Childhood Overweight, Social Media, and Osteoarthritis: Is there a Possible Emergent, yet Unrecognized Linkage?
Abstract
Background
Osteoarthritis, a serious and increasingly prevalent disabling global health condition found largely among older adults, has been linked to the presence of excess body weight. But what contributes to this growing health epidemic of excess weight, which is increasingly observed in children? Moreover, can a case be made for predicting a possible negative linkage between the pervasive use of social media from the earliest point in time and possible subsequent childhood overweight or obesity and late life osteoarthritis that may be amenable to intervention?
Methods
To examine the most probable answers to these questions, the EBSCO, Scopus and PUBMED data bases were sourced for relevant data. The extracted data were carefully reviewed, categorized and documented in narrative format.
Results
While one cannot readily carry out research to answer the above questions, prevailing data imply that there is more risk of being overweight in childhood, as well as acquiring possible later life disabling osteoarthritis, or a more serious manifestation of this disease, through the prolonged, unfettered and frequent use of social media in early and middle childhood.
Conclusion
Those in the realm of developing preventive strategies against childhood overweight or obesity as well as osteoarthritis are strongly encouraged to examine the role of the media environment and messages children are exposed early on in this regard. Alternately, children who already have disabilities, joint pain due to arthritis or other health conditions, and who may have to rely more on social media than others who are active- may suffer more readily from an energy imbalance and become overweight if due precautions against this are not taken.
Author Contributions
Academic Editor: Ogadimma Arisukwu, Landmark University, Nigeria.
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2020 Ray Marks
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Background
Childhood overweight or obesity, a current pervasive health challenge of immense proportions, affecting more than 43 million preschool children worldwide, is a serious, often long lasting health condition that is highly challenging to reverse. These data, which do not reflect the known negative consequences of excess body weight in childhood, may also be underestimates since the prevalence of overweight or obesity among children and adolescents (aged 2-18 years) has increased rapidly, with more than 100 million being affected in 2015 1.
Occurring when a child is well above the normal weight for his or her age and height, this growing epidemic has failed to respond in any meaningful way to date despite substantive multi-component and uni-dimensional intervention efforts to offset this situation. Rather, the childhood overweight epidemic, appears to be on the way to continuing to affect untold numbers of children and adolescents worldwide, and hence possibly many aging adults, for years to come in multiple adverse ways.
As outlined by Kumar and Kelly 2, childhood obesity, which is a very debilitating condition in its own right and one that is very challenging to reverse, or eliminate, has consequently emerged as one of the most highly salient and pressing public health problems, not only in the United States (US), but in most other countries, including developing countries. As an example, current data show at least one third of children in the US are considered to be excessively overweight or obese. This situation, when viewed in the long-term, is not only highly relevant to the goal of attaining healthy aging for all in the US and other countries, as well as cost containment themes, as the population ages, but also to the recent COVID-19 pandemic, where obese adults are persistently found to be at higher risk for the viral infection, as well as worse outcomes than normal weight adults. In particular, because excess weight in youth, commonly leads to one or more irreversible costly negative health outcomes in later life, countries such as Britain are now making obesity prevention a number one public health imperative 3 (https://time.com/5872175/boris-johnson-weight-loss-coronavirus/).
That is, given that childhood overweight has both immediate, as well as long-term adverse effects on health and well-being, and that many researchers and health personnel have been and are seeking solutions to averting or eliminating this problem in most cases that are not based on genetics, but have not been totally successful, more thought about this health issue appears warranted.
Indeed, while childhood overweight has immense medical health implications, it also has immense financial, socioeconomic, as well as physical implications, if unrelieved or reversed. These problems include, but are not limited to an increased risk for one or more of the following health challenges:
An increased risk for cardiovascular diseases, such as stroke, and/or high blood pressure.
The risk of pre-diabetes, which can lead to adult type 2 diabetes.
An increased risk for various forms of cancer.
An increased risk for bone and joint problems, sleep apnea, chronic pain and psychosocial problems such as stigmatization, depression, social anxiety, poor self-esteem, and opioid addiction.
In addition, obese children and adolescents are likely to become obese adults4 whoare at high risk for adult health problems such as heart disease, type 2 diabetes, stroke, several types of cancer, and osteoarthritis, among other health issues 5. Indeed, one study showed that children who became obese as early as age two were more likely to be obese as adults. Another, showed young boys presenting with a high body fat content had objectively assessed lower limb joint kinematic pattern alterations that could potentially predispose them to variable degrees of joint dysfunction and mobility problems later on 6.
Thus, as outlined by Kumar and Kelly 2 the increasing prevalence of childhood obesity is not only an academic issue, but an immensely problematic individual potential social problem, and one consistently associated with the emergence of one or more comorbid health conditions previously considered to be solely "adult" in nature such as type 2 diabetes, hypertension, nonalcoholic fatty liver disease, obstructive sleep apnea, osteoarthritis and dyslipidemia. These diseases, along with obesity in its own right are also very strong predictors of COVID-19 risk and worse health outcomes, hence of key concern.
While Di Cesare et al. 7 report that key drivers of this obesity epidemic stem from an obesogenic environment, which includes changing food systems and reduced physical activity, they do not mention social media explicitly. Yet, according to Deoke et al. 8 among the many reasons underpinning the rise in childhood obesity are the changing lifestyles of families with increased purchasing power, food marketing and manipulation, addictive foods, coupled with the increasing hours of daily inactivity due to television, video games and computers that have replaced outdoor games and other social activities. Globally, it is not surprising therefore, that an estimated 10% of school-aged children, between 5 and 17 years of age, who often are subjected to the advertising they encounter on social media, are said to be overweight and obese. These data do also not include the impact of situational factors, such as the 2020 COVID-19 pandemic related ‘lockdowns’ where children are kept ‘home’, and potentially experience anxiety, as well as more sedentary lifestyles, while interacting even more excessively with social media than during pre-coronavirus times, and possibly with more readily available food snacks.
In support of the aforementioned ideas, Lee et al. 1 propose childhood and adolescent obesity, which is linked to adulthood mortality and premature death is due largely to an imbalance between caloric intake and physical activity, as well as environmental factors. In addition, not discounting genetic and biological factors, socio-economic factors, including family, school, community, and national policies are cited to play a crucial role.
This current article focuses on the possible linkage of social media usage in excess, as a relatively unexplored determinant of childhood obesity. It explores if a case can be made for excess social media usage to heighten the risk for the late life disease known as osteoarthritis, a widespread joint disease affecting largely older adults that is irreversible and highly disabling. Affecting the knee and spinal joints, in particular 5, the reason for exploring this potential injurious source, is that among one of its major causes, as well having a worse overall health outcome in the case of osteoarthritis is obesity. It specifically examines what is known about the direct impact of social media usage on the emergence of childhood obesity. Drawing on the available literature it outlines a potential pathway to adolescent and adult obesity that is relatively unexplored and is partly determined by the nature of social media messages, content, and time on social media messaging tasks.
Since the risk factors for childhood obesity of diet and physical activity are well studied, and the link between early obesity and cardiovascular diseases is well established, this overview specifically elected to examine whether social media usage, a reasonably new form of media adopted by young people as a key communication and social interactive tool, has the potential to exacerbate childhood overweight trends, due to its impact on physical activity 15, as well as messages and interactions experienced by this medium of communication, even if social media can be favorably employed to counter this health issue.
In particular, this report investigates the evidence base concerning the idea that excess or uncontrolled social media usage by young people may have an immensely negative impact in our view on physical activity, dietary choices, and messages that are aversive and emotionally charged and that can heighten obesity risk in young people especially if usage is unrestricted. Because overweight and obesity in childhood (including adolescence) are independently associated with serious physiological, psychological, and social consequences, including negative impacts on the musculoskeletal system, a major disabler of older persons, it examines if more efforts to regulate social media usage at various levels are desirable in efforts to prevent a life of possible pain, disability, opioid usage and possible addiction, among other negative situations, and if there is support for the ideas presented in Figure 1.
Figure 1.Hypothetical interaction of obesity and osteoarthritis, wherein those with an early obesity onset are likely to have higher risk for acquiring osteoarthritis at any age, especially higher ages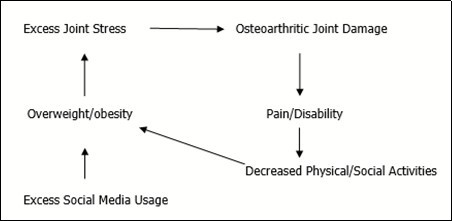
The review does not examine some of the other leading causes leading of childhood obesity, such as limited amount of safe space available for physical activities, lack of healthy food sources in the area, and the abundance of fast-food chain. Using EBSCO, Scopus, and PUBMED data bases and key words: childhood overweight or obesity and osteoarthritis/social media influences/usage, salient articles speaking to social media marketing and sleep issues were specially sought. Other media were not examined directly, and the use of social media to prevent childhood obesity, as well as parental social media use and influences were not explicitly explored. The term social media was applied to represent usage of one or more of the media sources highlighted in Table 1.
Table 1. Popular social media sites used by children and adolescents even though some may have age restrictions| Popular media mode sources | Actions of use |
| -*Instagram vloggers | |
| GroupMe | |
| Chatting | |
| Meeting | |
| KikMessenger (Companies may communicate with user directly at high rates) | Micro Blogging |
| *SnapChat | Picture sharing |
| Tumblir | Sharing videos |
| Texting | |
| *UTube | |
| -*UTube vloggers | |
Results
Osteoarthritis and Childhood Obesity
Among the various noteworthy findings in the context of this exploratory overview, work by Anthony et al. 9 clearly shows childhood overweight measures to be significantly associated with adulthood knee mechanical joint pain, stiffness and dysfunction among men, independent of adult overweight. Anthony et al. 9 who sought todescribe the associations between measures of overweight in childhood and knee pain, stiffness and dysfunction among adults 25 years later using subjects broadly representative of the Australian population (n=449, aged 31-41 years, female 48%) from the Australian Schools Health and Fitness Survey of 1985 found the prevalence of knee pain was 34% and overweight inchildhood and adulthood was 7% and 48%, respectively. Overall, there were no significant associations between childhood overweight measures and total knee pain scores, stiffness and dysfunction scores in adulthood. However, in men, overweight in childhood was associated with the adulthood onset of knee pain and childhood weight and body mass indices were associated with their subjective stiffness and dysfunction measures. Subjects who were overweight in both childhood and adult life had a significant increase in the risk and prevalence of adulthood walking pain.
In another study, Bout-Tabaku et al. 10 found significantly greater variability in knee alignment among females at higher body mass index Z-scores, as well as greater valgus alignment of the lower limb in obese adolescents during late puberty. Although this group concluded that longitudinal studies would be needed to determine whether childhood obesity is a risk factor for progressive lower leg mal-alignment that may predispose to pain and risk of early osteoarthritis, this possibility seems to be quite well founded.
Indeed, according to Schulz et al. 11, obese children tend to produce greater peak angular displacement and displacement integrals at the hip, as well as at the foot, that could have a bearing on lower leg joint alignment and mechanics disturbances, when compared to non-obese children. Obese children also appear to exhibit a greater peak knee external rotation joint force reactions than non-obese children that could predispose to future knee joint damage.
Wills et al. 12 further suggest that the risk of knee osteoarthritis is likely to accumulate as a result of any persistent exposure to a high body mass through adulthood. Not much work has been done as to the role of childhood illness or joint disease on childhood obesity, but this association cannot be excluded on the basis of the prevailing largely cross-sectional data sets.
Interestingly, those factors cited to increase a child's risk of becoming overweight or incurring excessive weight gain, are very similar to those cited to heighten adult obesity risk, as well as osteoarthritis, and osteoarthritis severity. These include, but are not limited to: dietary influences, including the regular ingestion of high-calorie foods, fast foods, baked goods and vending machine snacks, soft drinks containing sugar, candy and desserts 1, 13, 14. Another is lack of exercise 14, 15. As per Le-Bourgeois et al. 16 the digital revolution, which is altering sleep and circadian rhythms across development (infancy to adulthood) can negatively impact weight status.
Fakeeh et al. 13 for example, found the prevalence of overweight and obesity was 10.1% and 12.4%, respectively, among the study participants in a Saudia Arabian school context. There was a significant difference in the overweight and obesity between urban and rural study population. Overweight and obesity was found higher among children who frequently ate junk food. The research reviewed by Morrissey et al. 17 showing a screen time link to obesity in youth, also noted that shorter sleep durations among children and adolescents that might accrue with excess use of media at bedtime that might lead to an energy deficit, and therefore to higher rates of energy/caloric dense food consumption, including candy, takeaway meals and sugar sweetened beverages.
However, many ongoing or proposed interventions for purposes of combating childhood obesity tend to focus exclusively on fostering behavioral changes such as increasing daily physical exercise or optimizing diet with little effect. Although effective methods of intervening are very necessary and urgent to apply, community-based / environment-oriented measures, plus the promotion of healthy food choices by taxing unhealthy foods, mandatory standards for meals in kindergarten and schools, increase of daily physical activity at kindergartens, and schools as well a ban on unhealthy food advertisement for children and other such approaches, are all presently on hold during the COVID-19 pandemic. At the same time, it is imperative to minimize the impact of the pandemic on obesity rates or any trend towards being moderately overweight before the start of puberty, which is associated with a significantly increased risk for type 2 diabetes and cardiovascular disease in midlife 18.
Social Media Usage
Social media are communication platforms enabling widespread messaging and interactions through a variety of communication channels (see Box 1). In terms of factors that have the potential to foster rather than decrease childhood obesity, the widespread daily use of one or more of these various forms of communication that involve little energy expenditure may prove more harmful than not or more harmful than anticipated. Indeed, as noted by Coates et al. 19 popular social media can impact as well as influence the promotion of foods that can affect children's food intake, as well as ‘bad eating habits’ especially if promoted by social media influencers. According to Coates et al. 19, the presence on social media of ‘influencer marketing’ strategies, aimed at glamorizing ‘unhealthy’ snacks and other foods, is highly potent, impactful, and often exploitive. Their study showed that food oriented marketing messages aimed at unhealthy foods, and received by youth, were strongly associated with an increase in children's immediate food intake, whereas the equivalent marketing of healthy foods had no effect.
Mazur et al. 20 who similarly found evidence of a strong link between obesity levels across European countries and childhood media exposure, implied that parents and society needed a far better understanding of the influence of social media on dietary habits than they have at present.
In support of this view, Tan et al. 21 found that as with television, unhealthy food ads predominate in content aimed toward children on YouTube. Kelly et al. 22 further confirmed that there is accumulating evidence that food marketing on new media, which is increasing, influences children's food preferences and choices. Moreover, the authors propose that the impact of integrated campaigns, which reinforce commercial messages across multiple platforms, and of new media, which often engage personally with potential consumers, is likely to be greater than that of traditional marketing.
Potvin Kent et al. 23 who studied 101 children and adolescents (ages 7-16 years) using a survey that examined their media use, and recorded their two favorite social media apps for 5 minutes to identify food marketing exposures showed 72% of participants were exposed to food marketing, and of the 215 food marketing exposures identified, most promoted unhealthy products such as fast food (44%) and sugar-sweetened beverages (9%). Adolescents viewed more instances of food marketing, on average, per 10-minute period compared with children, but it was still estimated that children and adolescents see food marketing 30 and 189 times on average per week on social media apps, respectively. The term food marketing was applied to food advertisements, celebrity-generated fod marketing, user-generated fod marketing, and food marketing embedded in other content, such as entertainment.
Robinson et al. 24 too have presented some current data to show that screen media exposure does tend to lead to obesity among children and adolescents through its impact on increased eating opportunities, for example, while viewing; exposure to high-calorie, low-nutrient food and beverage marketing that can influence children's food and beverage preferences, purchase requests, consumption habits; as well as reducing sleep duration and physical activity participation.
McKetta et al. 25 conclude that exposure to electronic screen media can powerfully influence the risk of childhood overweight/obesity, while social media exposure can also impact sleep, which can heighten obesity risk. It is possible images on social media, antisocial messages, bullying, and aspects of usage such as competing for ‘likes’ provokes immense stress, low self-esteem, and depression in its own right, that are possible precursors of obesity, regardless of age, as may disability and health challenges of various sorts. Morrissey et al. 17 conducted a study that highlighted how the usage of screen devices in bed and sugar sweetened beverages consumption behaviors might influence children’s weight status via the sleep-obesity nexus.
The American Academy of Pediatrics 26 states that the risks of such media include negative health effects on sleep, attention, and learning; a higher incidence of obesity and depression; exposure to inaccurate, inappropriate, or unsafe content and contacts; and compromised privacy and confidentiality. Many media users are found to be underage users, and may have limited ability to discern unhealthy social media messages from healthy messages due to their youth.
Foods marketed to youth via social media may be especially harmful in the long run, given their unhealthy oftentimes obesogenic promoting content, and highly pervasive presence. Indeed in a study by Potvin Kent et al. 23, this group located over 6000 adverts for unhealthy foods on one of five social media sites to prevail per year. Moreover, even if discounting the hours of usage that youth employ in this sedentary behavior mode, and its possible obesogenic impact, it was found that kids exposed to food marketing on their favourite social media apps are exposed 111 times a week on average, equating to 5772 food and beverage ads per annum on those five apps alone, the majority of which tended to promote “ultra-processed foods and beverages high in fat, salt or sugar” including fast food, sugar sweetened beverages, candy, and snacks 23.
Discussion
When considering the emergence of several non-communicable diseases that have an enormous economic and health impact, childhood obesity is noteworthy, especially due to its high potential to persist into adulthood with all its attendant health risks including cardiovascular diseases, type 2 diabetes, and osteoarthritis 7, 8, among many other negatively impactful health challenges.
At the same time efforts to prevent, reduce, or treat obesity are highly challenging and surely warrant insightful comprehensive immediate efforts given the added problems obesity is found to have on most major life threatening illnesses, as well as the 2020 COVID-19 infection rate and its severity. However, as outlined by Ludwig et al. 27 the prevalence of obesity failed to show any decreasing trend for any age group, rather the trend continued upward among many subgroups. Of particular concern was that previously documented racial and ethnic disparities, especially at the most extreme weight categories showed no sign of abating. Indeed, while obesity in children aged 5-19 years was relatively rare in 1975, it was much more common in 2016 7. In addition, class III obesity trends have now been shown to be two- to fourfold more prevalent among African American or Hispanic girls and boys compared to their white counterparts 27.
As argued by Ludwig et al. 27, the fundamental lesson here is that our public health approach to the childhood obesity epidemic has largely failed to this point. Indeed, a new study, based on life-course growth trajectories adjusted for secular trends through 2014, predicts that the majority of 2-year-olds today will be obese by age 35 years. Moreover, if current rates have not yet plateaued, as suggested by the NHANES 2015 and 2016 survey data, then even this bleak projection may be underestimating, rather than providing a valid data set concerning the magnitude of the problem. Also noted was that the obesity epidemic not only threatens to shorten life expectancy in the US and elsewhere, but to possibly bankrupt the US health care system. Yet progressive weight gain from one generation to the next is not inevitable according to Ludwig et al. 27. This group noted that indeed most children in the US have had access to abundant food since the end of the Great Depression and most have not been engaged in heavy physical labor, but that the generally stable obesity rates started to increase only during the 1980s.
The reasons for this increase have been discussed at length and include but are not limited to biological factors, poor diet quality, excessive sedentary time, inadequate physical activity, stress, sleep deprivation, perinatal factors, and probably environmental endocrine-disrupting chemicals. Unfortunately, what appears to be lacking is an effective strategy to address these drivers, and their determinants with sufficient intensity, consistency, and persistence, and across the school, home, health care personnel and community related situations. It especially does not appear to protect against the incessant exposure to manipulative food marketing through conventional media and, increasingly, the use of social media, such as Facebook, Instagram, Twitter, and other sites 27. Bozzolo et al. 55 cite alarming facts including the fact that not only do many adolescents feel the necessity to use a media device as a means to construct a social identity and express themselves, but for some children, smartphone ownership starts even sooner as young as 7 yrs, according to internet safety experts. This intense and pervasive usage may have negative influences not only on their psychophysical development, but also on sleep health, as well as obesity related physical and emotional problems.
At the same time, the severe impact of childhood obesity on multiple comorbid health conditions, including osteoarthritis and osteoarthritis risk factors, which has been succinctly highlighted 28, 29, 30, may be further compounded by the greater likelihood that youth who are already obese or overweight, may arguably be selecting social media as a recreational or stress relieving outlet, rather than other more active modes of recreation, if no restraints are placed on them. Youth may currently be suffering excess stress, a surfeit of highly processed foods, and boredom due to their inability to attend schools or partake in sporting and other active forms of exercise and self expression.
These aforementioned ideas arguably comport quite closely with the most salient mechanism offered to explain the increased overweight/obesity prevalence in youth as well as older persons, which is primarily increased food consumption due to both altered eating behaviors and exposure to advertising; plus sedentary activities, including screen viewing behaviors. In particular, digital marketing to young people is a specific factor highlighted by Boyland et al. 31 as a major contributor in this regard.
Jiminez-Marin et al. 32 report that there are now many studies that point to various media as a key contributing element to this growth in obesity rates in youth and possibly across the lifespan. In this sense, they argue that it should be noted that Spanish children are exposed to an average of 9000 television commercials per year and the vast majority of these are for food and beverage products of little or no nutritional value. It is possible social media use compounds this enormous exposure, and increases it, or emulates this, in order to maintain sales of unhealthy food products and soft drinks.
The American Academy of Pediatrics 26 implies furthermore that in contrast to some beneficial uses of media, negative health effects on weight and sleep; exposure to inaccurate, inappropriate, or unsafe content when viewed by children should be acknowledged. In this regard, moderators of the relationship between screen media use and overweight/obesity include context of use, family culture and socio economic status, gender, and sleep.
Kaur et al. 33 confirm that childhood screen-viewing time is now a primary means of entertainment, during their unstructured time, and at present, this time period is likely to be increasing markedly in light of the COVID-19 lockdown situations, recreational outlets and school closures. The additional use of social media for learning purposes does also not readily prevent young learners from sourcing websites that may portray negative food messages and others, even if apps are being developed to regulate children’s social media use.
As per Chassiokas et al. 34 early childhood is a crucial time for establishing healthy lifestyle behaviors and while parents play an important role in this regard, the factors influencing youth via social media usage require more broad policy interventions, among other approaches. The application of social media to intervene on reducing childhood obesity-and possibly requiring more screen time than not-also needs to be carefully examined.
In the meantime, while it is recognized that the key drivers of the childhood and adult obesity epidemic stem from an increasingly prevalent obesogenic environment, including, but not limited to: changing food systems and reduced physical activity 7, this broad view of the problem fails to explicitly account for social media screen time effects, as well as media messages that might foster harmful food choices, as well as eating practices in our view.
Media exposure by virtue of its influence on increased eating while viewing; exposure to high-calorie, low-nutrient food and beverage marketing that influences children's preferences, purchase requests, consumption habits; and reduced sleep duration are hence all potentially important issues to address 24.
In this regard, Karaagac 35 argue that the pervasive media environment and excess social media usage, is an immense social problem shared by most of the countries around the world, and where several studies have focused on the negative outcomes of excess time spent by children watching television, playing with computers or using mobile media devices, thus warranting strong concerns. Yet others have tried to explain the associations between the obesity, postural abnormalities or psychological problems of children, and their media use, and duly discussed approaches to curbing the negative influence of media on children, which currently must be considered as an increasing, rather than a decreasing trend.
However, the prevention of childhood overweight and obesity to some meaningful degree, by curtailing social media use and content has not truly been exploited to date. In this regard, parental education, along with policy interventions to control marketing of unhealthy foods and beverages, as well as an emphasis on the universal adoption of a more balanced lifestyle that could be applied to all children and adolescents, regardless of socioeconomic or lockdown status appears especially desirable. Jaul et al. 36 support this view by concluding that the adoption of healthy behaviors starting in early childhood can optimize quality of life among the oldest-old, including weight control, a major determinant of health in adult life 13.
Yet, uni-dimensional intervention approaches, such as labeling foods as harmful, or banning junk food sales to kids, as proposed in Mexico, can arguably still not begin to address a broader array of concerns about the origins of the stimuli that drive young people towards fast foods, sugary drinks, and a distaste for fruits and vegetables (https://time.com/5872175/boris-johnson-weight-loss-coronavirus/). Similarly apps to control viewing time and content by parents must be considered less than sufficient, especially if food advertising to children is not subject to censure. The role of loneliness, anxiety, boredom, and anger due to stressful childhood situations including on line bullying and body image glorification of extreme thinness might drive excess food ingestion and heightened sedentarity and their possible unique or collective negative social media effects on body weight gain should undoubtedly be explored intently and immediately. The ability of media to influence the very young child adversely has also not received due attention.
Conclusion
A review of the salient literature, provides a strong case for limiting social media use in childhood obesity prevention efforts in later life, as well as early life, especially in light of the increased risk of COVID-19 and adverse COVID-19 outcomes 37, 38, 39, plus many comorbid health conditions, such as osteoarthritis, a musculoskeletal condition that causes untold pain and misery to many older adults, as well as younger adults, and even youth, and can manifest over a period of 10 years in obese or overweight cases 49.
Unfortunately, ample evidence suggests that not only is childhood obesity a growing, and burgeoning concern, rather than a shrinking concern, but that the problem of childhood obesity is often addressed in ways that have no proven efficacy or that do not account for the nature of the role social media and social media influencers might play in fostering an obesogenic environment as well as obesogenic behaviors. Moreover, current programs do not appear to consider the adverse impact prolonged closures or delays in school re opening, plus access to school-based preventive strategies may be having currently, not in the future.
Insightful immediate public health and policy making actions are clearly desirable and strongly advocated in this regard as stressed by Kaur et al. 33. Moreover, in the face of a possible further period of enforced social isolation and home schooling, and the use of telemedicine rather than face to face counseling, it may be essential for clinicians to be highly proactive in helping parents to reduce the added risk of media influences on their child as far as them becoming overweight inadvertently.
At the same time, the present data support the view of the American Academy of Pediatrics 26 that further concludes that clinicians not only consider their young client’s developmental stages in order to individualize an appropriate for them, but they should simultaneously stress the importance of parents need to control media usage time, and to set boundaries for using these devices. Parental education about the impacts of social media screen time and content also appears very crucial in this regard. As well, the possible negative implications of using apps to help children to control weight, should be carefully evaluated and explained.
Additionally, as stressed by Nicolson et al. 42, in light of the challenges that prevail in efforts to avert the possible devastating effects of premature osteoarthritis, and other physical, as well as mental and social health concerns, depression, poorer perceived lower scores on health-related quality of life among a high percentage of young and older adults, resources to assist parents, especially those who are socially disadvantaged are strongly indicated.
On the other hand, a failure to focus on this potentially catastrophic high risk health issue, is bound to predictably yield an unwarranted high degree of emotional and behavioral disorders, low self-esteem, bullying, and stigma effects 44 that can be lifelong problems in the making among overweight children 46, 47, 48, 49, 50. Hence, a universal well-funded and organized carefully targeted holistic effort by families and clinicians along with national and local supportive policy efforts is especially advocated in highly recommended this regard 23, 43. In addition, effective counter marketing that promotes nutrition, healthful foods, or physical activity is indicated 45. A parental obligation to monitor their children’s media usage, while providing guidance for their safe use, along with the ability to just say ‘no’ appears warranted as well.
In particular, efforts to identify preventive intervention to counter childhood obesity approaches other than those using social media appear warranted 19, 48, as these have not proven universally effective, and could possibly increase, rather than decrease young people’s participation time in the social media environment, as well as issues such as decreased self-esteem, depression, poor body image, and well-being 51, weight bias, and shaming 52.
To tease out fact from fiction, as identified by Richards et al. 51 more research into social media effects from the earliest point in time across the lifespan, especially those related to body weight issues, is strongly advocated in efforts to develop efficacious preventive and successful aging interventions. As per Stanford et al. 52, to move forwards in this realm, more attention to conveying accurate messaging about obesity and the evidence-base supporting its negative health effects will also need to be forthcoming across a broad spectrum of society in efforts to stem the tide of possible unprecedented future suffering and adverse impact on the publics’ health that currently emanates from this chronic disease.
Verily, as documented by Coates et al. 19, it is concluded that without tighter restrictions on the digital marketing of unhealthy foods to children, as well as efforts to prohibit ‘vloggers’ from promoting unhealthy foods to vulnerable young people on social media, plus limitations on viewing time, home environmental modifications 54, and teaching kids to identify advertisements that are risk promoting, the upcoming generation is likely to suffer from early onset of one or more preventable disabling physical and mental health challenges, as well as COVID-19 risk and severity at unprecedented rates. Preschoolers are especially at risk for high rates of weight gain, and their parents as well these youth should be targeted preferentially as they are more prone to developing obesity at high rates 19.
Coda
Unrelenting social media use that greatly competes with physical activity participation appears well correlated with numerous interdependent adverse future health events such as poor diet, sedative behavior, obesity, reduced immunity, stunted growth, and multiple mental health issues 53, 54 that are hard to reverse at any age. At the same time, childhood obesity, already at epidemic levels, can not only lead to significant health issues in later life, but can profoundly affect children's prevailing physical, social, and emotional well-being, plus their self-concept and body image. academic performance and quality of life. It can predispose to the possible onset of non genetic co-morbid conditions such as metabolic, cardiovascular, orthopedic, neurological, hepatic, pulmonary, and renal disorders 58.
As such, and given the undue misery and hardship associated with excess body weight at any age, we would like to assert that much more must be done to make parents, caregivers, and clinicians themselves aware of the widespread phenomenon of media device use among young people, and its possible impact on obesity risk in childhood, as this form of media is potentially addictive and may produce highly irreversible physical, as well as adverse long-term consequences, such as the potential for diminished therapeutic and prophylactic treatments against COVID-19 with large significant increases in morbidity and mortality, and the comorbid diseases that predict COVID-19 risk, and lower life quality among both the young, as well as the older adult 55, 56, 57, 58. To avert the impact of the immense costs of an increasingly overweight society, a holistic interdisciplinary approach including parents, teachers, caregivers, marketers, ‘vloggers’, politicians, and clinicians, and that is not dependent solely on emerging data, is currently imperative and is strongly urged in this regard.
Funding
None
Acknowledgements
None
References
- 1.Lee E Y, Yoon K H.Epidemic obesity in children and adolescents: risk factors and prevention. , Front Med 12(6), 658-666.
- 2.Kumar S, Kelly A S. (2017) Review of childhood obesity: from epidemiology, etiology, and comorbidities to clinical assessment and treatment. Mayo Clin Proc. 92(2), 251-265.
- 3.Duran-Tauleria E, Rona R J, Chinn S. (1995) Factors associated with weight for height and skinfold thickness in British children. , JEpidemioland Community Health 49(5), 466-473.
- 4.Ogden C L, Carroll M D, Flegal K M. (2003) Epidemiologic trends in overweight and obesity. , EndocrinolMetabClin North 32(4), 741-760.
- 5.Xu S, Xue Y. (2016) Pediatric obesity: causes, symptoms, prevention and treatment. , ExpTherMed 11(1), 15-20.
- 6.Mahaffey R, Morrison S C, Bassett P. (2018) Biomechanical characteristics of lower limb gait waveforms: associations with body fat in children. , Gait Posture 61, 220-225.
- 7.M Di Cesare, Sorić M, Bovet P. (2019) The epidemiological burden of obesity in childhood: a worldwide epidemic requiring urgent action. , BMC Med 17(1), 212.
- 8.Deoke A, Hajare S, Saoji A. (2012) Prevalence of overweight in high school students with special reference to cardiovascular efficiency. , Glob J Health Sci 4(2), 147-152.
- 9.Antony B, Jones G, Venn A. (2015) Association between childhood overweight measures and adulthood knee pain, stiffness and dysfunction: a 25-year cohort study. , Ann Rheum 74(4), 711-717.
- 10.Bout-Tabaku S, Shults J, Zemel B S. (2015) Obesity is associated with greater valgus knee alignment in pubertal children, and higher body mass index is associated with greater variability in knee alignment in girls. , JRheumatol 42(1), 126-133.
- 11.Shultz S P, D'Hondt E, Fink P W. (2014) The effects of pediatric obesity on dynamic joint malalignment during gait. , ClinBiomech(Bristol, Avon) 29(7), 835-838.
- 12.Wills A K, Black S, Cooper R. (2012) Life course body mass index and risk of knee osteoarthritis at the age of 53 years: evidence from the 1946 British birth cohort study. Ann Rheum Dis. 71(5), 655-660.
- 13.Fakeeh M I, Shanawaz M, Azeez F K. (2019) Overweight and obesity among the boys of primary public schools of Baish City in Jazan Province, Saudi Arabia: a cross-sectional study. , Indian J Public Health 63(4), 330-333.
- 14.Dadaeva V A, Alexandrov A A, Drapkina O M. (2020) . Prevention of obesity in children and 2(1), 142-147.
- 15.Booth F W, Roberts C K, Laye M J.Lack of exercise is a major cause of chronic diseases. , ComprPhysiol 2(2), 1143-1211.
- 16.LeBourgeois M K, Hale L, Chang A M. (2017) Digital media and sleep in childhood and adolescence. , Pediatrics 140(2), 92-96.
- 17.Morrissey B, Allender S, Strugnell C. (2019) Dietary and activity factors influence poor sleep and the sleep-obesity nexus among children. , Int J Environ Res Public 16(10), 1778.
- 18.Weihrauch-Blüher S, Wiegand S. (2018) Risk factors and implications of childhood obesity. , CurrObesRep 7(4), 254-259.
- 19.Coates A E, Hardman C A, JCG Halford. (2019) Social media influencer marketing and children's food intake: a randomized trial. , Pediatrics 143(4), 2018-2554.
- 20.Mazur A, Caroli M, Radziewicz-Winnicki I. (2018) Reviewing and addressing the link between mass media and the increase in obesity among European children: the European Academy of Paediatrics (EAP) and The European Childhood Obesity Group (ECOG) consensus statement. , ActaPaediatr 107(4), 568-576.
- 21.Tan L, Ng S H, Omar A, Karupaiah T. (2018) What's on YouTube? A case study on food and beverage advertising in videos targeted at children on social media. , Child 14(5), 280-290.
- 22.Kelly B, Vandevijvere S, Freeman B. (2015) New media but same old tricks: food marketing to children in the digital age. , CurrObesRep 4(1), 37-45.
- 23.Potvin Kent M, Pauzé E, Roy E A. (2019) Children and adolescents' exposure to food and beverage marketing in social media apps. , PediatrObes 14(6), 1-9.
- 24.Robinson T N, Banda J A, Hale L. (2017) Screen media exposure and obesity in children and adolescents. , Pediatrics 140(2), 97-101.
- 25.McKetta S, Rich M. (2011) The fault, dear viewer, lies not in the screens, but in ourselves: relationships between screen media and childhood overweight/obesity. , PediatricClinics of North America 58(6), 1493-1508.
- 26. (2016) American Academy of Pediatrics media use in school-aged children and adolescentsPediatrics. 138(5), 1-6.
- 27.Ludwig D S. (2018) Epidemic childhood obesity: not yet the end of the beginning. , Pediatrics 141(3), 1-2.
- 29.Vingård E. (1991) Overweight predisposes to coxarthrosis. Body-mass index studied in 239 males with hip arthroplasty. , ActaOrthopScand 62(2), 106-109.
- 30.Petrilli C M, Jones S A, Yang J. (2020) Factors associated with hospitalization and critical illness among 4,103 patients with COVID‐19 disease in New York. , MedRxiv 1, 25.
- 31.Boyland E, Thivel D, Mazur A. (2020) Digital food marketing to young people: a substantial public health challenge.Ann Nutrition Metabolism. 76(1), 6-9.
- 32.Jiménez-Marín G, Zambrano R E, Galiano-Coronil A. (2020) Food and beverage advertising aimed at Spanish children issued through mobile devices: a study from a social marketing and happiness management perspective.Int J Environ Res Public Health. 17(14), 5056.
- 33.Kaur N, Gupta M, Malhi P. (2019) . Screen time in under-five children.IndianPediatrics.56(9): 773-788.
- 34.Reid Chassiakos Y, Radesky J, Christakis D. (2016) Children and adolescents and digital media. , Pediatrics.; 138(5), 1-18.
- 35.Karaagac A T. (2015) Undesirable effects of media on children: why limitation is necessary?. , IndianPediatrics 52(6), 469-471.
- 36.Jaul E, Barron J. (2017) Age-related diseases and clinical and public health implications for the 85 old and over population. Front Public Health. 5, 335.
- 37.Lighter J, Phillips M, Hochman S. (2020) Obesity in patients younger than 60 years is a risk factor for Covid-19 hospital admission.Clin Infect Dis. 71(15), 896-897.
- 38.Sattar N, McInnes I B, JJV McMurray. (2020) Obesity is a risk factor for severe Covid-19 infection: multiple potential mechanisms.Circulation. , Jul 142(1), 4-6.
- 39.Yang J, Hu J, Zhu C. (2020) Obesity aggravates COVID-19: a systematic review and meta-analysis.J MedVirol. 1-20.
- 40.Kessler J I, Jacobs JC Jr, Cannamela P C. (2018) Childhood obesity is associated with osteochondritis dissecans of the knee, ankle, and elbow in children and adolescents. , JPediatrOrthop 38(5), 296-299.
- 41.McCann M R, Ratneswaran A. (2019) The role of PPARγ in childhood obesity-induced fractures. Published , GenesNutr 14, 31.
- 42.Nicholson S, Dickman K, Maradiegue A. (2009) Reducing premature osteoarthritis in the adolescent through appropriate screening. , JPediatrNurs 24(1), 69-74.
- 43.Duran-Tauleria E, Rona R J, Chinn S. (1995) Factors associated with weight for height and skinfold thickness in British children. , JEepidemiologyand Community Health 49(5), 466-473.
- 44.Rankin J, Matthews L, Cobley S. (2016) Psychological consequences of childhood obesity: psychiatric comorbidity and prevention. AdolescHealth Med Ther.7:. 125-146.
- 45. (2013) Standing Committee on Childhood Obesity Prevention; Food and Nutrition Board; Institute of Medicine. Challenges and Opportunities for Change in Food Marketing to Children and Youth: Workshop Summary. Washington (DC): National Academies Press (US);.
- 46.Holliday K L, McWilliams D F, Maciewicz R A. (2011) Lifetime body mass index, other anthropometric measures of obesity and risk of knee or hip osteoarthritis in the GOAL case-control study. , Osteoarthritis Cartilage 19(1), 37-43.
- 47.Singer S P, Dammerer D, Krismer M. (2018) Maximum lifetime body mass index is the appropriate predictor of knee and hip osteoarthritis. , ArchOrthopTrauma Surg 138(1), 99-103.
- 48.Weihrauch-Blüher S, Koormann S, Brauchmann J. (2016) . Elektronische Medien in der Adipositas-Prävention bei Kindern und Jugendlichen [Electronic media in obesity prevention in childhood and adolescence].BundesgesundheitsblattGesundheitsforschungGesundheitsschutz 59(11), 1452-1464.
- 49.Manninen P, Riihimäki H, Heliövaara M. (1996) Overweight, gender and knee osteoarthritis. , Int JObesRelatMetabDisord 20(6), 595-597.
- 50.Cimmino M A, Scarpa R, Caporali R. (2013) Body mass and osteoarthritic pain: results from a study in general practice. , Clin ExpRheumatol 31(6), 843-849.
- 51.Richards D, Caldwell P H, Go H. (2015) Impact of social media on the health of children and young people. JPaediatrChild Health. 51(12), 1152-1157.
- 52.Stanford F C, Tauqeer Z, Kyle T K. (2018) Media and its influence on obesity. , CurrObesRep 7(2), 186-192.
- 53.Carter B, Rees P, Hale L. (2016) Association between portable screen-based media device access or use and sleep outcomes: a systematic review and meta-analysis. , JAMAPediatr 170(12), 1202-1208.
- 54.E de Jong, Visscher T L, HiraSing R A. (2013) Association between TV viewing, computer use and overweight, determinants and competing activities of screen time in 4- to 13-year-old children. , Int 37(1), 47-53.
- 55.Bozzola E, Spina G, Ruggiero M. (2019) Media use during adolescence: the recommendations of the Italian Pediatric Society. , Ital JPediatr 145(149), 1-9.
- 56.Hales C M, Carroll M D, Fryar C D. (2017) Prevalence of obesity among adults and youth: United States. , NCHS Data Brief 288, 1-8.
