Pyrexia And Liver Injury After A Second SARS-CoV-2 Vaccination: Macrophage Activation Manifested In Liver
Abstract
Vaccination against severe acute respiratory syndrome coronavirus 2 (SARS-Co V-2) has contributed to control of the coronavirus disease 2019 (COVID-19). On the other side, vaccination of SARS-CoV-2 could trigger autoimmune or inflammatory diseases. We present a 50-year-old female with well-controlled optic neuromyelitis with prednisolone (PSL) maintained at a dose of 2.5 mg/day. She ran a fever and liver injury was indicated 5 weeks after a second COVID-19 vaccination (BNT162b2 mRNA/Pfizer ). Liver biopsy showed accumulation of macrophages around the central veins, identified using anti-CD68 antibodies. As the treatment, cyclosporine A improved liver injury. COVID- 19 vaccination may have triggered liver inflammation due to cytokine storm via macrophage activation in the liver.
Author Contributions
Academic Editor: Sasho Stoleski, Institute of Occupational Health of R. MacedoniaWHO CC and Ga2len CC.
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2023 Tomiko Ryu, et al.
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Introduction
The world has faced the pandemic of COVID-19 since December 2019. As a countermeasure of SARS-CoV-2 infection, vaccines of different mechanisms have been approved. SARS-CoV-2 infection has been associated with the development of autoimmune process1, such as Guillain-Barre syndrome, systemic lupus erythematosus, autoimmune haemolytic anaemia, immune thrombocytopenic purpura, autoimmune thyroid disease and Kawasaki disease2. It is speculated that SARS-CoV-2 can disturb self-tolerance and trigger autoimmune response through cross-reactivity with host cells. There are also reports of immune diseases that develop after COVID-19 vaccination. COVID-19 vaccination could trigger auto-immunity, as same as other vaccines.
Recently, several cases of immune thrombocytopenic purpura (ITP) developing after COVID-19 vaccination 3 have been reported to the Vaccine Adverse Event
Reporting System. Autoimmune hepatitis (AIH) after COVID-19 vaccination is extremely rare. Until now, about 10 cases of AIH has been reported in the literature 4, 5, 6, 7, 8. Although the exact mechanism of autoimmune develop is unknown, molecular mimicry and bystander activation is a potential mechanism. In vitro study, Vojdani A et al. showed a molecular mimicry mechanism between the nucleoprotein/spike protein of SARS-CoV-2 and self-antigens 9.
Macrophage activation syndrome (MAS) is a severe, potentially life-threatening complication of autoimmune disease, viral infection and malignancy. It is a subset of hemophagocytic lympohistiocyto-sis (HLH). The excessive activation and proliferation of macrophages and T lymphocytes leads to inflammation via cytokine storm.
We present a case of pyrexia and liver injury after a second COVID-19 vaccination (BNT162b2 mRNA/Pfizer). Pathological findings of liver biopsy showed accumulation of macrophages around the central veins. As our case did not fill HLH-2004 diagnostic criteria, MAS was denied. Organ damage due to macrophage activation was only manifested in the liver. COVID-19 vaccination may cause a single organ inflammation as an abnormal immune response. Administration of cyclosporine A for immunosuppression was effective, and liver damage improved. As far as we could confirm, this is the first reported case.
Case Reports
A 50-year-old woman received a second COVID-19 vaccination (BNT162b2 mRNA/Pfizer) in March, 2021. She presented to our hospital with a 1-week history of pyrexia at night (5 weeks after mRNA COVID-19 vaccination). C-reactive protein (CRP) was 0.8mg/dL and COVID-19 polymerase chain reaction (PCR) was negative, however, elevated liver enzymes were indicated with aspartate aminotransferase (AST) 125 IU/L and alanine aminotransferase (ALT) 161 IU/L. She was admitted to our hospital in May. As her medical history, she was diagnosed as optic neuromyelitis when she was 32 years old. No recurrences had been noted in the past 7 to 8 years with prednisolone (PSL) maintained at a dose of 2.5 mg/day. She was also suspected as fatty liver at the age of 39 years old.
On admission, the body temperature was 36.7℃. Eruptions, articular symptoms, abnormal neurological findings including the visual field and ocular fundus were not observed. In blood examination, no abnormalities were indicated in blood cell counts (white blood cell count 6,960/μL, neutrophil 79.5%, hemoglobin 11.8 g/dL, platelet count 177,000/μL), coagulation and renal function, but liver enzymes revealed with AST, ALT, and r-GTP 188, 24, and 439, respectively. The patient had been previously suspected of fatty liver, and the baseline hepatic function for AST, ALT, and r-GTP were at 62, 102, and 80 IU/L, respectively. The examination for infections and autoimmune diseases conducted for differential diagnoses were negative (EBV and CMV past infection, CMV pp65 negative T-Spot.TB negative, rheumatoid factor negative, antinuclear antibody 80 × , antimitochondrial antibody negative, cytoplasmic and perinuclear-antineutrophil cytoplasmic antibody negative, IgG4 88.9 mg/dL). Increased ferritin and soluble interleukin-2 receptor (sIL-2 R) levels were noted at 1706 ng/mL and 1241 U/mL, respectively. Cerebrospinal fluid analysis showed no abnormalities. Magnetic resonance imaging (MRI)/magnetic resonance cholangio pancreatography (MRCP) revealed no particular abnormalities.
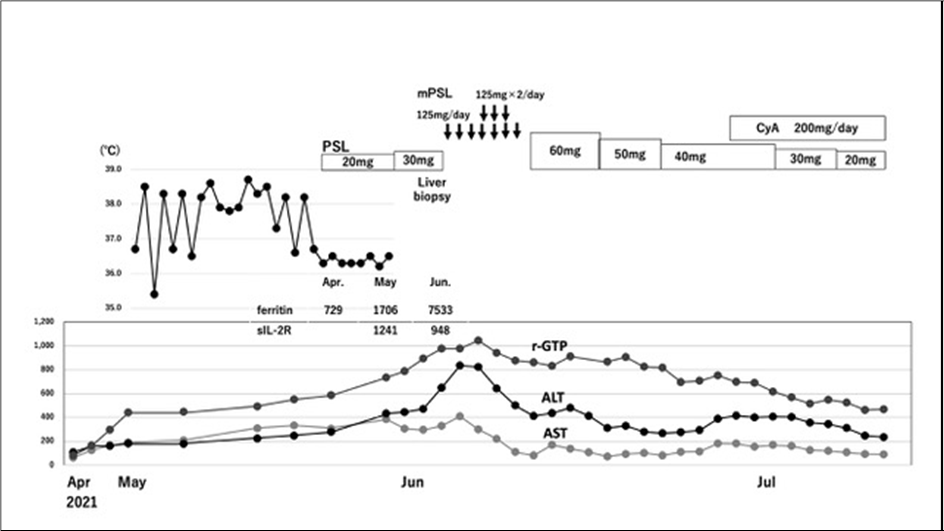
Following admission, the WBC count was stable with around 6000, and CRP ranged from 1 to 2 mg/dL, but the fever persisted intermittently. Increases in ferritin and sIL-2R indicated the involvement of activated macrophages and T-lymphocytes. As immunological abnormalities like cytokine storm were suggested, prednisolone (PSL) was initiated at 20mg/day to suppress immune reaction, and the fever resolved the following day. However, hepatic damage progressed. Subsequently, PSL was increased to 30 mg/day. The AST, ALT, and r-GTP levels increased to 409, 832, 1044, , respectively (Figure 1).
A liver biopsy was performed. The following day, ferritin increased considerably to 7533 ng/mL, while soluble IL-2 receptor was also high level of 948 U/mL. On the same day, semi-pulse therapy was initiated. The figure (Figure 2) shows the pathological findings of the liver tissue biopsy. (Figure 2A) shows a low-power field image of the HE-stained specimen showing sporadic concentrations of inflammatory cells, indicating focal necrosis. (Figure 2B) is a high-power field image showing concentrations of macrophages and lymphocytes. Denaturation of nuclei was observed in the surrounding hepatic cells. To confirm sites of focal necrosis, immunostaining was performed using anti-CK7 antibodies to identify biliary epithelial cells (Figure 2C). The sites of focal necrosis were negative for CK7 and were not portal regions. These findings were different from the viral hepatitis. Immunostaining was performed using anti-CD68 antibodies identified macrophages (Figure 2D). Accumulation of macrophages was observed around the central veins. No malignant findings were noted. When PSL was tapered off from 60 mg/day following semi-pulse therapy, reaggravation of liver function was noted at 40mg/day. To suppress inflammation, cyclosporine A (CyA) 200mg/day (3mg/Kg) was added. With the hepatic functions improving, the patient was discharged in July and followed up as out-patient. Thereafter, PSL was tapered until maintenance dose of PSL 2.5 mg/day in September with CyA being withdrawn in October. Ferritin and soluble IL-2R levels normalized. During follow-up, no eruptions, articular symptoms, or pancytopenia developed (Figure 3).
Figure 2.Pathological findings of the liver tissue biopsy. (A) Low-power field image of the HE-stained speci-men showing sporadic concentrations of inflammatory cells, indicating focal necrosis (HE 20×). (B)High-power field image showing concentrations of macrophages and lymphocytes. Denaturation of nuclei was ob-served in the surrounding hepatic cells (HE400×).(C)Immunostaining using anti-CK7 antibodies to identify biliary epithelial cells. The sites of focal necrosis were negative for CK7 and were not portal regions. (D)Immunostaining using anti-CD68 antibodies to identify macrophages. Accumulation of macrophages was ob-served around the central veins.
Discussion
We presented a rare case of pyrexia and liver injury following a second COVID-19 vaccination. Although reports of liver injury from COVID-19 vaccination are rare, AIH and HLH have been reported.
The first case of AIH after COVID-19 vaccination in the literature was presented by Bril F et al. in 2021 4. They reported a case of autoimmune hepatitis in which the patient developed itchiness, jaundice, and hepatic damage one week after COVID-19 vaccination. The liver biopsy findings included pan-lobular hepatitis and lobular inflammation, severe portal and periportal lymphocyte infiltration with plasma cells, periseptal interface hepatitis, spotty necrosis, and limiting plate disorder.
Afterward, the number of cases shared in the literature has increased up to about 11 cases. Avci E et al. reported a female case of AIH after COVID-19 vaccine 7. She had Hashimoto’s thyroiditis. Lessard EV et al. reported a case of a 76-year-old woman with Hashimoto thyroiditis and prior COVID-19 infection who developed severe autoimmune hepatitis following COVID-19 vaccination (mRNA-1273, Moderna). Caution may be warranted when vaccinating individuals with known autoimmune diseases. Cumali E et al. evaluated clinical features, treatment response and outcomes of liver injury following COVID-19 vaccination in a large case series, including 87 patients from 18 countries 10. Liver injury was diagnosed a medium 15 days after vaccination. 51 cases (59%) were attributed to the BNT162b2 mRNA/Pfizer vaccine, 20 cases (23%) to the Oxford-Astra Zeneca (ChAdOX1 nCoV-19) vaccine and 16 cases (18%) to the Moderna (mRNA-1273) vaccine. The liver injury was predominantly hepatocellular (84%) and 57% of patients showed features of immune-mediated hepatitis. Corticosteroids were given more often for patients with than without immune-mediated hepatitis. All patients showed resolution of liver injury except for one man who developed liver failure.
Our case had optic neuromyelitis maintained with PSL at a dose of 2.5 mg/day. AIH was denied accord-ing to blood examination and pathological findings of liver biopsy. Muench F et al. reported a first case of adult-onset Still’s disease (AOSD) who developed macrophage activation syndrome (MAS) after SARS-CoV-2 vaccination with BNT162b2 mRNA/Pfizer 11. MAS is a complication of AOSD with high mortality rate. However, the occurrence of MAS after vaccination is extremely rare and has been described in a few cases after measles or influenza vaccinations and more recently after COVID-19 vaccination.
Hieber ML et al. reported a 24-year-old female who developed HLH after immunization with COVID-19 vaccine, BNT162b2 mRNA/Pfizer 12. Diagnosis was made according to HLH-2004 criteria. In 16 cases of post-vaccine HLH in a literature search, the meantime from vaccination to symptom onset was 7.4 days. In our case, the time from a second COVID-19 vaccination to symptom onset was 5 weeks. The reasons for the longer time to symptom onset were thought to be the immunosuppressive effect of PSL, which the patient was taking for optic neuromyelitis.
A detailed etiology of hepatopathy caused by MAS following COVID-19 vaccination has not been elucidated. SARS-CoV-2 spike proteins were possibly produced following the vaccination, which induced humoral and cellular immunity. These spike proteins and other analogs within the body might have further induced abnormal or excessive immune reactions, thereby activating macrophages and causing hepatopathy. COVID-19 vaccine also might have induced Th1 cell activation, which in turn prompted the secretion of cytokines, such as IFN-γ and IL-2. Consequently, the activated macrophages and the ensuing inflammatory reactions triggered hepatopathy 13.
Given the risks of autoimmune and inflammatory diseases caused by vaccination, careful consideration of administering vaccination is essential, for patients with autoimmune diseases. An early diagnosis and prompt initial treatment are very important for favorable outcome.
Conclusions
Macrophage activation should be included in the differential diagnosis in cases of liver injury of unexplained etilogy secondary to COVID-19 vaccination. COVID-19 vaccination may cause a single organ inflammation as an abnormal immune response, especially in patients with autoimmune diseases. Administration of cyclosporine A for immunosuppression was effective, and liver damage improved. Understanding of the involved mechanisms helps to prevent the incidence or exacerbation of autoimmune manifestations and choose the appropriate treatment.
References
- 2.Yu L, Amr H S, Qianjin L. (2022) COVID-19 and autoimmune diseases:. , Cur Opin Rheumatol 33, 155-162.
- 3.Eun-Ju L, Douglas B C, Terry G, Craig K, Marc M. (2021) Thrombocytopenia following Pfizer and moderna SARS-CoV-2 vaccination. , Am J Hematol. Feb 19, 534-537.
- 4.Bril F, Diffalha S, Dean M.Fettig DM.(2021) Autoimmune hepatitis developing after coronavirus disease 2019 (COVID-19) vaccine: Causality or casualty?. , J Hepatol 75(5), 1248-1249.
- 5.Maria C L, Jordi G G, Joaquin S P. (2021) Another case of autoimmune hepatitis after SARS-CoV-2 vaccination. Still casualty?. , J Hepatol 75, 1248-1249.
- 6.Elise V L, Matteo M, Jaume B, Nasser S. (2021) Autoimmune hepatitis triggered by SARS-CoV-2 vaccination. , J. Autoimmune 123.
- 7.Enver A, Fatma A. (2021) Autoimmune hepatitis after SARS-CoV-2 vaccine: New-onset or flare-up?. , J. Autoimmunity 125.
- 8.Chin Kimg T, Yu Jun W, Lai Mun W, Tiing Leong A, Rahul K. (2021) Autoimmune hepatitis following COVID-19 vaccination: true causality or mere association?. , J Hepatol 75(5), 1250-1252.
- 9.Vojdani A, Kharrazian D. (2020) Potential antigenic cross-reactivity between SARS-CoV- 2 and human tissue with a possible link to an increase in autoimmune disease. Clin Immunol. 217.
- 10.Cumali E, V K Anand, TBP Benedetta, Bianca M, Albert S. (2022) Liver injury after SARS-CoV-2 vaccination: Features of immune-mediated hepatitis, role of corticosteroid therapy and outcome. , Hepatology 76(6), 1576-1586.
- 11.Frederic M, Martin K, Leif E S, Thomas R, Gerd-RB. (2021) Macrophage activating syn-drome in a patient with adult-onset Still’s disease following first COVID-19 vaccination with BNT162b2. , BMC Rheumatology 5(1), 60-63.