Abstract
Trichomegaly is a known adverse effect with the epidermal growth factor receptor inhibitor (EGFRI) and prostaglandin analogue drug classes. We present a chronic Latanoprost user who developed symptomatic trichomegaly subsequent to initiating an EGFRI medication and believe this case offers evidence that the two classes of medications may cause a similar eyelash manifestation through different mechanisms.
Author Contributions
Academic Editor: Vijaya Bhatt, University of Nebraska Medical Center
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2015 Burris CK, et al
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Introduction
It has been predicted that the world cancer incidence will nearly double over the next 20 years.1 Though chemotherapies are constantly evolving, the use of EGFRI medications may also increase. Epidermal growth factor is thought to play a role in the conversion of hair follicles from the active anagen phase to the quiescent catagen phase, regulating eyelash length.2 Though most chemotherapeutic agents would be expected to cause hair loss, EGFRI drugs such as Erlotinib have been shown to cause a paradoxical trichomegaly (increased length, thickness, and pigmentation) of the eyelashes due to a dysregulation of this process.3, 4, 5 Interestingly, prostaglandin F2α receptors have been shown to be expressed predominately during the anagen phase in the inner root sheath of the bulb and stem of eyelashes.6
Case Presentation
An 81 year-old African American male presented complaining of ocular irritation, foreign body sensation, and obstruction of his visual field by his eyelashes for over 1 year. Past ocular history was significant for primary open angle glaucoma, cataracts, posterior vitreous detachments, and elongated eyelashes requiring regular trimming approximately every 2 months during the past year. Family history was positive for glaucoma in his father and two siblings. Medical history included metastatic bronchogenic adenocarcinoma, hyperlipidemia, lipoma, benign prostatic hypertrophy, and seasonal allergies. Ophthalmic medications were Latanoprost, Timolol, and artificial tears used in both eyes. Systemic medications consisted of Guaifenesin, Albuterol, Sodium Chloride nasal spray, Loratadine, Erlotinib, Simvastatin, and Simethicone.
On exam he appeared well nourished and his spectacle corrected visual acuity was 6/9-2 OD and 6/6-2 OS. External exam showed trichomegaly and trichiasis with cilia measuring 18 and 17mm OD and OS (see Figure 1and Figure 2). Both corneas had inferior superficial punctate keratopathy but there were no abrasions or ulcers. Besides a choroidal nevus, the remainder of his exam was similar to his previous with 1-2+ nuclear sclerotic change in his lenses, cup to disc ratios of 0.85 and 0.7, and posterior vitreous detachments. His eyelashes were trimmed to 3mm and he was given refills of his artificial tears.
Figure 1.Note loss of eyebrow hair with paradoxical trichomegaly and trichiasis of the eyelashes.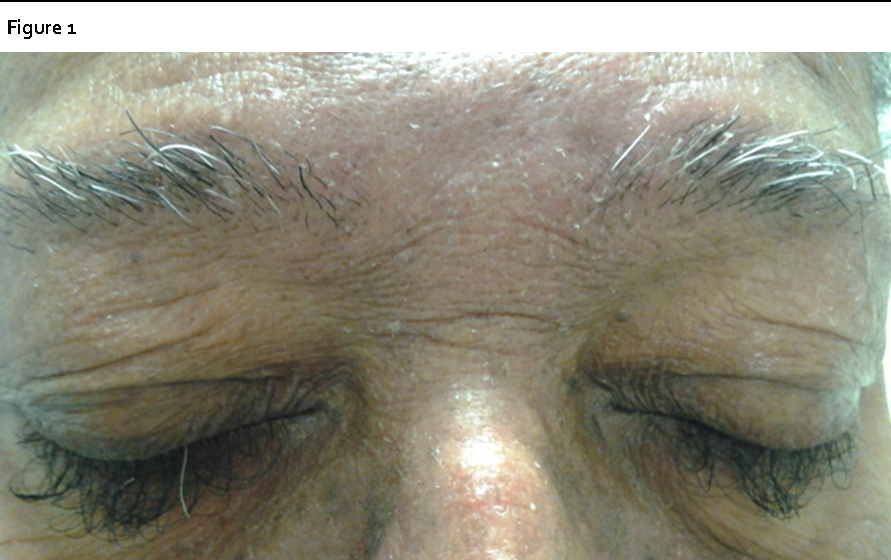
Figure 2.Note loss of eyebrow hair with paradoxical trichomegaly and trichiasis of the eyelashes.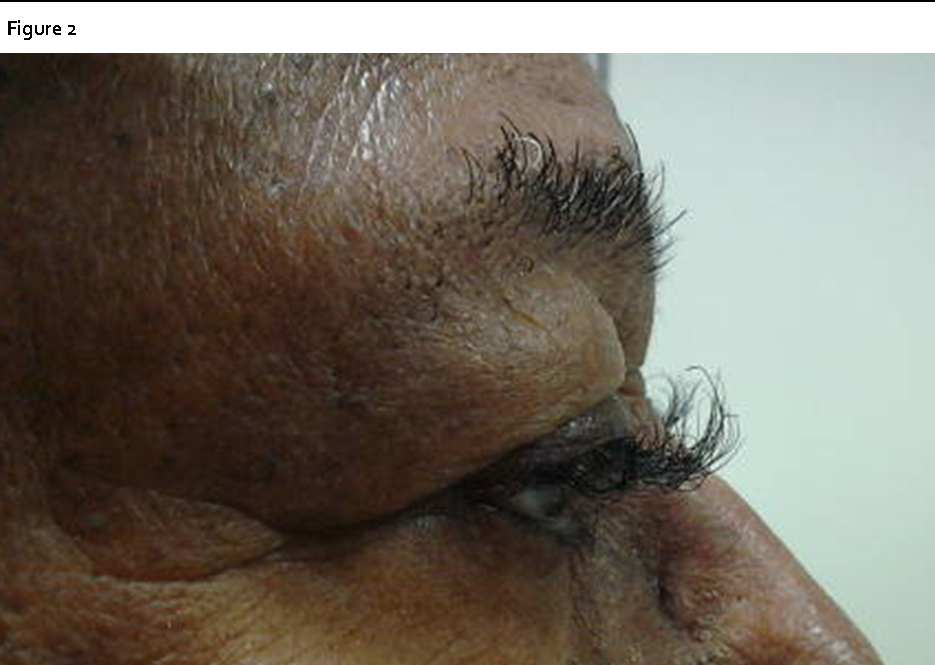
Discussions
Trichomegaly of the eyelashes has a long differential, but the main causes are congenital, acquired, and medication associated. Congenital associations include: Familial trichomegaly, Oliver-McFarlane syndrome, Aghaei-Dastgheib syndrome, Hermansky-Pudlak syndrome, Goldstein-Hutt syndrome, Congenital heart disease, Cone-rod dystrophy, and Phylloid hypomelanosis.7, 8, 9, 10, 11, 12, 13 Acquired causes often have a nutritional or inflammatory component and have been documented in: Anorexia, Alopecia areata, Atopic dermatitis, Vernal keratoconjunctivitis, Dermatomyositis, HIV, Systemic lupus erythematosus, and Uveitis.14, 15, 16, 17, 18, 19, 20, 21 Medications associated with this pattern of eyelash growth include: Cyclosporine, EGFRI, Interferon alpha, Prostaglandin analogues, Tacrolimus, and Topiramate.22, 23, 24, 25, 26, 27
This patient was using two medications shown to cause trichomegaly; Erlotinib (an EGFRI), and Latanoprost (a prostaglandin analogue). According to one large series, 94% of patients developing trichomegaly from prostaglandin analogue eye drops within the first year of use develop symptoms in the first 6 months of treatment (44.6% in 6 months versus 46.2% in 1 year).28 Although he may have had some eyelash changes during his long course of prostaglandin use, it is unlikely that this medication would cause him to become symptomatic in his 10th year of use, and he had regular follow up (approximately every 3 months during this period). The timing of his symptoms, requiring eyelash trimmings coincided with the year he initiated the EGFRI, Erlotinib. This case suggests that these drug classes could cause trichomegaly through separate mechanisms. It is not known whether their effects could be additive or synergistic. Plasma concentrations of Erlotinib were not measured, but therapeutic response and survival have been shown to correlate with side effects of the medication such as skin rash.29 He did have typical changes seen with chemotherapeutic agents such as skin rash, and loss of eyebrow hair along with incongruous eyelash growth. Thankfully at this time his tumor is still radio graphically controlled.
Conclusions
Trichomegaly is a known side effect of the EGFRI class of medications. Clinicians should be familiar with this drug class in order to prevent corneal abrasions and secondary infections. Patients initiating these medications should be followed at regular intervals, instead of depending on visual or corneal symptoms to guide management
Though the mechanism of eyelash growth is unclear, it is potentially dissimilar to that of prostaglandin analogues.
References
- 1.Bray F, Jemal A, Grey N, Ferlay J, Forman D.Global cancer transitions according to the Human Development Index (2008-2030): a population-based study. Lancet Oncol.2012Aug;. 13(8), 790-801.
- 2.Thibaut S, E De Becker, Caisey L, Baras D, Karatas S et al.Human eyelash characterization. , Br J Dermatol.2010Feb1; 162(2), 304-10.
- 3.Braiteh F, Kurzrock R, Johnson F M.Trichomegaly of the eyelashes after lung cancer treatment with the epidermal growth factor receptor inhibitor erlotinib. , J Clin Oncol.2008Jul10; 26(20), 3460-2.
- 4.Jazayeri F, Malhotra R.A case of acquired trichomegaly following treatment with erlotinib. BMJ Case Rep. 2009;2009. doi:pii: bcr01.2009.1473. 10.1136/bcr.01.2009.1473. Epub2009May20 .
- 5.Alexandrescu D T, Kauffman C L, Dasanu C A.The cutaneous epidermal growth factor network: Can it be translated clinically to stimulate hair growth?. Dermatol Online J.2009Mar15; 15(3), 1.
- 6.Nesher R, Mimouni M, Elnaddaf H, Nemet A, Kidron D.Characterization of prostaglandin F2α receptors in human eyelids. , Eur J Ophthalmol.2015Mar-Apr; 25(2), 81-4.
- 8.Sampson J R, Tolmie J L, Cant J S.Oliver McFarlane syndrome: a 25-year follow-up. , Am J Med Genet.1989Oct; 34(2), 199-201.
- 9.Aghaei S, Dastgheib L.Acquired eyelash trichomegaly and generalized hypertrichosis associated with breast anomaly. Dermatol Online J.2006Feb28; 12(2) 19.
- 10.Toro J, Turner M, Gahl W A.Dermatologic manifestations of Hermansky-Pudlak syndrome in patients with and without a 16-base pair duplication in the HPS1 gene. Arch Dermatol.1999Jul;. 135(7), 774-80.
- 11.Goldstein J H, Hutt A E.Trichomegaly,cataract and hereditary spherocytosis in two siblings. , Am J Ophthalmol.1972Mar; 73(3), 333-5.
- 12.Mansour A M, Bitar F F, Traboulsi E I, Kassak K M, Obeid M Y et al.Ocular pathology in congenital heart disease. , Eye (Lond).2005Jan; 19(1), 29-34.
- 13.Jalili I K.Cone-rod congenital amaurosis associated with congenital hypertrichosis: an autosomal recessive condition. , J Med Genet.1989Aug; 26(8), 504-10.
- 14.Vélez A, Kindelán J M, García-Herola A, García-Lázaro M, Sánchez-Guijo P.Acquired trichomegaly and hypertrichosis in metastatic adenocarcinoma. Clin Exp Dermatol.1995May;. 20(3), 237-9.
- 15.Droubi D, Nazareth M R, Rothman I L.Long-term follow-up of previously reported case of trichomegaly associated with alopecia areata in a 3-year-old girl. Pediatr Dermatol.2012Mar-Apr;. 29(2), 234-5.
- 16.Levy Y, Segal N, Ben-Amitai D, Danon Y L.Eyelash length in children and adolescents with allergic diseases. Pediatr Dermatol.2004Sep-Oct;. 21(5), 534-7.
- 17.Pucci N, Novembre E, Lombardi E, Massai C, Bernardini R et al.Long eyelashes in a case series of 93 children with vernal keratoconjunctivitis. , Pediatrics.2005Jan; 115(1), 86-91.
- 18.Sharma R C, Mahajan V K, Sharma N L, Sharma A. (2002) Trichomegaly of the eyelashes in dermatomyositis. , Dermatology 205(3), 305.
- 19.Kaplan M H, Sadick N S, Talmor M.Acquired trichomegaly of the eyelashes: a cutaneous marker of acquired immunodeficiency syndrome. , J Am Acad Dermatol.1991Nov; 25(5 Pt 1, 801-4.
- 20.Santiago M, Travassos A C, Rocha M C, Souza S. (2000) Hypertrichosis in systemic lupus erythematosus (SLE). , Clin Rheumatol 19(3), 245-6.
- 21.Bayer A, Bagkesen H, Sobaci G.Acquired trichomegaly in uveitis. , Can J Ophthalmol.2007Feb; 42(1), 101-6.
- 22.Weaver D T, Bartley G B.Cyclosporine-induced trichomegaly. , Am J Ophthalmol.1990Feb15; 109(2), 239.
- 23.Jazayeri F, Malhotra R. (2009) A case of acquired trichomegaly following treatment with erlotinib. BMJ Case Rep.2009.doi:pii:bcr01.2009.1473.10.1136/bcr.01.2009.1473.
- 24.Kadayifcilar S, Boyacioglu S, Kart H, Gursoy M, Aydin P.Ocular complications with high-dose interferon alpha in chronic active hepatitis. , Eye (Lond).1999Apr; 13 ( Pt 2, 241-6.
- 25.Woo T L, Francis I C.Intermittent blurred vision and trichomegaly due to latanoprost. Clin Experiment Ophthalmol.2001Aug;. 29(4), 272-3.
- 26.Ward K M, Barnett C, Fox L P, Grossman M E.Eyelash trichomegaly associated with systemic tacrolimus. , Arch Dermatol.2006Feb; 142(2), 248.
- 27.Santmyire-Rosenberger B R, Albert M.Acquired trichomegaly with topiramate. , J Am Acad Dermatol.2005Aug; 53(2), 362-3.