Abstract
Background
Eighty five percent of cervical cancer occurrence in resource-poor countries. Contributing factors for these are inadequate knowledge about the disease, early initiation of sexual intercourse and multiple sexual partners. Early screening is an intervention in reduction of maternal deaths due to cervical cancer. Consequently this study was conducted aiming to find out about the practice of cervical cancer screening and its associated factors.
Methods
A facility based cross sectional study was conducted using a pretested structured questionnaire among women attended Maternal and Child Health (MCH) department of Felege Hiwot Referral Hospital (FHRH) from March15 to April 15, 2019. The study participants were selected systematically. The collected data were entered and analyzed using SPSS version 20. Logistic regression analysis was employed to examine factors association with cervical cancer screening that was confirmed using AOR with its 95% CI.
Results
A total of 400 study participants were included with a response rate of 99.5%. Of the total study participants only 78 (19.5%; 95% CI: 15.6, 23.4) practiced screening for cervical cancer. The cervical cancer screening practice was affected by age (AOR=2.025; 95% CI: 1.118, 3.668). Of those women who had ever heard of about cervical cancer were seven fold more likely to practice cervical screening (AOR=6.924; 95% CI: 1.602, 29.928) compared to those who did not have any information before. Moreover, knowing genital tract discharge as a problem of female organ implement fourfold more likely compared to that of knowing nothing about problem of genital tract (AOR=3.766; 95% CI: 1.761,8.055).
Conclusion and Recommendation
The study depicted there was low utilization of cervical cancer screening. Awareness creation about cervical cancer and knowledge of genital tract problems had positive influence for screening practice.
Author Contributions
Academic Editor: Hong Zhang, China.
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2021 Tenagnework Antefe Abebe, et al
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Introduction
Majority (85%) of cervical cancer occurs as global burden in less developed regions with an estimate of 528,000 cases every year worldwide. It ranks the fourth most cancer affecting women 1.
Low and middle income countries approximately contributed 90% the total deaths occurred from cervical cancer in 20152. Nearly half a million women will die of cervical cancer by 2030.From these, low and middle-income countries will have more than 98% deaths 3.
Cervical cancer is also common in Eastern Africa region and in Ethiopia, which is estimated as, 45,707 new cases and 28,197 deaths, and 7,095 new cases and 4,732 deaths every year respectively 4.
The first top cancer in adults above age of 14 years old is cervical cancer which was the second most common of all cancers (15.2%) based on a study handled at Gondar referral hospital in 20165.
Cervical cancer, malignant neoplasm arising from cells originating in cervix uteri, may be completely asymptomatic in early stages 6. It can be presented as persistent pelvic pain, unexplained weight loss, bleeding between periods, unusual vaginal discharge, bleeding, and pain after sexual intercourse 7. Globally, 75% of cervical cancer is initiated by human papilloma virus (HPV) types 16 and 18 infection while other risk factors like tobacco consumption, multiple sexual partners, early age of sexual intercourse, increasing parity, prolonged use of oral contraceptive pills, and sexually transmitted diseases also subsidized the rest 8, 9.
Ethiopia lost around 4,732 women per year, cancer related highest mortality rate, due to cervical cancer with an adjusted incidence of 18.9 per 100, 000 women. These may be also underestimated by way of low level of awareness, screening and diagnostic limited access and national cancer registry unavailability10, 11, 12, 13.
Screen and treat cervical cancer with a single-visit approach is suggested by many studies in low-resource settings as the most successful and cost-effective way since Papanicolaou (pap) smear is used in a limited scope and no national screening program in Ethiopia14.
Studies which assess the current knowledge of women about cervical cancer and their preventive practice in Ethiopia are rare particularly in the study area. Identifying practice and its associated factors related to cervical cancer screening among women of age ≥21 will enable to reverse the increasing trend of cervical cancer in Ethiopia particularly in FHRH, and there by its immediate and long term consequences through design of effective preventive strategies Figure 1.
Figure 1.Conceptual framework for factors influencing cervical cancer screening practice taken from review literature and adapted contextually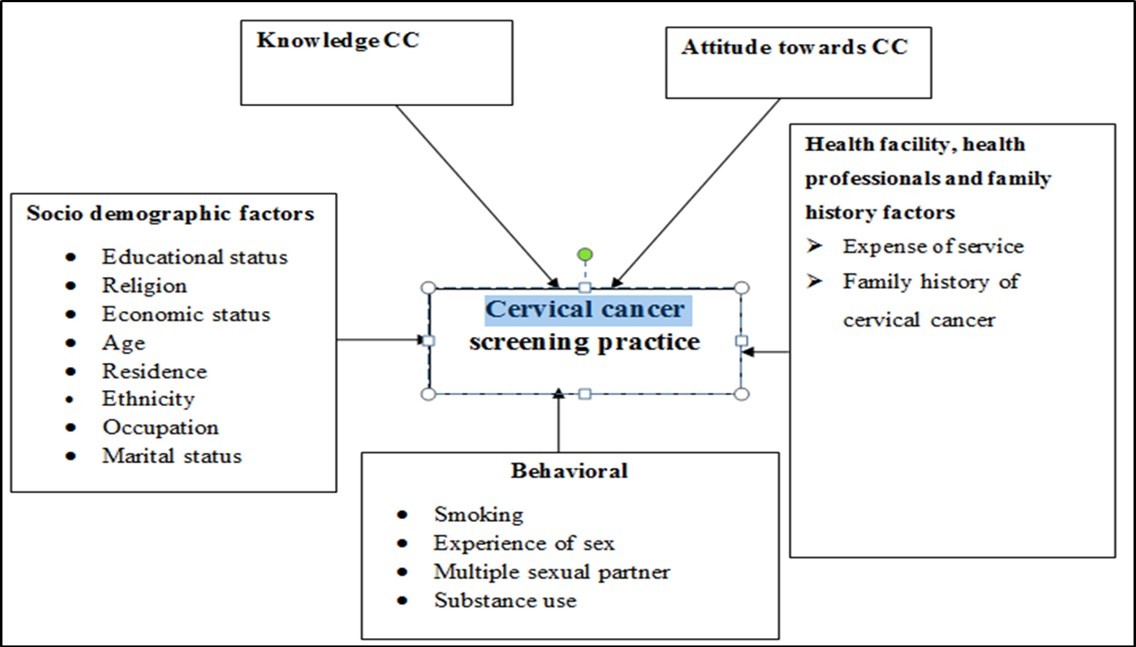
Methods and Materials
Study Periods and Setting
An institutional based quantitative cross-sectional study was conducted in Maternal and child health department Felege Hiwot Referral Hospital from March 15 -April 15, 2019.
Target Population
All women aged ≥21 years who were attending in Felege Hiwot Referral Hospital at MCH department to obtain different health services. Women unable to communicate due to their sick condition were excluded from the study.
Sample Size Determination and Sampling Technique
The sample size was determined using single population proportion formula using the following assumptions: 95% level of confidence, proportion of women have been screened for cervical cancer, 19.8% community based cross-sectional study conducted in Mekellezone15, 5% margin of error (desired precision between sample and population parameter), design effect 1.5, and contingency of 10% for possibilities of non–response rate and incomplete data. The calculated sample size was = 402.
Sample size was allocated to each MCH departments based on the proportion of eligible women (Figure 2). Selected study subjects at each MCH department using systematic random sampling every 5th entry at each department during study period, and interviewed to collect information until the proportion of the sample size reached. The first participant was drawn using lottery method random sampling technique.
Figure 2.Sampling technique for cervical cancer screening practice among women aged ≥21 years who have attended MCH Department at Felege Hiwo Referral Hospital, Amhara Region, Ethiopia, 2019.
Data Collection Instrument and Procedure
A Semi-structured and pretested questionnaire was used to collect data on demographic, knowledge, and practice assessing questions. The data collection tool (questionnaire) was adapted by reviewing literature16. Face-to face interview was used.
The questionnaire was initially prepared in English and translated into the local language (Amharic) by fluent speakers of both languages to maintain its consistency. Training was given for data collectors and about the objectives, methods, tool and ethics (confidentiality and privacy) of the study to be conducting; and pre-test was conducted on 5% of the sample in an area where the study was not be undertaken; with similar set up in order to assess the quality of the data collection tool, and time consuming. Based on the pre-test finding modification was made on the questionnaire. Data was collected only by trained data collectors and supervised by trained supervisor. Regular meetings were held between the data collectors, supervisor, and principal investigator to solve problematic issues faced during data collection period. Each questionnaire was checked for completeness and consistency daily.
Data were coded and entered, cleaned, analyzed using statistical package for social science (SPSS) version 20. Frequency and cross tab was performed to clean the data. Descriptive statistics (Frequency distribution, percentages, graphs and proportion) was computed. A binary logistic regression was used to identify associated factors. Adjusted Odds ratios at 95% confidence interval were used to see the significance of the study and the strength of association between study variables.
Ethical Consideration and Permission
Ethical approval was obtained from Institutional Review Board of GAMBY medical & Business College. An official letter of co-operation was written from GAMBY medical & Business College of science by department of public health to Amhara public Health institute and then to Felege Hiwot Referral Hospital. Respondents were informed about the objectives and purpose of the study to obtain verbal consent from each respondent before interview. A one page cover information sheet that explained the purpose, procedure and significance of the study was attached with each questionnaire. The data were maintained confidential and used only the purpose of this study.
Operational Definitions
1. Knowledgeable: refers those who respond ‘Yes’ for Yes/No knowledge measuring questions and minimum one of the alternatives except the alternative ‘I don’t know’ for multiple questions.
2. Attitude: refer those who answer attitude questions scored above the mean have positive attitude while, those who answered below the mean said to be negative attitude.
3. Ever been diagnosed for cervical cancer (Practice) woman that has been diagnosed for cervical cancer in the past pelvic examination Pap or VIA test.
4. multiple sexual partners is to identify those who have had sexual intercourse with more than one partner
5. Smoking - questions are responded yes or no for active smoking practices and those who respond yes are analyzed as below 10 years and above.
6. Substance abuse is any response other than never to any of the substance questions chat, alcohol, marijuana, narcotic &drugs.
Results
Socio-Demographic Status Factors of Respondents
A total of 400 women were included with a response rate of 99.5%. Of these, 53.8%, 92.8%, 95.0%, 80.5%, 36.5%, 78.5%, 42.8% and 27.2% were at the age group of 21-29 years, Orthodox Christian, Amhara ethnic group, married, at college and above educational status, rural dweller, housewife and earned less than 1001 Ethiopian Birr per month correspondingly as stated on table 1.
Table 1. Socio demographic status of study participants at maternal and child health department in FHRH from March 15- April 15, 2019 (n=400)| Variable | Category | Frequency | Percent |
| Age of women | 21-29 Years | 215 | 53.8 |
| 30-65 Years | 185 | 46.2 | |
| Religion | Orthodox | 371 | 92.8 |
| Protestant | 8 | 2.0 | |
| Muslim | 21 | 5.2 | |
| Ethnic group | Amhara | 380 | 95.0 |
| Oromo | 10 | 2.5 | |
| Tigirie | 4 | 1.0 | |
| Agew | 6 | 1.5 | |
| Marital status | Single | 53 | 13.2 |
| Married | 322 | 80.5 | |
| Separated | 11 | 2.8 | |
| Widowed | 7 | 1.8 | |
| Divorced | 7 | 1.8 | |
| Educational status | Unable to read and write | 90 | 22.5 |
| Able to read and write | 35 | 8.8 | |
| Primary | 48 | 12.0 | |
| Secondary | 81 | 20.2 | |
| College and above | 146 | 36.5 | |
| Residence | Urban | 314 | 78.5 |
| Rural | 86 | 21.5 | |
| Occupation | Student | 26 | 6.5 |
| Self | 55 | 13.8 | |
| Government employee | 111 | 27.8 | |
| Private employee | 22 | 5.5 | |
| Housewife | 171 | 42.8 | |
| No work | 15 | 3.8 | |
| Monthly income (Ethiopian birr) | up to 1000 | 109 | 27.2 |
| 1001-2000 | 107 | 26.8 | |
| 2001-2500 | 25 | 6.2 | |
| 2501-4500 | 84 | 21.0 | |
| > 4501 | 75 | 18.8 |
Behavioral, Health Facility and Family History Factors of Respondents
Six (1.5%) individuals smoke cigarette from two to five years. On other hand, 29 (7.2%) of the participants were addicted to different substance use (khat, alcohol and stimulant drugs) that ranges from one to fifteen years and 353 (88.2%) experienced sexual intercourse; of them 278 (78.8%) have been experienced with one sexual partner (Table 2).
Table 2. Family history of women cervical cancer of study participants at maternal and child Health Department in FHRH from March 15- April 15, 2019 (n=400).| Variable | Category | Frequency | Percent |
| Family history for Cervical CA | Yes | 50 | 12.2 |
| No | 350 | 87.8 | |
| Relationship of family history | Mother | 15 | 30.0 |
| Sister | 15 | 30.0 | |
| Grandmother | 2 | 4.0 | |
| Aunt | 8 | 16.0 | |
| Other | 10 | 20.0 | |
| Experienced sexual intercourse | Yes | 353 | 88.2 |
| No | 47 | 11.8 | |
| Number of sexual partner (s) (n=353) | One person | 278 | 78.8 |
| Two person | 53 | 15.0 | |
| Three person | 14 | 4.0 | |
| Five and more | 8 | 2.3 | |
| Addicted with substance abuse | Yes | 29 | 7.2 |
| No | 371 | 92.8 |
Knowledge of Study Participants about Cervical Cancer
A quarter of study participants did not hear about cervical cancer (Table 3). Many of the participants also did not know about cause of cervical cancer (48.0%), symptom of cervical cancer (30.8%) and treatment of cervical cancer (39.0%).
Table 3. Knowledge of study participants about cervical cancer screening at maternal and child Health Department in FHRH from March 15- April 15, 2019 (n=400).| Variable | Category | Frequency | Percent |
| Problems of genital tract | I don't know | 180 | 45 |
| Discharge | 97 | 24.2 | |
| Sexual transmitted disease | 38 | 9.5 | |
| Cervical cancer | 59 | 14.8 | |
| Uterine tumor | 26 | 6.5 | |
| Ever heard about cervical cancer | Yes | 306 | 76.5 |
| No | 94 | 23.5 | |
| Causes of cervical cancer | I don't know | 192 | 48 |
| Any sexual partner | 24 | 6 | |
| Early initiation of sexual intercourse | 39 | 9.8 | |
| Havening multiple sexual partner | 67 | 16.8 | |
| Sexual transmitted disease | 19 | 4.8 | |
| HIV | 11 | 2.8 | |
| Papiloma virus | 18 | 4.5 | |
| Long years use of Combined oral contraceptives | 16 | 4 | |
| Other | 14 | 3.5 | |
| symptoms of cervical cancer | I Don’t know | 123 | 30.8 |
| Bleeding | 94 | 23.5 | |
| Post coital bleeding | 25 | 6.2 | |
| Vaginal foul smelling discharges | 100 | 25 | |
| Painful coitus | 29 | 7.2 | |
| Post-menopausal bleeding | 29 | 7.2 | |
| Treatment of cervical cancer | I don’t know | 156 | 39 |
| Surgery | 95 | 23.8 | |
| Chemotherapy | 70 | 17.5 | |
| Radiotherapy | 72 | 18 | |
| Others | 7 | 1.8 | |
| The outcomes early undetected of cervical cancer | I don’t know | 84 | 21 |
| Metastasis | 82 | 20.5 | |
| Chronic illness | 19 | 4.8 | |
| Bleeding | 8 | 2 | |
| Death | 202 | 50.5 | |
| Other | 5 | 1.2 | |
| Ever heard of cervical cancer screening method | Yes | 304 | 76 |
| No | 96 | 24 | |
| Methods of cervical cancer screening | VIP | 145 | 36.2 |
| Pap smear | 159 | 39.8 | |
| Who should be screened | I don't know | 99 | 24.8 |
| Age greater than 21 | 114 | 28.5 | |
| Commercial sex workers | 71 | 17.8 | |
| Elderly women | 104 | 26 | |
| Other | 12 | 3 | |
| Frequency of screening | Every year | 185 | 46.2 |
| Every two year | 54 | 13.5 | |
| Every three year | 74 | 18.5 | |
| Every five year | 43 | 10.8 | |
| Other | 44 | 11 | |
| Expense of cervical cancer screening | I don’t know | 135 | 33.8 |
| Free | 105 | 26.2 | |
| It is reasonably priced | 47 | 11.8 | |
| moderately expensive | 54 | 13.5 | |
| very expensive | 59 | 14.8 | |
| Reason of cervical cancer screening | I do not know | 117 | 29.2 |
| To check cervix | 218 | 54.5 | |
| To check infections passed through sex | 24 | 6 | |
| To check infections transmitted through blood transfusion | 18 | 4.5 | |
| Others | 23 | 5.8 | |
| Cervical cancer preventable | Yes | 344 | 86 |
| No | 56 | 14 | |
| Prevention method cervicalcancer | I do not know | 60 | 17.4 |
| No multiple partner | 151 | 43.9 | |
| Treat papiloma virus | 52 | 15.1 | |
| Use condom | 36 | 10.5 | |
| Vaccine | 30 | 8.7 | |
| Other | 15 | 4.4 |
Among the study participants who had ever heard about cervical cancer (306), majority got the information from media (41.8%) while the least numbers heard from religious leaders (figure 3).
Figure 3.Source of information about cervical cancer among study participants at maternal and child Health Department in FHRH from March 15- April 15, 2019.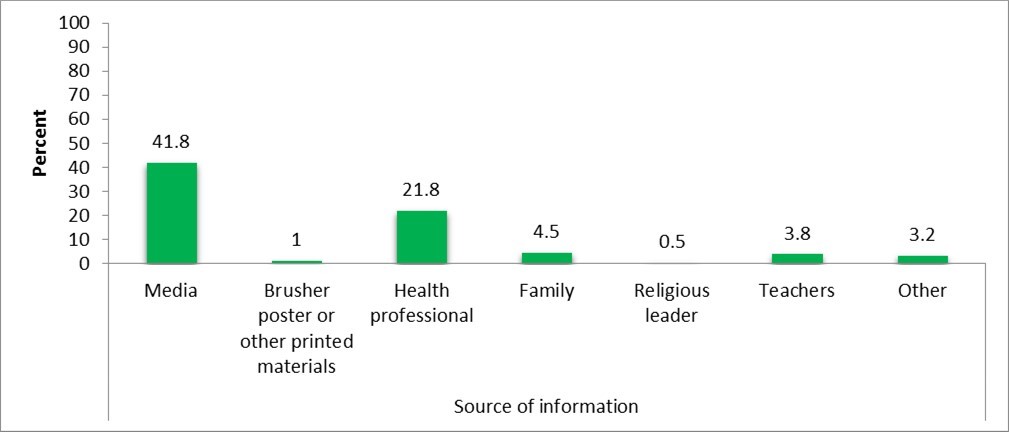
Attitude Assessment of Cervical Screenings
Out of total (400) participants 56.2% had good attitude about cervical cancer screening and 43.8 % were by the side of poor attitude with mean score of 31.725+4.71559 for the eight questionnaires (figure 4).
Figure 4.Attitude of study participants about cervical cancer screening at maternal and child Health Department in FHRH from March 15- April 15, 2019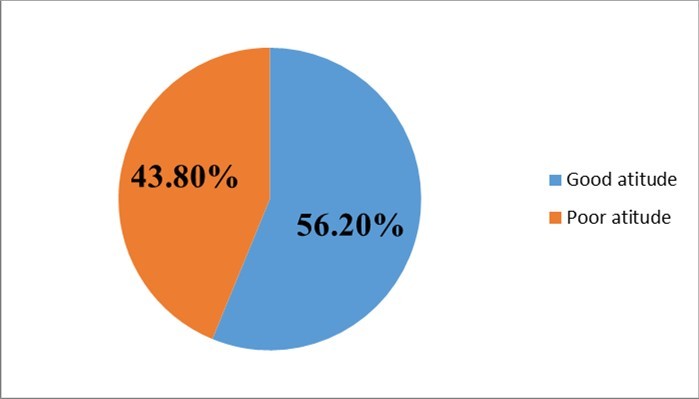
Practice of Cervical Cancer Screenings
Recent study showed that, out of total 78(19.5%) had practiced cervical cancer screening, 77 ̸ 78 (98.7) did it at once in their life (Table 4). Of these, three (3.9%), 32 (41.0%) and 43 (55.1%) explained it should be practiced with a frequency of every year, two years and three years respectively.
Table 4. Cervical cancer screening practice of study participants at maternal and child Health Department in FHRH from March 15- April 15, 2019 (n=400).| Variable | Category | Frequency | Percent |
| Have you ever screened for cervical cancer | Yes | 78 | 19.5 |
| No | 322 | 80.5 | |
| Time of last cervical cancer screening | less than two years | 50 | 64.1 |
| Two to three years | 19 | 24.4 | |
| Greater than three years | 9 | 11.5 | |
| Method of screening | PAP smear | 50 | 64.1 |
| VIA | 17 | 21.8 | |
| Both method | 11 | 14.1 | |
| Reason of not to get screening | Screening is painful | 44 | 11.0 |
| Healthy | 129 | 32.2 | |
| Her husband would not agree | 9 | 2.2 | |
| No information about screening | 58 | 14.5 | |
| Not informed health professional | 69 | 17.2 | |
| Workload | 11 | 2.8 | |
| Other | 2 | 0.5 |
Association of Socio-Demographic Characteristics
Participants whose age belong to the range of 30-65years were two times more likely to have a good level of performance (AOR=2.025; 95% CI: 1.118, 3.668) than those age were fallen in the range of 21-29 years (Table 5). Of the total study participants family history about cervical cancer were two fold more likely to practice cervical cancer screening than who do not have (AOR =2.441; 95% CI: 1.278, 4.661) while, who had ever heard about cervical cancer were seven fold more likely to practice cervical screening (AOR=6.924; 95% CI: 1.602, 29.928) compared to those who did not have any information before. Moreover, knowing genital tract discharge as a problem of female genital organ implement fourfold more likely compared to that of knowing nothing about problem of genital tract (AOR=3.766; 95% CI: 1.761,8.055) (Table 6).
Table 5. Association of socio demographic status of study participants to the practice of cervical cancer screening at maternal and child health department in FHRH from March 15-April15, 2019| Variable | Category | Have you ever screened for cervical cancer | X2 test /Fisher exact test/ | COR ( 95%CI) | AOR at 95%CI | |
| Yes | No | |||||
| Age group | 21-29 Years | 34 | 181 | 0.045 | 1 | 1 |
| 30-65 Years | 44 | 141 | 1.661(1.009,2.736) | 2.025(1.118,3.668) | ||
| Religion | Orthodox | 71 | 300 | 0.000* | ||
| Protestant | 6 | 2 | ||||
| Muslim | 1 | 20 | ||||
| Ethnic group | Amhara | 75 | 305 | 0.371* | ||
| Oromo | 3 | 7 | ||||
| Tigirie | 0 | 4 | ||||
| Agew | 0 | 6 | ||||
| Marital status of women | Single | 6 | 47 | 0.210* | ||
| Married | 70 | 252 | ||||
| Separated | 1 | 10 | ||||
| Widowed | 1 | 6 | ||||
| Divorced | 0 | 7 | ||||
| Educational status of women | Unable to read and write | 15 | 75 | 0.834 | ||
| Able read and write | 6 | 29 | ||||
| Primary | 10 | 38 | ||||
| Secondary | 19 | 62 | ||||
| College and above | 28 | 118 | ||||
| Address of women | Urban | 65 | 249 | 0.247 | ||
| Rural | 13 | 73 | ||||
| Occupation of women | Student | 3 | 23 | 0.215 | ||
| Self | 11 | 44 | ||||
| Government employee | 30 | 81 | ||||
| Private employee | 5 | 17 | ||||
| Housewife | 27 | 144 | ||||
| No work | 2 | 13 | ||||
| Monthly income (Ethiopian birr) | up to 1000 | 14 | 95 | 0.192 | ||
| 1001-2000 | 20 | 87 | ||||
| 2001-2500 | 7 | 18 | ||||
| 2501-4500 | 18 | 66 | ||||
| greater than 4501 | 19 | 56 | ||||
| Category | Have you ever screened for cervical cancer | X2 test | COR at 95% CI | AOR at 95% CI | ||
| Yes | No | |||||
| Family history of cervical cancer | Yes | 17 | 32 | 0.006 | 2.441(1.278, 4.661) | |
| No | 61 | 290 | 1 | |||
| Experience of sexual intercourse | Yes | 71 | 282 | 0.396 | ||
| No | 7 | 40 | ||||
| Problem of genital tract of women | I don't know | 22 | 158 | 0.018 | 1 | 1 |
| Discharge | 27 | 70 | 2.770(1.476, 5.198) | 3.766(1.761,8.055) | ||
| Sexual transmitted disease | 9 | 29 | 2.229(0.933, 5.324) | 1.872(0.664,5.281) | ||
| Cervical cancer | 13 | 46 | 2.030(0.949, 4.341) | 2.091(0.864,5.059) | ||
| Uterine tumor | 7 | 19 | 2.646(0.998, 7.012) | 2.709(0.871,8.425) | ||
| Ever heard of cervical cancer | Yes | 74 | 232 | 0 | 7.177(2.549, 20.206) | 6.924(1.602,29.928) |
| No | 4 | 90 | 1 | 1 | ||
| Source of information about Cervical Cancer | Media | 36 | 130 | 0.032* | ||
| Brusher poster other printed material | 2 | 1 | ||||
| Health professional | 24 | 63 | ||||
| Family | 4 | 14 | ||||
| Religious leader | 2 | 0 | ||||
| Teachers | 3 | 12 | ||||
| Other | 2 | 11 | ||||
| Causes of cervical cancer | I don't know | 27 | 165 | 0.026* | ||
| Any sexual partner | 8 | 16 | ||||
| Early initiation of sexual intercourse | 12 | 27 | ||||
| Havening multiple sexual partner | 11 | 56 | ||||
| Sexual transmitted disease | 3 | 16 | ||||
| HIV | 5 | 6 | ||||
| Papiolma virus | 5 | 13 | ||||
| Long years use of Combined oral contraceptives | 5 | 11 | ||||
| Other | 2 | 12 | ||||
| Symptom of cervical cancer of women | I Don’t know | 10 | 113 | 0.002 | 1 | |
| Bleeding | 21 | 73 | 3.251(1.448,7.296) | |||
| Post coital bleeding | 4 | 21 | 2.152(0.617,7.509) | |||
| Vaginal foul smelling discharges | 27 | 73 | 4.179(1.910,9.144) | |||
| Painful coitus | 6 | 23 | 2.948(0.974,8.918) | |||
| Post-menopausal bleeding | 10 | 19 | 5.947(2.183,16.203) | |||
| Treatment of cervical cancer | I don’t know | 22 | 134 | 0.125 | ||
| Surgery | 23 | 72 | ||||
| Chemotherapy | 16 | 54 | ||||
| Radiotherapy | 17 | 55 | ||||
| Others | 0 | 7 | ||||
| Outcome of untreated cervical cancer | I don’t know | 2 | 82 | 0.000* | ||
| Metastasis | 19 | 63 | ||||
| Chronic illness | 6 | 13 | ||||
| Bleeding | 3 | 5 | ||||
| Death | 48 | 154 | ||||
| Other | 0 | 5 | ||||
| Ever heard of cervical cancer screening method | Yes | 68 | 236 | 0.01 | 2.478(1.220,5.031) | |
| No | 10 | 86 | 1 | |||
| Who should be screened | I don't know | 8 | 91 | 0.005 | 1 | |
| agegreaterthan21 | 20 | 94 | 2.420(1.015,5.772) | |||
| Commercial sex workers | 20 | 51 | 4.461(1.834,10.849) | |||
| Elderly women | 27 | 77 | 3.989(1.713,9.288) | |||
| Other | 3 | 9 | 3.792(0.852,16.878) | |||
| Expense of screening | I don’t know | 9 | 126 | 1 | ||
| Free | 26 | 79 | 0 | 4.608(2.053,10.342) | ||
| It is reasonably priced | 14 | 33 | 5.939(2.365,14.918) | |||
| moderately expensive | 14 | 40 | 4.900(1.973,12.171) | |||
| very expensive | 15 | 44 | 4.773(1.951,11.678) | |||
| Expense of screening | I don’t know | 9 | 126 | 1 | ||
| Free | 26 | 79 | 0 | 4.608(2.053,10.342) | ||
| It is reasonably priced | 14 | 33 | 5.939(2.365,14.918) | |||
| moderately expensive | 14 | 40 | 4.900(1.973,12.171) | |||
| very expensive | 15 | 44 | 4.773(1.951,11.678) | |||
| Reason of screening | Do not know | 14 | 103 | 0.152* | ||
| To check cervix | 50 | 168 | ||||
| To check infections passed through sex | 4 | 20 | ||||
| To check infections passed through blood transfusion | 4 | 14 | ||||
| Others | 6 | 17 | ||||
| Is cervical cancer preventable | Yes | 70 | 274 | 0.288 | ||
| No | 8 | 48 | ||||
| Prevention method of cervical cancer | I do not know | 2 | 58 | 0.017 | 1 | |
| No multiple partner | 38 | 113 | 9.752(2.272,41.855) | |||
| Treat papilomavirus | 11 | 41 | 7.780(1.637,36.982) | |||
| Use condom | 9 | 27 | 9.667(1.954,47.820) | |||
| Vaccine | 6 | 24 | 7.250(1.365,38.494) | |||
| Other | 4 | 11 | 10.545(1.716,64.802) | |||
| Know age of cervical cancer manifestation | Yes | 69 | 294 | 0.437 | ||
| No | 9 | 28 | ||||
| Know the right sex starting age group | Yes | 69 | 242 | 0.009 | 5.560(1.309,23.607) | |
| No | 2 | 39 | 1 | |||
| Had good attitude towards cervical cancer screening | Yes | 40 | 185 | 0.324 | ||
| No | 38 | 137 | ||||
Factors of Cervical Cancer Screening Practice
Of the total study participants who had ever heard about cervical cancer were seven fold more likely to practice cervical screening (AOR=6.924; 95% CI: 1.602, 29.928) as compared to those who did not have any information before. Moreover, knowing genital tract discharge as a problem of female genital organ implement fourfold more likely compared to that who have nothing knowledge about genital tract problems (AOR=3.766; 95% CI: 1.761,8.055) (Table 7)
Table 7. Association of knowledge and attitude of study participants to the practice of cervical cancer screening at maternal and child health department in FHRH from March 15-April 15, 2019.| Variable | Have you ever screened for cervical cancer | COR at 95% CI | AOR at 95% CI | |
| Yes | No | |||
| Age group | ||||
| 21-29 Years | 34 | 181 | 1 | 1 |
| 30-65 Years | 44 | 141 | 1.661(1.009, 2.736) | 2.025(1.118,3.668) |
| Family history of cervical cancer | ||||
| Yes | 17 | 33 | 2.441(1.278, 4.661) | 1.572(0.673,3.670) |
| No | 61 | 289 | 1 | |
| Experience of sexual intercourse | ||||
| Yes | 71 | 282 | 1.439(0.619,3.346) | |
| No | 7 | 40 | 1 | |
| Problem of genital tract of women | ||||
| Discharge | 27 | 70 | 2.770(1.476, 5.198) | 3.766(1.761,8.055) |
| STD | 9 | 29 | 2.229(0.933, 5.324) | 1.872(0.664,5.281) |
| Cervical cancer | 13 | 46 | 2.030(0.949, 4.341) | 2.091(0.864,5.059) |
| Uterine tumor | 7 | 19 | 2.646(0.998, 7.012) | 2.709(0.871,8.425) |
| I don't know | 22 | 158 | 1 | 1 |
| Ever heard of cervical cancer | ||||
| Yes | 74 | 232 | 7.177(2.549, 20.206) | 6.924(1.602,29.928) |
| No | 4 | 90 | 1 | 1 |
| Symptom of cervical cancer of women | ||||
| Bleeding | 21 | 73 | 3.251(1.448,7.296) | 1.022(0.299,3.494) |
| Post coital bleeding | 4 | 21 | 2.152(0.617,7.509) | 0.804(0.156,4.154) |
| Vaginal foul smelling discharges | 27 | 73 | 4.179(1.910,9.144) | 1.460(0.436,4.889) |
| Painful coitus | 6 | 23 | 2.948(0.974,8.918) | 2.001(0.416,9.624) |
| Post-menopausal bleeding | 10 | 19 | 5.947(2.183,16.203) | 2.844(0.591,13.679) |
| I Don’t know | 10 | 113 | 1 | 1 |
| Ever heard of cervical cancer screening method | ||||
| Yes | 68 | 236 | 2.478(1.220,5.031) | 0.642(0.231,1.786) |
| No | 10 | 86 | 1 | 1 |
| Who should be screened | ||||
| Age greater than 21 | 20 | 94 | 2.420(1.015,5.772) | 0.747(0.182,3.069) |
| Commercial sex workers | 20 | 51 | 4.461(1.834,10.849) | 1.214(0.280,5.260) |
| Elderly women | 27 | 77 | 3.989(1.713,9.288) | 0.900(0.221,3.657) |
| Other | 3 | 9 | 3.792(0.852,16.878) | 5.868(0.711,48.418) |
| I don't know | 8 | 91 | 1 | 1 |
| Expense of screening | ||||
| Free | 26 | 79 | 4.608(2.053,10.342) | 1.575(0.592,4.187) |
| It is reasonably priced | 14 | 33 | 5.939(2.365,14.918) | 3.547(1.111,11.320) |
| moderately expensive | 14 | 40 | 4.900(1.973,12.171) | 2.814(0.942,8.406) |
| very expensive | 15 | 44 | 4.773(1.951,11.678) | 2.225(0.757,6.546) |
| I don’t know | 9 | 126 | 1 | 1 |
| Is cervical cancer preventable | ||||
| Yes | 70 | 274 | 1.533(0.693,3.388) | |
| No | 8 | 48 | 1 | |
| Prevention method of cervical cancer | ||||
| No multiple partner | 38 | 113 | 9.752(2.272,41.855) | 6.806(1.405,32.967) |
| Treat papilomavirus | 11 | 41 | 7.780(1.637,36.982) | 6.978(1.279,38.070) |
| Use condom | 9 | 27 | 9.667(1.954,47.820) | 5.214(0.868,31.327) |
| Vaccine | 6 | 24 | 7.250(1.365,38.494) | 8.597(1.401,52.744) |
| Other | 4 | 11 | 10.545(1.716,64.802) | 16.989(2.328,123.982) |
| I do not know | 2 | 58 | 1 | 1 |
| Know age of cervical cancer manifestation | ||||
| Yes | 69 | 294 | 0.730(0.330,1.618) | |
| No | 9 | 28 | 1 | |
| Know the right sex starting age group | ||||
| Yes | 69 | 242 | 5.560(1.309,23.607) | 3.996(0.880,18.149) |
| No | 2 | 39 | 1 | 1 |
| Knowledgeable about cervical cancer | ||||
| Yes | 62 | 191 | 2.658(1.469,4.808) | 0.624(0.182,2.142) |
| No | 16 | 131 | 1 | |
| Presence of substance abuse | ||||
| Yes | 4 | 25 | 0.642(0.217,1.902) | |
| No | 74 | 297 | 1 | |
| Had good attitude towards cervical cancer screening | ||||
| Yes | 40 | 185 | 0.780(0.475,1.280) | |
| No | 38 | 137 | 1 | |
Discussion
The result of our study revealed that, out of total 400 participants enrolled in this study, 78 (19.5%) were subjected for cervical cancer screening. Of these, 17/78 (21.8%) were screened by Visual Inspection Acetic Acid(VIA) method. This may contribute for the low screening of cervical cancer screening though low resource settings should implement evidence-based and affordable alternative approach for cervical cancer screening science VIA reduce the deaths of women in developing countries because it is the simplest method for screening with relative ease of use and lowest cost17.
The current study illustrated as it is fallen in the practice of developing countries; screening coverage is still low, ranging from 0.4% to 14.0% in rural areas and from 2.0% to 20.2% in urban areas18. Cross sectional studies conducted in Nigeria, India, Ghana, Mekele town and Ethiopia exhibited 10%, 8%, 11.6%, 10.7% and 0.6% of cervical cancer screening practice respectively 15, 18, 19, 20, 21. It is far from developed countries carry out; the proportions of women who are screened by Pap test vary from 68 to 84%22. A good example for this utilization reported in study conducted in Brazil gave a picture of 94.7% service consumption 23.
It was founded that out of total screened, 78 (19.5%), study participants 77 (98.7%) did it at once. This also depicted the low utilization of cervical screening service in the study area though women aged 18–69 who are or have ever been sexually active recommended to have two-yearly Pap tests with the current screening program 24.
In the current study 94 (23.5%) and 180 (45%) of study participants did not hear about cervical cancer and problems of genital tract. Many of the participants also did not know about cause of cervical cancer 192(48.0%), symptom of cervical cancer 123(30.8%) and treatment of cervical cancer 156(39.0%). Forty two percent of participants got information about cervical cancer from media.
Very small number of women being screened in sub-Saharan Africa and other developing countries was evidenced by reasons of low levels of awareness and poor knowledge of cervical cancer coupled with unavailability and inaccessibility of cervical cancer screening services23.
The result 94 (23.5%) was found less than carried out in Finote Selam town, Amhara region in 2017 that the awareness of women on cervical cancer was 34.3%21..
Regarding participants who know about prevention methods ((Avoid multiple partner (AOR=6.806; 95%CI: 1.405, 32.967) and treatment of Papilloma virus (AOR=6.978; 95% CI: 1.279, 38.070) of cervical cancer had seven times more likely to get cervical cancer screening service compared to individuals that did not be familiar about methods of prevention. Moreover, the recent study revealed that patients who have knowledge on vaccination against Papilloma virus were nine times more likely to practice screening (AOR= 8.597; 95%: 1.401, 52.744).
Mass campaign early screening and focus from the government and other stake holders to control having multiple sexual partners, human immune deficiency virus positive, history of sexually transmitted infection and early age at initiation of sexual intercourse will reduce cervical cancer by strengthening both cancer prevention and control program and implementation strategies through due attention on the associated risk factors of the study25. Multiple sexual partners’ increases the risk of cervical cancer has been previously documented in studies conducted in Ethiopia and Tanzania 26, 27.
On other hand, the present study showed that the reasonably priced had four times more likely for screening practice for cervical cancer (AOR=3.547; 95% CI: 1.111, 11.320). This is in agreement with Hadiya, Southern Ethiopia16.
Conclusion and Recommendation
The study depicted that there was low utilization of cervical cancer screening that is 19.5% got screened. Awareness about cervical cancer, knowledge of genital tract problems, increased age group, knowledge about prevention method of cervical cancer, and reasonably priced expense had positive influence for screening practice. Therefore, awareness creation about cervical cancer and prevention method is expected from different stakeholder.
Authors’ Contributions
Tenagnework Antefe Abebe, Berhanu Elfu, Abel Lule Tessema, Mulusew Alemneh Sinishaw designed the study, collected data, performed analysis and wrote the manuscript. All authors read and agreed on the final manuscript submitted.
Acknowledgments
The authors gratefully acknowledge GAMBY Medical & Business College of Sciences, Amhara Public Health Institute and Felege Hiwot Referral Hospital for giving the opportunity to study this title.
They would also like to extend their gratitude to the study participants for their volunteer participation. Finally they are confessing data collectors and supervisors for their devotion to the successful completion of the project.
References
- 1.Ferlay J, Soerjomataram I, Dikshit R. (2015) Cancer incidence and mortality worldwide: sources, methods and major patterns. in GLOBOCAN 2012. International journal of cancer 136(5), 359-86.
- 2.WHO. (2018) diagnosis and screening of cervical cancer. Available athttp://www.who.int/cancer/prevention/diagnosis-screening/cervical-cancer/en/
- 3. (2020) Cancer Global Crisis Card [Cervical Cancer Free Coalition Web site]. Available at:http://www.cervicalcancerfreecoalition.org/wp-content/uploads/Cervical-Cancer-Global-Crisis-Card_2013.pdf
- 4.Bruni L, Barrionuevo-Rosas L, Albero G. (2017) . ICO Information Centre on HPV and Cancer (HPV Information Centre). Human Papillomavirus and Related Diseases in Ethiopia .
- 5.Tefera B, Assefa M, Abebe B. (2016) Patterns of Cancer in University of Gondar Hospital: north-West Ethiopia. , J Oncol Med & Pract 1(106), 2.
- 7.Kaku M, Mathew A, Rajan B. (2008) Impact of socio-economic factors in delayed reporting and late-stage presentation among patients with cervix cancer in a major cancer hospital in South India. , Asian Pac J Cancer Prev 9(4), 589-94.
- 8.MM wALBooMER J, Mv Acos, MANosº M M. (1999) Human papillomavirus is a necessary cause of invasive cervical cancer. , vvorldwide. J pathol 189, 12-9.
- 9.Gadducci A, Barsotti C, Cosio S. (2011) Smoking habit, immune suppression, oral contraceptive use, and hormone replacement therapy use and cervical carcinogenesis: a review of the literature. , Gynecological Endocrinology 27(8), 597-604.
- 10.Bruni L, Barrionuevo-Rosas L, Albero G.Human papillomavirus and related diseases in the world. ICO/IARC Information Centre on HPV and Cancer (HPV Information Centre)(2017) .
- 11.Getahun F, Mazengia F, Abuhay M. (2013) Comprehensive knowledge about cervical cancer is low among women in Northwest Ethiopia. , BMC cancer 13(1), 2.
- 12.Birhanu Z, Abdissa A, Belachew T. (2012) Health seeking behavior for cervical cancer in Ethiopia: a qualitative study. International journal for Equity in health. 11(1), 83.
- 13.Hailu A, Mariam D H. (2013) Patient side cost and its predictors for cervical cancer in Ethiopia: a cross sectional hospital based study. , BMC cancer 13(1), 69.
- 14.Goldie S J, Gaffikin L, Goldhaber-Fiebert J D. (2005) Cost-effectiveness of cervical-cancer screening in five developing countries. , New England Journal of Medicine 353(20), 2158-68.
- 15.Bayu H, Berhe Y, Mulat A. (2016) Cervical cancer screening service uptake and associated factors among age eligible women in mekelle zone, northern ethiopia,2015:A community based study using health belief model. , PloS 11(3).
- 16.Aweke Y H, Ayanto S Y, Ersado T L. (2017) Knowledge, attitude and practice for cervical cancer prevention and control among women of childbearing age in Hossana Town, Hadiya zone, Southern Ethiopia: Community-based cross-sectional study. , PLoS One 12(7).
- 17.Wright Jr TC, Kuhn L. (2012) Alternative approaches to cervical cancer screening for developing countries. , Best practice & research Clinical obstetrics & gynaecology 26(2), 197-208.
- 18.Shah V, Vyas S, Singh A. (2012) Awareness and knowledge of cervical cancer and its prevention among the nursing staff of a tertiary health institute in Ahmedabad. , Gujarat, India 6.
- 19.Adageba R K, Danso K A, Ankobea F K. (2011) Knowledge of cervical cancer and patronage of cervical cancer screening services among female health workers in Kumasi. , Ghana. African Journal of Haematology and Oncology 2(1).
- 20.Abotchie P N, Shokar N K. (2009) Cervical cancer screening among college students in Ghana: knowledge and health beliefs. , International Journal of Gynecologic Cancer 19(3), 412-6.
- 21.Geremew A B, Gelagay A A, Azale T. (2018) Comprehensive knowledge on cervical cancer, attitude towards its screening and associated factors among women aged 30–49 years in Finote Selam town, northwest Ethiopia. Reproductive health. 15(1), 29.
- 22.Aswathy S, Quereshi M A, Kurian B, Leelamoni K. (2012) Cervical cancer screening: Current knowledge & practice among women in a rural population of Kerala, India. The Indian journal of medical research. 136(2), 205.
- 23.WorldHealthOrganization.Institut Catala d’Oncologia: Human Papillomavirus and Related Cancers in Ethiopia, Fact Sheet2014.
- 24.Karampotsis E, Dounias G, Jantzen J. (2019) Machine Learning Approaches for Pap-Smear Diagnosis: An Overview. Machine Learning Paradigms:. 67-127.
- 25.Getachew E. (2015) Knowledge Attitude and Practice on Cervical Cancer and Screening among Reproductive health Service Clients, Addis Ababa. , Ethiopia
