Abstract
Introduction:
Elevated serum troponin levels are a reliable indicator of right ventricular wall stress in patients with acute pulmonary artery embolism (PE). Raised troponin levels have been shown to predict adverse clinical outcome in these individuals. In this context it was our aim to determine the additional role of the heart-type fatty acid-binding protein (H-FABP) in patients with acute PE.
Methods:
87 consecutive patients with confirmed PE were included in the present study. On arrival a qualitative H-FABP-test (positive cut-off 7ng/ml) and a detailed echocardiographic study were performed in all patients. These findings were related to both in hospital and 30 days mortality.
Results:
Of the included 87 patients, 17 had positive H-FABP-tests. Right ventricular function was severely deteriorated in 10 patients (59%) in the H-FABP-positive group but only in 2 patients (3%) of the H-FABP-negative group (p<0.005). 15/17 patients (88%) of the H-FABP-positive group needed inotropic support, of these, 14 (82%) died in hospital. Only one patient with a H-FABP-negative test (n= 70) needed vasoactive drugs, and none of these patients died (p<0.005).
Conclusion:
H-FABP showed a better correlation with in-hospital mortality and RV-function than troponin I. Our data show that H-FABP significantly correlates with in hospital and 30-day mortality in patients with PE. Furthermore, it is associated with impaired right ventricular function and showed better correlation with mortality in patients with PE as compared to Troponin I. Thus, it may be viewed as a novel and promising tool to optimise the management strategy in these patients.
Author Contributions
Academic Editor: Dongmei Wu, Department of Research Mount Sinai Medical Center
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2013 Utz Richter, et al.
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Introduction
Despite recent advances in diagnosis and treatment, assessment of risk and appropriate management of patients with acute pulmonary embolism (PE) remain difficult due to the variability of clinical presentation and degree of hemodynamic instability 1,2. Recent studies focussed on a better definition of patients at higher risk in whom the use of a more aggressive therapy (e.g. thrombolysis) might confer clinical benefit.
Echocardiography plays an important role in the diagnosis and risk stratification of PE, showing that right ventricular dysfunction strongly correlates with in-hospital mortality 3,4. But echocardiography may not be available anytime; therefore the attention was drawn to the more easily available serum measurement of biomarkers. Recently, it has been proposed that the degree of right ventricular wall stress with consecutive release of cellular proteins from injured cadiomyocytes correlates with the clinical impairment and with mortality in patients with PE. Of the proposed biomarkers, troponin I and troponin T have been shown to correlate with right ventricular dysfunction and moreover with in hospital mortality. Moreover, elevated troponin levels predicted a complicated in-hospital course of patients with PE, as compared to other biomarkers such as CKMB, D-Dimers or NT-Pro-BNP 5,6.
Lately, several studies reported that heart-type fatty acid binding protein (H-FABP), a novel low molecular weight cytosolic protein, enables earlier and precise diagnosis and risk assessment in patients with acute coronary syndromes as compared to other biomarkers 7,8. Recent data could even demonstrate an association of elevated levels of H-FABP with increased risk of death and major cardiac events in this setting, thus having important prognostic power 9.
There are only few data regarding the diagnostic and prognostic value of H-FABP in patients presenting with PE 10,11. It was therefore our aim to assess the prognostic value of H-FABP in acute pulmonary embolism and to correlate it to other established biomarkers such as troponin I and to echocardiographic data.
Methods
Study Population and Design
A total of 87 consecutive patients (51 women, 36 men, mean age 65±17 years) with acute pulmonary embolism were prospectively included in this trial over a period of 20 months. No patient had connective tissue or pre-existent severe lung disease.
Typical clinical presentation, elevated D-Dimers and the presence of deep venous thrombosis suggested the presence of PE, which was confirmed by ventilation-perfusion lung scan or spiral CT-scan. All patients with potential PE were screened, but only when PE was confirmed they were included in the study. In patients in whom transport was not possible due to hemodynamic instability (n=4), diagnosis was based on echocardiographic findings of acute pulmonary hypertension and right ventricular pressure overload together with the presence of deep venous thrombosis. In case of death, post-mortem autopsy was performed; in all autopsies with suspected PE the diagnosis was confirmed. PE was classified according to the current PE guidelines by the European Society of Cardiology in following severity levels: high risk and non-high risk PE, whereas non-high risk can further be classified in low risk and intermediate risk PE 12.
Echocardiographic Criteria
On admission, experienced echocardiographers blinded to the result of the H-FABP-test performed transthoracic echocardiography using the Hewlett Packard SONOS 5500 system, with the patient in left lateral decubitus position when patient was awake.
To detect right ventricular overload, the following parameters were determined as described previously in detail 13: Briefly, dilatation of the right ventricle was defined when end-diastolic diameter was greater than 30mm from the parasternal view; the RV/LV-ratio was defined abnormal when greater than 0,6 10. Another recent trial reported an RV/LV-ratio >0,78 as a cut-off 14. In the recently published guidelines of the European Society of Cardiology a cut-off value >1 was suggested 12. Parameters for detecting right ventricular overload and dysfunction were a right ventricular end systolic pressure >35mmHg, the grade of tricuspid regurgitation, the presence of a paradoxical septal movement, a tricuspid annular plane systolic excursion (TAPSE) <20mm and the presence of typical wall motion with normokinesia of the apical segment, akinesia of the free mid-wall and abnormal wall motion of the base segment, also known as the McConnell sign 15. After measuring all these parameters, visual estimate of RV-function and the modified Simpson’s method for estimation of RV ejection fraction was performed 16. An impaired right ventricle was defined when RV ejection fraction was <45% according to a recent report 17.
Biochemical Analyses
On admission, blood samples were obtained prior to initiation of treatment in all patients with suspected pulmonary embolism. Plasma concentrations of Troponin I, CK, CK-MB and D-Dimers were measured quantitatively. All patients gave their consent for measurement of H-FABP, which was done only once on admission with routine blood samples. For Troponin I, a quantitative chemiluminescence assay (Ortho-Clinical Diagnosis) was performed. Reported values in normal healthy adults were <0,08 ng/ml. The manufacturer proposed a cut-off point of 0,4 ng/ml as a diagnostic limit for myocardial infarction. We considered an elevated Troponin I when the cut-off exceeded the cut-off of 0,07 ng/ml like described previously 5. For Creatine kinase (CK), a kinetic UV-Test, and for CK-MB isoenzyme, an enzymatic immunological inhibition-test (both on Olympus-Analyzer) were performed. Normal values for CK are < 2,85µkat/l, for CK-MB < 0,4 µkat/l. For D-Dimers a quantitative automated latex agglutination test for fibrin D-Dimer was performed on Hitachy analyser (trinity Biotech plc, Ireland). The normal cut-off value is <0,25 µg/ml. Plasma concentrations of H-FABP were measured qualitatively using a sandwich ELISA purchased from Rennesens GmbH, Berlin. The clinical cut-off value for H-FABP was 7ng/ml, as previously established by several independent researchers and as proposed by the manufacturer 18. The H-FABP levels were not used for therapeutic decisions. Glomerular filtration rate (GFR) was estimated by the Modification of Diet in Renal Disease (MDRD) formula 19. Neither the treating clinician nor the echocardiographers were aware of the patients’ H-FABP levels on admission. Our study did not influence diagnostic or therapeutic decisions.
Statistical Analysis
The data were expressed as mean followed by standard deviation. Comparison of mean values in 2 groups was made using the unpaired Student’s t-test. The Chi square test with Fischer’s exact test was used to compare discrete variables. Univariate in-hospital mortality hazard risk ratios were estimated for prognostic factors. Kaplan-Meier curve was performed for H-FABP and Troponin I to show survival. A p-value less than 0.05 was considered to be statistically significant. These analyses were performed using the SPSS statistical program package (SPSS version 15.0)
Results
Baseline Demographics
H-FABP was elevated (≥7µg/l) in 17 of the 87 patients (20%). The baseline characteristics of the study population are displayed in Table 1. Concerning baseline characteristics, patients with elevated levels of H-FABP did not differ substantially from those with normal H-FABP levels. To the best of our knowledge none of the patients received known medication which could possibly influence the H-FABP test.
Table 1. Baseline characteristics in 87 consecutive patients with confirmed PE:| FABP pos (≥7ng/ml) n=17 | FABP neg | p-value | |
| (<7ng/ml) n=70 | |||
| Age | 63±17 | 67±17 | n.s. |
| Females n (%) | 11 (65) | 40 (57) | n.s. |
| Hypertension n (%) | 11 (65) | 41 (59) | n.s. |
| Diabetes mellitus n (%) | 7 (41) | 23 (33) | n.s. |
| Hyperlipoproteinaemia n (%) | 7 (41) | 27 (39) | n.s. |
| BMI >30 n (%) | 4 (24) | 14 (20) | n.s. |
| Smoker n (%) | 0 (0) | 3 (4) | n.s. |
| Cancer n (%) | 3 (18) | 11 (16) | n.s. |
| Renal insufficiency (GFR<30) n (%) | 2 (12) | 6 (9) | n.s. |
| Provoked vein thrombosis n (%) | 7 (41) | 23 (33) | n.s. |
| High-risk PE | 6 (35) | 1 (1) | p<0.05 |
| Intermediate-risk PE | 11 (65) | 51 (73) | n.s. |
| Non-high-risk PE | 0 | 18 (26) | p<0,05 |
The great majority of patients presented with intermediate-risk PE. Most patients presenting with high-risk PE where H-FABP positive, while none presenting with non-high-risk PE had a positive H-FABP test.
Clinical Presentation
Patients with Elevated H-FABP on Admission:
Of the 17 patients with elevated H-FABP levels, 6/17 required vasopressor support on admission. The vasoactive substances used were dobutamine and, if not effective alone, norepinephrine as adjunctive therapy. Vasopressors were administered when patients were hypotensive <90/60mmHg though presenting with normal volume status. 5 of these patients requiring vasopressor support on admission also got thrombolysis directly after confirmed diagnosis. One patient had a contraindication for thrombolysis because of a recent operation on a recurrent cerebral astrocytoma. The number of patients needing vasopressor support rose to 15/17 during the hospital stay. In 14 patients cardiopulmonary resuscitation (CPR) during the hospital stay was needed. 12/17 patients received thrombolysis because they all became hemodynamically unstable and had no contraindications against thrombolysis. Thrombolysis was performed straight away as soon as it was indicated. Nevertheless, 14/17 died during hospital stay. Mechanism of death was either prolonged CPR or congestive right heart failure.
Patients with Non-Elevated H-FABP on Admission:
Of the 70 patients with normal H-FABP levels, only 1 needed vasopressors (1%) on admission due to low blood pressure. None needed CPR or deteriorated hemodynamically during the hospital stay. Only 5 patients got thrombolytic therapy because of massive thrombus overload, none of these patients was hemodynamically unstable. Two of them had a floating thrombus in the right atrium and ventricle which fortunately dissolved with thrombolysis so that surgical removal was not needed. No other patient was a potential candidate for acute surgical removal. None of these individuals died during hospital stay. The differences in need for vasopressors, hemodynamic instability and in-hospital mortality between the 2 H-FABP-groups were statistically significant (Figure 1).
Figure 1.Significant differences between the two groups in regard of mortality, acuteness of symptom onset and catecholamine use.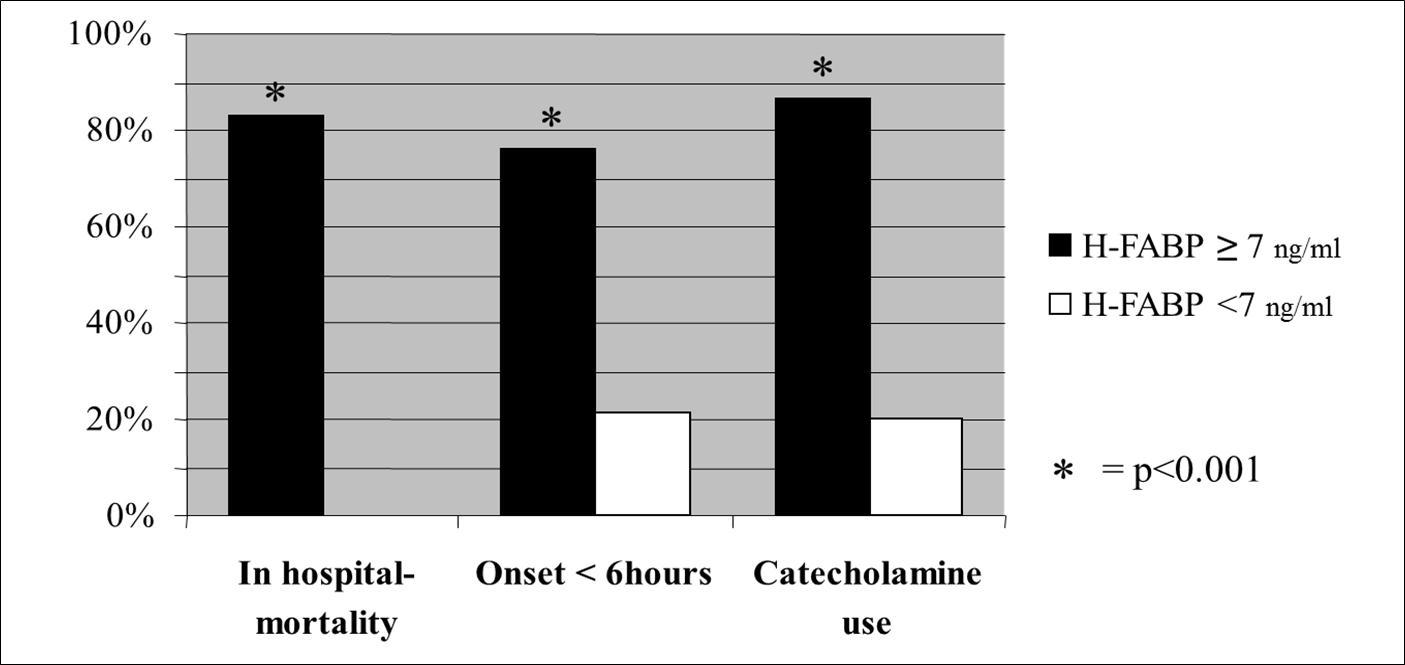
The 30-day survival curves of both positive and negative H-FABP-groups are displayed in Figure 2.
Figure 2.The Kaplan-Meier-Curves (30-day mortality) for H-FABP (a)and Troponin I (b) are displayed. There was no significant difference in 30-day mortality for Troponin ≥ or <0.08 ng/ml.
Echocardiographic Findings
Echocardiographic data of the 2 groups are shown in Figure 3. Of the patients with elevated H-FABP levels, all (100%) had moderate to severely impaired right ventricular ejection fraction compared to only 19/70 patients (27%) of the negative H-FABP group (p<0.001). Paradoxic septal movement and McConnell sign were both seen in 16/17 (94%) of the H-FABP positive group. This is in contrast with the H-FABP negative group, where paradoxic septal movement was seen in only 22/70 (31%) and a positive McConnell sign in only 28/70 (40%) patients (p<0.001). Regarding the RV/LV ratio, 14 17/17 patients (100%) of the H-FABP positive group and 31/70 patients (44%) of the H-FABP negative group had a ratio >1 (p<0,001). Also moderate or severe tricuspid insufficiency was significantly more often seen in the H-FABP positive group than in the H-FABP negative group: 17/17 (100%) and 19/70 (27%), respectively (p<0.001). (Figure 3) When TAPSE was measured, all patients of the H-FABP positive group had a TAPSE <20mm, while in only 15/70 patients (21%) TAPSE <20 mm could be detected. (p<0.001) The mean TAPSE was 13 ± 5mm in the H-FABP positive group and 21± 4 in the H-FABP negative group (p<0.001). Of the 36 patients with moderate to highly impaired RV-function, 14 (39%) died during hospital stay, none died within the next 30 days after onset. No patient of those who died had a normal right ventricular function (data not shown).
Figure 3.Echocardiographic parameters on admission for H-FABP. The presence of mentioned parameters significantly correlates with H-FABP level.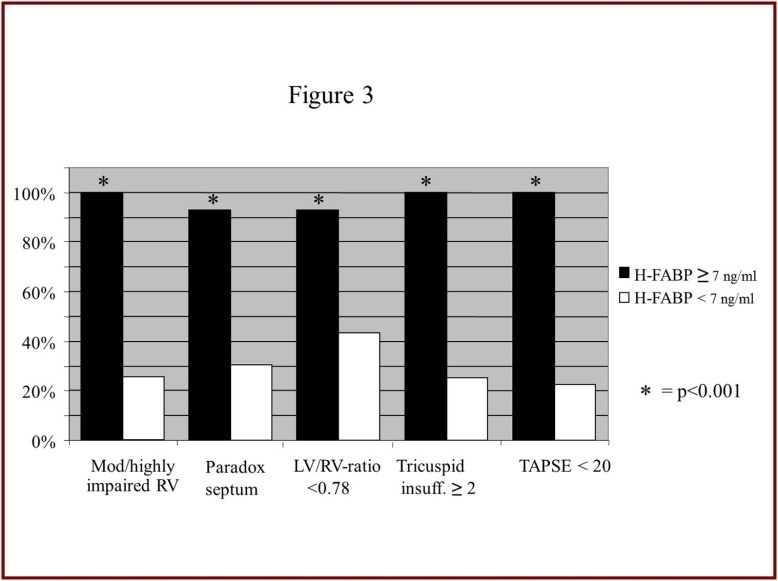
Troponin I and other Biomarkers:
Elevated Troponin I levels did not correlate significantly with mortality (Figure 2b), although a trend towards greater mortality could be seen in patients with elevated Troponin I levels. Regarding the severity of PE, 6/7 (86%) patients with high-risk PE, 36/62 (58%) patients with intermediate risk PE and 6/18 (33%) patients with non-high-risk PE were Troponin I positive. For echocardiographic parameters, we could detect a significant correlation between elevated Troponin I levels and an impaired RV-ejection fraction as well as the presence of paradoxical septal movement. The other right ventricular parameters like TAPSE, LV/RV-ratio and a significant tricuspid insufficiency did not correlate to raised Troponin I levels (Figure 4), although there is a trend towards greater RV-impairment in Troponin I positive patients. For the other biomarkers such as CK, CKMB and D-Dimers, no significant differences could be detected between patients who died and those who survived (data not shown). Negative values of troponin, CK and CKMB correlated well with the absence of significantly impaired RV function and with survival, resulting in a negative predictive value for troponin I of 88% (data not shown).
Figure 4.Echocardiographic parameters on admission for Troponin I. Only for RVEF and the presence of paradoxical septal movement there was a statistically significant difference.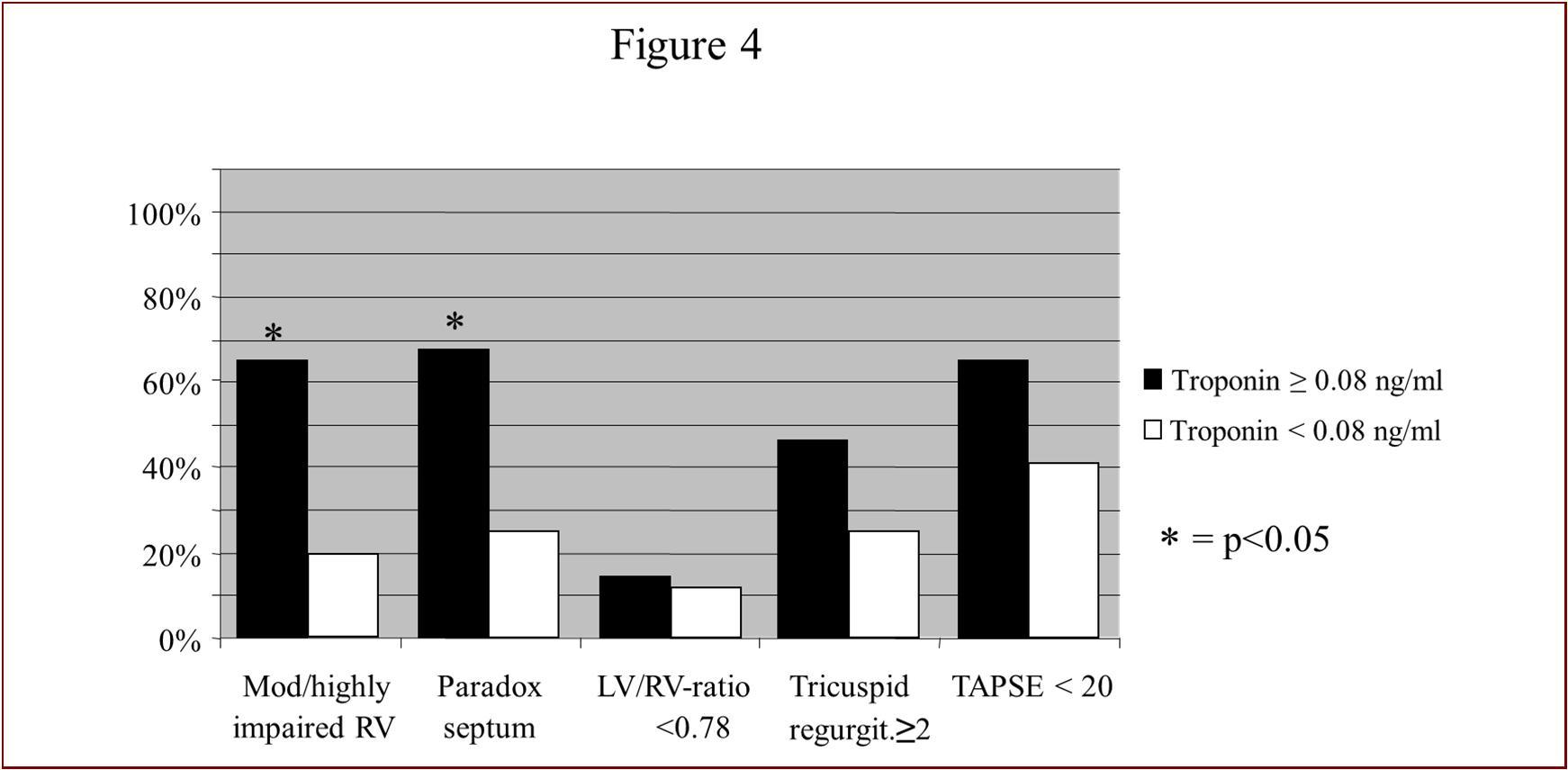
Discussion
One salient finding of our prospective study is that H-FABP seems to be an important prognostic parameter in patients presenting with acute PE. In fact, elevated H-FABP levels were significantly associated with in hospital and 30-day mortality as well as with hemodynamic instability in the course of acute PE. H-FABP correlates significantly with each of the measured echocardiographic parameters of acute right ventricular impairment. It correlates better than troponin, CK, CKMB and D-Dimers with right ventricular dysfunction. At last, negative H-FABP levels had a high predictive value for positive in- hospital and 30-day outcome.
Despite important advances in diagnosis and risk stratification, PE remains an underdiagnosed entity with potentially life-threatening complications. Due to their correlation with in hospital mortality, both echocardiography and raised biomarkers such as troponins have become indispensable tools in the management of patients with PE 5, 20. There are, however, some limitations and caveats for echocardiography and troponin measurements: Echocardiography may not always be available on admission, it requires special training and owing to limited transthoracic window may not be applicable to all patients. Troponin has been shown to be the most reliable biomarker so far; nevertheless, if elevated, it does not necessarily predict bad outcome in all cases.
The abovementioned reasons illustrate that there is still the need for better tools to enable precise risk stratification and thereby permitting early therapeutic and potentially life-saving decisions. This is the reason why our attention was drawn to H-FABP, a biomarker that has gained increasing importance because of its specificity for myocardial damage and its early release. It is considered to be equal or superior to CK, CK-MB, cardiac troponins and myoglobin in the detection of myocardial injury and diagnosis for unstable coronary artery disease 21. Furthermore, elevation of H-FABP is associated with an increased risk of death and major cardiac events in coronary patients 7,21,22. Being a small soluble protein, which is abundantly present in the cytoplasm of cardiomyocytes, it rises earlier than the other biomarkers after the onset of sarcolemmal injury 7.
In our study, many patients with confirmed PE had normal H-FABP-levels suggesting that this parameter is not suitable for the diagnosis of PE. But in view of our data it proved to be a very reliable marker in the prognostic assessment of this study population. This is in accordance with recent reports, where, compared to troponin or N-terminal pro-brain natriuretic peptide, H-FABP was the only biomarker reliably predicting an adverse outcome 11. Collectively, there is accumulating evidence that H-FABP may become an important tool for the management of patients with PE.
In 5 patients with massive thrombus overload the result of the H-FABP test was surprisingly negative. It is tempting to speculate on possible explanations: the visible floating thrombus in the right atrium and ventricle which did not (yet?) embolize into the pulmonary circulation or PE happened several days before, and with H-FABP being positive only until 24 hours after the onset of PE, we may have missed the positive period.
In regard to echocardiographic findings it has been previously shown that right ventricular dysfunction is as an independent predictor of early mortality in PE. This seems true not only in patients presenting with arterial hypotension and cardiogenic shock, but also in normotensive patients 3,4,11,20. In the reported studies, an at least twofold elevation of risk for PE-related mortality could be found in patients with right ventricular dysfunction. Similar results were found in the present study: Of the 36 patients with moderate to highly impaired RV-function, 14 (39%) died during hospital stay. No patient with a normal right ventricular function died in the course of the disease. Thus echocardiography has a very high negative predictive value, although having a low positive predictive value. The present study argues for the additional use of H-FABP in this setting because it permits a better risk stratification since mortality was demonstrated to significantly correlate with elevated H-FABP-levels. Nevertheless we should remember that H-FABP is also elevated in other conditions of myocardial necrosis such as myocardial infarction. Thus, a combination of echocardiography and H-FABP may facilitate the identification of high-risk patients with PE and could thereby help the clinician to consider a close cardiopulmonary monitoring together with aggressive medical therapy including thrombolysis and/or vasoactive therapy.
It has been reported that H-FABP could be falsely positive in patients with renal impairment. In our study, patients with a glomerular filtration rate (GFR) <60ml/min were equally distributed in both groups. By leaving out patients with a GFR <60ml/min from calculations, still the same conclusions of H-FABP could be done. O’Donoghue et al have previously described this same finding in patients with acute coronary syndromes 22.
Ghanima et al recently found a relationship between D-Dimer-levels and the severity of pulmonary embolism in a cohort of 100 consecutive patients based on radiographic and echocardiographic data 11. Although we did not measure the radiographic extent of PE, there was no difference between the D-Dimer levels in the two groups and thus no correlation with echocardiographic data and H-FABP-level.
Despite very promising data, some limitations and caveats should be mentioned: First, although prospective and blinded to the clinician and echocardiographer, it is a single centre trial of consecutive patients. Second, H-FABP was tested only on admission; no further testing was performed during the hospital stay. It seems conceivable that patients who deteriorated during hospital stay due to repetitive emboli could have been detected by serial testing H-FABP. Since this interesting question was beyond our initial study protocol we aim to evaluate this point in detail in the near future.Third, the biomarker NT-pro-Brain natriuretic peptide was not tested, because it has been extensively studied in the past. Additionally, it has been considered as non-specific because associated with a multitude of possible risk factors. Our aim was to compare H-FABP with already established measurements such as the association between troponin I and echocardiography, which has been previously shown to be a reliable predictor for outcome, with NT-pro BNP not showing marked additional advantages. At last, it is a relatively small patient population though similar to other studies with patients presenting with PE. Of course these results will have to be confirmed in a larger cohort of patients.
Conclusion
H-FABP is a promising and very early parameter showing a high correlation with both in hospital and 30-day mortality in patients with acute PE. Furthermore, echocardiographic signs of RV- dysfunction correlated with elevated H-FABP on admission in these patients. It therefore permits rapid risk assessment of patients presenting with PE, thus helping to identify patients most likely to benefit from a more aggressive therapy. Being easily available, it should be performed routinely in every emergency department.
Although being a small study, it showed a great potential benefit in identifying patients at greater risk which should be evaluated further in bigger studies.
References
- 1.Alpert J S, Smith R, Carlson J, Ockene I S, Dexter L et al. (1976) Mortality in patients treated for pulmonary embolism. , JAMA 236, 1477-80.
- 2.Carson J L, Kelley M A, Duff A, Weg J G, Fulkerson W J et al. (1992) The clinical course of pulmonary embolism. , N Engl J Med 326, 1240-45.
- 3.Kucher N, Rossi E, M De Rosa, Goldhaber S Z. (2005) Prognostic role of echocardiography among patients with acute pulmonary embolism and a systolic arterial pressure of 90 mm Hg or higher. , Arch Intern Med 165, 1777-81.
- 4.Goldhaber S Z, Visani L, M De Rosa. (1999) Acute pulmonary embolism: clinical outcomes in the International Cooperative Pulmonary Embolism Registry (ICOPER). , Lancet 353, 1386-89.
- 5.Konstantinides S, Geibel A, Olschewski M, Kasper W, Hruska N et al. (2002) Importance of cardiac troponins I and T in risk stratification of patients with acute pulmonary embolism. , Circulation 106, 1263-68.
- 6.Hsu J T, Chu C M, Chang S T, Cheng H W, Cheng N J et al. (2006) Prognostic role of right ventricular dilatation and troponin I elevation in acute pulmonary embolism. , Int Heart J 47, 775-81.
- 7.Nagahara D, Nakata T, Hashimoto A, Takahashi T, Kyuma M et al. (2006) Early positive biomarker in relation to myocardial necrosis and impaired fatty acid metabolism in patients presenting with acute chest pain at an emergency room. , Circ J 70, 419-25.
- 8.Chmurzynska A. (2006) The multigene family of fatty acid-binding proteins (FABPs): function, structure and polymorphism. , J Appl Genet 47, 39-48.
- 9.Iida K, Nagao K, Uchiyama T, Kushiro T. (2005) Relationship between heart-type fatty acid-binding protein levels and the risk of death in patients with serious condition on arrival at the emergency department. , Intern Med 44, 1039-45.
- 10.Kaczynska A, Pelsers M M, Bochowicz A, Kostrubiec M, Glatz J F et al. (2005) Plasma heart-type fatty acid binding protein is superior to troponin and myoglobin for rapid risk stratification in acute pulmonary embolism. , Clin Chim Acta 371, 117-23.
- 11.Puls M, Dellas C, Lankeit M, Olschewski M, Binder L et al. (2006) Heart-type fatty acid-binding protein permits early risk stratification of pulmonary embolism. , Eur Heart J 28, 224-29.
- 12.Torbicki A, Perrier A, Konstantinides S, Agnelli G, Gallié N et al. (2008) Guidelines on the diagnosis and management of acute pulmonary embolism. , Eur Heart J 29, 2276-2315.
- 13.Hsiao S H, Chang S M, Lee C Y, Yang S H, Lin S K et al. (2006) Usefulness of tissue Doppler parameters for identifying pulmonary embolism in patients with signs of pulmonary hypertension. , Am J Cardiol 98, 685-90.
- 14.Kjaergaard J, Schaadt B K, Lund J O, Hassager C. (2006) Quantitative measures of right ventricular dysfunction by echocardiography in the diagnosis of acute nonmassive pulmonary embolism. , J Am Soc Echocardiogr 19, 1264-71.
- 15.Haghi D, Sueselbeck T, Poerner T, Borggrefe M, Haase K K. (2005) A novel regional right ventricular wall-motion abnormality observed in a case of acute pulmonary embolism (reverse McConnell sign). , J Am Soc Echocardiogr 18, 75-77.
- 16.Miller D, Farah M G, Liner A, Fox K, Schluchter M et al. (2004) The relation between quantitative right ventricular ejection fraction and indices of tricuspid annular motion and myocardial performance. , J Am Soc Echocardiogr 17, 443-47.
- 17.Ueti O M, Camargo E E, Ueti A A, Lima-Filho E C, Nogueira E A. (2002) Assessment of right ventricular function with Doppler echocardiographic indices derived from tricuspid annular motion: comparison with radionuclide angiography. , Heart 88, 244-48.
- 18.Seino Y, Tomita Y, Takano T, Ohbayashi K. (2004) Office cardiologists cooperative study on whole blood rapid panel tests in patients with suspicious acute myocardial infarction: comparison between heart-type fatty acid-binding protein and troponin T tests. , Circ J 68, 144-48.
- 19.Levey A S, Bosch J P, Lewis J B, Greene T, Rogers N et al. (1999) A more accurate method to estimate glomerular filtration rate from serum creatinine: a new prediction equation. , Modification of Diet in Renal Disease Study Group. Ann Intern Med 130, 461-70.
- 20.Konstantinides S. (2005) Pulmonary embolism: impact of right ventricular dysfunction. , Curr Opin Cardiol 20, 496-501.
Cited by (1)
- 1.Bajaj Anurag, Rathor Parul, Sehgal Vishal, Shetty Ajay, Kabak Besher, et al, 2015, Risk stratification in acute pulmonary embolism with heart-type fatty acid–binding protein: A meta-analysis, Journal of Critical Care, 30(5), 1151.e1, 10.1016/j.jcrc.2015.05.026
