Compression between Combined Anti-VGEF with Steroids Versus Pure Anti-VEGF in Retinal Vein Occlusion
Abstract
Aim
To compare the efficacy of combined anti-VGEF (IVB) with steroids versus pure anti-VEGF for the treatment of macular edema secondary to retinal vein occlusion (RVO).
Methods
In this prospective study, 51 eyes were randomized into 2 groups according to treatment of clinically identified macular edema secondary to retinal vein occlusion within 4 weeks of onset: Group 1 (19 eyes) was given intravitreal Bevacizumab (IVB) (1.25mg/.05ml) + Triamcinolone (IVTA) (2mg/.05ml); Group 2 (22 eyes) was given pure intravitreal Bevacizumab (IVB) (1.25mg/.05ml) at baseline, at month 1, and at month 2. The outcome of the study represented the EDRTS letters gain, IOP change and (CRT) by using Spectral domain optical coherence tomography (OCT) at month 1, 2, 3 and 6 in each group. Both central retinal vein occlusion (CRVO) and branch retinal vein occlusion (BRVO) patients with at least 6 months FU were enrolled in the study.
Results
EDRTS letters gain was (20.37±15.28, 28.05±16.68, 35.16±17.12, 36.47±18.17) in group1 and (14.50±14.56, 18.41±14.56, 20.59±16.13, 21.06±15.72) in group2 at month 2,3 and 6 p value (0.18, .04, 0.004, 0.002). Mean IOP pre-injection (14.00±2.67) in group 1 and (13.5±5.89) in group 2. Group 1 has transient increase in IOP at month 1 and then return to baseline over 6 months. CRT from baseline to final FU decrease by 264.82 (µm) ±147.66 in group 1 and 308.42(µm) ±226.78 in group 2 with no significant difference between two group p value 0.57. There was no significant difference in EDRTS letters gain between CRVO patients and BRVO patients at month 1, 2, 3 and 6 p values (0.83, 0.23, 0.29, 0.13).
Conclusion
Early treatment macular edema in RVO patients by combined anti-VGEF+ steroid effectively improve functional outcome better than pure anti-VGEF injection.
Author Contributions
Academic Editor: Ntodie M, Department of Optometry, University of Cape Coast, Cape Coast, Ghana.
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2020 Eman Abo Taleb, et al.
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Introduction
Retinal vein occlusion (RVO) is the second most common retinal vascular disease after diabetic retinopathy and is estimated to affect 16 million adults worldwide, with a reported prevalence of 4.6% in those aged 480 years 1 Decreased blood flow through the retinal vasculature results in tissue ischemia, up regulates vascular endothelial growth factor (VEGF), breaks down the blood–retinal barrier, and causes vision loss primarily because of macular edema.2
In the nearly two decades following the publication of the Branch Retinal Vein Occlusion Study (BVOS) and Central Retinal Vein Occlusion Study (CVOS), pharmacologic therapy for retinal vein occlusion (RVO) was almost nonexistent. However, the introduction of intravitreal therapy-namely corticosteroids and anti-VEGF agents-has provided a host of new pharmacologic options to clinicians. As evidenced by several large-scale clinical trials,3, 4, 5, 6 intravitreal monotherapy is effective for the vast majority of patients with RVO and has thus become the predominant therapeutic approach. 7
Unfortunately, a small minority of patients display recalcitrant macular edema despite frequent intravitreal monotherapy dosing. In the SCORE trials, 11.6% to 12.0% of patients treated with repeated intravitreal triamcinolone lost at least 15 letters, and more than 20% had central point thicknesses greater than 500 μm at 12-month follow-up.3, 4 although the rate of refractory edema was lower in the BRAVO/CRUISE trial (0.7% to 3.8% lost at least 15 letters, and 6.7% to 15.9% had central foveal thickness greater than 400 μm at 12 months), frequent ranibizumab monotherapy was not universally successful. 5, 6 Such recalcitrant cases have prompted the search for therapeutic alternatives, most notably combination pharmacologic and pharmaco-laser treatments.
AntiVEGF agents and steroids appear to have some overlap in their functions of bloodretinal barrier consolidation and VEGF down regulation, but their precise biologic role in combination has not been clearly elucidated
Most recently, the antiVEGF agent ranibizumab and the dexamethasonecontaining Ozurdex implant have been approved by the FDA for the treatment of macular edema secondary to BRVO and CRVO. AntiVEGF agents and steroids including Ozurdex implant have been used in conjunction in a small prospective, noncomparative trial.8 The purpose of this study is to compare the efficacy of combined IVB and IVTA versus pure IVB in patients with early onset macular edema secondary to RVO.
Materials and Methods
This prospective, institutional, single-masked, randomized trial was approved by the institutional review board Quorum International. Each subject provided written informed consent before enrollment. From March 25, 2015, to October 30, 2019, 51 subjects were enrolled in the study.
Eligible patients had macular edema of less than 4 week’s duration due to BRVO or CRVO, with central Retinal thickness (CRT) > 250 μm as measured by time-domain optical coherence tomography (Stratus®; Carl Zeiss Meditec, Inc, Dublin, CA, USA). Exclusion criteria included evidence of other retinal or retinal pigment epithelial abnormalities, a previous vitrectomy or preexisting glaucoma. The amount of retinal ischemia was not an exclusionary factor.
Subjects in this cohort were randomly assigned 1:1 to one of two study groups. Group 1 (19 eyes) was given IVB (Avastin®; Genentech, South San Francisco, CA, USA/Roche, Basel, Switzerland) (1.25mg/.05ml) and IVTA (Kenacort suspension 40mg/1ml) (2mg/.05ml); Group 2 (22 eyes) was given pure (IVB) (1.25mg/.05ml).
The risks and benefits of the offlabel use of IVB and IVTA were discussed with patients prior to administration of the injections and informed consent was obtained. The injections were administered in a standard sterile fashion including betadyne preparation and use of a lid speculum in a designated injection room in an ophthalmology clinic. In group 1 Bevacizumab (1.25mg/.05ml) was mixed with triamcinolone (2mg/.05ml) in the same (29 G/1 ml) insulin syringe and both drugs were simultaneously administered 3.5mm posterior to the limbus, gentle scleral massage with Cotton tip was applied, One drop of diluted betadyne put in the lower fornix of the conjunctiva and the eye is covered for 2 hours after the injection. Instruction was given to all patients to remove the eye cover after 2 hours and start combined anti-biotic/dexamethasone eye drop every 4 hours for one week. Group1 patients were seen on the second day to measure their intraocular pressure IOP.
Group 1 patients were given combined (IVB+IVTA) 3 consecutive injection1 months apart. Also group 2 patients were given pure (IVB) 3 consecutive injection 1 month apart. Both group patients were followed for another 3 month after the last injection.
Patient characteristics reviewed were age, gender, diagnosed diabetic mellitus (DM) or hypertension (HT), previous ocular interventions (i.e. laser photocoagulation) and duration of vein occlusion symptoms. Visual acuity in Early Diabetic Retinopathy Treatment Study (EDRTS) letters score, (IOP in mmHg), and central retinal thickness (CRT in μm) by Spectralis optical coherence tomography (OCT) were measured for each patients in both group pre and on each post injection F/U at 1, 2, 3, and 6 months.
Statistical Analysis
Mean was used for description of quantitative data, and percentages were used for qualitative data. Univariate analyses, such as the chi-square test were used to compare qualitative data; where as independent t-test was used to compare quantitative data after normal distribution was checked. Repeated measures analysis of variance (ANOVA) corrected by the Bonferroni method was used to compare the mean BCVA in EDRTS letters score, CRT, IOP and letters gain among each postoperative period in the same group after normal distribution was checked. Independent t-test was calculated to compare mean BCVA in EDRTS letters scores, CRT, IOP and letters gain at each postoperative period between the two groups after normal distribution was checked. Statistical analyses were doneusing SPSS statistical software (version 14.0; SPSS,Inc., Chicago, IL). For all statistical tests, P ≤ 0.05 was considered significant.
Results
Baseline Characteristic
There was no statically significant difference between both group in all the baseline characteristic including age, sex, number of CRVO and BRVO patients, lens status, previous PRP laser, presenting BCVA, IOP , CRT……Baseline characteristics of the two treatment groups are shown in Table 1.
Table 1. Baseline characteristics| Initial characteristics | Bevacizumab + triamcinolone group1 N=19 | Pure Bevacizumab group2 | P-value |
| N=22 | |||
| Age in years, mean ± SD | 58.68 ± 11.06 | 53.41 ± 11.63 | .12† |
| Sex, N | |||
| Male | 10 | 16 | 0.56* |
| Female | 9 | 16 | |
| Type 2 diabetes, N | |||
| Yes | 4 | 9 | 42* |
| no | 15 | 23 | |
| 6 | 13 | 56* | |
| 13 | 19 | ||
| Type of vein occlusion, N | |||
| CRVO | 11 | 8 | |
| BRVO | 16 | 16 | 77* |
| Lens status, N | |||
| Phakic | 18 | 32 | .37* |
| PC IOL | 1 | 0 | |
| Peripheral laser photocoagulation (PRP) | |||
| Yes | 8 | 11 | |
| no | 11 | 21 | .40* |
| Presenting BCVA (letters), mean ± SD | 19.84 ±21.81 | 24.3750±22.50 | .49† |
| Presenting CRT( µm), mean ± SD | 555.07 ±173.11 | 572.00±189.66 | .78† |
| Presenting IOP( Hmg), mean ± SD | 14.05±2.73 | 14.5313±4.59 | .68† |
| Duration of symptoms (weeks) mean ± SD | 3.92±3.62 | 3.21±7.392 | .69† |
Effect of Treatment on VA, IOP and CRT
(Figure 1) reveals time course of changes in visual acuity in both groups. Best-corrected visual acuity significantly improved by the treatment in both group. Best-corrected visual acuity significantly improved at all time points compared with baseline in group 1 and group 2 (P < 0.0001).
Figure 1.Best-corrected visual acuity significantly improved at all time points compared with baseline in group1 and group 2. Repeated measure ANOVAs (P < 0.0001).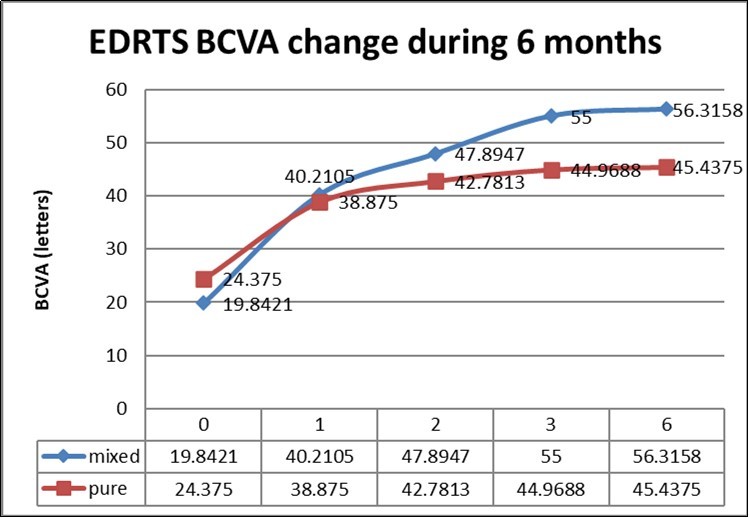
After month 1from the first injection EDRTS letters gain was (20.37±15.28) in group 1 and (14.50±14.56) in group 2. Although there is 6 letters gain more in combined group p value was (0.18) not significant. At month 2 after the second injection EDRTS letters gain was (28.05±16.68) in group 1 whereas group 2 was only (18.41±14.56) with significant p value (.04). At month 3 after the third injection EDRTS letters gain was (35.16±17.12) whereas group 2 were only (20.59±16.13) with significant p value (0.004). After 6 months from the first injection EDRTS letters gain was (36.47±18.17) in group 1 whereas group 2 was only (21.06±15.72) with significant p value (.002). Independent t-test was used to compare between both groups. Figure 2.
Figure 2.EDRTS letters gain in group 1 is more than group 2 during 6 months of F/U with significant p value independent sample t-test.
Although EDRTS letters gain is more in CRVO then BRVO P value still not significant in all months of F/U. Figure 3.
Figure 3.EDRTS letters gain in CRVO is more than BRVO during 6 months of F/U with not significant p value independent sample t-test.
In group1 IOP transiently increased 1 month after injection in 5 patients (25%), but returned to baseline levels with one topical beta blocker. Each of those 5 patients was successfully withdrawn from the topical medication at 6 months with restoration of IOP to baseline levels. Figure 4.
Figure 4.Transient increase and then return to baseline of mean intraocular pressure over 6 months in group 1.
Central retinal thickness also showed significant improvement by the treatment in both group (P< 0.0001). Figure 5.
Figure 5.CRT significantly decrease pre and post the 3 injections.
Safety
No serious safety concerns emerged in the study. There were no cases of endophthalmitis, retinal detachment, or traumatic cataract occurred in this series.
Discussion
Current understanding of mechanism of action of these treatment is that Intravitreal bevacizumab likely treats macular edema through countering VEGF-mediated permeability, and intravitreal triamcinolone likely reduces inflammation, limits extravasation from blood vessels, and stabilizes endothelial cells. Thus, their effects in reducing macular edema may be through different pathways. It is also known that intravitreal bevacizumab has a much shorter half-life compared to intravitreal triamcinolone. Combined IVB and IVT may allow a prolonged efficacy against macular edema through different pathways, explaining a reduced number of intravitreal injections required to achieve prompt and sustained decrease in macular edema. It follows that fewer administered injections will reduce the risk of elevated IOP associated with corticosteroids.9
Ehrlich et al,10previously investigated the combined treatment of IVB and IVT in patients with RVO.In their study the authors found no advantage of combined IVT and IVB over IVB alone in the treatment of retinal vein occlusion. However, their study had important differences in the power of their study population and interval to intervention. Their study had a small number (n=16) of patients and the mean time from RVO diagnosis to injection was 9 months. Although not clearly reported, these patients may have had macular edema for 9 months as well, with potential irreversible photoreceptor damage after chronic macular edema that would yield poorer visual outcomes. 11 In our study, early intervention (less than 4 weeks) was offered to patients. Our study further supported early intervention in that patients with the shortest identification to treatment time experienced the greatest gains in visual acuity.
Rasha I Ali et al,9 in their study prove that the early combined treatment with IVB and IVT is effective in improving anatomic and functional outcomes in patients with macular edema secondary to BRVO with lack of a control arm. Although our results support their results, the power of our study is more as it is a comparative study.
Our administration of the combined drugs to the vitreous is through one single injection by mixing both drugs in one 29 G insulin syringe. This way of administration which differs from the ways in the previous studies will definitely lessen the complication of two entrance site to the vitreous.
In the last 5 years, Michael Singer et al, 12 and others 10, 13, 14 have studied the effects of combining anti-VEGF medications with dexamethasone intravitreal implants to determine improvement in visual acuity, CFT (central foveal thickness) and the sustainability of multiple applications of combination therapy in RVO. Michael et al, 12 studies showed that the addition of dexamethasone intravitreal implant 2 weeks following anti-VEGF therapy provides improvements in best corrected visual acuity and macular thickness in patients with retinal vein occlusion. Singer MA et al, 10 also examine the efficacy of combined dexamethasone intravitreal implant with bevacizumab in RVO and they conclude that there is synergistic in combination therapy increasing visual acuity and prolonging the time between injections. These studies support our result even though we have used different type of steroid Triamcinolone (2mg/0.5ml) which is much cheaper than dexamethasone intravitreal implant and still has the job especially at developing country where they still consider dexamethasone intravitreal implant very expensive.
References
- 1.Klein R, Moss S E, Meuer S M, Klein B E. (2008) The 15-year cumulative incidence of retinal vein occlusion: the Beaver Dam Eye Study. Arch Ophthalmol. 126(4), 513-518.
- 2.Rehak J, Rehak M. (2008) Branch retinal vein occlusion: pathogenesis, visual prognosis, and treatment modalities.CurrEye. Res.33: 111-131.
- 3.Ip M S, Scott I U, VanVeldhuisen P C. (2009) A randomized trial comparing the efficacy and safety of intravitreal triamcinolone with observation to treat vision loss associated with macular edema secondary to central retinal vein occlusion: the Standard Care vs Corticosteroid for Retinal Vein Occlusion (SCORE) study report 5.ArchOphthalmol. 127(9), 1101-1114.
- 4.Scott I U, Ip M S, VanVeldhuisen P C. (2009) A randomized trial comparing the efficacy and safety of intravitreal triamcinolone with standard care to treat vision loss associated with macular Edema secondary to branch retinal vein occlusion: the Standard Care vs Corticosteroid for Retinal Vein Occlusion (SCORE) study report 6.ArchOphthalmol. 127(9), 1115-1128.
- 5.Brown D M, Campochiaro P A, Bhisitkul R B. (2011) Sustained benefits from ranibizumab for macular edema following branch retinal vein occlusion: 12-month outcomes of a phase. , III 118(8), 1594-1602.
- 6.Campochiaro P A, Brown D M, Awh C C. (2011) Sustained benefits from ranibizumab for macular edema following central retinal vein occlusion: twelve-month outcomes of a phase III study.Ophthalmology. 118(10), 2041-2049.
- 7.Jumper J M, Mittra R A. (2011) Preferences and trends survey. , [Online].http://www.asrs.org/asrs-community/pat-survey/pat-survey-archive. Accessed 27.
- 8.Singer M A, Bell D J, Woods P. (2012) Effect of combination therapy with bevacizumab and dexamethasone intravitreal implant in patients with retinal vein occlusion.Retina. 32(7), 1289-1294.
- 9.Rasha I Ali, Kapil G Kapoor, Adeel N Khan, Syed K Gibran. (2014) Efficacy of combined intravitreal bevacizumab and triamcinolone for branch retinal vein occlusion. , Indian Journal of Ophthalmology 62, 4.
- 10.Jaissle G B, Szurman P, Feltgen N, Spitzer B, Pielen A.Rehak M,et al.(2011). Retinal Vein Occlusion Study Group. Predictive factors for functional improvement after intravitreal bevacizumab therapy for macular edema due to branch retinal vein occlusion. Graefes Arch Clin Exp Ophthalmol. 249, 183-192.
- 11.Ehrlich R, Ciulla T A, Moss A M, Harris A. (2010) Combined treatment of intravitreal bevacizumab and intravitreal triamcinolone in patients with retinal vein occlusion: 6 months of followup. Graefes Arch Clin Exp Ophthalmol. 248, 375-380.
- 12.Singer Michael, Tyler Lyndon, Jansen Michael, Jana.. Waters.(2016). Comparison of Anti-VEGF, Steroid, and Combination Therapy in the Treatment of Retinal Vein Occlusion 2, 2.
- 13.Singer M A, Capone A Jr, Dugel P U, Dreyer R F, Dodwell D G et al. (2015) SHASTA Study Group. Two or more dexamethasone intravitreal implants as monotherapy or in combination therapy for macular edema in retinal vein occlusion: subgroup analysis of a retrospective chart review study.BMCOphthalmol. , Apr 1, 15-33.
Cited by (1)
This article has been cited by 1 scholarly work according to:
Citing Articles:
