Improving Effective Screening and Management of Obesity in an Urgent Care Clinic
Abstract
Background
Nearly 40% of the adult population in the United States are considered obese by current standards, which equates to approximately 93 million people. Obesity is a chronic disease that is linked to more than 40 other diseases, including hypertension, heart disease, stroke, diabetes, and at least 13 distinct types of cancers. The direct and indirect costs of obesity have been estimated at up to $210 billion annually.
Local Problem
In Cumberland County, North Carolina, 34% of the adult population was considered obese. The aim of this quality improvement study was to increase effective care (screening, patient engagement, and referral to treatment) in adult patients with a BMI greater than 30 kg/m2 to 75% within 90 days.
Methods
A rapid cycle plan-do-study-act framework was used to evaluate four focus areas concurrently over 8 weeks with a small test of change completed in each 2-week cycle.
Interventions
An expanded screening with a checklist, shared decision-making tools (SDMTs), and a referral to treatment checklist were implemented. Activities from the team engagement plan were initiated.
Results
The effective care of patients increased by 42 percentage points while engaging both the patients and the staff.
Conclusions
Utilizing standardized communication, SDMTs, checklists, and management plans improved effective care while motivating and enabling patients to take control of their care and make sustainable lifestyle changes that enhance overall health.
Author Contributions
Academic Editor: Fatih Ozcelik, University of Health Sciences Turkey, Sultan. Abdulhamid Han Training and Education Hospital, Department of Biochemistry
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2023 Heather
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Introduction
The most current reports estimated that nearly 40% of the adult population aged 18 and over are obese, defined as having a body mass index greater than 30 kg/m2, which equates to almost 93 million people 5. This is significant because the inherent risks are linked to 40 diseases including hypertension, heart disease, stroke, diabetes, and at least 13 distinct types of cancers 2. The Robert Wood Johnson Foundation 19 reports that spending on obesity is between $147 and $210 billion annually. The American Association of Clinical Endocrinologists (AACE) and the American College of Endocrinology (ACE) recommend screening all adults for overweight and obesity as well as initiating weight management 10. Data from the clinical site showed that 60% of patients were screened for body mass index (BMI), while waist circumference (WC) was not measured per AACE/ACE recommendations. There was no utilization of SDMTs. Further data revealed that only 24% of patients were receiving effective care for obesity management. Team data showed that 43% of staff feel that there is a need for standardized processes and engagement of the team.
Available Knowledge
The Obesity Society 13 indicates obesity is not only a contributing factor to multiple health conditions but a chronic disease in its own right. Multiple agencies, including the AACE, American Heart Association, World Health Organization, and the National Institute for Health share the same consensus in guidelines that recommend the use of body mass index (BMI), waist circumference (WC), and additional patient risk factors in screening for obesity on a yearly basis 8, 14. Best practices included encouraging physical activity, decreasing calorie intake, assessing readiness to change as well as barriers to change, screening for co-morbidities, monitoring medication therapy, and using pharmacotherapy with comprehensive lifestyle changes 3, 4, 14. Nonetheless, there are numerous gaps in obesity care from screening recommendations, to diagnosis, to a consensus on what constitutes best practices in and how to standardize care.
Rationale
Effective healthcare defined by the Institute of Medicine (IOM) focuses on aiding those who need it based on a specific set of data while avoiding misuse and underutilization 1. Effective care was implemented utilizing SBIRT (screening, a brief intervention, and referral to treatment), which provides a concise, universal, and comprehensive framework. The aim of this quality improvement study was to increase effective care (screening, patient engagement, and referral to treatment) in adult patients with a BMI greater than 30 kg/m2 to 75% within 90 days.
Methods
This project was implemented at QwikMed Pharmacy and Clinic, a private urgent care clinic within house pharmacy, open seven days a week, located in urban east North Carolina. It employs three nurse practitioners (one per shift), one pharmacist, two pharmacy technicians, and several part-time pharmacists. The nurse practitioner saw a combination of 10 to 25 sick and weight loss patients daily on a walk-in basis. Patients were of various ages, socioeconomic, and diverse backgrounds. The weight loss program is a self-pay program, so no insurance was accepted or filed.
This project was a rapid-cycle quality improvement process that included four plan-do-study-act (PDSA) cycles for four interventions over 90 days. Every 2 weeks during this iterative process, a small test of change was initiated or modified and evaluated for improvement. The “plan” consisted of the test of change, learning objectives, and predictions. The “do” utilized field notes, run charts, and aggregate data files. The “study” was comprised of what was learned from the predictions and analyzing the data to inform the “act” for the subsequent cycle 17.
Interventions
The project started with four core interventions related to screening, patient engagement, referral to treatment, and team engagement. All patients presenting for weight loss were screened with BMI and waist circumference for improved identification and management initiation. Patients were educated on the correlation between BMI and waist circumference, stressing the health risks of obesity. Each patient was asked to complete a readiness to change questionnaire and a menu for action to incorporate personalized goals. To ensure best practices and needs were being met, a referral to the treatment log, which had 10 specific targets, was completed. A team engagement plan was prepared to educate and empower the staff while augmenting teamwork in the change process. Further interventions and modifications are found in Table 1.
Table 1 . Tests of Change| PDSA cycle 1 | PDSA cycle 2 | PDSA cycle 3 | PDSA cycle 4 | |
| Screening | Implement Obesity Screening Checklist | Put waist circumference reminders in exam rooms | Highlight waist circumference on the screening checklist as an additional reminder | Add a sticker to charts specifically for waist circumference |
| Patient Engagement/ Experience of care | Implement Ready to Change Questionnaire and Menu for Action | Implement revised Menu for Action | Have techs give SDM to patients prior to the visit | Implement revised Ready to Change Questionnaire |
| Referral to Treatment | Initiate Referral checklist | Initiate a reminder card for patients | Initiate logbook of patients that need to be followed up | Initiate contest (drawing) for extrinsic motivation |
| Teamwork/ engagement | Implement the Vision Board and One-on-One teaching | Implement team huddles and teleconferences | Contest for the team member with the highest percentage of completed project-specific tasks | Implement a pre/posttest for obesity bias |
Study of Interventions
Qualitative and quantitative data were obtained through chart audits, SDMTs, and referral checklists every 3 days, while staff survey data was collected every 14 days over the four PDSA cycles. The information was then used to evaluate each intervention and the influence it had on effective care 17.
Data points were recorded on run charts and evaluated for shifts, trends, and runs to determine if the interventions were effective or needed modification. Evaluations and changes were made on a bi-weekly basis during this iterative process.
Measures
A total of 10 measures were evaluated, which included the aim, a process, and an outcome for each of the four interventions and a balancing measure. The measurement worksheet (Table 2) provides operational definitions related to each of the 10 measures. Outcome measures included a screening and referral checklist to track qualifying patients, a validated readiness to change questionnaire, and a menu for action to promote patient engagement, explaining the stages of change and encouraging small meaningful goals. A team engagement plan was devised to motivate and foster enhanced collaboration and communication.
Table 2. Measurements Worksheet.| TOC/Core Intervention Tool & Hyperlink | Measure | Operational Definition (Numerator / Denominator or Mean Score) | Baseline % | Goal % | Final % |
| AIM: Increase effective care (screening, patient engagement, referral to treatment) in adult patients with a BMI >30 kg/m 2 to 75% within 90 days. | Total # of effective care points/total # points (Average percent of screening, patient engagement, referral/3) | 33 | 75 | 75 | |
| Screening | Process: | # of patients screened /# of adult weight loss patients | 69 | 75 | 95 |
| Outcome: | # of adults with BMI > 30 kg/m2 /total # of adult weight loss patients screened | 55 | 75 | 79.4 | |
| Patient engagement | Process: | # tools completed/# of adults with BMI > 30 kg/m2seen | 50 | 75 | 87.8 |
| Outcome: | # of adults ready to change and/or 1 weekly goal set/# tools completed | 30 | 50 | 92 | |
| Referral to Treatment https://docs.google.com/document/d/1s8j76Spf23wIvJKH3WJ7ivmNMDTBhfx49EbPgmuJd7g/edit?usp=sharing | Process: | # of checklists completed/# of adults with a BMI > 30 kg/m2seen | 50 | 75 | 72.4 |
| Outcome: | Average percent of score of right care # of checklist items completed/10 | 24 | 50 | 66.5 | |
| Team Engagement Plan https://docs.google.com/document/d/1I9yPWH0qev6TpNMXtlFBQbya_Q4vBaHUznsblbvPqco/edit?usp=sharing | Process: | # of responses/attendance of encounters/# encounters/meeting attendance | 50 | 25 | 84.8 |
| Outcome: | Average of ATOP Survey (78 possible)Average of BAOP survey (48 possible) | 6521 | 7025 | 6519.4 | |
| Balancing Measure: Job Satisfaction will not decrease from baseline average on a 1-5 Likert Scale | Mean Likert Scale Satisfaction Survey | 4.7 | 4.7 | 4.125 | |
A staff satisfaction survey was incorporated to ascertain if the increased workload had a negative impact. All the weight loss charts were reviewed by the project team lead, and the result was shared with the team to ensure the completeness and accuracy of the data.
Analysis
Quantitative data from checklists, surveys, and Likert-scales was plotted on run charts and evaluated for impact based on a calculated median and set goal. Qualitative data from SDMTs was collected, tracked in aggregate data worksheets, and used to identify patterns. This doctoral project was excused from review by the Institutional Review Board at Frontier Nursing University because it does not qualify as human subjects research and meets federal requirements for quality improvement. No outside funding for this project was received.
Results
Throughout the four rapid PDSA cycles, a total of 133 patients were included in the project. The patient screening, patient engagement, and referral to treatment interventions all had improved scores from the baselines, which enhanced the effectiveness of care. Identification of a realistic goal each week motivated the patients to do more and increased their confidence. Referral to treatment had small gains (see Table 3). Team engagement had variations; however, participation was improved when huddles and face-to-face interactions were utilized.
Screening
In PDSA 1, the screening checklist was implemented, and 38 patients were screened for height, weight, and BMI accounting for a 41.2% increase. The height, weight, and BMI were completed 100% of the time in the last three PDSA cycles. WC was obtained at 65.8% in PDSA1. After receiving feedback that providers were not remembering to measure it, PDSA 2 introduced a reminder card for obtaining the WC on the screening checklist. It proved to be successful as there was a 25.2% increase in WC recordings. PDSA 3 placed more emphasis on obtaining a WC by highlighting it on the screening checklist which increased it modestly by another 2.42%. PDSA 4 included one final reminder to obtain WC by placing a sticker on all the charts, which was the most successful intervention, resulting in 92.9% being screened.
Patient Engagement
Ready to Change Questionnaire (RTC) and the Menu for Action (MFA) were both implemented in PDSA 1. In PDSA 1, 71.1% of patients completed the tool, with an average RTC score of 23, improved from a baseline of 22.6. In PDSA 2, 76.5% of patients were ready to initiate a change scoring of 24. PDSA 3, had 93.3% of patients submitting the RTC tool with an average score of 24.3. The revised RTC tool in PDSA 4, showed 85.7% of patients were ready to take action with a slightly lower average score of 23.5. The MFA had 81.6% of patients choosing a goal in PDSA 1. During PDSA 2, 94.1% of patients decided on a goal. In PDSA 3, the pharmacy technicians provided the MFA to patients before seeing the provider, proving the most impactful intervention, with 97% of patients committing to a goal. The MFA was used with 100% of patients in PDSA 4. The most common goals for the MFA in each PDSA cycle were increasing physical activity and increasing daily water intake.
Referral to Treatment
In PDSA 1, data showed the referral checklist was used with varying degrees dependent on the checklist item with an average mean percent total of 15.2% over the baseline. The average mean percent total increased in PDSA 2 by 8.2 percentage points after initiating a reminder card. When a logbook was introduced in PDSA 3, there was a decrease in the use of the referral checklist of 3.47%. The completion of the checklist increased 8.2 percentage points in PDSA 4. Significant omissions included lipid and HgbA1C levels, food trackers, and blood pressure not at goal (Table 3).
Table 3. Referral to Treatment Aggregate Data| PDSA 1 38 (100%) | PDSA 2 34 (100%) | PDSA 3 33 (100%) | PDSA 4 28 (100%) | Total 133 (100%) | |
| Referral to Treatment Targets | |||||
| Blood pressure <130/80 | 16 (42.1%) | 11 (32.4%) | 8 (24.2%) | 15 (53.6%) | 50 (37.6%) |
| Tobacco Screening | 32 (84.2%) | 32 (94.1%) | 33 (100%) | 28 (100%) | 125 (94%) |
| Regular Exercise | 24 (63.2%) | 19 (55.9%) | 14 (42.4%) | 18 (64.3%) | 75 (56.4%) |
| Current Medication Review | 38 (100%) | 34 (100%) | 33 (100%) | 28 (100%) | 133 (100%) |
| Lipid Level | 4 (10.5%) | 12 35.3%) | 11 (33.3%) | 10 (35.7%) | 37 (27.8%) |
| HgbA1C Level | 5 (13.2%) | 13 (38.2%) | 10 (30.3%) | 10 (35.7%) | 38 (38.6%) |
| Food Tracker | 6 (15.8%) | 15 (44.1%) | 9 (27.3%) | 12 (42.9%) | 42 (31.6%) |
| Health History < 6 months old | 37 (97.4%) | 32 (94.1%) | 33 (100%) | 28 (100%) | 130 (97.7%) |
| Prescribed Phentermine | 34 (89.5%) | 34 (100%) | 33 (100%) | 28 (100%) | 129 (97%) |
| Referral to PCP/Nutrition or Follow up in Clinic | 23 (60.5%) | 23 (67.6%) | 27 (81.8%) | 25 (89.3%) | 98 (73.7%) |
Lipid level compliance increased by 25.2 percentage points between PDSA 1and PDSA 4 HgbA1C compliance improved from PDSA 1 to PDSA 4 by 22.5 percentage points. Food trackers were returned 15.8% in PDSA 1 and increased 27.1 percentage points by PDSA 4. Blood pressure at goal showed a 27% increase from PDSA 1 to PDSA 4. Extrinsic motivation in the form of an incentive prize drawing was attempted to improve patient compliance for individual items, which was minimally successful.
Team Engagement
Team engagement for PDSA 1 was 75.5% with the introduction of the team engagement plan and increased to 93.1% by PDSA 4. Survey data showed that Attitudes Towards Obese Persons (ATOP) at baseline was 65 of a possible 78 and had risen by 3.6% at the end of PDSA 4 indicating a positive attitude regarding obesity as a disease. The Beliefs About Obese Persons (BAOP) at baseline was 21 of a possible 48 and showed an 8.2% drop at the end of PDSA 4 indicating a personal bias that the individual is to blame for their obesity (Figure 1). A total of 23 questionnaires were collected over the four PDSA cycles, twice during PDSA 1 then only once in the remaining cycles. Staff satisfaction, a balancing measure, demonstrated a significant regression of 17.1% from a baseline of 4.7 of a possible five in PDSA 1, showing the negative consequences of the added workload. By PDSA 4 staff satisfaction had improved but remained below baseline by 1.2%.
Figure 1.Mean Team Values Regarding Obesity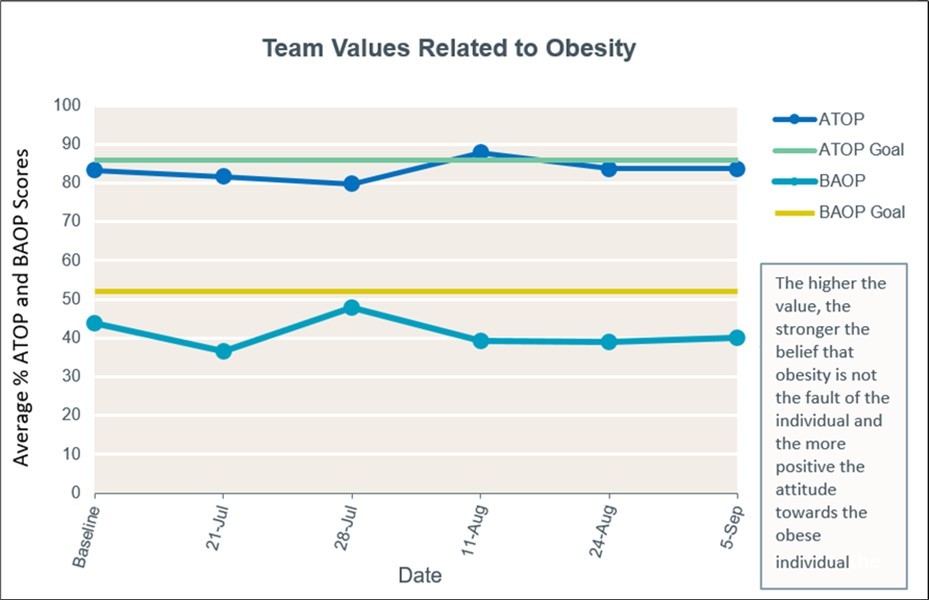
Figure 1. ATOP and BAOP surveys showed that there were mostly positive attitudes towards our obese patients but some of the staff held biases believing it was the individual’s choice or lack of action as the cause of obesity.
Discussion
The aim of this quality improvement study, to increase effective care (screening, patient engagement, and referral to treatment) in adult patients with a BMI greater than 30 kg/m2 to 75% within 90 days, was achieved. Effective care increased by 42 percentage points. Screening and identification of high-risk patients increased by 44.4%. Patient engagement improved by 62 percentage points. Team engagement had many variations with both downward and upward trends that were partially affected by the timing of the requested surveys being completed and the mix of staff type. Identification of obesity and patient engagement were the strengths of this project. Effective care had several areas of concern in the beginning, including labs, food tracking, and blood pressure at goal.
Interpretation
This initiative impacted the knowledge and awareness of best practices related to obesity care within the urgent care setting. Standardization of the process augmented the effectiveness of care provided.Patients with a BMI greater than 30 kg/m2 at increased risk were identified and educated about the correlation of BMI and waist circumference to co-morbidities. This helped the patients better understand the inherent risks associated with obesity through dialog that was initiated through the measurement of WC. It encouraged action and modification of behaviors to support improved health. The initiative was a success because both providers and patients became more informed and educated. Patients were apprehensive and not completely confident in their ability to make lifestyle changes for more than a few days to a week at a time, but as the project progressed and the patients saw the improvements, they became more willing to commit to the changes. Focusing on one small realistic goal enabled the patients to see that they could make a sustainable, impactful change. The patients contributed to successful effective care through their engagement in the tests of change. The project supported the literature that the patient engagement with provider relationship builds trust and motivation 12.
Despite the success, there were barriers encountered during each PDSA cycle with the staff, which included time constraints, added workload, memory lapses regarding new processes, and small staffing numbers. This project demonstrated that support and communication are essential for any change and improvement to occur. The team was supportive, encouraging, and adaptable with each test of change, which confirmed the literature according to Fiscella, Maukshc, Bodenheimer, and Salas (2017) that it is crucial to go from “I provide care” to “We provide care.” The role of the staff as change agents and their positive attitude and flexibility was invaluable to every aspect of this undertaking.
Limitations
Several limitations were noted during this project. The project was completed over a brief time in a small urgent care setting, and generalizability to primary care, other specialty care clinics, or a larger practice may not be possible. Patient engagement may have been because of obligation or extrinsic motivation versus genuine desire. Internal validity may have been limited by ambiguity in measurement techniques. Efforts were made to minimize limitations through reminders, one-on-one teaching, and assistance from the project lead.
Conclusion
Improving effective screening and management of obesity in an urgent care clinic, specifically those patients with a BMI greater than 30 kg/m2, was achieved through the course of this quality improvement project. Aspects of this initiative, including waist circumference with screening, the use of shared decision-making tools, and team huddles are sustainable with minimal cost or change to clinic processes. Some of the comprehensive care aspects, particularly concerning labs, should be maintained and followed by the patient’s primary care provider. The correlation of specific health behavior changes and motivational interviewing with health improvements of a defined group of patients could be the focus of future studies.
References
- 1.Agency for Healthcare Research and Quality [AHRQ]. (2018).Six Domains of Health Care Quality. Retrieved from Agency for Healthcare Research and Quality:https://www.ahrq.gov/talkingquality/measures/six-domains.html.
- 2. (2018) for Metabolic and Bariatric Surgery [ASMBS]. October).Obesity in America Fact Sheet.Retrieved 2018-11.
- 3.G A Bray, Frühbeck G, D H Ryan, Wilding J P H. (2016) Management of obesity. , Lancet (London, England) 387, 1947-1956.
- 4.Campos-Outcalt D. (2016) 8 USPSTF recommendations FPs need to know about. 65(5),338-341.Retrieved from https://frontier.idm.oclc.org/login?url=http://search.ebscohost.com/login.aspx?direct=true&db=cmedm&AN=27275937&site=ehost-live , The Journal of Family Practice
- 6.S G Chrysant, G S Chrysant. (2019) Thesingle useof body mass index for the obesity paradox is misleading and should be used in conjunction with other obesity indices. , Postgraduate Medicine 131(2), 96-102.
- 7.County Health Rankings. (2019).North Carolina.Retrieved from County Health Rankings and Roadmaps:https://www.countyhealthrankings.org/app/north-carolina/2019/rankings/cumberland/county/outcomes/overall/snapshot .
- 8.Edshteyn I, K A Uduhiri, T O Morgan, K L Rhodes, K M Sherin. (2016) Practice policy statement: Integrating effective weight management into practice. , American Journal of Preventive Medicine 51(4), 542-548.
- 10.W T Garvey, J I Mechanick, E M Brett, A J Garber, D L Hurley et al. (2016) American association of clinical endocrinologists and American college of endocrinology comprehensive clinical practice guidelines for medical care of patients with obesity. Endocrine Practice:. , Official Journal of the American College of Endocrinology and the American Association of Clinical Endocrinologists 22, 1-203.
- 11.Hargraves D, White C, Frederick R, Cinibulk M, Peters M et al. (2017) Implementing SBIRT (screening, brief intervention and referral to treatment) in primary care: Lessons learned from a multi-practice evaluation portfolio.Public Health Reviews. 38(31), 1-11.
- 12.Holdsworth E, Thorogood N, Sorhaindo A, Nanchahal K. (2017) A qualitative study of participant engagement with a weight loss intervention. Health Promotion Practice. 18(2), 245-252.
- 13.A M Jastreboff, C M Kotz, Kahan S, A S Kelley, S B Heymsfield. (2018) Obesity as a disease: The obesity society 2018 position statement.Obesity. 7-9.
- 14.M D Jensen, D H Ryan, C M Apovian, J D Ard, A G Comuzzie et al. (2014) AHA/ACC/TOS guideline for the management of overweight and obesity in adults.Journal of the American College of Cardiology. 63(25), 2985-3023.
- 15.R F Kushner, D H Ryan. (2014) Assessment and lifestyle management of patients with obesity: Clinical recommendations from systematic reviews. , Jama 312(9), 943-952.
- 17.G S Ogrinc, L A Headrick, S M Moore, A J Barton, M A Dolansky et al.(2012).Fundamentals of health care improvement: A guide to improving your patients'. care(2nd ed.). Oakbrook Terrace, Illinois: The Joint Commission and the Institute for Healthcare Improvement .
- 18. (2019) Office of Disease Prevention and Health Promotion. 31).Nutrition, Physical Activity, and Obesity. Retrieved from HealthyPeople.gov:https://www.healthypeople.gov/2020/leading-health-indicators/2020-lhi-topics/Nutrition-Physical-Activity-and-Obesity/data#NWS-9 .
- 19.Wood Robert. (2019) Johnson Foundation [RWJF]. (2019).The Healthcare Costs of Obesity. Retrieved.
- 20.J C Seidell, Halberstadt J. (2015) The global burden of obesity and the challenges of prevention. , Annals of Nutrition & Metabolism 66, 7-12.
