Abstract
The three most common elbow fractures classically reported in pediatric orthopedic literature are supracondylar (50–70%), lateral condylar (17–34%), and medial epicondylar fractures (10%).
The mechanism of injury varies, but the most commonly described mechanism involves a fall on an outstretched hand with varus, valgus or rotational force or a combination thereof. The vectors of force and the degree of chondro-osseous development dictate the type of injury incurred.
A review of the literature was conducted to see the most frequent injuries and complications.
Author Contributions
Academic Editor: Zhengping Liu, Department of Obstetrics, Southern Medical University Affiliated Maternal & Child Health Hospital of Foshan, China
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2018 Tepeneu N.F
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Introduction
The three most common elbow fractures classically reported in pediatric orthopedic literature are supracondylar (50–70%), lateral condylar (17–34%), and medial epicondylar fractures (10%).
The mechanism of injury varies, but the most commonly described mechanism involves a fall on an outstretched hand with varus, valgus or rotational force or a combination thereof. The vectors of force and the degree of chondro-osseous development dictate the type of injury incurred.
Material and Methods
A review of the literature on this complex subject was conducted using the key words “trauma”, “humerus”, “humeral condyle fracture”, “children”
Results
Lateral Humeral Condylar Fractures
are the second most common pediatric elbow fractures after supracondylar humeral fractures 1, 2. They comprise about 10–20% of all childhood elbow fractures having the annual incidence of 1.6/10,000 partly because of the increasing number of young athletes participating in highly competitive athletics 3.
Fractures involving the lateral condyle in the immature skeleton can either cross the physis or follow it for a short distance into the trochlear cartilage.
Associated Injuries
Fractures of the lateral condylar physis rarely are associated with injuries outside the elbow region and unlike supracondylar humeral fractures, fractures of the lateral condyle rarely are associated with neurovascular injuries. Within the elbow region, the associated injuries that uncommonly occur with this fracture include dislocation of the elbow (which may be a result of the injury to the lateral condylar physis rather than a separate injury), radial head fractures, and fractures of the olecranon, which are often greenstick fractures. Acute fractures involving only the articular capitellum are rare in skeletally immature patients but are serious injuries that need to be recognized and treated appropriately.
Mechanism of Injury
Two mechanisms have been suggested: “push-off” and “pull-off.” The pull-off or avulsion theory has more advocates than the push-off mechanism.
The mechanism of injury includes either avulsion forces from the lateral ligaments with the elbow extended, or impaction of the radius on the capitellum after a fall on an outstretched arm 4.
Clinical Presentation
Compared with the marked distortion of the elbow that occurs with displaced supracondylar fractures, little distortion of the elbow, other than that produced by the fracture hematoma, may be present with lateral condylar fractures. The key to the clinical evaluation of this fracture is the location of soft-tissue swelling and pain concentrated over the lateral aspect of the distal humerus.
Imaging Investigations
Diagnosis is made based on radiographs and it may be difficult in children 5. The radiographic appearance varies according to the fracture line’s anatomic location and the displacement stage.
The degree of displacement may be seen on the true lateral view. In determining whether the articular hinge is intact (i.e., stage I vs. stage II), the relationship of the proximal ulna to the distal humerus is evaluated for the presence of lateral translocation. Oblique views are especially helpful in patients in whom a stage I displacement is suspected but not evident on AP and lateral views. Figure 1 and Figure 2.
Figure 1.6 year old male patient with a undislocated left lateral condyle fracture which was succesfully treated with a cast (personal collection)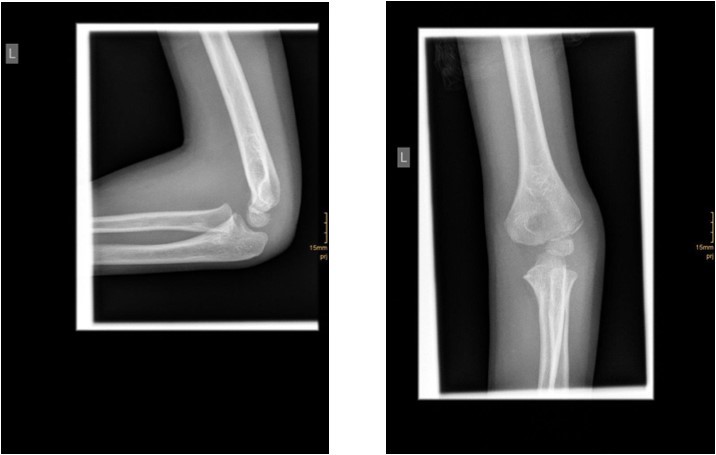
Figure 2.6 year old male patient with a dislocated right lateral condyle fracture which was treated by open reduction and osteosynthesis with a screw and a Kirschner wire (personal collection)
Arthrography or MRI evaluation has been suggested to identify unstable fractures in the acute
setting and to aid in preoperative planning for those with late displacement, delayed union, or malunion. MRI can be a very useful diagnostic aid to guiding treatment, especially with delayed unions.
Classification of Lateral Humeral Condylar Fractures
The Milch classification, based on whether or not the fracture extends through (type I) or around(type II) the capitellar ossific nucleus, is used infrequently because of its poor reliability and poor predictive value. Salter and Harris classified lateral condylar physeal injuries as a form of type IV injuries in their classification of physeal fractures. A true Salter– Harris type IV injury through the ossific nucleus of the lateral condyle is rare. Although lateral condylar fractures are similar to Salter–Harris type II and IV fractures, treatment guidelines follow those of a type IV injury: open reduction and internal fixation of displaced intra-articular fractures. Weiss et al. modified this classification based on fracture displacement and disruption of the cartilaginous hinge 6. They classified the lateral humeral condyle fractures in 3 types: type I, less than 2 mm of displacement; type II, 2 mm or more of displacement and congruity of the articular surface; type III, more than 2 mm of displacement and lack of articular congruity.
Treatment
Non-displaced and stable fractures may be treated by cast immobilization with close follow-up, but fractures displaced >2 to 3 mm may indicate surgical fixation 7, 8. Surgical treatment can be done either by closed reduction and percutaneous osteosynthesis or open reduction and osteosynthesis. Figure 3.
Figure 3.9 year old male patient with a elbow dislocation and a dislocated left lateral condyle fracture which was treated by open reduction and osteosynthesis with a screw (personal collection)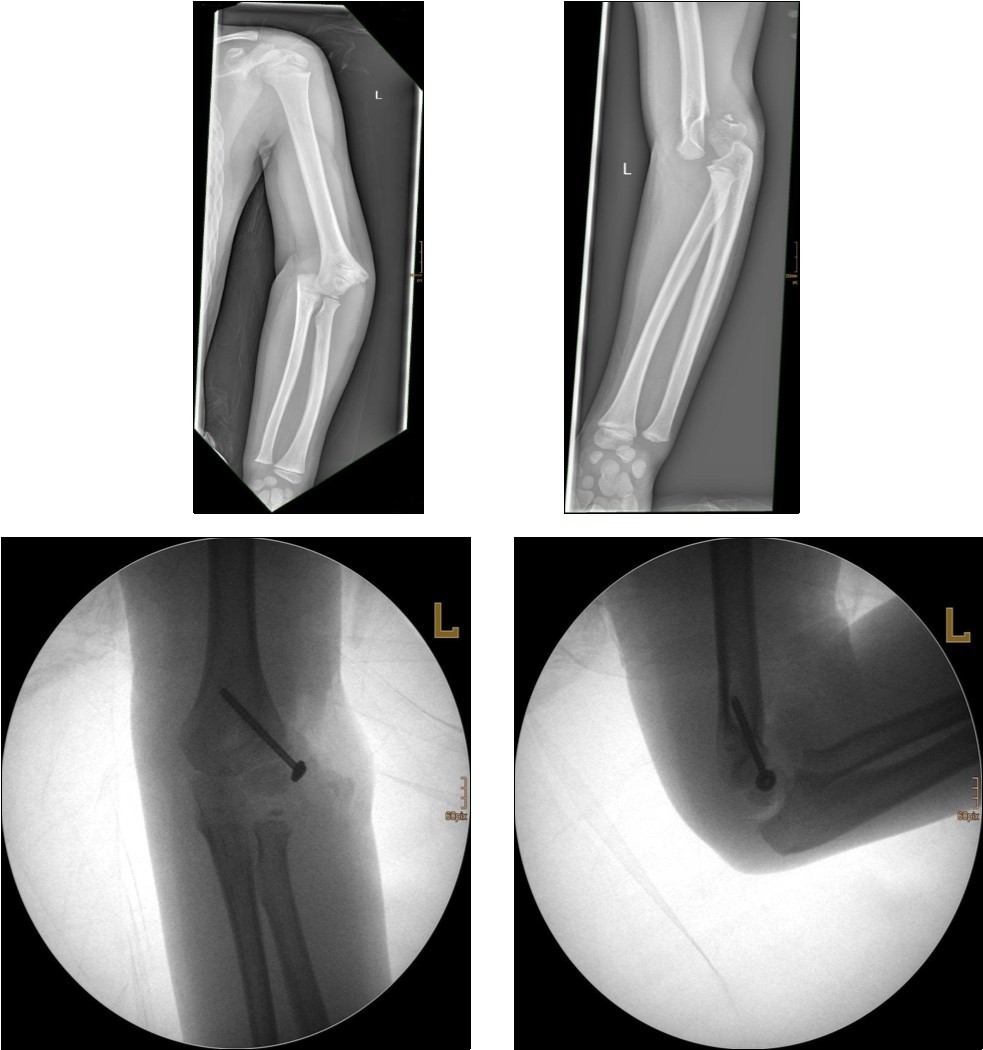
Surgical fixation is either by screw, smooth K-wires or both. The K-wires can be buried under the skin or not.
The idea behind burying K-wires is to reduce infection rates because it is felt that the wires have to stay in for a minimum of six weeks to prevent non-union. Some studies show no cases of non-union in either the buried or unburied wires group and infection rates that were comparable. In addition some of the cases with buried wires became effectively unburied. So that is why some authors concluded there is no justification in burying wires, which requires an additional general anaesthesia for removal 9.
Regarding pin orientation, most authors favor a divergent construct for greater stability.
For 2-pin constructs, maximizing pin divergence at the fracture site provided greater stability in torsional loading and valgus loading. The addition of a third pin in a divergent orientation increases stability compared with 2-pin constructs in valgus, internal, and external rotation loading. The pins must be placed in a bicortical manner, with maximum divergence and spread at the fracture site 10.
Complications
Many complications are known to be associated with childhood lateral condylar humeral fractures, with poor outcomes often related to delayed or inadequate initial treatment 5, 11.
Lateral humeral condylar fractures are the most common injuries that involve the growth line around the elbow region 12. There are also intra-articular fractures, which may affect bone healing and the joint surface 13. These fractures more commonly result in decreased range of movement more than any other elbow fractures 14. Up to 20% of patients with lateral condylar fractures show a cubitus varus deformity and >10% show a cubitus valgus deformity 15, 16, 17.
Medial Humeral Condyle Fractures
can be thought of as the mirror image of lateral condyle fractures. Although it was reported that isolated medial humeral condyle fractures account for 1–2 % of all distal humeral fractures, Landin found no cases of such a fracture in 589 pediatric elbow injuries 18. This type of fracture was reported to occur at a peak age of 8–12 years. However, case series in adolescents were also reported in literature 19, 20.
Associated Injuries
Fractures involving the medial condyle have two components. The intra-articular component involves, in some manner, the trochlear articular surface. The extra-articular portion includes the medial metaphysis and medial epicondyle.
As this fracture is rare, studies describing associated injuries are rare. Medial condylar physeal fractures have been reported in association with greenstick fractures of the olecranon and with true posterolateral elbow dislocations
Mechanism of Injury
Three possible mechanisms for medial condyle fracture are described; axial compression with concomitant valgus stress (fall on an outstretched arm), direct impaction of olecranon to medial condyle (direct fall on olecranon when the arm is flexed) and avulsion of the medial condyle due to violent contraction of the common flexor muscles of the forearm 21, 22.
A dislocation of the elbow ist most often associated with a fracture of the medial epicondyle.
Clinical Presentation
A fracture of the medial condylar physis is most often confused with a fracture of the medial epicondyle. In both types of intra- and extra-articular fractures, swelling is concentrated medially, and there may be valgus instability of the elbow joint. Ulnar nerve paresthesia may be present with both types of fractures.
Imaging Investigations
In older children with a large metaphyseal fragment, involvement of the entire condyle is usually obvious on radiographs. In younger children, in whom only the epicondyle is ossified, fracture of the medial condylar physis may be erroneously diagnosed as an isolated fracture of the medial epicondyle. In differentiating these two fractures, it is helpful to remember that medial epicondylar fractures are often associated with elbow dislocations, usually posterolateral, and that elbow dislocations are rare before ossification of the medial condylar epiphysis begins. With medial condylar physeal fractures, the elbow tends to subluxate posteromedially because of the loss of trochlear stability.
As the trochlea ossifies by the age of 9, the difficulty of making diagnosis by plain radiographs in younger children is not a major problem in adolescents. Nevertheless, some other problems may complicate the injury. These intraarticular fractures are prone to nonunion 23, 24. In addition, these fractures are Salter–Harris type IV physeal injuries, and even with adequate reduction, partial physeal arrest can develop and lead to consequent problems.
Classification of Lateral Humeral Condylar Fractures
Classification, as with fractures of the lateral condylar physis, is based on the fracture line’s location and the degree of the fracture’s displacement. Milch classified fractures of the medial condylar physis in adults into two types. In type I fractures, the fracture line traverses the apex of the trochlea. In type II fractures, it traverses more laterally through the capitulotrochlear groove.
Treatment
Undisplaced fractures are simply immobilized in a cast or posterior splint. As with fractures of the lateral condylar physis union may be slow. In fractures treated promptly, results have been satisfactory. Because there is usually more displacement in older children, the results in this age group are not as satisfactory as those in younger children, who tend to have relatively nondisplaced fractures. For displaced fractures, open reduction with internal fixation is the most often used treatment method.
The fracture fragment can be approached by a posteromedial incision that allows good exposure of both the fracture site and the ulnar nerve. Fixation is easily achieved with smooth K-wires or with screws in older adolescents. Two wires are necessary because of the sagittal rotation forces exerted on the fracture fragment by the common flexor muscles. Figure 4 and Figure 5.
Figure 4.14 year old female patient with a elbow dislocation and a dislocated left epicondyle fracture which was treated by open reduction and osteosynthesis with two divergent Kirschner wires (personal collection)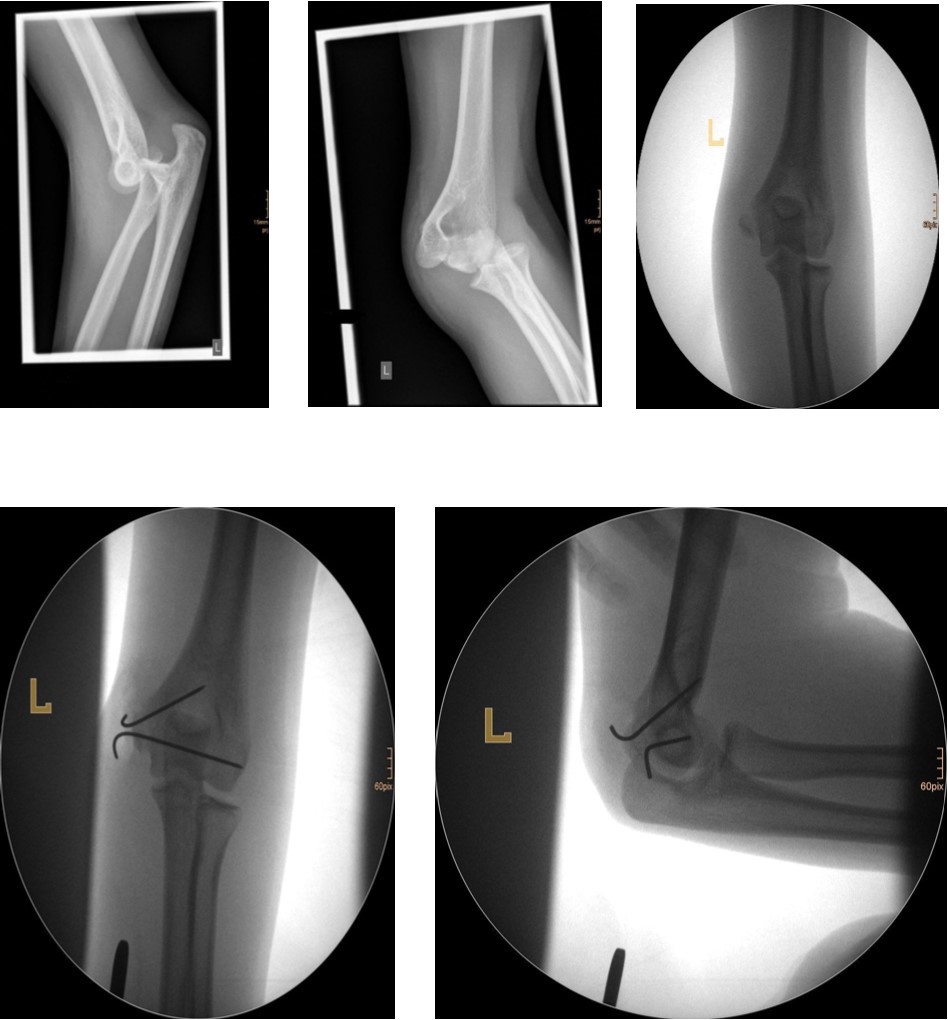
Figure 5.9 year old female patient with a elbow dislocation and a dislocated right medial condyle fracture which was treated by open reduction and osteosynthesis with a screw (personal collection)
Complications
Although nondisplaced or minimally displaced fractures can be treated nonoperatively in a cast, careful monitoring is required to identify further displacement and delayed union.
When displaced, open treatment with identification of the ulnar nerve and direct visualization of the joint surface is needed. The rate of complications is relatively high and may include osteonecrosis, elbow stiffness, malunion, or delayed union.
Leet et al.20 reported complications after 33% of 21 medial condylar fractures, including osteonecrosis of the trochlea, nonunion, and loss of reduction. Untreated displaced fractures usually result in nonunion with cubitus varus deformity. Both cubitus varus and valgus deformities have been reported in patients whose fractures united uneventfully. The valgus deformity appears to be caused by secondary stimulation or overgrowth of the medial condylar fragment. Some simple stimulation of the medial epicondyle’s prominence may also produce the false appearance of a cubitus valgus deformity. Cubitus varus appears to result from decreased growth of the trochlea, possibly caused by a vascular insult. Principles for treating nonunion of lateral condylar fractures are generally applicable to nonunions of the medial condyle.
Discussion
All the physes of the distal humerus are vulnerable to injury, each with a distinct fracture pattern. Next to those of the distal radius, injuries to the distal humeral physes are the most common the first 2 to 3 years of life 25, 26, 27. Fractures involving the lateral condylar physis occur early, with the average age around 6 years 18, 26. Fractures concerning the medial condylar physis are rare and occur most often in children 8 to 12 years of age 24.
The diagnosis of lateral condylar physeal injuries may be less obvious both clinically and on radiographs than that of supracondylar fractures, especially if the fracture is minimally displaced. Oblique views of the distal humerus are very helpful in making accurate diagnosis and defining the extent of fracture displacement for treatment decisions.
Fractures of the medial condyle of the humerus are rare elbow injuries. The mechanism of these fractures remains controversial. Fowles and Kassab 22 reported a patient with a concomitant valgus greenstick fracture of the olecranon associated with a fracture of the medial condyle. As this fracture is rare, studies describing associated injuries are rare. Medial condylar physeal fractures have been reported in association with greenstick fractures of the olecranon and with true posterolateral elbow dislocations 19, 24, 28 Some investigators 19, 28, 29 found that child abuse was more common in their younger patients with these fractures than with other elbow fractures. Regardless, the extremity should be evaluated for concomitant injuries of forearm, wrist, or hand, and the radiographs should be inspected for additional fractures about the elbow.
Humeral condyle fractures can be associated with elbow joint dislocations, although dislocations of the elbow joint in children are not common. Of all elbow injuries in skeletally immature patients, Henrikson 29 found that only about 3% of all were dislocations. The peak incidence of pediatric elbow dislocations typically occurs in the second decade of life, usually between 13 and 14 years of age when the physes begin to close 30
The largest proportion of elbow dislocations (44.5%) occur in conjunction with sports activities; football/ rugby, wrestling, and basketball being the most common sports for males and gymnastics and skating being the most common sports for females 31. Almost 60% of medial epicondyle fractures are associated with elbow dislocations in this age group. As with all joint dislocations, the principles of treatment include promptly obtaining a concentric reduction of the elbow joint while identifying and treating all associated injuries. The ultimate goal is allowing protected motion and rehabilitation with the goal of restoring full elbow motion without recurrent instability.
Because of the location of critical stabilizing factors and surrounding neurovascular structures, elbow dislocations should be considered based on the direction of dislocation and the associated fractures which may be present. As the mechanism of injury, the associated injuries, and imaging differ based on the nature of the injury, these factors should be considered for each dislocation pattern.
Medial epicondyle fractures commonly occur in association with elbow dislocation and the treating physician must have a high index of suspicion for this injury. Careful physical examination and thoughtful use of imaging studies will allow the treating physician to detect medial epicondyle fractures in all patients. The most common cause of a missed medial epicondyle fracture is that the treating physician did not think to specifically look for this injury 32.
Diagnosis of these traumatic entities is done by clinical examination and paraclinical investigations.
Trauma is a common indication for elbow imaging in children. Fractures in the developing pediatric elbow occur frequently and can be challenging to diagnose radiographically.
Although some fractures are quite apparent, knowledge of the normal developmental appearances and the radiographic clues to injury are necessary to optimize detection of more occult fractures. Sometimes a CT or better yet a CT with 3D reconstruction can help in the diagnosis and treatment of these fractures. A intraoperative arthrography is sometimes also useful.
The most important problem in the treatment of humeral condyle fractures is the pseudarthrosis that can happen in the framework of a conservative treatment of displaced fractures, rarely after operative treatment with K-wires or screws. A rather academic problem is the obligatory growth disturbance of a partial stimulation of the lateral part of the growth plate. This leads to radial overgrowth and thus to a more or less distinct varus deformity.
The extent of varus deformity is dependent on the time till consolidation, which is longest in conservatively treated fractures and shortest in those treated with compression screw osteosynthesis. An additional academic problem is the so-called fishtail deformity that becomes radiological visible at the end of growth. This deformity has no clinical significance. Pseudarthrosis, varus and fishtail deformity are a result of increasing instability of primarily or secondarily displaced fractures. Cubitus valgus and tardy ulnar nerve palsy are considered the main complications of nonunion lateral humeral condyle. The treatment of nonunion of the lateral humeral condyle with <1 cm of displacement is generally recommended, if care is taken to avoid damage to the vasculature of the lateral condylar fragment 33.
Conclusion
Fractures of the humeral condyles in children pose special problems which need to be addressed by a person specialized in pediatric traumatology. Conservative and operative treatment is possible, specific for each type of fracture.
Specific complications can occur after fractures of the humeral condyles which in turn can pose problems which need special expertise in order to be solved.
References
- 1.Tejwani N, Phillips D, Goldstein R Y. (2011) Management of lateral humeral condylar fracture in children. , J Am Acad Orthop Surg 19, 350-358.
- 2.Emery K H, Zingula S N, Anton C G, Salisbury S R, Tamai J. (2016) Pediatric elbow fractures: a new angle on an old topic. , Pediatr Radiol 46, 61-6.
- 3.Chen F S, Diaz V A, Loebenberg M, Rosen J E. (2005) Shoulder and elbow injuries in the skeletally immature athlete. JAmAcadOrthop Surg. 13, 172-185.
- 4.Cates R A, Mehlman C T. (2012) Growth arrest of the capitellar physis after displaced lateral condyle fractures in children. , J Pediatr Orthop 32, 57-62.
- 5.Marcheix P, Vacquerie V, Longis B, Peyrou P, Fourcade L et al. (2012) Distal humerus lateral condyle fracture in children: when is the conservative treatment a valid option? Orthop Traumatol Surg Res. 97, 304-307.
- 6.Weiss J M, Graves S, Yang S. (2009) A new classification system predictive of complications in surgically treated pediatric humeral lateral condyle fractures. , J Pediatr Orthop 29, 602-605.
- 7.Sullivan A J. (2006) Fractures of the lateral condyle of the humerus. , J Am Acad Orthop Surg 14, 58-62.
- 8.Bhandari M, Tornetta P, Swiontkowksi M F. (2003) Displaced lateral condyle fractures of the distal humerus. , J Orthop Trauma 17, 306-308.
- 9.McGonagle L, Elamin S, D M Wright.(Oct2012) Buried or unburied K-wires for lateral condyle elbow fractures. , Ann R Coll Surg Engl 94(7), 513-516.
- 10.Bloom T, L Y Chen, Sabharwal S.(Mar2011) Biomechanical analysis of lateral humeral condyle fracture pinning. , J Pediatr Orthop 31(2), 130-7.
- 11.Vallila N, Sommarhem A, Paavola M, Nietosvaara Y. (2015) Pediatric distal humeral fractures and complications of treatment in Finland: a review of compensation claims from1990through2010. , J Bone Joint Surg Am 97, 494-499.
- 12.Mizuta T, Benson W, Foster B, Morris L. (1987) Statistical analysis of the incidence of physeal injuries. , J Pediatr Orthop 7, 518-523.
- 13.Bernthal N M, Hoshino C M, Dichter D, Wong M, Silva M. (2011) Recovery of elbowmotion following pediatric lateral condylar fractures of the humerus. , J Bone Joint Surg Am 93, 871-877.
- 14.Launay F, Leet A I, Jacopin S, Jouve J, Bollini G et al. (2004) Lateral humeral condyle fractures in children: a comparison of two approaches to treatment. , J Pediatr Orthop 24, 385-391.
- 15.So Y, Fang D, Orth M C, Leong J, Bong S. (1985) Varus deformity following lateral humeral condylar fractures in children. , J Pediatr Orthop 5, 569-572.
- 16.Skak S V, Olsen S D, Smaabrekke A. (2001) Deformity after fracture of the lateral humeral condyle in children. , J Pediatr Orthop 10, 142-152.
- 17.Jakob R, Fowles J V, Rang M, Kassab M T. (1975) Observations concerning fractures of the lateral humeral condyle in children. , J Bone Joint Surg Br 57, 430-436.
- 18.Landin L A, Danielsson L G. (1986) Elbow fractures in children. An epidemiological analysis of 589 cases. , Acta Orthop Scand 57(4), 309-312.
- 19.Bensahel H, Csukonyi Z, Badelon O, Badaoui S. (1986) Fractures of the medial condyle of the humerus in children. , J Pediatr Orthop 6(4), 430-433.
- 20.Leet A I, Young C, Hoffer M M. (2002) Medial condyle fractures of the humerus in children. , J Pediatr Orthop 22(1), 2-7.
- 21.Chacha P B. (1970) Fracture of the medial condyle of the humerus with rotational displacement. Report of two cases. , J Bone Joint Surg Am 52(7), 1453-1458.
- 22.Fowles J V, Kassab M T. (1980) Displaced fractures of the medial humeral condyle in children. , J Bone Joint Surg Am 62(7), 1159-1163.
- 23.Ryu K, Nagaoka M, Ryu J. (2007) Osteosynthesis for nonunion of the medial humeral condyle in an adolescent: a case report. , J Shoulder Elbow Surg 16(3), 8-12.
- 24.Song K S, Ramnani K, Cho C H, Son E S. (2011) Late diagnosis of medial condyle fracture of the humerus with rotational displacement in a child. , J Orthop Traumatol 12(4), 219-222.
- 25.DeLee J C, Wilkins K E, Rogers L F. (1980) Fracture separation of the distal humeral epiphysis. , J Bone Joint Surg Am 67, 46-51.
- 27.Houshian S, Mehdi B, Larsen M S. (2001) The epidemiology of elbow fracture in children: Analysis of 355 fractures, with special reference to supracondylar humerus fractures.J Orthop Sci. 6, 312-315.
- 28.H De Boeck, Casteleyn P P, Opdecam P. (1987) Fracture of the medial humeral condyle. Report of a case in an infant. , J Bone Joint Surg Am 69(9), 1442-1444.
- 29.Henrikson B. (1966) Supracondylar fracture of the humerus in children. A late review of end results with special reference to the cause of deformity, disability and complications. Acta Chir Scand Suppl.369; 1. 72.
- 30.Potter C M. (1954) Fracture-dislocation of the trochlea. , J Bone Joint Surg Br.36-B(2): 250-253.
- 31.Stoneback J W, Owens B D, Sykes J. (2012) Incidence of elbow dislocations in the United States population. , J Bone Joint Surg Am 94(3), 240-245.
Cited by (2)
- 1.Bilo Rob A. C., de Vries Selena, Nagtegaal Michelle, Robben Simon G. F., van Rijn Rick R., 2023, , , (), 325, 10.1007/978-3-031-12041-1_12
- 2.Dorokhin A. I., Bagomedov H. G., 2019, MANAGEMENT OF LATERAL HUMERAL CONDYLAR FRACTURE IN CHILDREN, Russian Journal of Pediatric Surgery, Anesthesia and Intensive Care, 9(1), 62, 10.30946/2219-4061-2019-9-1-62-69
