Epidemio-Clinical Profile of Acute Diarrhea in Children From 0 To 5 Years and Prevalence of Rotavirus Before and After the Introduction of the Rotasiil Vaccine in the Democratic Republic of Congo.
Abstract
Introduction
Acute diarrhea remains one of the major health problems in developing countries. According to the WHO, rotavirus contributes to approximately 40% hospitalizations and is the leading cause of severe diarrhea in children 0-5 years old.
The objective was to determine the prevalence of rotavirus and the sociodemographic and clinical profile among children with diarrhea in 4 hospitals in the DRC.
Methods
This study is documentary, retrospective and analytical taking two periods, before and after introduction of the vaccine, i.e. January 2017 to December 2018 and January 2020 to December 2021 in 4 hospitals, i.e. 2 in Kinshasa and 2 in Lubumbashi.
Results
Total 1872 children, 924 (49.4%) of whom were enrolled before the introduction of the vaccine and 948 (50.6%) after. Only 1737 had performed serology, of which 875 (50.4%) were rotavirus positive and 862 (49.6%) were negative. Positive results, a reduction of 30.6% is noted since the introduction of the vaccine. The predominant age range was 6 to 11 months. The male gender was predominant at 56.7%.
Diarrhea was found in 88.5%, vomiting in 73.7% and fever in 73.9%. Before vaccination, the risk was more: 11 times to have diarrhea, 9-10 times the frequency between 3-10 times a day, 9 times vomiting, 2 times fever and 2 times to have a positive result.
Conclusion
From this study, we note a reduction frequency due to diarrhea unlike previous years, probably attributable to the vaccine.
Author Contributions
Academic Editor: Raul Isea, Fundación Instituto de Estudios Avanzados -IDEA.
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2023 Freddy Mboko Byamungu, et al
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Introduction
Acute diarrhea remains one of the major public health issues in a number of developing countries. According to the World Health Organization (WHO), rotavirus contributes to around 40% of hospitalizations and the main cause of severe diarrhea in under five children worldwide 1.
It is associated with the death of more than 600,000 children under the age of 5 per year worldwide, the most affected of which are malnourished infants living in disadvantaged, low-income rural areas, where access to health care is poor 1, 2, 3, 4.
Since 2006, rotavirus vaccines have been recommended for all countries by the World Health Organization (WHO). In 2009, more than 100 countries, including six with a high burden of disease (Afghanistan, Angola, Ethiopia, India, Kenya and Pakistan) introduced a rotavirus vaccine into their vaccination program 5, 6, 7.
The Democratic Republic of Congo (DRC) introduced the Rotasiil vaccine into its immunization schedule in 2019 12, 13. But few studies have assessed the impact of vaccination on the prevalence of rotavirus and the clinical profile of diarrhea. Thus this study aimed to determine the prevalence of rotavirus among children with diarrhea and the description of the sociodemographic and clinical profile of children from 0 to 5 years old with diarrhea in 4 hospitals in the DRC.
Methods
It’s a documentary, retrospective and analytical study which took into account two periods, before and after introduction of the rotasiil vaccine, i.e. from January 2017 to December 2018 and from January 2020 to December 2021. It took place in 4 hospital structures, i.e. 2 in Kinshasa, the capital of the DRC and 2 in Lubumbashi, the 2nd largest province of the country. In addition, these health structures had received support in diagnostic tools as part of rotavirus surveillance. The data was collected exhaustively and consecutively on the basis of consultation registers, patient files and laboratory registers.
All records of infants and children under 5 years of age who presented with diarrhea lasting less than 1 week were included in the study. Two stool samples were taken 2 days apart in these children, in 2 jars, within 48 hours of their admission for a SANDWICH ELISA serological test. We’re not included all the children who had not carried out the serological test or those who did not have stool results available or those whose medical records were not found. Socio-epidemiological (age, sex, origin, month of consultation) and clinical (fever, vomiting, diarrhea with its frequency, appearance and duration) data were collected. Data were analyzed using SPSS 26.0 software. Quantitative variables were summarized by the median with their interquartile spaces, categorical ones were presented as relative frequencies/percentage and Pearson's chi-square test or Fisher's test was used for the comparison of proportions. The p˂0.05 value was considered statistically significant. The study had received the approval of the ethics committee of the school of public health under the number ESP/CE/36/2022. The confidentiality of our results was guaranteed.
Results
A total of 924, or 49.4%, of children were enrolled before the introduction of the vaccine and 948, or 50.6% after the introduction of the vaccine, giving a total of 1,872 cases. Of this number, only 1737 had taken the serological test, of which 875 (50.4%) had a positive result for rotavirus and 862 (49.6%) had a negative result.
However, from these positive results before and after vaccination, there is a reduction of 30.6% since the introduction of the Rotasiil vaccine in the DRC.
Regarding children with diarrhea according to the sites, the provincial city of Kinshasa had registered 1,360 children, i.e. 72.6% and the city of Lubumbashi recorded 512 children, i.e. 24.6%.
The median age of the patients was 8 months (6 to 12 months of interquartile space). The predominant age range was 6 to 11 months. (Table 1)
Table 1. Distribution by age| Variables | Effectifs ( n =1872) | % |
| Age of children (Median, EIQ) | 8 months (6– 12months) | |
| Children's age range | ||
| 0-5 months | 465 | 24,8 |
| 6-11 months | 879 | 47,0 |
| 12-23 months | 434 | 23,2 |
| 24-60 months | 94 | 5,0 |
The socio-demographic data were presented according to the periods of the study (Table 2).
Table 2. Association between sociodemographic characteristics and vaccination| Vaccine | |||
|---|---|---|---|
| Variables | Before n( %) | After n( %) | P |
| Children’s age range | 0,00* | ||
| 0-5 months | 269 (29,1%) | 196 (27%) | |
| 6-11 months | 441 (47,7%) | 438 (46,2%) | |
| 12-23 months | 175 (18,9%) | 259 (27,3%) | |
| 24-59 months | 39 (4,2%) | 55 (5,8%) | |
| Gender of child | |||
| Male | 527 (57,0%) | 534 (56,3%) | 0,78 |
| Female | 397 (43,0%) | 414 (43,7%) | |
| City of origin | |||
| Kinshasa | 634 (68,6%) | 726 (76,6%) | 0,00* |
| Lubumbashi | 290 (31,4%) | 222 (23,4%) | |
The male sex was predominant with 1061 cases (56.7%) against 811 (43.3%) of female sex. The sex ratio was 1.3 in favor of boys.
The results showed a significant association with age and Kinshasa city, while gender had no significant statistical value.
In order to highlight the seasonality of the disease, the frequency of patients was presented monthly during the 2 periods of the study, namely, before and after vaccination. The figure 1 below shows the trend.
Figure 1.Seasonality in relation to the 2 periods of the study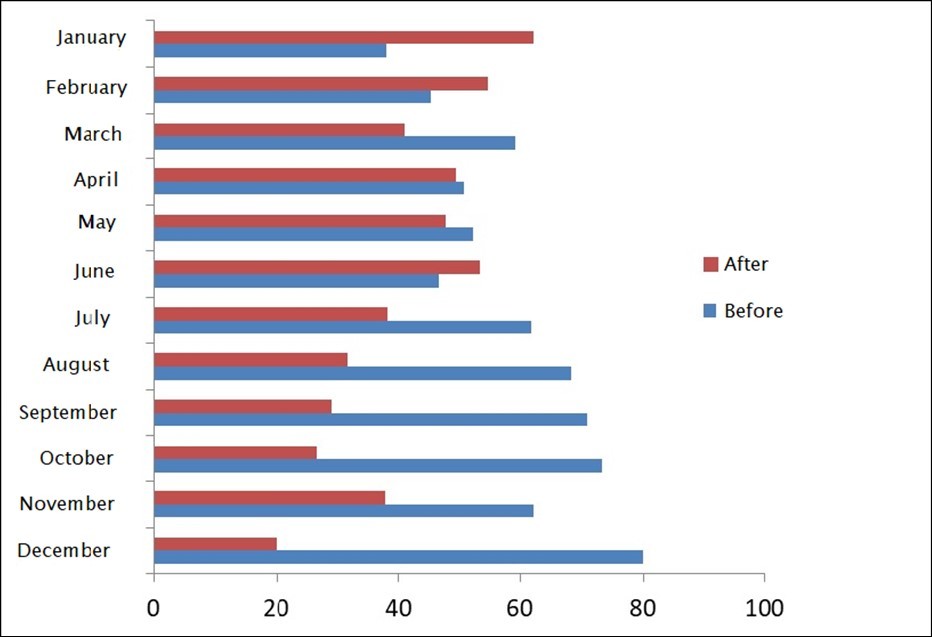
We note that before the introduction of the vaccine, the frequency generally decreased from January to December, while the opposite trend was observed after the introduction of the Rotasiil vaccine.
As for the clinical characteristics, in our series, diarrhea, vomiting and fever are the dominant symptoms in all children. Moderate to severe diarrhea being found in the majority of cases 88.5%, vomiting in 73.7% of cases and fever in 73.9% of cases.
The association between clinical characteristics and vaccination is presented in Table 3.
Table 3. Association between clinical characteristics and vaccination| Vaccine | ||||
| Variables | BeforeN (%) | AfterN (%) | IC 95% | P |
| Notion of diarrhea | ||||
| Yes | 903 (97,7%) | 754 (79,5%) | 11,1 (7,0; 17,5) | 0,00* |
| No | 21 (2,3%) | 194 (20,5%) | 1 | |
| Frequency of diarrhea by day | ||||
| 1-2 times | 238 (25,8%) | 479 (50,5%) | 1 | |
| 3-10 times | 677 (73,3%) | 467 (49,3%) | 2,9 (2,4; 3,5) | 0,00* |
| > 10 times | 9 (1,0%) | 2 (0,2%) | 9,1 (1,9; 42,2) | <0,01* |
| Notion of vomiting | ||||
| Yes | 852 (92,2%) | 527 (55,6%) | 9,5 (7,2; 12,4) | 0,00* |
| No | 72 (7,8%) | 421 (44,4%) | 1 | |
| Notion of fever* (n=1684) | ||||
| Yes | 773 (84,9%) | 611 (79,0%) | 1,5 (1,2; 1,9) | 0,02* |
| No | 138 (15,1%) | 162 (21,0%) | 1 | |
| ELISA Test * (n=1737) | ||||
|---|---|---|---|---|
| Positive | 521 (57,8%) | 354 (42,3%) | 1,9 (1,5; 2,3) | 0,00* |
| Negative | 380 (42,2%) | 482 (57,7%) | 1 | |
Note that children before vaccination were 11 times more likely to have diarrhea than after the vaccine. And the risk of having diarrhea between 3-10 times was 3 times, even 9-10 times greater before than after the introduction of the vaccine.
The risk of having an episode of vomiting was 9 times greater before vaccination than after. And the risk of fever was twice as great before the introduction of the vaccine as after it. The risk of having a positive result was twice as great before the introduction of the vaccine as after. (Table 3).
Discussion
Acute diarrhea remains one of the major public health issues in a number of developing countries. According to the World Health Organization (WHO), rotavirus contributes to around 40% of hospitalizations and the main cause of severe diarrhea in under five children worldwide. The objective was to determine the prevalence of rotavirus and the sociodemographic and clinical profile among children with diarrhea in 4 hospitals in the DRC. To achieve this, we conducted the study of certain socio-demographic parameters and prevalence.
Frequency
During our study, 1872 children aged 0-5 years were enrolled, i.e. 38% compared to the study carried out by Luhata et al. 14 from 2009-2019, i.e. 10 years, and who had enrolled 4,928 out of 4,952 (99.5%), there is a significant hospital reduction of 61.5% in cases of diarrhea recorded in the sentinel sites. This reduction is similar to those reported by Parveen Fathima et al. in Australia(66-79%). And, comparing the two periods, significant decreases were observed in children aged less than 12 months by 66% and between 12 and 23 months by 57% 15. It is also similar to that observed in Spain by Monica Lopez-Lacort which decreased with age, by 72% and 58% respectively in two-year-old children compared to those less than one-year-old 16. This reduction is far superior to that observed in Rwanda (17-29%) despite a very significant reduction in Rotavirus diarrhea after the introduction of the vaccine 17 and vaccination coverage reaching more than 95% and in Spain (20%) where a low vaccination coverage in Europe (50%) was noted. The average reduction observed in Sub-Saharan Africa is 25-42% 18, 19, 20, 21.
A study carried out in Afghanistan (highly affected country) showed that vaccination against Rotavirus has the potential to prevent more than one million cases; 660,000 outpatient visits; approximately 50,000 hospital admissions; 650,000 DALYs; and 12,000 deaths, over 10 years. This high frequency in our study would certainly be correlated with the presence of the vaccine.
Age and Sex
A. Age
The most affected age group was 6 - 11 months (47%), followed by 0 - 5 months (24.8%) and both accounted for 71.8% of children.
This result is similar by Luhata but also by many other authors 14, 22, 23, 24, 25 and the literature 3, 4.
This young age implies the time of exclusive breastfeeding recommended, the introduction of a varied diet with the risks that accompany it.
This highlights the importance of protective immunoglobulins in breast milk in preventing acute Rotavirus infections.
According to Seasonality
Clinical features
In our series, diarrhea, vomiting and fever are the dominant symptoms in all children.
Diarrhea being found in the majority of cases 88.5%, vomiting 73.7% and 73.9% presented fever. This result converges with the literature 1, 4, 6, 8, 27, 28 and Luhata: 100% diarrhea and 92% vomiting. Several infectious episodes (1-4) increase immunity and reduce the risk of subsequent diarrhea, especially that due to Rotavirus.
Comparing with the study carried out by Luhata on Rotavirus positivity before the introduction of the vaccine (60%), there is a small difference in our study, 57.8%. This rate is far higher than those observed in many African countries such as Kenya (26%), Gambia (22%), Ethiopia (23%), Benin (39.9%), Cote d' Ivory (28.8%) and RSA (24%).
This reduction is far from the reduction rate nevertheless of certain countries of the continent like Rwanda, 17-29% reduction in hospitalization due to diarrhea and 61-70% reduction due to Rotavirus (Vaccination rate between 98- 99%), in Ghana 5, a reduction ranging from 74.2% to 43.9%, in Madagascar where before the introduction of the vaccine, 56% of positive samples fell from 13% in 2015, 12% in 2016 27.29.30
In Pakistan, current trends note a halving of deaths due to AVR diarrhea 31. But also from some Asian countries such as India, 43.6% 32.
In our study, a 30.6% reduction was observed when comparing positive results before and after vaccination. This weakness is probably linked to the low vaccination rate in the DRC as in the majority of developing countries 10, 11, 13, 14. It is however close to that observed in Spain (36%), in Belgium, 32–43% against 55% before the introduction of the vaccine, in Turkey (45%), in Nigeria, 25-35% against 66% before the vaccine introduction 27, 28.
Compared to the reduction in hospitalization for diarrhea before and after vaccination, this weakness is to be considered globally in the countries of Africa and Asia (17-50%) compared to the developed countries of Europe and America (50-70% and 85-98% respectively intermediate and developed countries 33.
This study evaluated the epidemiological and clinical aspects of diarrhea after the introduction of the Rotasiil vaccine into the vaccination schedule in the DRC. It was limited by the fact of having only taken into account the hospitals of Kinshasa and Lubumbashi and not having emphasized the vaccination status of the children enrolled in this study and the strains of rotavirus identified.
Conclusion
The Democratic Republic of Congo, like many other countries on the continent, have introduced the vaccine against Rotavirus (Rotasiil) into their vaccination schedule. At the end of this study, we noted a reduction in frequency due to diarrhea unlike previous years, this is probably attributable to the presence of the vaccine and the age group under 12 months pays the greatest burden. of this pathology.
Declaration of interests
The authors declare that they have no competing financial interests or known personal relationships which might appear to influence the work reported in this article.
Contribution of the authors
1. Freddy Mboko Byamungu : design, writing of the work and data collection,
2. LoukiaPaizanosAketi: supervision and writing of the work,
3. Joseph Diayisu Shiku: work supervision,
4. Dr Joëlle Nzuzi Bemba: support for data collection,
5. Dr Rosette KevaaniLepira: support for data collection,
6. Dr Irène Kifutu Matula: support for data collection,
7. Éric TshitonaKaluli: support for data collection.
Thanks
We also appreciate the contribution of all the sentinel teams (nurses, laboratories and data managers) who not only allow the implementation of these surveillance activities in the field which have made the data available to us.
We would also like to thank the INRB team who contributed to making the database available to us, but also the families of the children for their passage through the care structures contributed to obtaining this data.
References
- 2.Troeger C, Khalil I A, Rao P C, Cao S, Blacker B F.Vaccination antirotavirus et fardeau mondial de la diarrhée à rotavirus chez les enfants de moins de 5 ans. JAMA Pédiatre 1er octobre 2018 ;172(10) : 958 65.
- 3.Mwenda J M, Ntoto K M, Abebe A, Enweronu-Laryea C, Amina I. (2010) Burden and epidemiology of rotavirus diarrhea in selected African countries : preliminary results from the African Rotavirus Surveillance Network. J Infect Dis. 202 Suppl : S5 –S11 .
- 4.Kotloff K L, Nataro J P, Blackwelder W C, Nasrin D, Farag T H.Burden and etiology of diarrhoea disease in infants and young children in developing countries (the Global Enteric Multicenter Study, GEMS) : a prospective, case-control study. Lancet. 2013 ;382(9888) : 209-22.
- 5.E O Asarea, M A Al-, G E Armahb, B A Lopmanc, Parashard Umesh D. (2020) Modeling of rotavirus transmission dynamics and impact of vaccination in Ghana Published in final edited form as: Vaccine. 38(31), 4820-4828.
- 6.Dennehy P H.Effets du vaccin sur la maladie à rotavirus dans la population pédiatrique. Opinion actuelle en pédiatrie. 2012ÿ ; 24(1) : 76–84. PMID : 22189398.
- 7.Lopmanc B A, Pitzer V E, Sarkar R, Gladstone B, Patel M. (2012) Comprendre l'efficacité réduite du vaccin antirotavirus dans les milieux socioéconomiques défavorisés. PLoS One. 7(8) : e41720
- 8.Vesikari T, Matson D O, Dennehy P, P Van Damme, Santosham M. (2006) Innocuité et efficacité d'un vaccin antirotavirus pentavalent humain-bovin (WC3) réassorti. , New England J Medicine 354(1), 23-33.
- 9.Diarrhoeal GBD. (2015) Diseases Collaborators. Estimates of global, regional, and national morbidity, mortality, and etiologies of diarrhoeal diseases : a systematic analysis for the Global Burden of Disease Study. Lancet Infectious Diseases 2017 ;17(9) : 909-48.
- 10.Bennett A, Nagelkerke N, Heinsbroek E, Premkumar P S, Wnÿk M. (2017) Estimation de l'incidence de l'infection à rotavirus chez les enfants de l'Inde et du Malawi à partir des titres en série d'IgA anti-rotavirus. PloS One.
- 11.Lopmanc B A, Pitzer V E, Sarkar R, Gladstone B, Patel M. (2012) Comprendre l'efficacité réduite du vaccin antirotavirus dans les milieux socioéconomiques défavorisés. PloS One. 7(8) : e41720
- 12.Gasparinho C, Piedade J, Mirante M C, Mendes C, Mayer C. (2017) Caractérisation de l'infection à rotavirus chez les enfants atteints de gastro-entérite aiguë dans la province de Bengo, au nord-ouest de l'Angola, avant l'introduction du vaccin. , PloS One 19, 0176046.
- 13.Kirkwood C D, Ma L F, Carey M E, Steele A D. (2017) Le pipeline de développement de vaccins contre le rotavirus. , Vaccine 07, 37-50.
- 14.C L Luhata, Burke Rachel M, Aimé Cikomola, Mukamba E, Eleanor Burnett. (2022) Epidemiology and pre-vaccine burden of rotavirus diarrhea in Democratic Republic of Congo (DRC) : Results of sentinel surveillance, 2009–2019. Vaccine. 40(41), 5033-5941.
- 15.Parveen Fathima, Jones A Mark, H C Moore, Blyth C, Robyn A Gibbs.. Impact of Rotavirus Vaccines on Gastroenteritis Hospitalizations in Western Australia : A Time-series Analysis 1,3,6,7. J Epidemiol 2021 ; 31(8) : 480-486.
- 16.López-Lacort M, Orrico-Sánchez A, M Á, Muñoz-Quiles C, Díez-Domingo J. (2020) Spatio-temporal impact of self-financed rotavirus vaccination on rotavirus and acute gastroenteritis hospitalisations in the Valencia region, Spain. BMC Infectious Diseases. 20-656.
- 17.P J Mwenda, Agnes Binagwaho. (2016) Parashar Umesh D. Effet de l'introduction du vaccin antirotavirus pentavalent sur les hospitalisations pour diarrhée et rotavirus chez les enfants au Rwanda. Lancet Global Health. 4(2) : e129–136 .
- 18.Akran V, Peenze I, Akoua-Koffi C, Kette H, de Beer MC. (2010) Caractérisation moléculaire et génotypage des souches de rotavirus humain à Abidjan. Côte d'Ivoire J Infect Dis .
- 19.Oppong T B, Yang H, Ampponsem-Boateng C, EKD Kyere, Abdullai T. (2020) Pathogènes entériques associés à la gastro-entérite chez les enfants de moins de 5 ans en Afrique subsaharienne : une revue systématique et une méta-analyse. Épidémiol Infect. 2, mars.
- 20.Waggie Z, Hawkridge A, Hussey G D. (1976) Examen des études sur le rotavirus en Afrique :. , J Infect Dis 202-1.
- 21.Kismul H, Acharya P, Mapatano M A. (2017) Haltey A ; Déterminants du retard de croissance chez l’enfant en République Démocratique du Congo : analyse approfondue de l’Enquête démographique et de santé 2013-14. Santé publique BMC. 1 aout. 18(1).
- 22.Mwenda J M, Ntoto K M, Abebe A, Enweronu-Laryea C, Amina I. (2010) . Burden and Epidemiology of Rotavirus Diarrhea in Selected African Countries : Preliminary Results from the African Rotavirus Surveillance Network. J Infect Dis 202(S1): S5–S .
- 23.Nitiema L W, Nordgren J, Ouermi D, Dianou D, Traore A S. (2011) Burden of rotavirus and other enteropathogens among children with diarrhea in Burkina Faso. 15(9) : e 646 , Int J Infect Dis 1, 52.
- 24.Godfrey O, Zhang W, Amponsem-Boateng C, Bonney Oppong T, Zhao Q et al. (2020) Evidence of rotavirus vaccine impact in sub-Saharan Africa : Systematic review and meta-analysis. PLoS ONE.
- 25.Athiyyah A F, Utsumi T, Wahyuni R M, Dinana Z, Yamani L N. (2019) Molecular Epidemiology and Clinical Features of Rotavirus Infection Among Pediatric Patients. in East Java, Indonesia During 2015–2018 : Dynamic Changes in Rotavirus Genotypes From Equine-Like G3 to Typical Human G1/G3. Front Microbiol [Internet] .
- 26.Gouandijka-Vasilache I, Manirakiza A, Gody J C, Banga-Mingo V, Kongombe O O. (2014) . Rotavirus Epidemiology in Bangui, Central African Republic, 20081. Emerg Infect Disease 20-7.
- 27.Athiyyah A F, Utsumi T, Wahyuni R M, Dinana Z, Yamani L N. (2019) Molecular Epidemiology and Clinical Features of Rotavirus Infection Among Pediatric Patients. in East Java, Indonesia During 2015–2018 : Dynamic Changes in Rotavirus Genotypes From Equine-Like G3 to Typical Human G1/G3. Front Microbiol [Internet] https://www. frontiersin.org/article/10.3389/fmicb.2019.00940 .
- 28.Gouandijka-Vasilache I, Manirakiza A, Gody J C, Banga-Mingo V, Kongombe O O. (2014) . Rotavirus Epidemiology in Bangui, Central African Republic, 20081. Emerg Infect Disease 20-7.
- 29.Raes M, Strens D, Vergison A. (2011) Réduction des hospitalisations pédiatriques liées au rotavirus après la vaccination universelle contre le rotavirus en Belgique. Pediatr Infect Dis J. 30 : e120–e125
- 30.Yıldızb İsmail.Impact of self-financed rotavirus vaccination on acute gastroenteritis in young children in Turkey a Clinic of Pediatrics, Ataşehir Memorial Hospital. b Clinic of Pediatrics, Şişli Memorial Hospital, Istanbul, Turkey VACCINS HUMAINS ET IMMUNOTHERAPEUTICS 2021, VOL , Istanbul, Turkey; 17, 510-516.
- 31.Sadiq A, Bostan N, Bokhari H, Matthijnssens J, Yinda Kwe C.Molecular characterization of human group A rotavirus genotypes circulating in Rawalpindi, Islamabad, Pakistan during 2015-2016, Plos/One Islamabad, Pakistan en 2015-2016. PLoS. ONE 14(7) : e 0220387.
