | 0.6±0.5* |
| Soup | 2.6±3.2 | 3.1±2.0 | 4.8±4.1 | 5.3±5.1 |
| Chocolate, nuts | 3.2±3.1 | 2.1±2.0* | 1.1±1.0 | 0.6±1.0* |
| Sugar | 0.03±0.1 | 0.01±0.1 | 0.01±0.1 | 0.0±0.1 |
The major contribution to daily food quantity came from vegetables, fruit, bread, carbohydrate accompaniments, meat, meat products and soup. These 7 food groups accounted for 71% of daily quantity.
Following the change of eating habits significant changes of energy intake were due to a significant reduction of bread, fast-food, meat products, cake, cheese, marmalade, fruit, butter and chocolate (Table 3). A significant increase was observed for eggs, curds and ham. Changes of energy intake are reflected by alterations of the respective food quantities. The reduction was due to a combination of fewer days where the respective food item was actually eaten and to a smaller daily portion size for bread, cake, cheese, butter, and chocolate.
A reduction of the frequency of intake with constant portion size was observed for marmalade, fruit and meat products (f).
The increased consumption of eggs and ham was due to intake on more days with similar portions when eaten while curd was eaten more frequently and in greater portions.
For two food groups subjects changed the frequency of intake, but without leading to a significant increase in the amount consumed. Meat intake frequency increased moderately but portion sizes were reduced thereby compensating the higher frequency of intake. The reduced number of days where yogurt was eaten was counterbalanced by significantly greater portions (Table 3).
The relative contributions of the various food groups to daily energy intake remained fairly similar(Table 4). The highest contributors before were, in order: meat products, carbohydrate accompaniments, meat, cheese, cake and fruit. Thereafter, meat was in second place and meat products in fourth, and cake and fruit changed places sixth and seventh, respectively. The relative contribution to food quantity showed a virtually unchanged ranking of vegetables, fruit, bread, carbohydrate and meat, while meat products and soup switched places 6 and 7 (Table 4).
Discussion
The present data demonstrate that in older, severely obese patients a change of individual eating habits can successfully reduce body weight, improve diabetes and enable patients to maintain their new weight for a prolonged period.
It is noteworthy that food intake prior to the start of treatment is characterized by low energy density and low total energy intake while food quantity is not much different from a cohort which was 25 years younger and of similar weight and gender 41, 42. We attribute this low ED food portfolio to the fact that virtually all these patients have had long periods of dieting in their life. Nevertheless, it must be noted that they were weight stable for at least 6 months prior to treatment and they did not lose weight while recording their intake. 44 patients of this population were part of the previously published data on weight loss and maintenance 35.
These patients were able to reduce their total energy intake by 334 kcal/day [solid food + liquid). The reduction of solid food energy intake is due to a combination of a small reduction in food quantity (down 100g) and reduced energy density. The reduction in food quantity is a mixture of smaller portion sizes and less frequent intake.
The number of meals has always been a matter of debate in obesity treatment concepts. Snacks between meals are well known to increase daily energy intake 44, 45, 46. Accordingly, omission of snacks can be favourable for a hypocaloric intake. The present data show that these patients reduce but do not abandon snack intake completely, which emphasizes the individual options of this concept. Reduction in snacking is certainly favorable but not mandatory for successful weight loss.
Skipping breakfast is of special interest. Several cross-sectional studies have demonstrated an association between greater energy intake at breakfast and lower body weight 47, 48, 49. On the other hand, an analysis of food intake in young adults in Bogalusa 50 showed that greater breakfast energy intake is associated with a higher total daily intake. This notion is also supported by acute feeding experiments of Cotton et al 51. Furthermore, a recent intraindividual analysis in free-living obese and normal weight subjects has demonstrated that greater breakfast intake leads to more overall daily energy intake 43. With regard to weight loss a short-time intervention study was unable to demonstrate clear results 52.
Data of the National Weight Control Registry have shown that 78% of the subjects with successful weight loss and maintenance regularly ate breakfast which led the authors to the conclusion that this is of great importance to be successful. The other 22 % who skipped breakfast were also successful 37. It must be kept in mind that approximately 20% of normal weight subjects regularly skip breakfast 42, 43. The present data clearly demonstrate that breakfast skipping does not jeopardize long-term weight loss and for some patients it was a good opportunity to save calories compatible with the individual’s eating habits.
Usual recommendations in obesity treatment concepts use defined limits of energy intake, an augmentation of dietary fiber and a reduction of certain macronutrients. Recently we have demonstrated that all this is not necessarily mandatory for successful weight loss and maintenance 35 and this is also true for this cohort of elderly subjects.
Prescription of energy intake is difficult to maintain due to the substantial fluctuations of daily energy intake which has been known for many decades in normal weight 53 and also obese subjects 41.
Dietary fiber intake prior to treatment was already far below the usual recommendations of 30g/day or more 54. Considering the quantities of the various food items that have to be consumed to reach this level it is rather unrealistic to expect that older patients in particular can adhere to these suggestions. Moreover, we have recently shown in an intraindividual analysis that greater fiber intake is associated with substantially greater energy intake 55. Dietary fiber is favorable when fiber replaces energy containing food ingredients such as flour (comparison: white bread – whole grain bread). This however, is also reflected in the energy density of these food items (2.5 vs. 2.0 kcal/g), which makes counting of fiber intake unnecessary.
Most treatment concepts for a hypocaloric diet are based on changes of the macronutrient ratio. Low-fat, low carb or high-protein/low fat diets have been shown to result in comparable rates of weight reduction 9, 10, 12, 14, 16, 17, 18, 19, 20, 21, 22. Furthermore, the analysis of eating habits has shown that adherence to the recommended macronutrient ratio was rather poor 10, 22, 56 60. In the present concept fixed dietary prescriptions were avoided. The focus on energy density leads to a reduction of both fat and carbohydrate intake while protein remains largely unchanged. These data demonstrate that the focus on ED as the only parameter makes a consideration of all macronutrients unnecessary which can be helpful to reduce the intellectual workload prior to taking a bite.
Reduction in energy intake has been accomplished by an exchange of food items with higher ED toward those with lower ED based on the individual’s preferences. Patients appreciate the option to select freely among a wide range of food items with the chance to counterbalance occasional or even regular intake of certain high ED foods. Especially in older persons it seems to be important that they can stick to their traditional dishes. A major change of life-long eating habits must be regarded as highly improbable.
When looking at the food items that contributed to reduction of energy intake it is interesting to note that the widely recommended higher intake of fruit and vegetables did not occur. On the contrary, fruit intake was significantly reduced which is primarily due to the smaller number of snacks. Bread is the most important energy source in German nutrition accounting for almost 20% of daily energy intake in normal weight as well as in obese subjects 42, 57.
The reduction of bread intake saves 50 kcal/day but it remains among the 3 most important contributors to food quantity. All in all, 9 of the 28 analyzed food groups contribute significantly to reduced calorie consumption. The reductions of the medium and high ED food are sufficient to allow an even greater energy intake by low ED food items (eggs, ham, curd).
When looking at the ranking of the various food groups for their contribution to energy intake and daily food quantity only small changes were observed. This suggests that the “new” eating habits are not so much different from the “old” ones, which in our experience is a major reason for better long-term adherence. In addition to alterations of solid food intake the substantial reduction of liquid calories is extremely important especially in these elderly subjects where nutritional habits prior to treatment were certainly not bad.
Some limitations of the present study have to be considered. Firstly, under- or over-reporting of food intake can not be excluded. However total daily EI of the present study population is in the same range of the age and gender related groups of the recent National Survey of Food Intake II in Germany 57. Whenever it occurs, it may differ systematically between subjects such that certain participants tend to under- or overestimate more than others 58. Furthermore, the results of the present study are based on changes of intake that are calculated individually for each subject. In addition to this, the present study recorded no parameters of strength and function. That might be of importance for improvement of functionality, further weight loss and maintenance. Future trials will therefore include functional parameters for an adequate evaluation of the effects of the ED approach in older persons. Additionally the combination with an exercise program has to be considered and might improve the results shown in this study.
The present data demonstrate that a change of eating habits based on food ED which is individually tailored leads to significant weight loss and also permits long-term weight maintenance. Food ED is simple and easy to handle in every day dietary counseling. The present data also demonstrate that apart from food ED, changes of beverages and reductions to the number of meals contribute to lower energy intake. A reduction of medium and high ED food intake is of greater importance than an augmentation of low ED food consumption.
All in all, older patients with severe obesity will most probably benefit from weight reduction leading to greater mobility and improving co-morbidities such as type-2 diabetes mellitus.
References
- 1.Ogden C L, Carroll M D, Curtin L R, McDowell M A, Tabak C J et al. (2006) Prevalence of overweight and obesity in the United States. , JAMA 295, 1549-55.
- 2.Gutiérrez-Fisac J L, Guallar-Castillón P, León-Muñoz L M, Graciani A, Banegas J R et al. (2012) Prevalence of general and abdominal obesity in the adult population of Spain, 2008-2010: the ENRICA study. , Obes Rev 13, 388-92.
- 3.Kaiser R, Winning K, Uter W, Volkert D, Lesser S et al. (2010) Functionality and mortality in obese nursing home residents: an example of 'risk factor paradox'?. , J Am Med Dir Assoc 11, 428-35.
- 4.Houston D K, Nicklas B J, Zizza C A. (2009) Weight concerns. The growing prevalence of obesity among older adults. , J Am Diet Assoc 109, 1886-1895.
- 5.Al Snih S, Ottenbacher K J, Markides K S, Kuo Y F, Eschbach K et al. (2007) The effect of obesity on disability vs mortality in older Americans. , Arch Intern Med 167, 74-80.
- 6.Koster A, Visser M, Simonsick E M, Yu B, Allison D B et al. (2010) Health, Aging and Body Composition Study. Association between fitness and changes in body composition and muscle strength. , J Am Geriatr Soc 58, 219-26.
- 7.Stenholm S, Alley D, Bandinelli S, Griswold M E, Koskinen S et al. (2009) The effect of obesity combined with low muscle strength on decline in mobility in older persons: results from the InCHIANTI study. , Int J Obes (Lond) 33, 635-44.
- 8.Villareal D T, Banks M, Sinacore D R, Siener C, Klein S. (2006) Effect of weight loss and exercise on frailty in obese older adults. , Arch Intern Med 166, 860-6.
- 9.Villareal D T, Chode S, Parimi N, Sinacore D R, Hilton T et al. (2011) Weight loss, exercise, or both and physical function in obese older adults. , N Engl J Med 364, 1218-1229.
- 10.Sacks F M, Bray G A, Carey V J, Smith S R, Ryan D H et al. (2009) Obarzanek E. , Williamson DA, N Engl J Med 360, 859-73.
- 11.Torgerson J S, Hauptman J, Boldrin M N, Sjostrom L. (2004) XENical in the prevention of diabetes in obese subjects (XENDOS) study: a randomized study of orlistat as an adjunct to lifestyle changes for the prevention of type 2 diabetes in obese patients. , Diabetes Care 27, 155-161.
- 12.Anderson J W, Konz E C, Frederich R C, Wood C L. (2001) Long-term weight-loss maintenance: a meta-analysis of US studies. , Am J Clin Nutr 74, 579-584.
- 13.Douketis J D, Macie C, Thabane L, Williamson D F. (2005) Systematic review of long-term weight loss studies in obese adults: clinical significance and applicability to clinical practice. , Int J Obes (Lond) 29, 1153-1167.
- 14.Dansinger M L, Tatsioni A, Wong J B, Chung M, Balk E M. (2007) Meta-analysis: the effect of dietary counseling for weight loss. , Ann Intern Med 147, 41-50.
- 15.Arnold A M, Newman A B, Cushman M, Ding J, Kritchevsky S. (2010) Body weight dynamics and their association with physical function and mortality in older adults: the Cardiovascular Health Study. , J Gerontol A Biol Sci Med Sci 65, 63-70.
- 16.Astrup A, Grunwald G K, Melanson E L, Saris W H, Hill J O. (2000) The role of low-fat diets in body weight control: a meta-analysis of ad libitum dietary intervention studies. , Int J Obes Relat Metab Disord 24, 1545-1552.
- 17.Nordmann A J, Nordmann A, Briel M, Briel M, Keller U et al. (2006) Effects of low-carbohydrate vs low-fat diets on weight loss and cardiovascular risk factors: a meta-analysis of randomized controlled trials. , Arch Intern Med 166, 285-293.
- 18.Skov A R, Toubro S, Ronn B, Holm L. (1999) Astrup A. , Int J Obes Relat Metab Disord 23, 528-536.
- 20.Dansinger M L, Gleason J A, Griffith J L, Selker H P, Schaefer E J. (2005) Comparison of the Atkins, Ornish, Weight Watchers, and Zone diets for weight loss and heart disease risk reduction: a randomized trial. , JAMA 293, 43-53.
- 21.Gardner C D, Kiazand A, Alhassan S, Kim S, Stafford R S et al. (2007) Comparison of the Atkins, Zone, Ornish, and LEARN diets for change in weight and related risk factors among overweight premenopausal women: the A TO Z Weight Loss Study: a randomized trial. , JAMA 297, 969-977.
- 22.Shai I, Schwarzfuchs D, Henkin Y, Shahar D R, Witkow S et al. (2008) Weight loss with a low-carbohydrate, Mediterranean, or low-fat diet. , N Engl J Med 359, 229-241.
- 23.Wing R R. (1998) Behavioral approaches to the treatment of obsesity. In:. Handbook of Obesity Bray G, Bouchard C, James P, editors , New York: 855-873.
- 24.Wing R R. (2003) Behavioral interventions for obesity: recognizing our progress and future challenges. Suppl: 3S-6S , Obes Res 11.
- 25.Stubbs R J, Ritz P, Coward W A, Prentice A M. (1995) Covert manipulation of the ratio of dietary fat to carbohydrate and energy density: effect on food intake and energy balance in free-living men eating ad libitum. , Am J Clin Nutr 62, 330-337.
- 26.Schick R R, Schusdziarra V. (1994) Regulation of food intake. Obesity in Europe 93 In: Ditschuneit HH, Gies FA, Hauner H, Schusdziarra V, Wechsler JG, editors , London: 335-348.
- 27.Westerterp-Plantenga M S, Pasman W J, Yedema M J, Wijckmans-Duijsens N E. (1996) Energy intake adaptation of food intake to extreme energy densities of food by obese and non-obese women. , Eur J Clin Nutr 50, 401-407.
- 28.Bell E A, Rolls B J. (2001) Energy density of foods affects energy intake across multiple levels of fat content in lean and obese women. , Am J Clin Nutr 73, 1010-1018.
- 29.Poppitt S D, Prentice A M. (1996) Energy density and its role in the control of food intake: evidence from metabolic and community studies. , Appetite 26, 153-174.
- 30.Kant A K, Graubard B I. (2005) Energy density of diets reported by American adults: association with food group intake, nutrient intake, and body weight. , Int J Obes (Lond) 29, 950-956.
- 31.Ledikwe J H, Blanck H M, Kettel K L, Serdula M K, Seymour J D et al. (2006) Dietary energy density is associated with energy intake and weight status in US adults. , Am J Clin Nutr 83, 1362-1368.
- 32.Rolls B J, Roe L S, Beach A M, Kris-Etherton P M. (2005) Provision of foods differing in energy density affects long-term weight loss. , Obes Res 13, 1052-1060.
- 33.Ledikwe J H, Rolls B J, Smiciklas-Wright H, Mitchell D C, Ard J D et al. (2007) Reductions in dietary energy density are associated with weight loss in overweight and obese participants in the PREMIER trial. , Am J Clin Nutr 85, 1212-1221.
- 34.Ello-Martin J A, Roe L S, Ledikwe J H, Beach A M, Rolls B J. (2007) Dietary energy density in the treatment of obesity: a year-long trial comparing 2 weight-loss diets. , Am J Clin Nutr 85, 1465-1477.
- 35.Schusdziarra V, Hausmann M, Wiedemann C, Hess J, Barth C et al. (2011) Successful weight loss and maintenance in everyday clinical practice with an individually tailored change of eating habits on the basis of food energy density.EurJNutr50:. 351-361.
- 37.Wyatt H R, Grunwald G K, Mosca C L, Klem M, Wing R R et al. (2002) Long-term weight loss and breakfast in subjects in the National Weight Control Registry. , Obes Res 10, 78-82.
- 38.Gorin A, Phelan S, Hill J A, Wing R R. (2004) Medical triggers are associated with better long-term weight maintenance. , Prev Med 39, 612-616.
- 40.Schusdziarra V, Hausmann M. (2007) Satt essen und abnehmen – individuelle Ernährungsumstellung ohne Diät. , Neu-Isenburg, Germany
- 41.Schusdziarra V, Hausmann M, Wittke C, Mittermeier J, Kellner M et al. (2010) Contribution of energy density and food quantity to short-term fluctuations of energy intake in normal weight and obese subjects. , Eur J Nutr 49, 37-43.
- 42.Schusdziarra V, Sassen M, Hausmann M, Wittke C, Erdmann J. (2009) [Food items, energy intake, food quantity and energy density during main meals and snacks of overweight and obese subjects] (German) Aktuel Ernahrungsmed. 34, 186-194.
- 43.Schusdziarra V, Hausmann M, Wittke C, Mittermeier J, Kellner M et al. (2011) Impact of breakfast on daily energy intake – an analysis of absolute versus relative breakfast calories. , Nutrition Journal 10, 5.
- 44.Berteus-Forslund H, Torgerson J S, Sjostrom L.Lindroos AK (2005) Snacking frequency in relation to energy intake and food choices in obese men and women compared to a reference population. , Int J Obes 29, 711-719.
- 45.Haveman-Nies A, de Groot LP, van Staveren WA. (1998) Snack patterns of older Europeans. , J Am Diet Assoc 98, 1297-1302.
- 46.Kerver J M, Yang E J, Obayashi S, Bianchi L, Song W O. (2006) Meal and snack patterns are associated with dietary intake of energy and nutrients in US adults. , J Am Diet Assoc 106, 46-53.
- 47.Cho S, Dietrich M, Brown C J, Clark C A, Block G. (2003) The effect of breakfast type on total daily energy intake and body mass index: results from the Third National Health and Nutrition Examination Survery (NHANES III). , J Am Coll Nutr 22, 296-302.
- 48.Summerbel C D, Moody R C, Shanks J, Stock M J, Geissler C. (1996) Relationship between feeding pattern and body mass index in 220 free-living people in four age groups. , Eur J Clin Nutr 50, 513-519.
- 49.Berteus-Forslund H, Lindroos A K, Sjostrom L, Lissner L. (2002) Meal patterns and obesity in Swedish women- a simple instrument describing usual meal types, frequency and temporal distribution. , Eur J Clin Nutr 56, 740-747.
- 50.Nicklas T A, Myers L, Reger C, Beech B, Berenson G S. (1998) Impact of breakfast consumption on nutritional adequacy of the diets of young adults in Bogalusa, Louisiana: ethnic and gender contrasts.J Am Diet Assoc98:. 1432-1438.
- 51.Cotton J R, Burley V J, Blundell J E. (1994) Fat and satiety: effect of fat in combination with either protein or carbohydrate. In: Obesity. in Europe 93, edited by Ditschuneit 349-355.
- 52.Schlundt D G, Hill J O, Sbrocco T, Pope-Cordle J, Sharp T. (1992) The role of breakfast in the treatment of obesity: a randomized clinical trial.Am JClinNutr55:. 645-651.
- 53.Sempos C T, Johnson N E, Smith E L, Gilligan C. (1985) Effects of intraindividual and interindividual variation in repeated dietary records. , Am J Epidemiol 121, 120-130.
- 54.korrigierter Nachdruck, Umschau Verlag (2008) D-A-CH-Referenzwerte für die Nährstoffzufuhr. , Frankfurt 1.
- 55.Schusdziarra V, Hausmann M, Sassen M, Kellner M, Mittermeier J et al. (2011) Ballaststoffe, Energieaufnahme und Lebensmittelverzehr. , Aktuel Ernaehrungsmed 36, 23-30.
- 56.Ullrich A, Erdmann J, Margraf J, Schusdziarra V. (2003) Impact of carbohydrate and fat intake on weight-reducing efficacy of orlistat. , Aliment Pharmacol Ther 17, 1007-1013.
