Infection Prevention and Control in Healthcare Facilities During the Covid-19 Pandemic in Ghana
Abstract
Background
Infection prevention and control system in healthcare facilities is essential in dealing with the spread of infectious diseases, especially during an outbreak period such as the COVID-19 pandemic.
Objectives
The study assessed the infection prevention and control (IPC) situation in selected healthcare facilities in the Greater Accra and Ashanti Regions of Ghana during the Covid-19 pandemic.
Methods
This was a multi-facility based cross-sectional study that used a monitoring tool of the Health Facilities Regulatory Agency (HeFRA) of Ghana to collect information on the IPC practices at the peak of the Covid-19 pandemic. Data was gathered from 501 healthcare facilities in the Greater Accra (335) and Ashanti (151) Regions. Descriptive, Chi-square, and multiple logistic regression were performed. All statistical analyses were considered significant at an alpha level of 0.05.
Results
50.6% of health facilities were assessed as having good IPC systems in the overall assessment. The majority of the health facilities were evaluated as good on governance/leadership. Similarly, the majority (54.3 %)of the facilities had effective infectious waste management. The assessment levels of governance/leadership, management, quality assurance system, human resource, IPC equipment, and water management were all significantly associated with the adherence to good IPC systems.
Conclusion
IPC systems in most facilities were assessed as good, but some areas require critical attention to help prevent the spread of infections in healthcare facilities in Ghana. Support systems such as revised policy on IPC, governance/leadership, and infectious waste management infrastructure are needed to strengthen facilities with weak or poor IPC systems.
Author Contributions
Academic Editor: Jigar Modi, Postdoctoral Fellow, Neuroscience, Florida Atlantic University.
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2021 Philip Ababio Bannor, et al.
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Introduction
Ghana has seen a steady increase in COVID-19 cases following the detection of the first two COVID-19 cases on March 12, 2020. According to the Ghana Health Service (GHS) COVID-19 situation update, as of April 5, 2021, Ghana had 1386 active cases among 91,109 cumulative confirmed cases and 752 cumulative deaths 1, 2, 3 (Figure 1a & 1b)
Figure 1a.Regional distribution of Covid-19 active cases in Ghana, 27 July, 2020. b. Regional distribution of Covid-19 total cases in Ghana by 27 July, 2021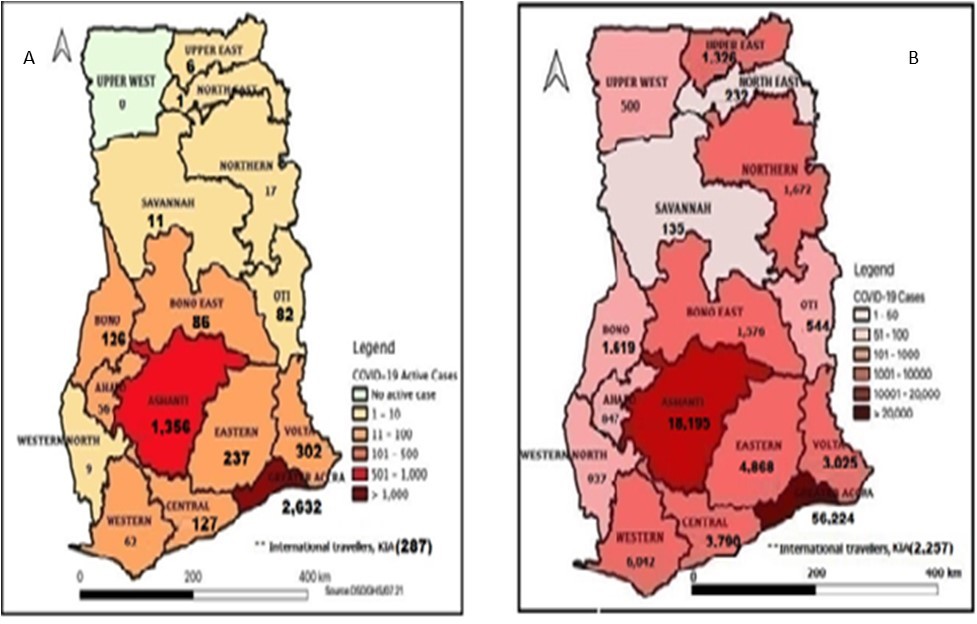
Globally, various precautionary measures have been put in place to help reduce the spread of the infection. These include frequent hand hygiene practices, social or physical distancing, the use of a nose mask, and social etiquettes such as avoiding handshakes and unnecessary touching of surfaces 4. Ghana implemented additional measures such as partial lockdown of some regions in the country (March 2020), closure of borders (air, land, and seaports), halting of public gatherings (i.e., religious activities, funerals, weddings, sporting events, restaurants, night clubs, and beaches). Also, fumigation of public places (such as community/farmers markets and public transit areas). Other measures included mass testing through contact tracing of targeted groups (in April 2020), quarantine, and isolation of suspected exposure and confirmed cases. In its quest to manage COVID-19, the Government of Ghana delivered six hundred thousand (600,000) doses of the AstraZeneca vaccine, the first consignment of many more to come, to vaccinate the populace.
The major challenge in this situation is appropriately managing the health facilities so that they do not become sources of infection or re-infection of COVID-19. Suppose the infection prevention and control system of the facilities are not robust enough. In that case, surfaces and materials in the health facilities may be contaminated, presenting a risk of infecting people who may contact these surfaces and materials within the health facilities 5 Hospital-based infections acquired during health delivery could be transmitted from the health worker to patients through contaminated equipment, surfaces, bed liners, and air droplets. Covid-19 has a varying lifespan ranging from 4 hours on copper surfaces, 24 hours on cardboards, 2-3 days on stainless steel materials, three days on plastics and sewage, and three to four days on fecal waste 6, 7, 8 Implementing a robust infection prevention and control system is essential as part of the nationwide fight against COVID-19 to prevent further infections in Ghana and safeguard people's lives and the environment.
Ghana has a national policy and guidelines for infection prevention and control in a health care setting 9, 10 The IPC policy aims to direct healthcare workers and clients on the prevention and control of hospital-acquired infection to protect health workers while ensuring the safety of patients. The policy outlines that blood, body fluids, secretions, excretion, non-intact skin, and mucous membranes may contain transmissible infectious agents. The policy proposes preventive measures such as hand washing and appropriate PPEs to reduce exposure to microorganisms and manage sharps as effective ways of infection control.
Several researchers have reported on the impact of Covid 19 on infection prevention and control 12 water, sanitation, and hygiene (WASH) 13, 14 and medical waste management 15, 16, 17, 18 While most of these researches were conducted in advanced economies, only limited studies 19, 20, 21 have assessed medical waste management during Covid 19 in sub-Sahara Africa. In Ghana, limited studies have reported Covid-19 and WASH, IPC, and healthcare waste management 22, 23, 24, 25.
In the era of this pandemic, health facilities are the central point of seeking health care, thus making this sector a potential epicenter for the spread of the Covid-19 virus if stringent measures, based on accurate data, are not implemented and enforced. Yet, the data needed to clarify the extent to which organizational systems (governance/leadership) affect IPC and healthcare waste management in the era of Covid-19 is challenging to access in Ghana at the moment. The above observation is due to insufficient publication data on findings after monitoring and data collection from health facilities by researchers and organizations.
Therefore, this paper seeks to fill the information gap by assessing the Governance and IPC from healthcare facilities in the Greater Accra and Ashanti Regions of Ghana in the COVID-19 era. These two regions are the epicenters of the pandemic in Ghana, with the Greater Accra Region recording 56,224 cumulative cases. At the same time, the Ashanti region has also recorded 18,195 patients so far as of July 27, 2021 2 as shown in Figure 1a and 1b. (Figures)
Methodology
Study Design
This multi-facility-based cross-sectional study used quantitative methods to collect data from health facilities using the Heath Facilities and Regulatory Agency (HeFRA) IPC and HCWM monitoring tool for Covid-19 from May 19 to August 13, 2020.
Study Population
This study was conducted in 501 health facilities in the Greater Accra and Ashanti Regions of Ghana; however, 486 facilities were considered for this analysis due to incomplete data. The two regions were selected for monitoring since they were the epicenters of Covid-19 in Ghana, accounting for over eighty percent (80%) of all cases between May and August 2020. Currently, the two regions are still the epicenter of the disease in Ghana as indicated in Figure 1a and 1b.
Inclusion and Exclusion Criteria
All health facilities designated by the Ghana Health Service to manage covid-19 patients in Greater Accra and Ashanti regions were included. Additionally, health facilities that have been registered by HeFRA or GHS providers in the locked-down referenced areas were also included. However, health facilities registered by HeFRA or GHS providers but not part of the locked-down areas were excluded.
Data Collection Instrument
A Health Facilities Monitoring Tool (HeFMT) developed by Health Facilities Regulatory Agency (HeFRA)- Ghana was modified to include the Governance and management, infrastructure and safety, sanitation, infection prevention, and control, water management, and healthcare waste management component of the Water, Sanitation for Health Facilities Improvement Tool (WASH-FIT) 26 was used to assess the Infection Prevention and Control (IPC) practices at the 501 selected health facilities. HeFRA has used the HeFMT for monitoring health facilities to ensure they operate within the law. The tool is divided into seven main components. These include background information of the health facility, organizational system, infrastructure, assets, signages, IPC, and HCWM.
The HeFMT was measured on a scale where 0 represent 'No' and one represents 'Yes' for two-level responses. Also, a scale of 0 representing 'non-available, 1 representing 'in-complete/fail (1%-49%)' 2 representing 'partially complete/pass (50%-99%)' and 3 representing 'complete (100%)' was used for four-level responses. The actual scores in each section were summed up and divided by Total Expected Score in a formula.
The percentage scored was obtained by multiplying the R by 100. The overall grade depended on the total percentage score and was categorized into groups as indicated in Table 1.
Table 1. Percentage Score and Categorisation Scheme| Percentage Scored (%) | Grade | Interpretation | |
| 1. | 90-100 | A | Excellent |
| 2. | 80-89 | B | Very Good |
| 3. | 70-79 | C | Good |
| 4. | 50-69 | D | Pass |
| 5. | <50 | E | Fail |
Data Collection Procedure
A team of fifteen (15) experts from HeFRA, two (2) Accra School of Hygiene, and one (1) United Nations Development Program (UNDP) Ghana was used for the monitoring and data collection. A list of all health facilities in the Greater Accra and Ashanti Regions was accessed from HeFRA and MoH. The list of health facilities was categorized into hospitals, polyclinics, clinics, health centers, maternity homes, diagnostic centers, medical laboratories, specialist clinics, and Community-based Health Planning and Services (CHPS) compounds. The purposive sampling technique was used to gather information with the aid of the HeFMT. These facilities were selected for the monitoring as they were likely to have asymptomatic patients visiting. During the visitation to health facilities, interviews with health facilities proprietors, managing employees, in-charge personnel were used to gather information on IPC and Governance with the aid of HeFMT.
Variables of Interest
Dependent Variables
Infection prevention and control: focuses on the availability of guidelines/policy for infection control, hand washing protocols at all service areas, disinfection practices, personnel protective equipment and sterilization system, knowledge on decontamination of soiled linens, posters on the appropriate use of toilet facilities displayed, and cleaning schedule available in all areas.
The Independent Variables in the Study were:
Organizational System
Advisory boards, strategic plans, management teams, human resource development, policies, guidelines or protocols/standard operating procedures, acute and emergency care protocols, qualified clinical staff per unit, support staff, and capacity development.
Infrastructure
Fair distribution of sinks, Veronica buckets with running water, carbolic soap, incinerators, placenta pits, labeled sharp boxes, and sterilizers.
Assets
Asset registry, planned preventive maintenance schedules, evidence of insurance, power supply systems, water supply systems, and running water at all service areas.
Signages
Block plan of the facility, labeling of departments and units, directional signs, emergency exits, and emergency assembling points or bays.
Statistical Analysis
Treatment of Missing Variables
Health facilities with missing an entire domain of the assessment tools were excluded from the analysis. Health facilities with at least one but not all items under a domain missing had an average score of the non-missing items used for the missing observation(s) in that domain.
The assessment percentage scores for the IPC were computed as the average score of the domain expressed as a percentage of 3. Thus:
The percentage scores for each domain were further categorized into three levels. Facilities with percentage scores below 50% were classified as poor, 50% to 69.9% as moderate, and 70.0% and above were categorized as good.
Data Analysis
The characteristics of health facilities in the study were described using percentages and frequencies. The bar chart was used to describe the percentages of health facilities based on their scorings from the individual items under IPC, the overall assessment levels of the IPC, the Organizational system, Infrastructure, Safety, Assets, and Signage assessment levels. The Pearson's chi-square test was used to assess the association between health facility characteristics and IPC systems. The Pearson's chi-square test was also used to determine the association between organizational systems, infrastructure, safety, assets, signage assessment levels, IPC systems.
The three IPC assessment levels were then dichotomized such that good and moderate assessment levels were combined against poor assessment levels. The crude and adjusted odds ratio of poor IPC assessment levels were then estimated using the binary logistic regression models. The 95% confidence interval and the corresponding p-values of all odds ratios were also calculated. All statistical analyses were considered significant at a p-value less than 0.05
Results
Descriptive Characteristics of Health Facilities in the Study
Out of a total of 501 health facilities initially identified for the study, 486 were included in the final analysis of the survey, thus representing a 97% response rate. Fifteen (15) of the sampled facilities were not included in the final analysis due to non-responses from the facilities and incomplete information. The inclusion of such data would have skewed the data analysis/output. More than two-thirds of the health facilities were in the Greater Accra (68.9%) and the remaining in the Ashanti region (31.1%). The majority of the health facilities were privately owned (87.2%), with 12.8% publicly owned. Over a third of the health facilities were health centers or clinics (36.2%), 32.1% were hospitals, 14.4% medical centers, 6.4% were maternity homes, 4.1% were diagnostic or laboratory facilities, 3.1% were specialist facilities, 2.5% were polyclinics, and 1.2% were CHPS compounds (Table 2).
Table 2. Descriptive characteristics of health facilities in the study| Characteristics | Frequency (N=486) | Percent |
| Region | ||
| Greater Accra | 335 | 68.9 |
| Ashanti | 151 | 31.1 |
| Ownership of facility | ||
| Private | 424 | 87.2 |
| Public | 62 | 12.8 |
| Type of facility | ||
| CHPS compounds | 6 | 1.2 |
| Diagnostic/laboratories | 20 | 4.1 |
| Health centres/Clinics | 176 | 36.2 |
| Hospitals | 156 | 32.1 |
| Maternity homes | 31 | 6.4 |
| Medical centres | 70 | 14.4 |
| Poly clinics | 12 | 2.5 |
| Specialist facilities | 15 | 3.1 |
Assessment of Health Facility on Infection Prevention and Control (IPC)
The majority of the health facilities were assessed highly (score of 3) for sterilization system (66.5%), knowledge on decontamination of instruments (60.5%), hand washing basin/veronica bucket with elbow tap (58.4%), personnel protective equipment (54.9%) and disinfection practices (52.5%). More than a fifth of the health facilities were also assessed lowly (score of 0) for handwashing protocol (21.6%), posters on appropriate handwashing technique displayed (25.7%), IPC/ WASH focal person (27.6%), and guidelines or policy for infection control (37.0%). More than a tenth of the facilities were assessed with a score of 1 on knowledge on decontamination of soiled linens (13.2%), display of posters on appropriate handwashing technique (13.6%), handwashing protocol (12.8%) and guidelines or policy for infection control (11.7%). Also, more than a third of the facilities were assessed with a score of 2 for display of posters on appropriate handwashing technique (34.0%), having protocol and procedures for prevention of spread of infectious disease (37.7%), and on personnel protective equipment (33.3%) (Figure 2).
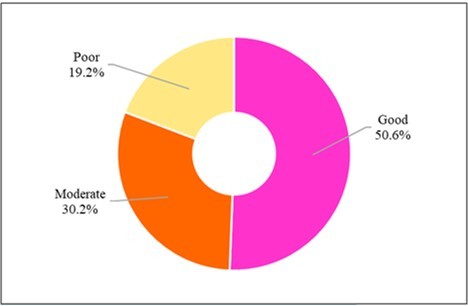
In the overall assessment level of health facilities on IPC, half of the health facilities were assessed as having a good IPC system (50.6%), 30.2% as having a moderate IPC system, and 19.1% poor IPC system (Figure 3).
Figure 2.Assessment of health facility on Infection prevention and control (IPC)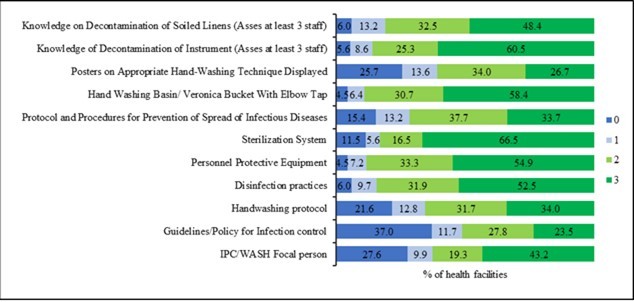
The Organizational System, Infrastructure, Safety, Assets, and Signage Assessment of Health Facility in the Study
Table 3 shows the assessments of health facilities on the individual items under the various domains of governance/ leadership, management, quality assurance systems, human resources, infection prevention control equipment, assets, signage, and water management.
Table 3. Assessment of IPC System in Health Facilities| Assessment Score | ||||
| Domains and items | 0 | 1 | 2 | 3 |
| n (%) | n (%) | n (%) | n (%) | |
| Governance / Leadership | ||||
| Advisory Board | 121 (24.9) | 27 (5.6) | 96 (19.7) | 242 (49.8) |
| Vision | 61 (12.6) | 24 (4.9) | 52 (10.7) | 349 (71.8) |
| Mission | 61 (12.6) | 24 (4.9) | 51 (10.5) | 350 (72.0) |
| Strategic Plan | 97 (20.0) | 34 (7.0) | 151 (31.1) | 204 (42.0) |
| Management | ||||
| Management team | 41 (8.4) | 18 (3.7) | 81 (16.7) | 346 (71.2) |
| Human Resource Development | 59 (12.1) | 36 (7.4) | 154 (31.7) | 237 (48.8) |
| Policies | 81 (16.7) | 40 (8.2) | 169 (34.8) | 196 (40.3) |
| Guidelines /Protocols/SOPs | 73 (15.0) | 44 (9.1) | 158 (32.5) | 211 (43.4) |
| Quality Assurance System | ||||
| Policies/Guidelines and Protocols | 83 (17.1) | 36 (7.4) | 171 (35.2) | 196 (40.3) |
| Client Satisfaction | 143 (29.4) | 28 (5.8) | 105 (21.6) | 210 (43.2) |
| Infection Prevention/Control | 129 (26.5) | 58 (11.9) | 157 (32.3) | 142 (29.2) |
| Acute/ Emergency Care Protocol | 125 (25.7) | 68 (14.0) | 160 (32.9) | 133 (27.4) |
| Human Resource | ||||
| Practitioner-in-charge | 24 (4.9) | 5 (1.0) | 35 (7.2) | 422 (86.8) |
| Qualified Clinical staff per unit | 18 (3.7) | 11 (2.3) | 54 (11.1) | 403 (82.9) |
| Support staff | 18 (3.7) | 17 (3.5) | 50 (10.3) | 401 (82.5) |
| Capacity development | 55 (11.3) | 21 (4.3) | 135 (27.8) | 275 (56.6) |
| IPC Equipment | ||||
| Fair Distribution of Sinks/Veronica Buckets with Running Water | 18 (3.7) | 19 (3.9) | 176 (36.2) | 273 (56.2) |
| Incinerators/Placenta Pit | 147 (30.2) | 23 (4.7) | 79 (16.3) | 237 (48.8) |
| Well Labelled Sharp Boxes | 35 (7.2) | 35 (7.2) | 133 (27.4) | 283 (58.2) |
| Sterilizers/Autoclave | 67 (13.8) | 10 (2.1) | 53 (10.9) | 356 (73.3) |
| Assets | ||||
| Assets Registry | 62 (12.8) | 21 (4.3) | 125 (25.7) | 278 (57.2) |
| Planned Preventive Maintenance Schedule | 118 (24.3) | 56 (11.5) | 168 (34.6) | 144 (29.6) |
| Evidence of Insurance | 176 (36.2) | 24 (4.9) | 86 (17.7) | 200 (41.2) |
| Power Supply System | 21 (4.3) | 13 (2.7) | 37 (7.6) | 415 (85.4) |
| Water Supply System/running water at all Service Areas | 18 (3.7) | 6 (1.2) | 27 (5.6) | 435 (89.5) |
| Signage | ||||
| Block Plan of Facility | 281 (57.8) | 13 (2.7) | 30 (6.2) | 162 (33.3) |
| Labelling of Departments and Units | 44 (9.1) | 8 (1.6) | 66 (13.6) | 368 (75.7) |
| Directional Signs | 117 (24.1) | 35 (7.2) | 97 (20.0) | 237 (48.8) |
| Emergency Exit | 88 (18.1) | 15 (3.1) | 78 (16.0) | 305 (62.8) |
| Emergency Assembling Point | 152 (31.3) | 35 (7.2) | 82 (16.9) | 217 (44.7) |
| Water Management | ||||
| Easy to open taps | 42 (8.6) | 12 (2.5) | 114 (23.5) | 318 (65.4) |
| Flowing water | 19 (3.9) | 2 (0.4) | 36 (7.4) | 429 (88.3) |
| Back up water supply | 23 (4.7) | 11 (2.3) | 30 (6.2) | 422 (86.8) |
In the overall assessment of health facilities on Governance or leadership, 65.6% were assessed good, 16.7% moderately, and 17.7% were evaluated poorly. For the comprehensive evaluation of health facilities on management, 62.8% were evaluated good, 20.2% were assessed moderately, and 17.1% were evaluated poorly. For the quality assurance system, 42.8% were evaluated as good, 24.5% moderately, and 32.7% poorly. For the human resource assessment, 88.1% were good, 6.6% were moderate, and 5.3% were poor. For IPC equipment, 67.5% were assessed good, 21.4% moderately, and 11.1% poorly. For assets, 64.6% of the facilities were considered good, 23.0% assessed moderately, and 12.3% assessed poorly. For signage, 49.2% were evaluated as good, 21.6% were evaluated moderately, and 29.2% were evaluated poorly. However, 84.2% were assessed as good for water management, 11.3% were evaluated moderately, and 4.5% were assessed poorly (Figure 4).
Figure 4.Assessment levels of organizational, infrastructure, safety, assets, and signage systems of health facilities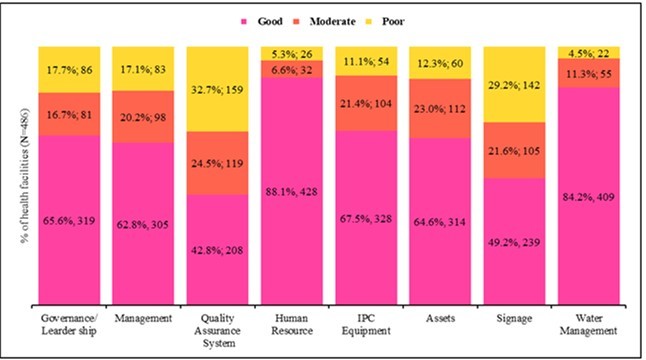
Factors Associated with IPC Assessment Levels
Among the 335 health facilities from the Greater Accra region, 50.7% had a good assessment on IPC, 26.0% were assessed moderately, and 23.3% were evaluated poorly. And among the 151 health facilities from the Ashanti region, 50.3% were evaluated good on IPC, 39.7% were assessed moderately, and 9.9% were poorly evaluated. There was a significant association between the region of location of the health facility and the assessment level on IPC (χ2=11.98, p=0.001). Among the 424 privately owned facilities in the study, 48.3% had good IPC assessment levels, 30.7% had moderate assessment levels, and 21.0% had poor. And among the 62 publicly owned facilities, 66.1% had good IPC assessment levels, 27.4% had moderate assessment levels, and 6.5% had poor assessment levels. The ownership type of health facilities was significantly associated with the IPC assessment level (χ2=9.54, p=0.008). The facility type was also significantly associated with the assessment level of IPC (χ2=69.48, p<0.001). For hospitals, 62.2%, 30.1%, and 7.7% were assessed as good, moderate, and poor, respectively, on IPC parameters. For health centers/clinics, 45.5%, 31.8%, and 22.7% were assessed as good, moderate, and poor, respectively, on IPC parameters. For diagnostic and laboratories, 5%, 30%, and 65% were assessed as good, moderate, and poor, respectively, on IPC parameters (Table 4).
Figure 5. describes the distribution of the IPC assessment levels within the various levels of organizational, infrastructure, safety, assets, and signage assessments. The assessment levels of governance/ leadership (χ2=84.14, p<0.001), management (χ2=71.31, p<0.001), quality assurance system (χ2=70.62, p<0.001), human resource (χ2=44.60, p<0.001), IPC equipment (χ2=78.29, p<0.001), assets (χ2=71.68, p<0.001), signage (χ2=64.64, p<0.001) and water management (χ2=36.03, p<0.001) were all significantly associated with IPC assessment levels.
Figure 5.Distribution of IPC assessment levels across organizational system, infrastructure, safety, assets, and signage assessment levels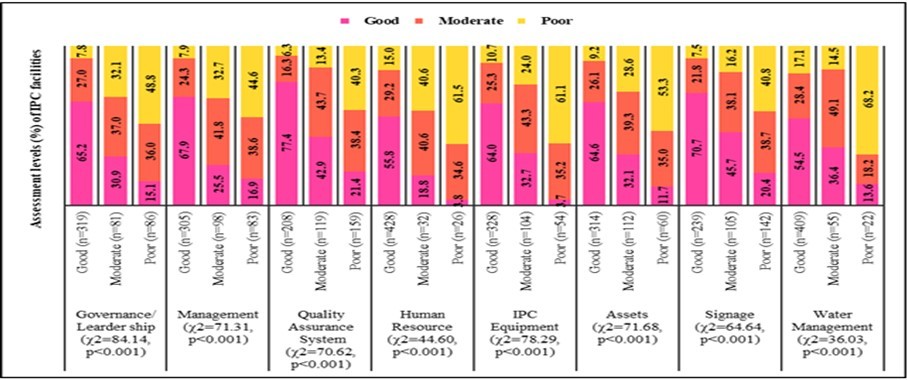
| Infection Prevention & Control Assessment levels | ||||||
| Factor | N | Good | Moderate | Poor | χ2-value | P-value |
| N | 486 | 246 | 147 | 93 | ||
| Region | 11.98 | 0.001 | ||||
| Greater Accra | 335 | 170 (50.7) | 87 (26.0) | 78 (23.3) | ||
| Ashanti | 151 | 76 (50.3) | 60 (39.7) | 15 (9.9) | ||
| Ownership of facility | 9.54 | 0.008 | ||||
| Private | 424 | 205 (48.3) | 130 (30.7) | 89 (21.0) | ||
| Public | 62 | 41 (66.1) | 17 (27.4) | 4 (6.5) | ||
| Facility type | 69.48 | <0.001 | ||||
| CHPS compound | 6 | 1 (16.7) | 3 (50.0) | 2 (33.3) | ||
| Diagnostic/laboratory | 20 | 1 (5.0) | 6 (30.0) | 13 (65.0) | ||
| Health centre/Clinic | 176 | 80 (45.5) | 56 (31.8) | 40 (22.7) | ||
| Hospital | 156 | 97 (62.2) | 47 (30.1) | 12 (7.7) | ||
| Maternity home | 31 | 13 (41.9) | 13 (41.9) | 5 (16.1) | ||
| Medical centre | 70 | 40 (57.1) | 15 (21.4) | 15 (21.4) | ||
| Poly clinic | 12 | 11 (91.7) | 1 (8.3) | 0 (0.0) | ||
| Specialist facility | 15 | 3 (20.0) | 6 (40.0) | 6 (40.0) | ||
Binary Logistic Regression Model of Factors Associated with the Poor Level of IPC
Results on the unadjusted binary logistic regression model of factors associated with poor assessment levels of IPC are shown in Table 5 below. Although significant from the unadjusted model, region of facility location, ownership of the facility, and the poor assessment levels of governance/leadership, management, quality assurance system, human resource, IPC equipment, and assets were not significantly associated with a poor level of IPC assessment from the adjusted model (see Table 5).
Table 5. Binary logistic regression model of factors associated with the poor level of IPC| Variables & categories | Infection Prevention & Control Assessment level | |||
| Unadjusted model | Adjusted model (P) | |||
| COR (95% CI) | P-value | AOR (95% CI) | P-value | |
| Region | ||||
| Greater Accra | 1.00 (reference) | 1.00 (reference) | ||
| Ashanti | 0.36 (0.20, 0.66) | 0.001 | 0.61 (0.30, 1.25) | 0.178 |
| Ownership of facility | ||||
| Private | 1.00 (reference) | 1.00 (reference) | ||
| Public | 0.26 (0.09, 0.73) | 0.011 | 0.56 (0.16, 1.96) | 0.368 |
| Facility type (P) | ||||
| Hospital | 1.00 (reference) | 1.00 (reference) | ||
| CHPS compound | 6.42 (1.23, 33.46) | 0.027 | 3.03 (0.34, 27.38) | 0.323 |
| Diagnostic/laboratory | 20.81 (7.19, 60.26) | <0.001 | 4.27 (1.16, 15.68) | 0.029 |
| Health Centre/Clinic | 3.43 (1.74, 6.74) | <0.001 | 1.76 (0.79, 3.94) | 0.169 |
| Maternity home | 2.40 (0.81, 7.10) | 0.114 | 1.52 (0.45, 5.15) | 0.502 |
| Medical Centre | 3.23 (1.44, 7.23) | 0.004 | 2.68 (1.05, 6.84) | 0.039 |
| Poly clinic | 0.46 (0.03, 8.28) | 0.6 | 1.00 (0.04, 23.34) | 0.998 |
| Specialist facility | 7.91 (2.50, 25.05) | <0.001 | 2.23 (0.59, 8.41) | 0.238 |
| Governance / Leadership | ||||
| Good/moderate | 1.00 (reference) | 1.00 (reference) | ||
| Poor | 6.53 (3.90, 10.93) | <0.001 | 1.21 (0.59, 2.48) | 0.608 |
| Management | ||||
| Good/moderate | 1.00 (reference) | 1.00 (reference) | ||
| Poor | 4.98 (2.97, 8.36) | <0.001 | 1.39 (0.65, 2.97) | 0.393 |
| Quality Assurance System | ||||
| Good/moderate | 1.00 (reference) | 1.00 (reference) | ||
| Poor | 6.92 (4.22, 11.37) | <0.001 | 1.93 (0.99, 3.75) | 0.054 |
| Human Resource | ||||
| Good/moderate | 1.00 (reference) | 1.00 (reference) | ||
| Poor | 7.96 (3.48, 18.20) | <0.001 | 2.18 (0.68, 7.01) | 0.193 |
| IPC Equipment | ||||
| Good/moderate | 1.00 (reference) | 1.00 (reference) | ||
| Poor | 9.74 (5.29, 17.95) | <0.001 | 1.82 (0.78, 4.23) | 0.165 |
| Assets | ||||
| Good/moderate | 1.00 (reference) | 1.00 (reference) | ||
| Poor | 6.84 (3.85, 12.15) | <0.001 | 1.72 (0.78, 3.79) | 0.178 |
| Signage | ||||
| Good/moderate | 1.00 (reference) | 1.00 (reference) | ||
| Poor | 6.10 (3.76, 9.89) | <0.001 | 3.15 (1.74, 5.71) | <0.001 |
| Water Management | ||||
| Good/moderate | 1.00 (reference) | 1.00 (reference) | ||
| Poor | 10.60 (4.19, 26.87) | <0.001 | 5.27 (1.57, 17.77) | 0.007 |
In the adjusted binary logistic regression model, when compared to hospitals, there was a significant increase in the odds of poor IPC assessment level among diagnostic and laboratories (AOR: 4.27, 95% CI: 1.16-15.68, p=0.029) and medical centers (AOR: 2.68, 95% CI: 1.05-6.84, p=0.039). However, the odds of poor IPC assessment level were not statistically significant when other facility types, different than diagnostic and laboratories and medical centers are compared to hospitals in the adjusted model (see Table 5).
Facilities with poor signage system assessment levels significantly increased the odds of poor IPC assessments (AOR: 3.15, 95% CI: 1.74-5.71, p<0.001). Likewise, health facilities with poor water management also significantly increased the odds of poor IPC assessments (AOR: 5.27, 95% CI: 1.57-17.77, p=0.007) (see Table 5).
Discussion
The facilities assessed included hospitals (32.1%), health centres and clinics (36.2%), medical centres (14.4%), maternity homes (6.4%), diagnostic/ laboratories (4.1%), specialist clinic (3.1%), polyclinics (2.5%) and CHPS compound (1.2%). The majority of the 486 health facilities assessed scored high for sterilization system (66.4%), knowledge on decontamination of instruments (60.5%), availability and use of handwashing basin/Veronica bucket with elbow tap (58.4%), PPE availability and use (55.0%) and disinfection practices (52.4%). 92.4% of the facilities had an adequate, fair distribution of sinks and veronica buckets with running water in the IPC equipment assessment domain. Findings from Oppong et al. (2020) study on IPC and associated determinants in 56 acute healthcare facilities in Ghana indicated that the majority of the facilities did not have a significant supply of IPC materials like detergents (66.1%), running water (57.1%) and PPEs availability and use (66.1%). In our study, only 25.7% of the health facilities scored poorly for displaying appropriate handwashing technique materials, 21.6% for handwashing protocol, 37.0% for guidelines or policy for infection control, and 27.6% for infection control IPC/ WASH focal person. This means that the poorly scored facilities have not prioritized providing information to remind staff and posters to support their adherence to standard practices. The implication is that healthcare workers may be limited in responding to emergencies to prevent infection or reinforce standard procedures for infection prevention in case of an outbreak such as COVID-19. 3 required that as part of SOPs for COVID-19 prevention in health facilities, information materials should be displayed at all healthcare facilities' entrances and vantage areas to educate and minimize the risk of transmission (droplet/ contact) of COVID-19. This is a potential non-adherence to the National IPC policy requiring facilities to develop training and learning materials such as flyers, brochures, and posters on IPC for all health workers (Ministry of Health, 2015).
In this study, the overall assessment level of health facilities on infection prevention and control determined as good/moderate IPC system is 80.8%. However, this finding is similar to Oppong et al. (2020), where 87.5% of facilities scored 'adequate' on IPC preparedness. Moreover, our result of 19.2% of facilities with poor IPC is consistent with Oppong et al., (2020) finding of 12.5% with inadequate IPC. This means that facilities with poor IPC systems are likely to expose employees, patients, and visitors to nosocomial infections and risk further COVID-19 infection. Such facilities are not adequately equipped to manage COVID-19 patients.
This study reported the overall assessment of health facilities as good/moderate (82.3%) concerning the Governance and Leadership metric. The facilities with good/moderate Governance and leadership scored higher on the IPC assessment metric (over 67%). The implication is that most facilities with good/moderate Governance and leadership systems support efficient operations and compliance with regulatory requirements. The effect of poor leadership and governance system can affect how the facilities manage infectious disease crises (example, COVID-19), create role conflicts and gaps that can contribute to a possible escalation of nosocomial infections 27 The finding assures that strengthening Governance and leadership at health facilities promotes adherence to IPC policy and guidelines, which will mitigate the risk of spread of infections and promote hygiene. The overall assessment of health facilities, management was good/moderate. Poor management of health facilities negatively affects the quality of health care, patient health outcomes, infection prevention and control, and the image of the health facility 28 .
For the Quality Assurance system, 42.8% were assessed as good, 24.5% moderate, and 32.7% were poor. Further analysis showed that the facilities with good/moderate Quality Assurance (67.3%) also scored higher on the IPC assessment metric (over 69%). Poor Quality Assurance score indicates a flawed health care delivery system and antecedent lack of readiness to prevent and control an outbreak of infection through a standardized approach, with low client interest and satisfaction and high mortality 29. Again, the above further underscores the importance of investment in Quality Assurance systems to improve adherence to IPC policy and guidelines significantly.
For Human Resource assessment, 88.1% were good, 6.6% were moderate, and 5.3% were poor. Most facilities in these regions have access to qualified health workers with a high doctor and nurse-to-patient ratios 30
With respect to the IPC assessment metric, the proportion of facilities from the Greater Accra region with poor assessment (23.3%) was significantly higher when compared to the facility with poor assessment in the Ashanti Region (9.9%). This means that majority of the health facilities in the Ashanti region are not complying with the IPC policy of the country, and therefore have poor IPC systems in place. The ability of such facilities to prevent and control the spread of infection within their operational areas cannot be assured. Therefore, workers and care seekers (patients) may be vulnerable to nosocomial infections.
Strength and Limitations
This study used primary data collected from selected health facilities in Ghana's Greater Accra and Ashanti regions with a high participation rate. Hence, selection bias is minimized. The study population was relatively homogeneous with regard to background factors. Hence, the potential effect of unmeasured confounders was minimized. Additionally, findings from this study can be generalized considering the homogeneity of the facilities at various levels in the country, from CHPS compound to regional referral hospitals, inclusive of private and public facilities. No tertiary hospitals were included.
This study used a cross-sectional design; hence, causality cannot be established, and therefore, this study could only report on associations and not cause and effects. There is the possibility of information biases as a selection of variables and self-reported information on Governance and IPC were not controlled by the researchers.
Conclusion
The monitoring has revealed that the majority of the health facilities in the two regions (Greater Accra and Ashanti) have a good system to ensure effective infection prevention and control and have been adhering to the regulatory requirements of the Health Facilities Regulatory Agency. These areas of compliance with adequate performance include Water supply, Human Resources, Governance, Management, IPC Equipment, Quality Assurance, and Assets of the facilities. However, signage was a significant challenge in many facilities, which is likely to affect communication within the facilities on IPC-related actions. The leadership and Governance system of the health facilities influenced compliance to IPC requirements, good assets available in the facility positively influenced the IPC system, and a good water supply system contributed to an enhanced IPC system. IPC assessment was poor in the Greater Accra region.
From the Findings of the Study, the Following are
Recommended
1. HeFRA should intensify the monitoring of health facilities and results of such exercises shared with facility owners to know their performance as part of the feedback system with the recommended remedial actions and sanctions. This will help facilities commit to improving IPC systems in their facilities and comply with regulatory requirements.
2. HeFRA should collaborate with relevant stakeholders to design and implement capacity support services to health facilities performing poorly. Where no effort is made for improvement, such facilities should be closed down.
3. Health facilities should provide appropriate signage on IPC at various health facilities to provide information to staff and clients to safeguard them.
4. The Regional Health Directorates' role in monitoring should be strengthened in infection prevention systems in health facilities.
5. Managers of health facilities should prioritize and commit to implementing effective IPC systems for enhanced health care delivery and effective nosocomial infection prevention measures.
Abbreviations
AOR: Adjusted Odds Ratio; CHPS: Community-based Health Planning and Services; CI: Confidence Interval; COR: Crude Odds Ratio; GHS: Ghana Health Service; HeFRA: Health Facilities and Regulatory Agency; HeFMT: Health Facilities Monitoring Tool; HCWM: Healthcare Waste Management; IPC: Infection Prevention and Control; MoH: Ministry of Health; TES: Total Expected Score; UNDP: United Nations Development Program; UNICEF: United Nations Children's Fund; WHO: World Health Organization;
Ethics Approval and Consent to Participate
Not applicable
Consent for Publication
Not applicable
Availability of Data and Materials
Available on request from PAB
Funding
The study received significant funding from United Nations Development Program UNDP and Ghana Ministry of Health.
Authors' Contributions
PAB developed the research strategy and concept. BAK, MA, JA, F.O., L.O., and AY supervised the data collection and conceptualized the data analysis. E.A., MA, S.T., RMO, and D.D. drafted the first version of the manuscript. PAB, E.A., MA, R.Q., RMO, and Y.A. conceptualized the research questions and interpreted the final version of the manuscript. All authors read and approved the manuscript.
Acknowledgment
We acknowledge the support from HeFRA and management and owners of all health facilities in the Greater Accra and Kumasi Regions.
References
- 1.Huang C, Wang Y, Li X, Ren L, Zhao J. (2019) Clinical features of patients infected with 2019 novel coronavirus in Wuhan. , China. Lancet.395,497–506
- 2.Ghana Health Service. (2021) Situation Update. Covid-19 Outbreak in Ghana as ofApril5,2021. https://ghanahealthservice.org/covid19/latest.php .
- 4.World Health Organization, UNICEF. (2020) . Water, Sanitation, Hygiene, and Waste Management for Covid-19 Virus Technical Brief. https://www.who.int/emergencies/diseases/novel-coronavirus-2019/technical-guidance/infection-prevention-and-control .
- 5.Health World.Organization (WHO (2ED)) (2014). Safe management of waste from healthcare activities. Geneva [Switzerland]:.
- 6.N van Doremalen, Bushmaker T, Morris D H, Holbrook M G, Gamble A.et al.(2020) Aerosol and surface stability of SARS-CoV-2 as compared with SARS-CoV-1. , N Engl J. Med.10.1056/NEJMc2004973
- 7.Chin A, Chu J, Perera M, Hui K, Yen H L. (2020) Stability of SARS-CoV-2 in different environmental conditions. The Lancet. , Microbe 1(1), 10.
- 8.Nghiem L D, Morgon B, Donner E, Short M D. (2020) The COVID-19 pandemic: Considerations for the waste and wastewater services sector. Case Studies in Chemical and Environmental Engineering.1, Article 100006.
- 10.Ministry of Health (2015) National Policy and Guidelines for Infection Prevention and Control in Health Care Settings. https://www.ghanahealthservice.org/downloads/National_Policy_and_Guidelines%20_fo r_Infection_Prevention_and_Control_in_Health_Care_Settings_2015.pdf
- 11.UN-Habitat. (2020) How to continue waste management services during the COVID-19 pandemic. https://buff.ly/3c5XC4h
- 12.Islam M, Rahman K, Sun Y, Qureshi M, Abdi I et al. (2020) Current knowledge of COVID-19 and infection prevention and control strategies in healthcare settings: A global analysis. , Infection Control & Hospital Epidemiology 41(10), 1196-1206.
- 13.Rainey R, Weinger M. (2016) The role of water, sanitation, and hygiene (wash) in healthcare settings to reduce transmission of antimicrobial resistance. Infection Prevention and Control. 2,59–62. The role of water, sanitation, and hygiene (WASH) in healthcare settings to reduce transmissionof antimicrobial resistance AMR Control (resistancecontrol.info).
- 14.McGriff J A, Denny L. (2020) What COVID-19 reveals about the neglect of WASH within infection prevention in low-resource healthcare facilities. , American Journal of Tropical Medicine and Hygiene 103(5), 1762-1764.
- 15.Kalantary R R, Jamshidi A, Mofrad M, Jafari A J, Heidari N et al. (2021) Effect of COVID-19 pandemic on medical waste management: a case study. Journal of environmental health science and engineering. 1-6.
- 16.Kashyap S, Ramaprasad A, Bidare Sastry N. (2020) Waste quarantine to reduce COVID- 19 infection spread. The International Journal of health planning and management. 35(5), 1277-1278.
- 17.Liang Y, Song Q, Wu N, Li J, Zhong Y et al. (2021) Repercussions of COVID-19 pandemic on solid waste generation and management strategies. , Frontiers of environmental science & engineering 15(6), 115.
- 18.Shammi M, Behal A, Tareq S M. (2021) The escalating biomedical waste management to control the environmental transmission of COVID-19 Pandemic: A Perspective from Two South Asian Countries. , Environmental Science & Technology 55(7), 4087-4093.
- 19.Belhadi A, Kamble S S, SAR Khan, Touriki F E, Dileep K M. (2020) Infectious waste management strategy during COVID-19 pandemic in Africa: an integrated decision- making framework for selecting sustainable technologies. , Environmental Management.66 1085, 1104.
- 20.DTO Temitope, Kasim O F, Famewo A, Oyedotun T D, Moonsammy S. (2020) Municipal waste management in the era of COVID- 19: Perceptions, practices, and potentials for research in developing countries. , Research in Globalization 2.
- 21.Nzeadibe T C.Ejike-Alieji AUP.(2020) Solid waste management during Covid-19 pandemic: policy gaps and prospects for inclusive waste governance in Nigeria. Local Environment. 25(7), 527-535.
- 22.Sarkodie S A, Owusu P A. (2020) . Impact of COVID19 pandemic on waste management. Environment, Development, and Sustainability .
- 23.Ashinyo M E, Amegah K E, Dubik S D, Ntow-Kummi G, Kudzo-Adjei M.(2021a) The WASH FIT approach evaluates the water, sanitation, and hygiene status of COVID-19 healthcare facilities in Ghana. , Journal of Water, Sanitation and Hygiene for Development 11(3), 398-404.
- 24.Ashinyo M E, Dubik S D, Duti V, Amegah K E, Ashinyo A et al.(2021b) Infection prevention and control compliance among exposed healthcare workers in COVID-19 treatment centers in Ghana: A descriptive cross-sectional study. , PloS one 16(3), 0248282-10.
- 25.Oppong T B, Amponsem-Boateng C, Kyere E, Wang Y, Gheisari Z. (2020) . Infection Prevention and Control Preparedness Level and Associated Determinants in 56 Acute Healthcare Facilities in Ghana. Infection and drug resistance 13, 4263-4271.
- 26.WHO. (2020) Infection prevention and control healthcare facility response for COVID-19: A module from the suite of health service capacity assessments in the context of the COVID-19 pandemic. , INTERIM GUIDANCE
- 27.Gould D J, Gallagher R, Allen D. (2016) Leadership and management for infection prevention and control: what do we have and what do we need?. , Journal of Hospital Infection 94(2), 165-168.
- 28.Allen E P, Muhwezi W W, Henriksson D K, Mbonye A K. (2017) Health facility management and access: a qualitative analysis of challenges to seeking healthcare for children under five in Uganda. Health policy and planning. 32(7), 934-942.