Maxillary Constriction with Skeletal Class II Malocclusion - A Comprehensive Treatment Approach.
Abstract
This case report reiterates the fact that a bilateral posterior crossbite with severe skeletal class II malocclusion in the growth period could be effectively treated by a comprehensive approach with a rapid palatal expansion appliance followed by fixed appliance therapy. A 14-year-old boy presented with a severe skeletal Class II malocclusion with an orthognathic maxilla, retrognathic mandible and a high mandibular plane angle with an Angles’ Class II division 1 subdivision malocclusion with maxillary constriction, increased overjet, deep bite and severe crowding of maxillary and mandibular incisors. A banded rapid palatal expansion appliance was initially given to correct the bilateral posterior cross bite and subsequently maxillary and mandibular first premolars were extracted and Roths’ Pre adjusted edgewise appliance therapy (0.022 x 0.28-inch slot) was strapped up to correct the severe tooth size-arch length discrepancy. The patient’s soft tissue profile and dentofacial esthetics improved dramatically with increased self-confidence and enthused self-esteem.
Author Contributions
Academic Editor: Stefanos Kourtis, Associate Professor
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2016 A. Arif Yezdani, et al
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Introduction
Growth period of an individual is an ideal period for the treatment of desired orthopaedic effects of skeletal jaw discrepancies. It has been reported that a deficiency in maxillary arch width is associated with Class II malocclusion.Skeletal maxillary constriction treated with rapid palatal expansion appliance has been widely reported in literature, however, other possible indications of this technique have also been proposed in addition to its prime objective of correction of posterior cross bite.1,2
Haas3 opined that all Class II division 1 and Class division 2 patients present mandibular functional retrusion and that with Class II division 1 group the retrusion was due to constriction of maxillary dental arch, especially between the canines. It has been reported that skeletal Class II malocclusion with retrognathic mandible have benefited immensely with spontaneous forward positioning of the mandible facilitated by the widening of the constricted maxilla.4, 5
This case report illustrates the treatment of a skeletal Class II malocclusion with an orthognathic maxilla and retrognathic mandible with Angles’ Class II division 1 subdivision malocclusion with maxillary constriction and severe maxillary and mandibular tooth size-arch length discrepancy. Initial treatment with rapid palatal expansion appliance to correct the maxillary constriction to promote spontaneous forward positioning of the mandible and subsequent orthodontic treatment with fixed appliance therapy resulted in a remarkable change in the patient’s dentofacial esthetics.
Case Report
Diagnosis and Etiology
A 14-year-old male presented with severe crowding and forward placement of the maxillary and mandibular incisors. Inherited growth pattern could have been the most possible etiological factor.
Extraoral assessment. (Figure 1a,Figure 1b,Figure 1c).
Figure 1a.Pre-treatment extra-oral-Frontal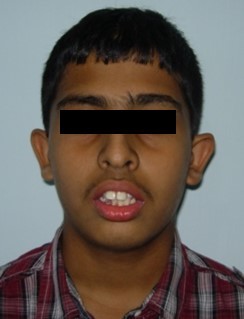
Figure 1b.Pre-treatment extra-oral-Profile
Figure 1c.Pre-treatment extra-oral-Smiling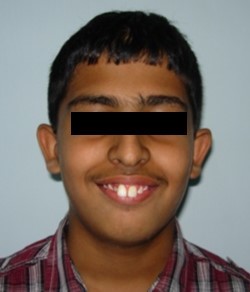
The patient had a leptoprosopic face, convex profile, posterior divergence, incompetent lips, clinical high mandibular plane angle, complete maxillary incisor display on smiling with no signs of temporomandibular joint dysfunction.
Intraoral assessment. (Figure 1d,Figure 1e,Figure 1f,Figure 1g,Figure 1h).
Figure 1d.Pre-treatment intra-oral-Frontal
Figure 1e.Pre-treatment intra-oral-Right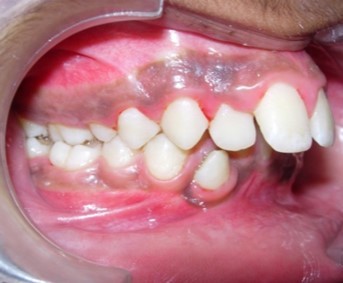
Figure 1f.Pre-treatment intra-oral-Left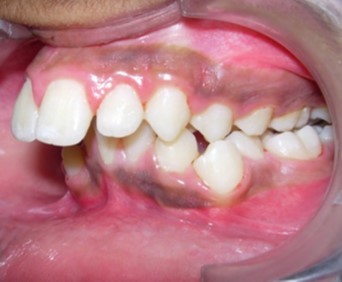
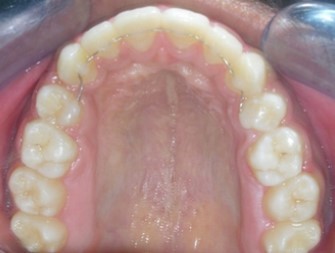
Figure 1g.Pre-treatment intra-oral-Upper occlusal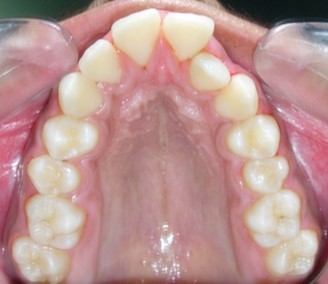
Figure 1h.Pre-treatment intra-oral-Lower occlusal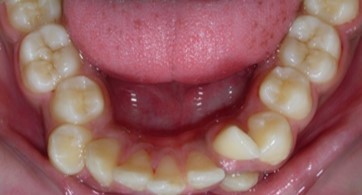
The maxillary arch was V-shaped with severely proclined and rotated maxillary incisors with a palatally placed 12. The mandibular arch was U-shaped with severe crowding of mandibular incisors, with 43 partially erupted and buccally placed with transpositioned 42 and 43, with 42 mesiolingually rotated, 33 distolingually rotated and 34 distolingually rotated and buccally placed.
Severe increase in overjet and deep bite were both observed. The maxillary midline coincided with the skeletal midline but the mandibular midline was shifted to the right side by 1 mm. Bilateral maxillary posterior crossbite was also observed. On right side the molar relation was Class I and on the left side it was Class II. The canine relation was Class II on the left side and the curve of Spee was increased.
Radiographic assessment. The panoramic radiograph confirmed the presence of all permanent teeth with the presence of 18, 28, 38 and 48 tooth germs with normal alveolar bone levels. (Figure 2).
Figure 2.Pre-treatment panoramic radiograph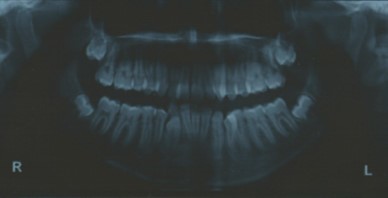
Cephalometric analysis revealed a skeletal Class II pattern, with an orthognathic maxilla and retrognathic mandible with high mandibular plane angle and severely proclined maxillary and mandibular incisors with increased lower anterior facial height. (Figure 3).
Treatment Objectives
The main treatment objective was to improve the phonation, lip competence, smile esthetics and soft tissue profile. The initial phase of treatment was initiated with a banded rapid palatal expansion appliance to correct the bilateral maxillary posterior crossbite. (Figure 4). Subsequent to correction of the same, maxillary and mandibular first premolars were extracted and the orthodontic phase was commenced to correct the severe crowding of the maxillary and mandibular dental arch.
Treatment Alternatives
An orthopaedic phase with a functional appliance for the retrognathic mandible could have been contemplated, but the need of the hour was to correct the maxillary constriction and the severe tooth size-arch length discrepancy. Correction of maxillary constriction would release the mandible anteriorly to express its inherent genetic potential.
Bonded RME consists of an acrylic capping covering the occlusal surfaces of maxillary premolars and molars, housing the arms of the rapid maxillary expansion screw which is cemented to the maxillary posteriors with glass ionomer cement. This is useful in high angle cases to achieve mild intrusion of the maxillary posteriors to facilitate autorotation of the mandible in an upward and forward direction.
Though bonded RME could have been used, we however, preferred to use banded RME as it is more hygienic and easy to maintain with good patient co-operation.
Treatment Progress
The mandibular first premolars were first extracted to commence treatment of the mandibular arch simultaneously with expansion of the constricted maxilla. Preadjusted edgewise brackets (Roth prescription, 0.022 x 0.028-inch slot) were initially bonded to the maxillary and mandibular teeth. Banded Hyrax (Hygienic rapid palatal expander) was cemented to the maxillary first premolars and molars. (Figure 5). The patient was advised to activate the appliance a quarter turn once or twice a day to achieve adequate expansion consistently. Subsequent to over-expansion of the maxilla the Hyrax was inactivated with a ligature tie tied into the screw holes and was retained in situ for a period of 6 months, after which the maxillary first premolars were extracted and the maxillary arch treatment was commenced.
Figure 5.Rapid palatal expansion appliance in situ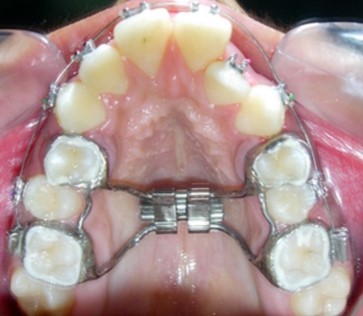
Initial alignment was done with upper and lower 0.014-inch nickel titanium archwires (Figure 6a,Figure 6b,Figure 6c). This was followed with 0.016-inch nickel titanium archwires. Space for blocked out 42 was created by an open coil spring on a 0.018-inch stainless steel archwire. Deep bite was corrected with a lower 0.016-inch reverse curve nickel titanium wire. Extraction spaces in the maxillary and mandibular dental arches were closed with 9mm nickel titanium retraction coil springs attached to crimpable hooks on 0.017 x 0.025-inch stainless steel archwires and finishing and detailing was completed with 0.019 x 0.025-inch stainless steel archwires.
Figure 6a.Initial levelling and alignment – Upper / Lower 0.014-inch nickel titanium wires – Frontal
Figure 6b.Initial levelling and alignment – Upper / Lower 0.014-inch nickel titanium wires – Right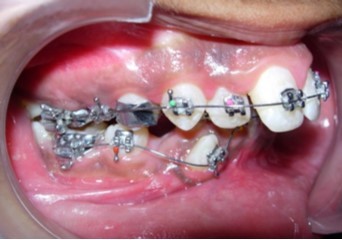
Figure 6c.Initial levelling and alignment – Upper / Lower 0.014-inch nickel titanium wires – Left
Results
The soft tissue frontal and profile improved dramatically. (Figure 7a-b). The bilateral posterior crossbite was corrected. The severe increase in overjet of about 13mm was effectively reduced to 3mm and the severe deep bite was also corrected (Figure 7c,Figure 7d). Fixed maxillary and mandibular lingual retainers were given. (Figure 7e, Figure 7f). Post orthodontic treatment, normal root inclinations of the teeth and normal alveolar bone levels was observed. (Figure 8).
Figure 7a.Post-treatment extra-oral-Frontal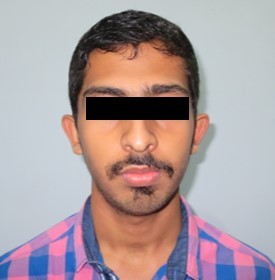
Figure 7b.Post-treatment extra-oral-Smiling
Figure 7c.Post-treatment intra-oral-Frontal
Figure 7d.Post treatment intra-oral – Right
Figure 7e.Post-treatment intra-oral-Upper occlusal
Figure 7f.Post-treatment intra oral-Lower occlusal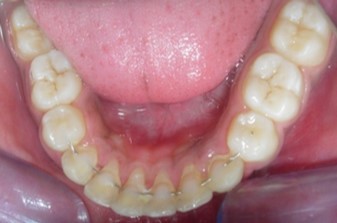
Figure 8.Post-treatment panoramic radiograph
Post treatment lateral cephalometric radiograph was taken to assess the treatment changes. (Figure 9). The changes in maxilla in the anteroposterior direction was insignificant, however an increase in the length of the mandible measured from Condylion (Co) to Gnathion (Gn) and an increase in anterior facial height was observed. Maxillary incisors were retracted dramatically by 8mm and the mandibular incisors were proclined by 3mm to camouflage the skeletal class II malocclusion.(Table 1). Effective expansion of the maxillary constriction as an end-of treatment goal was achieved. (Figure 10a,Figure 10b).
Figure 9.Post-treatment lateral cephalometric radiograph
| Variable | Norm | Pre-treatment | Post-treatment |
| SNA (degrees) | 82 ± 2 | 80 | 80 |
| SNB (degrees) | 80 ± 2 | 72.5 | 71 |
| ANB | 2 ± 2 | 7.5 | 9 |
| U1 to NA (degrees) | 22 | 26 | 17 |
| U1 to NA (mm) | 4 | 9 | 1 |
| L1 to NB (degrees) | 25 | 30 | 33 |
| L1 to NB (mm) | 4 | 8 | 11 |
| N-Me (mm) | 123 ± 5 | 112 | 142 |
| N-ANS (mm) | 56 ± 3 | 53 | 66 |
| ANS-Me (mm) | 70 ± 3 | 59 | 78 |
| FMA (degrees) | 25 | 32 | 36 |
| Co-Gn (mm) | - | 102 | 121 |
| E-plane LL (mm) | -2 ± 2 | 2.5 | 5 |
Figure 10a.Pre aexpansion - maxillary arch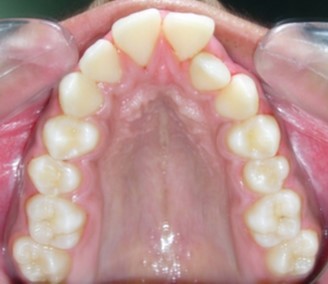
Discussion
Bilateral posterior cross bite with severe skeletal Class II malocclusion is a routinely encountered malocclusion in an orthodontic practice. The probable causes for skeletal posterior crossbite could be hereditary, airway obstruction, non-nutritive sucking habits, lowered tongue position, and early loss of primary teeth. The skeletal malocclusion in the case reported had an orthognathic maxilla and retrognathic mandible with severe maxillary constriction. Some authors are of the opinion that functional appliances have no real effect on mandibular length 6,7 while others believe that mandibular growth can be increased with functional appliance treatment 8, 9, 10. However, Wendling11was of the opinion that a spontaneous correction of some Class II malocclusions is favoured with initial rapid palatal expansion. It has been reported in the literature that in the Class II, division 1 group, the retrusion was due to constriction of the maxillary dental arch and that in such cases, it is important to expand the maxillary arch to obtain a permanent orthopedic effect on the maxilla by releasing the mandible to move anteriorly. Literature reports too point to a strong correlation of deficient maxillary arch width and Class II malocclusion.12,13In compliance with this tenet banded Hyrax was used to expand the maxilla to permit spontaneous forward positioning of the mandible. The rapid maxillary expansion appliance widens the intermaxillary suture and increases basal bone width 14, 15, 16, 17as also causes an increase in dental arch perimeter18 as had been observed in the treated case too. Post treatment cephalometric analysis revealed an increase in length of the mandible with no orthopaedic functional device given to jump the mandible. This could most probably have been attributed to the widening of the constricted maxilla with the banded rapid maxillary expansion appliance that promoted the mandible to express normal growth in an anterior direction. However mandibular growth was not sufficient enough to correct the severe anteroposterior skeletal discrepancy but the dentoalveolar compensation was maximized. The increased overjet of 13 mm was reduced to 3mm at the end of treatment most probably attributed to retroclination of the maxillary anteriors and proclination of the mandibular incisors. The mesial movement of the mandibular arch observed in this patient was favourable for the reduction in the increased overjet in compliance to the observation by Voudouris et al 19who too found mesial movement of the mandibular arch in both experimental animals and human subjects. The increased overbite was reduced to normal overbite by the flattening of the curve of Spee. A two-phase treatment therapy was instrumental in reducing the severity of the skeletal jaw discrepancy. The increase in lower anterior facial height could have been attributed to the effects of the banded rapid palatal expansion appliance that caused an initial downward and forward movement of the maxilla, together with a downward and backward rotation of the mandible. The initial increase in the anterior facial height is a temporary occurrence as long term follow-up of cephalometric analyses have shown a reversal back to normal and therefore concerns about using rapid maxillary expansion in patients with vertical growth patterns or an extremely convex facial profile are not substantiated.20
The end of treatment result showed a good improvement in the transverse, anteroposterior, and vertical dimensions with markedly improved dentofacial esthetics.
Conclusion
A combination therapy of a banded rapid palatal expansion appliance and orthodontic treatment with pre adjusted edgewise appliance therapy was instrumental in the correction of a severe skeletal Class II malocclusion with an orthognathic maxilla and retrognathic mandible. This two-phase therapy resulted in a dramatic improvement of the facial and smile esthetics with good occlusal interdigitation that enhanced the patient’s speech, personality and self-esteem.
References
- 1.Baccetti T, Franchi L, McNamara J, Tollaro I. (1997) Early dentofacial features of Class II malocclusion: a longitudinal study from the deciduous through the mixed dentition. , Am J Orthod Dentofacial Orthop; 111, 502-509.
- 2.Will L A. (1996) Transverse maxillary deformities: diagnosis and treatment. Oral Maxillofacial Surg. 5, 1-28.
- 3.Haas A J. (1970) Palatal expansion: just the beginning of dentofacial orthopedics. Am JOrthod. 57, 219-255.
- 4.McNamara J A. (2000) Maxillary transverse deficiency. , Am J Orthod Dentofacial Orthop; 117, 567-570.
- 6.Janson I. (1983) Skeletal and dentoalveolar changes in patients treated with a bionator during prepubertal and pubertal growth.In:McNamara JA Jr,Ribbens KA,Howe RP,editors. Clinical alteration of the growing face. Monograph 14. Craniofacial Growth Series. Ann Arbor: Center for Human Growth and Development;University of Michigan.
- 7.Vargervik K, Harvold E P. (1985) Response to activator treatment in Class II malocclusions. , Am J Orthod; 88, 242-51.
- 8.Luder H U. (1983) Skeletal profile changes related to two patterns of activator effects. , Am J Orthod; 81, 390-6.
- 9.McNamara JA Jr, Bookstein F L, Shaughnessy T G. (1985) Skeletal and dental changes following functional regulator therapy on Class II patients. , Am J Orthod; 88, 91-110.
- 10.Mamandras A H, Allen L P. (1990) Mandibular response to orthodontic treatment with the bionator appliance. , Am J Orthod Dentofacial Orthop; 97, 113-20.
- 11.Wendling L K. (1997) Short-Term Skeletal and Dental Effects of the Acrylic Splint Rapid Maxillary Expansion Appliance [master’s thesis]. Ann Arbor, Mich: The University of Michigan;.
- 12.Kirjavainen M, Kirjavainen T, Haavikko K. (1997) Changes in dental arch dimensions by use of an orthopedic cervical headgear in Class II correction. , Am J Orthod Dentofacial Orthop; 111, 59-66.
- 13.RMA Lima, Lima A L. (2000) Case report: long-term outcome of Class II division 1 malocclusion treated with rapid palatal expansion and cervical traction. , Angle Orthod; 70, 89-94.
- 14.Haas A J. (1961) Rapid expansion of the maxillary dental arch and nasal cavity by opening the midpalatal suture. , Angle Orthod; 31(2), 73-90.
- 15.Starnbach H, Bayne D, Cleall J, Subtelny J D. (1966) Facioskeletal and dental changes resulting from rapid maxillary expansion. , Angle Orthod; 36(2), 152-164.
- 16.Wertz R A. (1970) Skeletal and dental changes accompanying rapid midpalatal suture opening. , Am J Orthod; 58(1), 41-66.
- 17.Garib D G, JFC Henriques, Janson G, Freitas M R, Coelho R A. (2005) Rapid maxillary expansion—tooth tissue-borne versus tooth-borne expanders: a computed tomography evaluation of dentoskeletal effects. , Angle Orthod; 75(4), 548-557.
- 18.Adkins M D, Nanda R S, Currier G F. (1990) Arch perimeter changes on rapid palatal expansion. , Am J Orthod Dentofacial Or-thop; 97(3), 194-199.