Scrotal Epidermoid Cyst Presenting as Extra-Testicular Scrotal Mass: A Diagnostic Dilemma
Abstract
We hereby report a scrotal epidermoid cyst presenting as a scrotal mass which a rare entity in the absence of trauma. 36years old male presents with a complaint of left sided testicular swelling and discomfort. The workup included clinical examination, alpha-fetoprotein (αFP) and beta-human chorionic gonadotropin (β-hCG) analyses and scrotal ultrasound. Clinically confused as testicular malignancy. Complete surgical excision of the cyst was performed. Histopathology confirmed epidermoid cyst with no evidence of malignancy.
Author Contributions
Academic Editor: Adil Khan, School of Computer Science and Technology, Harbin Institute of Technology, Harbin 150001, People's Republic of China.
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2020 Vaishali Shirale, et al.
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Introduction
Epidermoid cysts are common benign inclusion cysts occurring due to implantation of epidermal tissue into the dermis or subcutaneous tissues.1 Epidermoid cysts usually occur on scalp, ear, face and back. Scrotal localization can occur from developmental closure of the median raphe to include the epidermal tissue in which case they are located along the midline. Another route of implantation is through trauma.1 Epidermoid cyst is one of the benign lesions in the scrotum and can occur within the testis and in extra-testicular tissues. Scrotal and extra-testicular epidermoid cysts, as was the case in our patient, are very rare; the number of cases published in the English literature is less than 10.2
Case Report
A 36-year-old male presented in outpatient department with testicular discomfort and left scrotal swelling. He reported that the swelling appeared around two years back and has gradually progressed. There was no history of preceding trauma or any scrotal surgery. Initially he had no symptoms, until recently when he began to experience some discomfort during daily routine as dragging sensation.
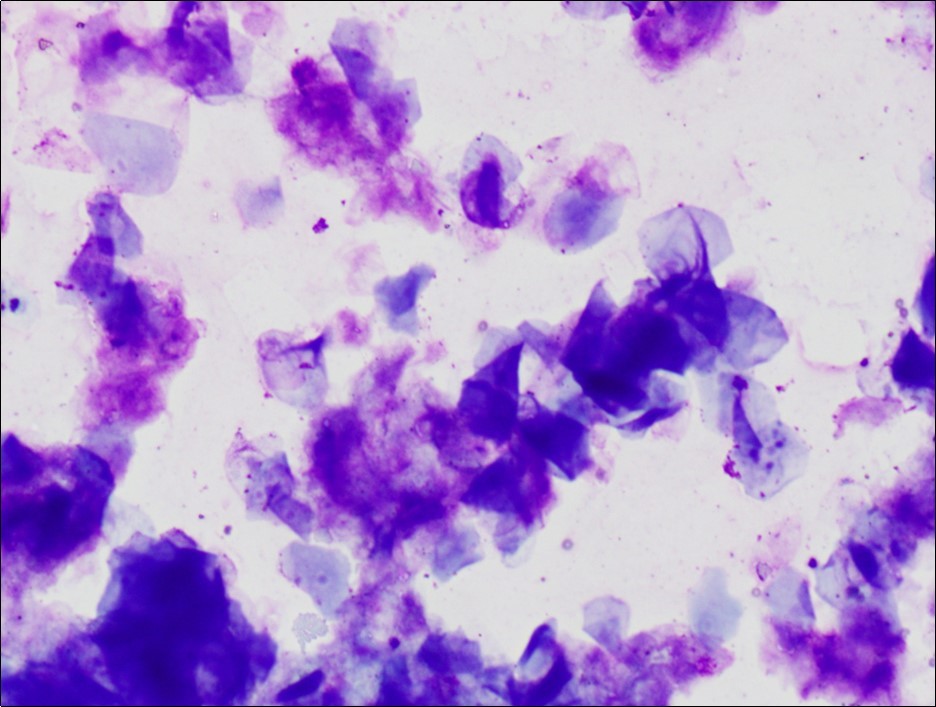
On physical exam, a well-defined cystic swelling of 10 x 4 cm size was palpable in the left scrotum (Figure 1). It was non tender and mobile within the subcutaneous tissue, with left testis palpable separately from the swelling. Trans-illumination test was negative. Scrotal ultrasound revealed a uniform, hypoechoic left extra-testicular lesion which appeared to be avascular. Alpha-fetoprotein (αFP) and beta-human chorionic gonadotropin (β-hCG) analyses were within normal limits. Fine needle aspiration revealed thick aspirate with cytological features suggestive of keratinous cyst (Figure 2).
Figure 1.Photo of scrotal swelling (testis separate from swelling)
The patient underwent excision of the mass. The mass was found to be inferolateral to the left testicle, but not originating from it (Figure 3). Complete excision was done and intraoperative findings revealed the cyst to be covered with a thin sac filled with necrotic, pultuscious material.
Figure 3.Operative picture showing testis separate from cyst
Histopathological findings revealed benign epidermoid cyst. The patient was seen at 3 months follow up. There was complete recovery with no postoperative complications.
Discussion
Epidermoid cysts are benign tumors consisting of a sac lined by stratified squamous epithelium filled with laminated keratin, cholesterol crystals, and debris.3 They have low malignant potential and are usually asymptomatic unless they become large enough to interfere with function, become infected, or rupture causing inflammation of adjacent structures. 3
Epidermoid cysts are divided into two types: congenital and acquired. 4 Although there are many theories about histogenesis, such as teratoma and metaplasia, the most likely explanation of epidermoid cysts throughout the body is an early intrauterine abnormal closure of neural groove or epithelial fusion lines.4, 5, 6 It has been reported in any place from the cranium to the anus in midline.4, 7 Epidermoid cyst is one of the benign lesions in the scrotum and can occur within the testis and in extra testicular tissues. Scrotal and extratesticular epidermoid cysts, as was the case in our patient, are very rare; the number of cases published in the English literature is less than 10. 2
Typical locations are scalp, ear, face and back and have been reported in perineum, penis, testis and scrotum. In our patient, the mass presented as a well-defined swelling in left scrotum palpable separate to left testis. Our patient denied any history of scrotal trauma or previous surgery. These extratesticular epidermoid cysts can be diagnosed earlier due to easy visibility, but some patients hesitate to visit doctor as in case in our patient. Tumor markers are of value as an initial workup for malignant lesions. 8 αFP, β-hCG and LDH in addition to routine biochemical tests were within normal limits. No additional hormonal analysis was carried out.
Ultrasound has become the gold standard for diagnosis of intra-scrotal lesions. It can differentiate the location of lesions as intra-testicular or extra-testicular and the content of the lesions as solid or cystic.9 For the intra-testicular lesions, the most famous ultrasound pattern is “onion skin” appearance formed by the enlarging cyst within the testis and the surrounding parenchyma forced outward. 5For extra-testicular lesions, a well-circumscribed mass can be seen, but the echotexture may be hypoechoic or hyperechoic depending on its content.10In our patient, scrotal ultrasound showed a hypoechoic, separate, extra-testicular, well-defined cyst.
In addition, magnetic resonance imaging (MRI) has become a popular tool in the evaluation of scrotal masses. On MRI, epidermoid cysts are described as high intensity well defined solid masses surrounded by a low signal capsule on T2-weighted imaging. 11
Although, scrotal extra-testicular lesions are usually benign in nature, the preoperative diagnosis of a scrotal epidermoid cyst is very difficult especially when presenting as an intra-scrotal mass. Extra caution should be used when it comes to the evaluation and management of these masses. Although epidermoid cysts are considered not to have malignant potential, malignant transformations have been reported and include basal cell carcinoma or squamous cell carcinoma. Complete excision is the treatment of choice.
Conclusion
We share a case of an extra testicular epidermoid cyst of the scrotum presenting as a scrotal mass. The mass presented with benign features on physical exam and on ultrasound imaging. Complete excision of the mass was done following thorough evaluation. Epidermoid inclusion cysts of scrotum are very rare, benign masses, with low malignant potential. Management should be scrotal exploration with testicular sparing resection as to prevent infection or rupture complications.
References
- 1.Yang W T, Whitman G J, GMK Tse. (2004) . , Extratesticular Epidermal Cyst of the Scrotum. Am J Roentgenol 1183(4), 1084-1084.
- 2.Sağlam H S, Kumsar S, Köse O, Adsan O. (2013) A unique scrotal extratesticular epidermod cyst attached to the seminal vesicles. , Can Urol Assoc J J Assoc Urol Can.7(3-4): 244-247.
- 3.Shah K H, Maxted W C, Chun B. (1981) Epidermoid cysts of the testis: a report of three cases and an analysis of 141 cases from the world literature. , Cancer 47(3), 577-82.
- 4.Pear B L. (1970) Epidermoid and dermoid sequestration cysts. , Am J Roentgenol Radium Ther Nucl Med 110(1), 148-55.
- 5.Malvica R P. (1993) Epidermoid cyst of the testicle: an unusual sonographic finding. , AJR Am J Roentgenol 160(5), 1047-8.
- 6.Lee S J, Lee J H, Jeon S H, Kim M J. (2010) Multiple epidermoid cysts arising from the extratesticular scrotal, spermatic cord and perineal area. , Korean J Urol 51(7), 505-7.
- 7.Suwa M, Takeda M, Bilim V, Takahashi K. (2000) Epidermoid cyst of the penis: a case report and review of the literature. , Int J Urol Off J Jpn Urol Assoc 7(11), 431-3.
- 8.Loya A G, Said J W, Grant E G. (2004) Epidermoid cyst of the testis: radiologic-pathologic correlation. Radiogr Rev Publ Radiol Soc N Am Inc.24Suppl1: 243-246.
- 9.Lee H S, Joo K B, Song H T, Kim Y S, Park D W et al. (2001) Relationship between sonographic and pathologic findings in epidermal inclusion cysts. , J Clin Ultrasound JCU 29(7), 374-83.
Cited by (2)
This article has been cited by 2 scholarly works according to:
Citing Articles:
Pan African Medical Journal (2024) OpenAlex
The Pan African Medical Journal (2024) Crossref