Risk Factors Associated with Breast Cancer
Abstract
In Mexico, breast cancer is the second most common site of cancer in women and in most developed and emerging countries. Incidence rates have increased in many countries, although in some, mortality has remained stable with a slight reduction. There are geographical differences with high rates of breast cancer in North America, Northern Europe and Oceania, and lower rates in Central and South America, South and East Europe; in addition to emerging countries in Africa and Asia. Genetic and hereditary factors constitute less than 5% of breast cancer cases and other risk factors for breast cancer are related to the reproductive life of the woman. This work was carried out in order to determine if the risk factors considered classic are really associated with breast cancer in our sample of Mexican women studied.
Author Contributions
Academic Editor: Nasim Habibzadeh, Teesside university, United Kingdom.
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2020 Víctor Manuel Vargas-Hernández
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Introduction
In Mexico, breast cancer is the second most common site of cancer in women and in most developed and emerging countries 1. Incidence rates have increased in many countries, although in some, mortality has remained stable with a slight reduction 2 There are geographical differences with high rates of breast cancer in North America, Northern Europe and Oceania, and lower rates in Central and South America, South and East Europe; in addition to emerging countries in Africa and Asia 3. Genetic and hereditary factors constitute less than 5% of breast cancer cases and other risk factors for breast cancer are related to the reproductive life of the woman 4. This work was carried out in order to determine if the risk factors considered classic are really associated with breast cancer in our sample of Mexican women studied.
Material and Methods
A retrospective, observational and descriptive study was carried out in 162 women with breast cancer over (2002-2004) in the Oncology Gynecology Service of the Hospital Juárez de México to determine whether reproductive risk factors are factors that are in these patients related to breast cancer. Patients with a complete medical record and a diagnosis of breast cancer were included. The variables studied were: age at the time of breast cancer diagnosis, age at menarche, duration of breastfeeding, number of pregnancies, age of first delivery, history of the use of menopausal hormone therapy; other variables were body mass index, diabetes mellitus, arterial hypertension, alcoholism, and a family history of breast cancer.
Statistical Analysis
A statistical analysis was carried out using the SPSS statistical package, after data capture of the variables studied in the Microsoft Excel program for Windows 2003. It is a clinical investigation of a descriptive analysis that included location and dispersion measures, as well as graphic analysis using bar charts.
Results
The sample size was 200 patients, of which 38 were excluded due to not having inclusion criteria and only 162 patients were studied. The age range at the time of breast cancer diagnosis was 27 to 78 years (mean 47.60, standard deviation 13.09); (Figure 1) early menarche occurred only in 12.3% (n = 20) of patients; 64.4% (n = 104) presented menarche between 12 and 13 years of age. The mean age at the time of breast cancer diagnosis for the early menarche group was 55 years and for the general group it was 47.6 years. The mean age of the first pregnancy was 22 years and the age of menopause was 51 years; 54% of the patients had 3 pregnancies; 72.2% were breastfed (n = 117) and 45.1% were for more than 6 months (n = 73); menstrual disorders occurred in 22.8% of cases (n = 37), oligomenorrhea predominating in 43.3% of cases (n = 16); Hormone therapy for menopause was previously used in 19.8% (n = 32). Hereditary-family history of breast cancer occurred in 14.2% (n = 23) and smoking in 11.1% (n = 18). It was correlated that nulliparous patients, with alcoholism and absence of breastfeeding, breast cancer occurred in those under 45 years of age and only the risk factor that was related to breast cancer was overweight and obesity with 54.26 and 17.11% respectively (mean 28.00, standard deviation 3.032). (Figure 2).
Figure 1.The age range at the time of breast cancer diagnosis was 27 to 78 years (mean 47.60, standard deviation 13.09).
Figure 2.Overweight was presented in 54.26% and Obesity in 17.11. The average body mass index was 28 m² of body surface; with a mode of 29 m² of body surface.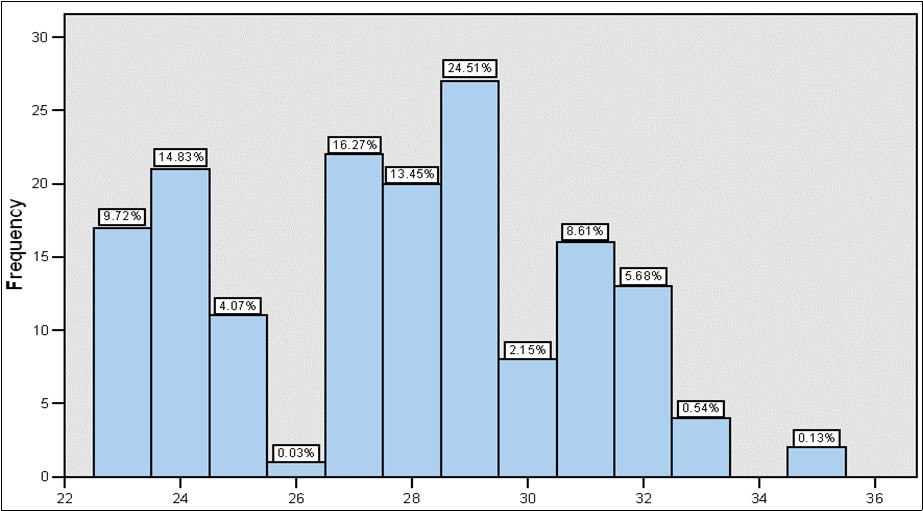
Discussion
There are risk factors considered important that are associated with breast cancer; including risk reduction surgery 5. The documented risk factors are different according to the population studied; mainly the age of presentation, where the incidence of breast cancer before 30 years of age is low 6.The patients in our study the average age was (43 years) at the diagnosis of breast cancer lower than that reported in the literature (1.7).
Other reports of women with menarche before the age of 12, increased the relative risk of 1.3 of invasive breast cancer compared, with those, if they started it after 15 years, and in the present study early menarche only appeared in 12.3 % of cases were not observed to be associated with early detection of breast cancer. 8
A higher risk is also reported in nulliparous women or those who had their first childbirth after the age of 30, in the present study this relationship was not observed either and nulliparity was only present in 15.4% and women who had a child after 30 years was 2.37% 9. The absence of breastfeeding was also considered a risk factor; 10 in our study, 72.2% lactated and did not show a relationship, only the absence of breastfeeding was related to the appearance of breast cancer at an earlier age (less than 42 years), in the same study a significant relationship was reported with the use of oral contraception, while in this sample only 25.3% had this antecedent, an increase in the incidence of breast cancer was also reported with the use of menopausal hormone therapy, without being observed in the sample that was studied, only 19.8% had this antecedent and 3.7% used it for more than 5 years. (eleven)
A relationship between alcohol consumption and smoking with an increase in breast cancer is reported, which was also not observed in this study, only patients with alcohol consumption had breast cancer at an earlier age. 12. It is observed that a high body mass index is a lower risk factor, unlike the sample studied, a greater correlation with breast cancer was found with a BMI greater than 25m²sc 13, a risk of 1.8 is also reported for women with a history of family cancer while this study was found to occur in 14.2% of cases. 14. The results obtained from this study surprise us that of all the usual risk factors reported, they do not seem to have a correlation in our sample; only a strong correlation exists between overweight, obesity, and breast cancer, which needs to be confirmed with randomized control groups; This highlights the importance of having our own epidemiology in Mexican women; Current and future studies are based on molecular biology in relation to the genes involved in the breast cancer process 15 as part of a strategy in the evaluation of a definitive risk of breast cancer. 16.
Conclusions
Through our observation in the current study, we have concluded that there is no correlation between the usual risk factors associated with breast cancer; only overweight and obesity are related. Further research is required in other different countries and to study other risk factors involved in the genesis of breast cancer such as inflammatory factors, insulin-like growth factors, and hyperinsulinism.
References
- 1.LAG Ries, Eisner M P, Kosary C L. (2000) . SEER Cancer Statistics Review, 1973–1997, National Cancer Institute. NIH Pub. No. 00–2789 , Bethesda, MD .
- 2.Vogel V G. (1998) Breast cancer risk factors and preventive approaches to breast cancer. In: Kavanagh. Cancer in women. Malden,MA: Blackwell Science 58-91.
- 3.Prout M N. (2000) Breast cancer risk reduction: what do we know and where should we go? Medscape Women’s Health eJournal. 5, 1-9.
- 4.PDP Pharoah, Day N E, Duffy S. (1997) Family history and the risk of breast cancer: a systematic review and meta-analysis. , Int 71, 800-809.
- 5.Stybo T M, Wood W D. (1999) The management of ductal and lobular breast cancer. Surg Oncol. 8, 67-75.
- 6.McGuire Andrew, Brown James A L, Malone Carmel, McLaughlin Ray, Michael J Kerin. (2015) . Effects of Age on the Detection and Management of Breast Cancer. Cancers , (Basel) 7(2), 908-929.
- 7.Steinberg K K, Thacker S B, Smith S J. (1991) A meta-analysis of the effect of estrogen replacement therapy on the risk of breast cancer. , JAMA 265, 1985-1990.
- 8.Brinton L A, Schaiere C, Hoover R N. (1988) Menstrual factors and risk of breast cancer. Cancer Invest. 6, 145-154.
- 9.Guo F, Kuo Y F, YCT Shih, Giordano S H, Berenson A B. (2018) Trends in breast cancer mortality by stage at diagnosis among young women in the United States. , Cancer 124(17), 3500-3509.
- 10.Paredes A. (1991) Factores de riesgo en cáncer de mamario. Ginecología y Obstetricia de México. 59, 49-45.
- 11. (1997) Collaborative Group on Hormonal Factors in Breast Cancer. Breast cancer and hormone replacement therapy: collaborative reanalysis of data from 51 epidemiological studies of 52,705 women with breast cancer and 108,411 women without breast cancer. , Lancet 350, 1047-1059.
- 12.Harvey E B, Schairer C, Brinton L A. (1987) Alcohol consumption and breast cancer. , J Natl Cancer Inst 78, 657-661.
- 13.Thomas E Rohan, Heo Moonseong, Choi Lydia, Datta Mridul, Jo L Freudenheim et al. (2013) Body Fat and Breast Cancer Risk in Postmenopausal Women: A Longitudinal StudyJ Cancer Epidemiol. 1-13.
- 14.Brentnall A R, van Veen EM, Harkness E F. (2020) Una evaluación de control de casos de 143 polimorfismos de nucleótidos individuales para la estratificación del riesgo de cáncer de mama con factores clásicos y densidad mamográfica. , Int J Cáncer 146(8), 2122-2129.
